This information will help you check if your medicines or dietary supplements have aspirin, other NSAIDs, vitamin E, or fish oil as an active ingredient. NSAID stands for nonsteroidal anti-inflammatory drug.
It’s important to stop taking these medicines and supplements before many cancer treatments. They affect your platelets (blood cells that clot to prevent bleeding) and can raise your risk of bleeding.
Other dietary supplements, such as vitamins and herbal remedies, can also affect your cancer treatment. Read Herbal Remedies and Cancer Treatment to learn more.
A prescription medicine is one you can only get with a prescription from your healthcare provider. An over-the-counter medicine is one you can buy without a prescription.
What is an active ingredient?
An active ingredient is the part of a medicine or supplement that makes it work. Some medicines and supplements have just one active ingredient. Others have more. For example:
- Ibuprofen is the active ingredient in Advil® and Motrin®. Ibuprofen is an NSAID.
- Naproxen is the active ingredient in Aleve®. Naproxen is an NSAID.
- Acetaminophen is the active ingredient in Tylenol®.
- Aspirin, acetaminophen, and caffeine are the active ingredients in Excedrin®.
Generic medicines sometimes use their active ingredient as their name. But people often call medicines and supplements by a brand name, even if they’re generic. This can make it hard to know their active ingredients.
How to find a medicine or supplement’s active ingredients
You can always find the active ingredients by reading the label.
Over-the-counter medicines

Over-the-counter medicines list their active ingredients in the “Drug Facts” label (see Figure 1). Active ingredients are always the first thing on the Drug Facts label.
Prescription medicines

Prescription medicines list their active ingredients on the label. Their active ingredients and their generic name are the same thing.
Labels often look different depending on which pharmacy you use. Here’s an example of where to find a medicine’s active ingredients (generic name) on a label from MSK’s pharmacy (see Figure 2).
Dietary supplements
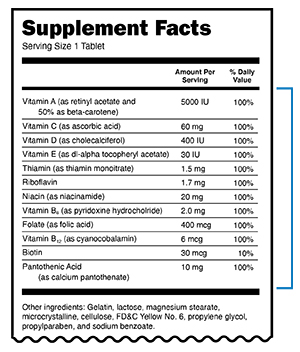
Dietary supplements list their active ingredients in the “Supplement Facts” label (see Figure 3). The active ingredients always have an amount per serving and % daily value included.
Active ingredients to look for
If your medicine or supplement has any of these active ingredients, you may need to stop taking it before, during, or after your cancer treatment or surgery. Follow your care team’s instructions.
| Active ingredients to look for | ||
|---|---|---|
|
|
|
* The full name acetaminophen isn’t always written out. Look for the common abbreviations listed below, especially on prescription pain relievers.
| Common abbreviations for acetaminophen | ||
|---|---|---|
|
|
|
About acetaminophen (Tylenol)
In general, acetaminophen is safe to take during cancer treatment. It doesn’t affect platelets. That means it will not raise your chance of bleeding. If you’re getting chemotherapy, talk with your healthcare provider before taking acetaminophen.
There is a limit to how much acetaminophen you can take in a day. Always follow the instructions from your care team or on the medicine’s label.
Acetaminophen is in many different prescription and over-the-counter medicines. It’s possible to take too much without knowing. Always read the label on the medicines you take. Do not take more than 1 medicine that has acetaminophen at a time without talking with a member of your care team.
Instructions before your cancer treatment
Tell your healthcare provider if you take aspirin, other NSAIDs, vitamin E, or fish oil. They’ll tell you if you need to stop taking it. You’ll also find instructions in the information about your treatment.
Before your surgery
Follow these instructions if you’re having surgery or a surgical procedure. If your healthcare provider gives you other instructions, follow those instead.
- If you take aspirin or a medicine that has aspirin, you may need to change your dose or stop taking it 7 days before your surgery. Follow your healthcare provider’s instructions. Do not stop taking aspirin unless your healthcare provider tells you to.
- If you take vitamin E, fish oil, or a supplement that has vitamin E or fish oil, stop taking it 7 days before your surgery or as directed by your healthcare provider.
- If you take an NSAID or a medicine that has an NSAID, stop taking it 48 hours (2 days) before your surgery or as directed by your healthcare provider.
Before your radiology procedure
Follow these instructions if you’re having a radiology procedure (including Interventional Radiology, Interventional Mammography, Breast Imaging, and General Radiology). If your healthcare provider gives you other instructions, follow those instead.
- If you take aspirin or a medicine that has aspirin, you may need to stop taking it 5 days before your procedure. Follow your healthcare provider’s instructions. Do not stop taking aspirin unless your healthcare provider tells you to.
- If you take an NSAID or a medicine that has an NSAID, you may need to stop taking it 24 hours (1 day) before your procedure. Follow your healthcare provider’s instructions.
Before and during your chemotherapy
Chemotherapy can lower your platelet count, which can increase your risk of bleeding. No matter if you’re just starting chemotherapy or have been getting it, talk with your healthcare provider before taking aspirin, other NSAIDs, vitamin E, or fish oil.
Learn about our Health Information Policy.
