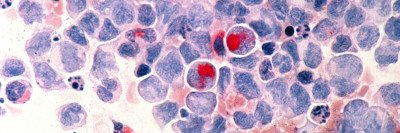
Researchers have found that proteins in the cell called molecular chaperones work together in a communal relationship, much like bees in a hive.
Children on field trips aren’t the only ones who need chaperones. It turns out that chaperones of the molecular sort exist inside our cells, helping to direct and coordinate all kinds of activities that are crucial to life, such as protein folding and assembly.
Because cancer cells are quite disorderly compared with normal cells, they require more chaperones to help manage their activities. Therefore, researchers have long thought that thwarting these chaperones might be an effective way to shut down cancer cells.
This approach is beginning to be studied in patients in the clinic, and researchers are already looking at ways to make these chaperone-blocking drugs even more effective.
“We know that chaperones play an important role in how cancer cells function, but when we dismantle one of the key chaperones, the cancer cell doesn’t always die as expected,” says Memorial Sloan Kettering researcher Gabriela Chiosis, the co-senior author of a study recently published in Nature.
“We decided to look systematically at those cancer cells that die and those that don’t when they have their chaperones targeted and determine what the differences are,” she says.
A “Shocking” Discovery
The molecular chaperone in the study, called heat shock protein 90 (Hsp90), is the most abundant chaperone in cancer cells. It’s known to stabilize the proteins inside cells that are required for tumor growth. For several years, Dr. Chiosis and her colleagues have been developing a drug called PU-H71, which they designed to block the action of Hsp90 and disrupt cancer cells’ ability to grow.
In their latest research, they and co-senior author Monica Guzman of Weill Cornell Medical College probed cancer cells representing two types of patients. They compared tumor cells from those who respond to PU-H71 with those who don’t, looking for differences in chaperone activity.
What they found was something that had never been seen before: In the cells that were effectively killed by PU-H71, the chaperones worked together in a communal relationship, much like bees in a hive. They named this network of chaperones the “epichaperome.”
“Communal behavior is often seen in nature at the level of the whole organism, for example ants and bees who work together in colonies and their cooperative behavior determines the survival of the entire group,” Dr. Chiosis notes. “In the same way, individual chaperones form communal entities in aggressive cancers. The patterns found in nature are repeated at the cellular level.”
Weaker Together, Stronger Apart?
“When we looked further, we discovered that it was this communal relationship that made cancer cells vulnerable to Hsp90 inhibitors,” Dr. Chiosis says. “When one piece of the highly connected communal network was knocked out by a drug, a chain reaction led the entire network to fall apart, and cell death ensued.”
In contrast, in cancer cells in which PU-H71 was ineffective, the chaperones acted in a solitary fashion. Taking down one of them — Hsp90 — was not enough to stop tumor growth because the other chaperones continued to function, protecting the cell from destruction.
Further investigations revealed that a gene called MYC, which was already known to be one of the most common cancer-driving genes, caused the molecular chaperones to form networks and ultimately made them easier to target.
Taking the Findings to the Clinic
Based on their discoveries, the investigators are now working on better ways to predict which patients will respond to Hsp90-inhibiting drugs and which won’t. They are also using their findings about what causes cells to create the epichaperome to design new drugs and drug combinations that they think will be more effective.
“Of course we are not going to activate MYC, but we can look for other ways to stress the cells in a way that will make the chaperones band together,” Dr. Chiosis explains. The team is currently developing a clinical trial for breast cancer based on this approach.
Dr. Chiosis notes that this kind of research highlights MSK’s expertise in looking at medical problems from many different angles. “A multidisciplinary effort is required to address these kinds of complex problems,” she says. “Many of us are putting our brains together to advance these types of studies.” Co-authors on the paper included medical oncologists John Gerecitano and Shanu Modi, pathologist Adriana Corben, radiochemists Jason Lewis and Naga Vara Kishore Pillarsetty, and radiologists Mark Dunphy and Steven Larson.