A vision of creating a state-of-the-art treatment center in which multiple medical disciplines would practice in close proximity to one another became a reality on June 7 when Memorial Sloan Kettering opened a facility housing the novel Center for Image-Guided Interventions (CIGI), a suite of endoscopy rooms, and new operating rooms for the Surgical Day Hospital (SDH).
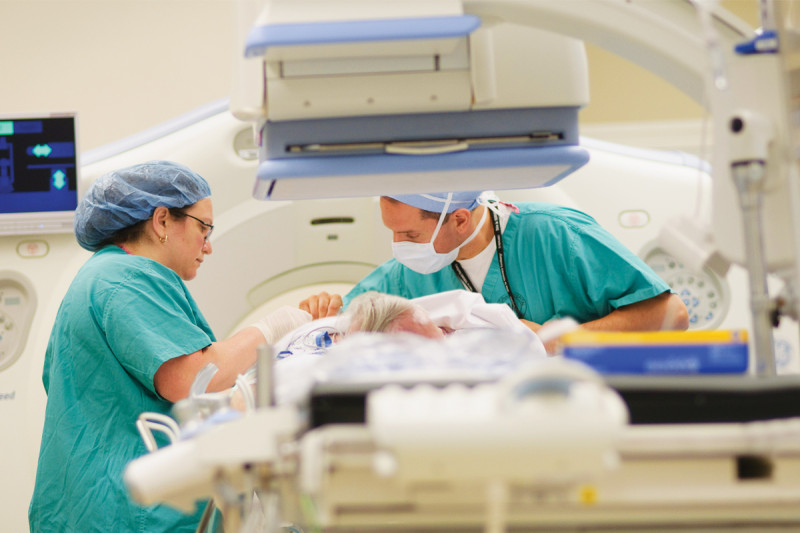
Enhancing the patient experience and supporting cooperative treatment and research among clinicians, this multidisciplinary platform — located on the second floor of Memorial Hospital (M2) — is anchored by CIGI, which features state-of-the-art imaging tools for guiding cancer diagnosis and treatment. The interventional radiologists working in CIGI will collaborate with their surgical and endoscopy colleagues to deliver minimally invasive cancer therapies that reduce risks, shorten hospital stays, and decrease the cost to patients.
“Seven years in the making, this magnificent facility is a result of shared vision and collaboration,” said Hedvig Hricak, Chair of the Department of Radiology, who, along with Peter T. Scardino, Chair of the Department of Surgery, was instrumental in conceptualizing and planning the M2 platform. “The close proximity of radiology, surgery, and endoscopy will produce innovations that advance the medicine of the 21st century and also provide a superb environment for our patients.”
Interventional radiology (IR) involves minimally invasive treatments using image guidance. The tools of IR physicians include fluoroscopy, computed tomography (CT), ultrasound, positron emission tomography (PET), and magnetic resonance imaging (MRI). CIGI has six procedure rooms that contain leading-edge imaging equipment. “The rooms are designed to provide much more than conventional IR rooms,” Dr. Hricak said. They are furnished with flat-panel displays — called the “Walls of Knowledge” — that include all patient clinical and laboratory data. In addition, a state-of-the-art communication system allows physicians in separate CIGI procedure rooms to consult via videoconferencing and share real-time images.
“Today’s research is tomorrow’s practice,” Dr. Hricak said. “Therefore, along with the clinical facility, we also have invested in a dedicated research facility.” The CIGI laboratory, located in the Zuckerman Research Center, is devoted to developing and testing in animal models techniques that can eventually be evaluated in clinical trials.
“CIGI is going to be an unbelievable platform for imaging and treating cancer,” said Stephen B. Solomon, Interventional Radiology Service Chief and Director of CIGI. “We have an interventional PET/CT scanner in the center that will allow us to take advantage of new markers and tracers to pinpoint cancers in ways that were impossible before. The two new MRI rooms will enable us to continue refining a new approach in which we use MRI not as a diagnostic tool but to guide and monitor therapies in real time. For example, we are developing ways to noninvasively destroy tumors with heat by using focused ultrasound technology, and minimally invasively by using lasers, and the MRIs enable us to closely monitor the temperature to ensure we are destroying the target.”
Collaboration Across Disciplines
Planning for CIGI began in 2003. As new technology began to emerge that allowed interventional radiologists to do new kinds of minimally invasive procedures under the most advanced forms of image guidance, Dr. Hricak and other Memorial Sloan Kettering clinical chairs concluded that such technological advances were not realizing their full potential in cancer therapy.
CIGI falls under the umbrella of Memorial Sloan Kettering’s Image-Guided Intervention Program (IGIP), established in 2008 to oversee and coordinate activities in the medical disciplines that use image guidance at Memorial Sloan Kettering. IGIP is directed by Dr. Solomon and Yuman Fong, Vice Chair of Technology Development in the Department of Surgery.
From its earliest stages, CIGI was envisioned as a multidisciplinary facility in which IR physicians could work with surgeons and other medical interventionalists. The M2 platform offers opportunities for combining noninvasive interventions in new ways.
“If you think about how surgeons, interventional radiologists, gastroenterologists, and pulmonologists work — everyone with an instrument that physically manipulates an anatomic structure or tumor — we each have our little area that we specialize in,” Dr. Fong said. “The exciting thing is that now we have a facility that allows all these different people, from different disciplines, to think together and work together. And for patients this means we will be able to combine procedures and therapies and do them in less invasive ways. For example, I can envision a gastroenterologist using an endoscope to come through the esophagus and stomach to remove a small tumor in the abdomen while an interventional radiologist occludes a blood vessel with a catheter to slow bleeding and improve visibility.”
Dr. Scardino explained that the new platform also makes it possible to consolidate several procedures performed by different specialists into a single patient visit. “A patient with an unspecified mass in the chest could typically require a CT scan by an interventional radiologist to biopsy it, an ultrasound by an endoscopist to stage it and determine its size, and a surgical procedure called a mediastinoscopy to take out a lymph node,” he said. “In the past, getting all three procedures would require three separate trips to the hospital over several weeks. Now we can do them consecutively in the same day and move promptly to therapy.”
Upgraded Operating Rooms
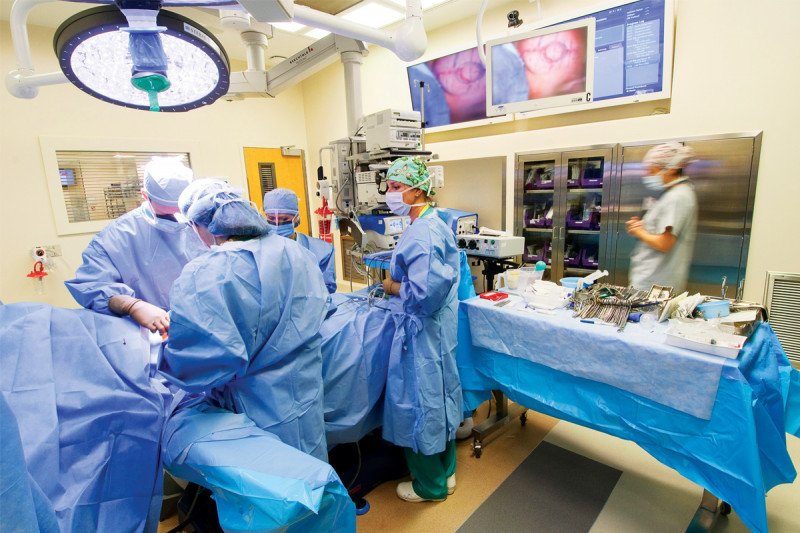
The seven new Surgical Day Hospital operating rooms replace five rooms in the former SDH location. Procedures done in the SDH — such as breast lumpectomies, prostate biopsies, or removal of certain head and neck lesions — are less intensive and of shorter duration than those performed in the main surgical center on Memorial Hospital’s sixth floor. A typical procedure in the SDH takes about two hours, and patients can usually leave the hospital to go home later the same day.
The new SDH operating rooms are larger than those in the former SDH and have many of same features found in the main surgical center. These include ceiling-mounted “booms,” which provide operating room essentials such as anesthesia, oxygen, and suction without taking up floor space; the Walls of Knowledge; and videoconferencing capabilities with physicians in other rooms.
Advanced Endoscopy Technology
Robert C. Kurtz, Chief of the Gastroenterology and Nutrition Service, said the new gastrointestinal endoscopy suite will help Memorial Sloan Kettering physicians address the surge in demand for complex interventional endoscopic procedures. “Many palliative procedures needed for management of cancer patients that used to be done in an operating room by surgeons are now done endoscopically by a gastroenterologist or using interventional radiology,” he explained. “As an example, in the past a patient with a bowel obstruction caused by a tumor would traditionally have required surgical correction of the obstruction during which the abdomen would be opened to unblock the bowel. Now we can use an endoscope to insert a self-expanding metal stent to relieve the obstruction, and anticancer therapy such as chemotherapy can begin much sooner without postoperative delay.”
The four new endoscopy rooms are equipped with the latest high-definition screens, which present sharper, clearer images. “This is the most modern endoscopic technology available,” Dr. Kurtz said. “The images have far more pixels, and the picture’s much easier to see. In addition, some of the endoscopes have what is called narrow band imaging, which improves our ability to detect abnormalities in the lining of the colon or stomach.” Dr. Kurtz praised Hans Gerdes, the director of the gastrointestinal endoscopy unit, and his colleagues for their hard work and vision in the planning of the new unit.
Dr. Kurtz also was enthusiastic about the new opportunities for combined procedures with surgical and radiology colleagues on the M2 platform. “Instead of going to a different floor with our equipment, we can just walk into an adjacent operating room or procedure room and perform an endoscopic procedure in conjunction with a surgical treatment,” he said. “The patient needs only one anesthesia in one location. That’s a tremendous benefit.”
Enhanced Patient Experience
In addition to having the most modern technology, the M2 platform offers amenities that enhance the patient experience. According to Michelle Burke, Assistant Hospital Administrator and Director of Nursing for Perioperative Services, the most significant improvement involves privacy. A patient preparation area consisting of 48 individual bays serves the facility.
After checking in, each patient is escorted to his or her private bay in the pre-procedure area. The bay includes a bed, sliding glass doors, a television, and a guest chair.
Each bay contains equipment to monitor vital signs and administer intravenous fluids, as well as a computer so medical staff can complete documentation without leaving the patient’s bedside. After the procedure is done, the patient is escorted to a similar bay in the post-procedure area for recovery before being discharged.
“It’s a calm, comforting environment for patients who often are feeling stress, and this allows them to be alone in their own space with a family member or friend, rather than in a crowded waiting area with other patients,” Ms. Burke said. “Our goal is to let patients know how much we care by doing this.”
M2 also has a pharmacy and five consultation rooms where patients, family members, or friends can meet privately with physicians. The platform will serve approximately 120 patients per day.
Building for the Future
CIGI was designed with the understanding that interventional radiology will continue to progress rapidly, making it difficult to predict how new technology might be implemented in the future. Procedure rooms were configured to have extra space for new devices that may be developed in upcoming years.
“The rapid pace at which new radiology instrumentation is being introduced necessitated that we design this space to maximize future flexibility,” elaborated Vice President for Facilities Management Edward J. Mahoney. “In the case of CIGI, there were a variety of new instrument modifications, some of which occurred at the very last minute. Flexible design allowed us to adapt to these changes in the field minimizing impact to the project schedule. Although designing state-of-the-art facilities today that are also capable of accommodating tomorrow’s technology is no small task, meeting this challenge is essential to ensuring that Memorial Sloan Kettering maintains its leadership position in the field of cancer care and research.”
It is expected that collaborative techniques generated in the M2 platform will improve the standard of care not just at Memorial Sloan Kettering but at other institutions as well. Dr. Solomon said a multidisciplinary group of Memorial Sloan Kettering physicians already has weekly meetings to discuss new cases and technologies. In the future, the plan is to host conferences that bring in scientists and physicians from other institutions to share information on image-guided- intervention techniques and to train them in new methods developed at Memorial Sloan Kettering.