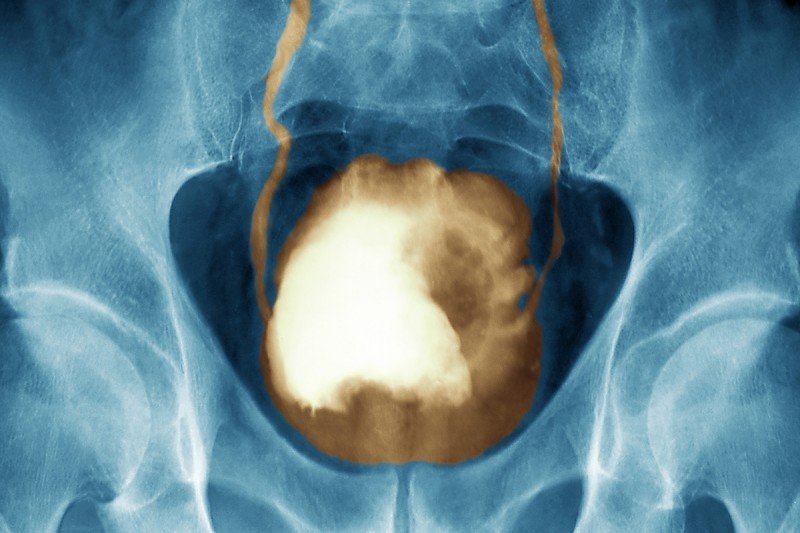
MSK is investigating ways to treat muscle-invasive bladder cancer without removing the bladder.
-
Bladder removal (radical cystectomy) is an effective treatment option for muscle-invasive bladder cancer but still a major operation.
-
MSK is taking a leading role in helping more people with bladder cancer keep their bladder without affecting survival rates.
- A new approach involves testing for DDR genetic mutations in bladder tumors to predict the effectiveness of chemotherapy.
Muscle-invasive bladder cancer (MIBC) can be treated very effectively with surgery. MSK oncologists and surgeons consider many factors to choose the best treatment plan, including the specifics of each person’s cancer, as well as the patient’s health and treatment goals. This helps determine the extent and type of surgery.
What Is the Standard Treatment for Muscle-Invasive Bladder Cancer?
For people with a bladder tumor that has invaded the muscle of the bladder wall (stage 2) or even spread through the wall to surrounding muscle and tissue (stage 3), the standard treatment is chemotherapy to shrink the tumor followed by a radical cystectomy. The operation removes the entire bladder as well as nearby lymph nodes and organs that may contain cancer. The procedure can be done either as open surgery or with minimally invasive methods.
While a radical cystectomy often provides the best chance of a cure, bladder removal is nonetheless a major operation. MSK is taking a leading role in studying approaches that allow more people with muscle-invasive cancer to preserve their bladder. The key is carefully selecting those who will respond well to other treatments.
“We have the expertise in pathology, radiology, oncology, and surgery to choose people who will have a lower risk of their cancer returning,” says MSK urologic surgeon Bernard Bochner, MD.
How MSK Can Help People With MIBC Avoid Bladder Removal
One way to select patients is by looking at the genes of the bladder tumors. Researchers at MSK and elsewhere noticed that people whose tumors have genetic changes called DNA-damage response (DDR) mutations respond especially well to chemotherapy given before surgery.
These patients did so well, in fact, that during the radical cystectomy that followed, little to no tumor was found. This suggests that the chemotherapy destroyed most, if not all, of the cancer in the bladder. Furthermore, this group of people also had a very low risk of their cancer ever coming back.
Weak Spot: DNA-Damage Response Genetic Mutations
Cells with DDR mutations are unable to repair the DNA damage caused by chemotherapy. About 20% of bladder cancers have DDR mutations. These tumor cells may be particularly sensitive to chemotherapy — so sensitive that no surgery is needed.
“Using this genetic information, we could potentially save patients a major surgery and manage their bladder cancer with chemotherapy alone,” MSK medical oncologist Gopa Iyer, MD, explains. “That would be of dramatic benefit and a major shift in the way we approach the treatment of these people.”
Clinical Trial Testing Bladder Preservation in People With DDR Genetic Mutations
Dr. Iyer is leading a phase 2 clinical trial testing bladder preservation in people whose muscle-invasive bladder cancer contains DDR genetic mutations. It is funded by the National Cancer Institute and involves numerous sites around the United States. (The trial is currently enrolling patients. Learn more.)
An important factor in the trial is analysis of patients’ tumors with MSK-IMPACT®, a genetic-sequencing test developed at MSK. All participants, regardless of where they are being treated, submit a sample for MSK-IMPACT testing for the DDR gene mutation. While waiting for the results, the patients receive 12 weeks of chemotherapy.
After the chemotherapy concludes, patients found to have certain DDR mutations are examined by cystoscopy to make sure no invasive disease remains. People with no invasive disease will be able to choose to keep their bladders. They will then be closely monitored with cystoscopies and radiology scans every few months.
People who do not have a DDR mutation or who have invasive cancer remaining after chemotherapy will have a cystectomy or radiation.
The trial will provide valuable information about other genes that predict sensitivity or resistance to chemotherapy. Not everyone who responds well to chemotherapy has a DDR gene mutation, so other mutations are likely involved.
“We are hopeful this trial will prove that more bladder cancer patients can receive less intensive treatment with good outcomes,” Dr. Bochner says.
Good Recovery After Bladder Removal at MSK
Even when bladder removal is necessary, MSK has the expertise to produce good outcomes for patients. Several techniques are available to reconstruct the urinary system if the bladder has been removed. This includes formation of a new bladder (neobladder) created from part of the small intestine. Other times, a diversion through an opening to a pouch worn outside the body may be best.
A recent study shows that most patients receiving radical cystectomy at MSK return to their previous quality of life after they recover. Most people said they were essentially back to normal within three months.
“MSK does a very high number of these procedures, and our doctors are experts at providing excellent outcomes over the long term,” Dr. Bochner says. “While we often are able to preserve the bladder, even patients who do receive radical cystectomy at MSK should feel confident they will be able to recover and adjust well.”





