At MSK, we have a team of experts in chronic lymphocytic leukemia (CLL). This includes doctors, nurses, and pharmacists. These professionals specialize in caring for people with CLL. Our team looks for characteristics in the CLL cells that can help us create the most effective care plan for each individual. We have expertise not only in using currently approved therapies but also in creating the next generation of treatments. We do clinical trials and work with researchers around the world.
Fortunately, many people with CLL do not have major symptoms and do not need treatment for years after the disease is discovered. Our team evaluates each person individually. We discuss when it’s time to consider therapy for CLL as well as come up with a plan to monitor the disease.
Current treatments help with the symptoms of CLL. They work by bringing on remission (when no evidence of cancer is visible) or slowing the disease’s growth. When treatment is needed, MSK doctors will tailor a care plan based on the stage and symptoms of the disease, the genetic and other markers found in the cancer, and other factors, like overall health.
Our team members have expertise and access to currently approved treatments. These include targeted drugs, antibodies, and chemotherapy combinations. We are leaders in CLL research. A number of clinical trials may be available at one of our locations in New York City, New Jersey, and Westchester or on Long Island.
Other treatment options may include:
Radiation Therapy for CLL
Occasionally, MSK doctors may use localized radiation therapy. In this treatment, high-energy rays destroy cancer cells. Radiation can be a used to control the symptoms of CLL in people who have enlarged lymph nodes or an enlarged spleen.
Stem Cell Transplant for CLL
Stem cell transplantation is not needed for the vast majority of people with CLL. Sometimes, though, it is the only potential cure. People who have CLL that has resisted other treatments may need a stem cell transplant.
Learn more about blood and marrow stem cell transplantation.
Investigational Approaches
Our researchers are constantly looking for new ways to treat CLL. These approaches might kill tumor cells directly, stop the body from producing substances that help the cancer grow, or improve the immune response against leukemia cells. See an up-to-date listing of our clinical trials in CLL.
Immunotherapy
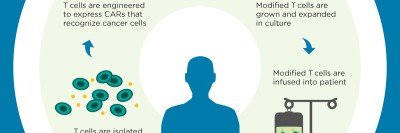
Immunotherapy has produced very encouraging results in people with certain types of leukemia. Our researchers are pioneers in this field. We engineer T cells, a form of white blood cell, that can recognize and attack cancer cells. This is called chimeric antigen receptor (CAR) T cell therapy.
Learn more about how CAR T cell therapy works.
New Therapeutic Drugs
Our researchers have conducted clinical trials to test groundbreaking targeted therapies for CLL. These include ibrutinib (Imbruvica®), venetoclax (Venclexta®), and idelalisib (Zydelig®). These drugs are highly effective in people with CLL that has been resistant to or has come back after standard treatments. The new medications may have fewer side effects than conventional chemotherapy.
Ongoing Care
People with CLL are likely to have regular visits with their doctor, who will monitor the disease and determine if it is growing. These check-ups may include a physical exam, blood tests, bone marrow aspirates, biopsies, and radiographic studies.