This information will help you get ready for your procedure to have a percutaneous endoscopic gastrostomy (PEG) drainage tube placed at MSK.
A PEG is a tube that’s put into your stomach to drain stomach juices and fluid. This will help relieve the nausea and vomiting caused by a blockage in your stomach or bowel and will make you feel more comfortable. The tube is placed during a procedure called an endoscopy, which is described in the “What to expect” section in this resource.
Having a PEG tube will let you enjoy eating and drinking. You will be able to drink liquids and eat soft foods or foods that have been mixed in the blender. However, these foods and liquids will only give you a small amount of nutrition. This is because they will mostly drain through the tube into a drainage bag. Your doctor or nurse will discuss with you how you will meet your nutritional needs.
1 week before your procedure
Ask about your medicines
You may need to stop taking some of your medicines before your procedure. We have included some common examples below.
- If you take medicine to thin your blood, ask the doctor who prescribes it for you when to stop taking it. Some examples are warfarin (Coumadin®), dalteparin (Fragmin®), heparin, tinzaparin (Innohep®), enoxaparin (Lovenox®), clopidogrel (Plavix®), and cilostazol (Pletal®).
- If you take insulin or other medicines for diabetes, you may need to change the dose. Ask the doctor who prescribes your diabetes medicine what you should do the morning of your procedure.
Get a letter from your doctor, if needed
If you have an automatic implantable cardioverter-defibrillator (AICD), you will need to get a clearance letter from your cardiologist before your procedure.
Arrange for someone to take you home
You must have a responsible care partner take you home after your procedure. A responsible care partner is someone who can help you get home safely. They should be able to contact your care team if they have any concerns. Make sure to plan this before the day of your procedure.
If you don’t have a responsible care partner to take you home, call one of the agencies below. They’ll send someone to go home with you. There’s a charge for this service, and you’ll need to provide transportation. It’s OK to use a taxi or car service, but you still need a responsible care partner with you.
| Agencies in New York | Agencies in New Jersey |
| VNS Health: 888-735-8913 | Caring People: 877-227-4649 |
| Caring People: 877-227-4649 |
3 days before your procedure
You will get a telephone call from an endoscopy nurse. They will review the instructions in this resource with you and ask you questions about your medical history. The nurse will also review your medicines and tell you which ones to take the morning of your procedure.
The day before your procedure
Note the time of your procedure
A staff member will call you after the day before your procedure. If your procedure is scheduled for a Monday, they’ll call you on the Friday before. If you do not get a call by , call 212-639-5014.
The staff member will tell you what time to arrive for your procedure. They’ll also remind you where to go.
If you need to cancel your procedure for any reason, call the doctor who scheduled it for you.
Instructions for eating and drinking: 8 hours before your arrival time
|
The day of your procedure
Instructions for eating and drinking: 8 hours before your arrival time
|
Things to remember
- Take the medicines you were instructed to take the morning of your procedure with a few sips of water.
- Don’t put on any lotion, cream, powder, deodorant, makeup, or perfume.
- Take off all jewelry, including body piercings.
- Leave all valuables, such as credit cards and jewelry, at home.
- If you wear contacts, wear your glasses instead.
What to bring with you
- A list of the medicines you take at home including patches and creams
- Medicines for breathing problems (such as inhalers), medicines for chest pain, or both
- A case for your glasses
- Your Health Care Proxy form, if you have completed one
Where to go
Your procedure will take place at one of these locations:
-
David H. Koch Center
530 E. 74th St.
New York, NY 10021
Take the elevator to the 8th floor. -
Endoscopy Suite at Memorial Hospital (MSK’s main hospital)
1275 York Ave. (between East 67th and East 68th streets)
New York, NY 10065
Take the B elevator to the 2nd floor. Turn right and enter the Endoscopy/Surgical Day Hospital Suite through the glass doors.
What to expect
Once you arrive at the hospital, doctors, nurses, and other staff members will ask you to state and spell your name and date of birth many times. This is for your safety. People with the same or similar names may be having procedures on the same day.
Your doctor will explain the procedure to you and answer any questions you may have. They will ask you to sign a consent form.
When it’s time for your procedure, you will be brought into the procedure room and helped onto an exam table. You will be attached to equipment to monitor your heart, breathing, and blood pressure. You will also get oxygen through your nose. A mouth guard will be placed over your teeth to protect them.
You will get anesthesia (medicine to make you sleepy) through your IV. Once you’re asleep, your doctor will pass the endoscope (a flexible tube with a camera at the end) through your mouth, down your esophagus (food pipe) and into your stomach.
Your doctor will make a tiny incision (surgical cut) on the skin of your abdominal (belly) wall and pass a feeding tube through the incision. The tube will come out about 8 to 12 inches outside your body and will be covered by a small bandage dressing to keep in place.
When your doctor has completed the procedure, they will take out the endoscope. They will connect the end of your PEG tube to a bag into which your stomach fluids will drain.
After your procedure
In the hospital
You will wake up in the Post Anesthesia Care Unit (PACU). Your nurse will monitor your temperature, pulse, breathing, and blood pressure. They will also check the bandage around your tube. You will stay in the PACU until you’re fully awake.
Your nurse and dietitian will tell you about the types of foods you can eat. Your nurse will also tell you where to get supplies and show you how to:
- Clean the skin around your PEG tube.
- Flush the tube.
- Fix the tube if it gets clogged.
- Take care of and change the drainage bag.
- Take medicines.
- Clamp or cap the tube.
Before you’re discharged from the hospital, your nurse will give you the following supplies to take home:
-
Supplies for dressing change:
- 4 x 4 gauze
- Tape or Cath-Secure®
- Zinc oxide (Desitin®) ointment
- Iodine (Betadine®) swab sticks
- 1 irrigation (flushing) kit
- 2 drainage bags
- 2 caps
Your doctor may also prescribe pain medicine to treat any pain or discomfort at your incision site.
At home
- You may feel some soreness in your throat. This is normal and will get better in 1 or 2 days.
- You may have some discomfort at your incision site for the first 24 to 48 hours. If so, take your pain medicine as instructed.
- You can shower 48 hours after your procedure. Don’t take tub baths or swim for 2 weeks after your procedure.
- You can resume your normal activities the day after your procedure.
Caring for your PEG tube
Caring for the skin around your PEG tube
You will need to care for the skin around your PEG tube. Follow the steps below.
Every day, inspect the skin around your feeding tube for any redness, swelling, or pus. Tell your doctor or nurse practitioner (NP) if you’re having any of these symptoms.
Follow these instructions for the first 2 days after your procedure.
- Take off the old dressing.
- Clean the skin around your tube with iodine swab sticks once a day.
- Apply zinc oxide ointment.
- Cover the incision site with a 4 x 4 gauze.
- Loop the tube and secure it with tape or use a Cath-Secure tab to hold it in place (see Figure 1).
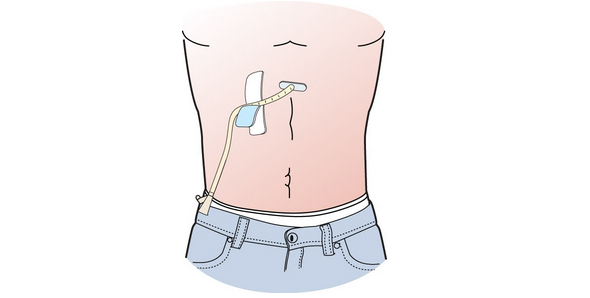
Figure 1. Securing your tube
On the third day after your procedure, start a daily routine of caring for the skin around your tube while showering.
- Before you shower, take off the old dressing around your tube. It may be stained with fluid or mucus. There may also be old blood or crusting around the tube. This is normal.
- Wash the skin around your tube with soap and water, removing any fluids or crusting. Gently pat it dry.
- After you get out of the shower, apply zinc oxide ointment.
- Cover your insertion site with a 4 x 4 gauze pad.
- Loop the tube and secure it with tape or with a Cath-Secure tab.
If your tube becomes dislodged or falls out, cover the opening with a thick bandage. Use several 4 x 4 gauzes. Then, call your doctor right away. Do not eat or drink anything.
Connecting your PEG tube to the drainage bag
Your PEG tube should be connected to the drainage bag when you eat, drink, feel nauseous, or sleep. It does not have to be connected at other times.
To connect the drainage bag to the PEG tube, take the tube down from the “looped” position. Take the clear plastic cap off the tubing on the bag and twist the end into the PEG tube.
Emptying and cleaning the drainage bag
You will need to empty the bag when it is about ⅓ to ½ full of stomach juices, or about every 8 hours.
If you’re eating soft foods, clean the drainage bag once a day. If you’re not eating, clean the bag every 3 to 4 days. To do this:
- Mix 1 part white vinegar with 3 parts cool water.
- Soak your bag in this solution for 10 to 15 minutes. Let the bag dry.
You may feel nausea or discomfort when the PEG tube is capped (not open to draining) while you clean and dry the bag. If this is the case, attach a second bag.
Eating and drinking with your PEG tube
You can drink clear liquids after your procedure. These include water, ginger ale, apple juice, coffee, tea, broth, flavored ice, and gelatin (Jell-O®).
Sit up when you drink or eat to let the foods or liquids to drain into the bag. Stay sitting up for at least 30 minutes after you eat. If you don’t, you may feel nauseous. If you feel nauseous, check to make sure the tube is not tangled. If it is, untangle it. This should make you feel better. If not, flush your tube. See the section “Flushing your PEG tube” for directions.
When you’re drinking clear liquids without any problems, you can increase your diet to full liquids, if your doctor approves. If you haven’t had any problems after 2 days of full liquids, you can start eating soft or puréed foods. Purée your foods in a blender or food processor. Only follow these steps if you have your doctor’s approval.
Your doctor may approve for you to eat food that isn’t puréed. You must eat it in tiny pieces and chew it very well. Eat very small portions. Don’t eat more than 4 cups of food or drink more than 1 liter (33.8 ounces) of liquids in 24 hours. Each time you eat or drink, you will lose some important nutrients. This is because they drain into the drainage bag with the food or liquid.
Some of what you eat and drink will drain through the tube into the drainage bag. For example, if you eat red gelatin, the drainage in the bag will be red. Stomach juices will drain into the bag even if you have not eaten. The colors will range from green to dark yellow.
Some people will need to have intravenous (IV, given through a vein) liquids when they are at home so they don’t become dehydrated. This may be done through different catheters and ports such as a Broviac or Hickman catheter, a Mediport® or peripherally inserted central catheter (PICC). Your doctor will insert one of these while you’re in the hospital, if you don’t already have one. If you need an IV line, your doctor or nurse will give you more information about it.
Flushing your PEG tube
You will need to flush the tube at least once a day. You or your caregiver should flush the tube once you’re done eating. This is because the tube can get clogged with food. It may also need to be flushed if thick stomach juices or mucus clog it. If you feel nauseous or full and don’t feel better after sitting up, flush your PEG tube.
To flush your tube, follow the instructions below.
-
Gather your supplies
- 60 mL syringe, either one with catheter tip or an ENFit syringe
- 60 mL of normal saline or water (room-temperature or warm, plain tap water) in a cup
- A plastic cap for the tube
- A clean drainage bag
- Paper towels
- Wash your hands with warm water and soap for at least 20 seconds or use an alcohol based hand sanitizer.
- Place the paper towels under the PEG tube to absorb any drainage.
- Draw up 60 mL of water into the syringe.
- Clamp the PEG tube.
- Disconnect the PEG tube from the drainage bag.
- Insert the syringe into the opening of the PEG tube.
- Unclamp the tube and inject the water with a gentle push of the plunger.
- Re-clamp the PEG tube.
- Take out the syringe, reconnect the PEG tube to the drainage bag, unclamp, and allow it to drain.
If the tube is still not draining anything, or if your nausea does not get better, call your nurse or doctor.
Taking medicine with your PEG tube
You can swallow medicine tablets by mouth. You must clamp your tube for at least 30 minutes after you take any medicines.
When to call your healthcare provider
Call your healthcare provider right away if:
- You have chest pain or shortness of breath.
- You have severe abdominal (belly) pain.
- You have diarrhea.
- You have nausea or vomiting.
- You have a fever of 100.4 °F (38 °C) or higher.
- You have any dizziness or weakness.
- You have bleeding that doesn’t stop, such as bright red oozing from your insertion site.
- You have pain at your incision site that doesn’t get better after taking pain medicine.
- You have trouble flushing your PEG tube.
- You have drainage around your insertion site that soaks 5 or more gauze pads per day.
- You have any sign of redness, swelling, or pus around the tube.
- Your PEG tube falls out.
