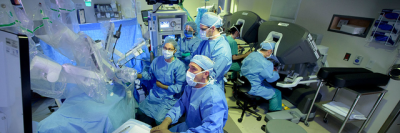
Radical prostatectomy is surgery to remove the prostate gland.
In this operation, our surgeons remove the entire prostate, some tissue surrounding the gland, and the seminal vesicles (small glands that help produce semen). In some cases, we also remove a number of nearby lymph nodes at the same time.
A critical aspect of surgery is our ability to tailor to the individual features of each patient’s cancer. One size does not fit all: This means the exact same procedure is not appropriate for every patient.
The location, size, and other features of your cancer will be considered to design an operation that is appropriate for your individual tumor. If you choose surgery, we will do a thorough review of the biopsy material and magnetic resonance imaging (MRI) so that we can better understand the likelihood that your cancer is contained within the prostate. Our surgeons work with our pathology and radiology colleagues to provide a more personalized approach to treatment.
Inspecting the lymph nodes can be an important step. It helps us determine whether your cancer has spread beyond the prostate and whether you should consider radiation therapy or systemic therapy (such as chemotherapy, hormone therapy, biologic therapy, or immunotherapy) following surgery. We are studying ways to better determine which men actually need lymph nodes removed during radical prostatectomy.
Surgery to remove the prostate may be an option for you if:
- You’re newly diagnosed with early-stage, localized prostate cancer; active surveillance is not an appropriate approach for you; and you have a long life expectancy. For men in this situation, radical prostatectomy alone can often eliminate the cancer.
- You have a rising prostate-specific antigen (PSA) level after initial treatment with focal therapy, indicating that the cancer wasn’t completely eliminated.
- You have a more advanced tumor that could safely be removed with surgery. In this situation, we often combine surgery to remove the prostate with other treatments.
If your cancer returns after you’ve received radiation therapy, you may undergo a type of surgery called salvage radical prostatectomy.
The prostate is surrounded by nerves and structures that are important to your ability to have normal urinary and sexual function. We take extreme care to minimize injury that can lead to side effects, such as incontinence (the inability to hold in urine) and erectile dysfunction. Learn more about how experts at MSK help minimize side effects from prostate cancer surgery and can help you manage them.
The good news is that over the past few decades, technical refinements have dramatically reduced the number of complications with this surgery. For example, we’ve developed techniques to incorporate the results of imaging tests into our surgical planning, enabling us to avoid injuring important structures, minimize the risk of incontinence, and maximize the chance of maintaining sexual function.
Although results for individual patients vary, studies have shown that surgeons who regularly perform radical prostatectomies have fewer complications on average than those who do these surgeries less often. Our surgeons are among the nation’s most experienced in conducting prostate operations, and we’re continually working to improve the safety and effectiveness of procedures through our clinical trials.
MSK’s Approach to Radical Prostatectomy
Our prostate surgery team includes experts in several techniques, including robot-assisted surgery, open surgery, and laparoscopic surgery. Regardless of which surgical approach you choose, our goal is to remove your cancer completely and preserve normal urinary and sexual function.
With all surgical approaches, we’ve developed and use innovative techniques to preserve the tiny nerves and blood vessels attached to the prostate that help control erections. These and other advances have made some of the complications of prostate cancer surgery less common and more manageable and can spare nerves from damage. We’ll work closely with you and your medical team to manage any short- or long-term side effects you may experience.
Ultimately, you’ll help determine which approach your surgeon takes.
Minimally Invasive Surgical Options
In minimally invasive surgical procedures, we make several small incisions in your abdomen. We then insert a tiny, lighted telescopic camera called a laparoscope, along with specially designed surgical instruments that a surgeon uses to perform the operation.
When you have minimally invasive surgery, you’re likely to have less discomfort after the procedure and more likely to recover faster than with a traditional open surgery, in which incisions are larger and more extensive. Many men who have their prostates removed in a minimally invasive operation are able to return home the following day.
We offer two types of minimally invasive surgery.
Many of our surgeons perform robot-assisted laparoscopic prostatectomy. This sophisticated tool offers much finer precision than any other surgical technique.
Using a device called the da Vinci® Surgical System, a surgeon performs the operation while seated at a console that has a viewing screen as well as hand, finger, and foot controls. The screen projects a three-dimensional image, magnified tenfold, of the prostate and the surrounding area. This allows the surgeon to view the surgical site in great detail. The robot then translates the surgeon’s hand, wrist, and finger movements into real-time movements of the instruments inside the patient.
In laparoscopic radical prostatectomy, a surgeon inserts a laparoscope through a small incision in the abdomen. The camera projects a magnified, high-definition image of the surgical area on a screen. Using the projected image as a guide, the surgeon removes the prostate, seminal vesicles, and lymph nodes with specialized surgical instruments.
Some men with localized prostate cancer choose radiation therapy for their initial treatment. However, a rising PSA level and a positive prostate biopsy after radiation therapy may indicate that your cancer hasn’t been completely eliminated or that it has returned.
Our surgeons are the world’s most experienced in performing a procedure called salvage radical prostatectomy, which we do following radiation therapy. This procedure destroys the disease in a high proportion of men when the cancer is confined to the prostate or the tissues immediately surrounding it, and has been shown to eliminate prostate cancer for ten years or more.
Salvage radical prostatectomy can be more difficult to perform than a radical prostatectomy that is done when the cancer is first diagnosed, before radiation therapy has been given. This is because of the effects of radiation on the prostate gland. Many hospitals do not offer this procedure because of its many technical challenges.
As an alternative to surgery, we are investigating using focal therapy or radiation treatment (MSK PreciseTM) instead of surgery to treat only the areas within the prostate gland where the cancer has returned.