This information answers common questions about lymphedema that’s related to breast cancer.
What is lymphedema?
Lymphedema is swelling that develops when the lymph vessels in an area of your body are no longer able to carry all the lymph fluid away from that area. When that happens, the lymph fluid can build up and cause swelling.
Lymphedema can develop in your arm, hand, fingers, breast, or torso on your affected side (the side where your lymph nodes were removed).
What’s my risk of developing lymphedema?
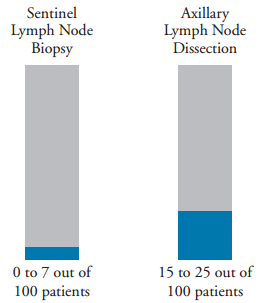
Your risk of developing lymphedema depends on how your lymph nodes were removed (see Figure 1). There are 2 types of surgeries used to remove lymph nodes: a sentinel lymph node biopsy and an axillary lymph node dissection.
During a sentinel lymph node biopsy, between 1 and a few lymph nodes are removed from your armpit and checked for cancer cells. The risk of developing lymphedema after a sentinel lymph node biopsy is low. About 0 to 7 out of every 100 people who have a sentinel lymph node biopsy may develop lymphedema.
During an axillary lymph node dissection, more than a few lymph nodes are removed from your armpit. This is done to remove additional lymph nodes that may have cancer cells. The risk of developing lymphedema is higher after an axillary lymph node dissection than it is after a sentinel lymph node biopsy. About 15 to 25 out of every 100 people who have an axillary lymph node dissection may develop lymphedema.
Damage to your lymphatic system can also increase your risk of developing lymphedema. The following things can damage your lymphatic system:
- Radiation therapy to your affected armpit
- An infection or severe injury (such as a serious burn) in your affected arm, hand, fingers, or breast after surgery
- Tumor growth in or near your armpit on your affected side
- Being overweight when you’re diagnosed with breast cancer
- Gaining or losing more than 10 pounds (4.5 kilograms) per month after your surgery
There’s no way to know for sure who will develop lymphedema.
What can I do to help lower my risk of developing lymphedema?
Doing the following things may help lower your risk of developing lymphedema.
- Stay at or safely work towards a healthy body weight.
- Use your unaffected arm or both arms to carry heavy packages until you get your strength back on your affected side.
-
Exercise and stretch your muscles regularly. Talk with your doctor or nurse about which exercises are right for you.
- When you resume exercise and activity, make sure to build up slowly and gradually. If you feel discomfort, stop and take a break. Exercise shouldn’t cause pain.
-
If you get a cut or scratch on your affected arm or hand:
- Clean the area with soap and water.
- Apply antibacterial ointment, such as Bacitracin® or Neosporin®.
- Cover the area with a bandage, such as a Band-Aid®.
-
If you get a burn on your affected arm or hand:
- Apply a cold pack to the area or run the area under cool tap water for about 10 minutes.
- Clean the area with soap and water.
- Cover the area with a bandage, such as a Band-Aid.
- If you notice any signs of infection (such as redness, swelling, skin that’s warmer than usual, or tenderness), call your healthcare provider.
If you had an axillary lymph node dissection:
-
Ask your healthcare providers to use your unaffected arm for blood draws, injections (shots), intravenous (IV) lines, and blood pressure measurements.
- In some situations, if blood can’t be drawn from your unaffected arm, it’s OK to use your affected arm. Your healthcare provider can discuss this with you.
- If an injection can’t be given in your unaffected arm, buttocks, thigh, or abdomen (belly), it’s OK to get it in your affected arm.
- If your blood pressure can’t be measured using your unaffected arm, it’s OK to use your affected arm.
- If lymph nodes were removed on both sides of your body, talk with your healthcare provider about which arm is safest to use.
- Be careful not to get sunburned. Use sunblock with an SPF of at least 30. Reapply it often.
- Use insect repellent to avoid stings and bug bites.
- Use a lotion or cream daily to help protect the skin on your affected arm and hand.
- Don’t cut your cuticles on your affected hand. Instead, push them back gently with a cuticle stick.
- Wear protective gloves when doing yard work or gardening, washing dishes, or cleaning with harsh detergents or steel wool.
- Wear a thimble when you’re sewing.
- Be careful if you shave under your affected arm. Think about using an electric razor. If you get a cut while shaving, take care of it following the instructions above.
- Don’t use heating pads or hot packs on your affected arm, shoulder, or torso.
- Don’t wear tight or heavy jewelry or clothing that has tight elastic and leaves a mark. These things can lead to swelling.
If you had a sentinel lymph node biopsy:
- It’s OK to use your affected arm for blood draws, injections, IV lines, and blood pressure measurements. But, ask your healthcare providers to try to use your unaffected arm if it’s available.
- If you start to notice any signs of lymphedema, always use your unaffected arm. If this isn’t possible, talk with your healthcare provider about which arm is safest to use.
How long does it take for lymphedema to develop?
Lymphedema can develop soon after surgery or months or years later.
Some mild swelling after surgery is normal. This swelling may last for up to 6 weeks. It’s often temporary and will gradually go away.
What are the signs of lymphedema?
- A feeling of heaviness, aching, or pain
- A tight feeling in your skin
- Less flexibility
- Swelling
- Skin changes, such as tightness or pitting (skin that stays indented after pressing on it)
If you have swelling, you may notice that:
- The veins in your affected hand are less noticeable than on your other hand.
- The rings on your affected finger(s) are tighter or don’t fit.
- The shirt sleeve on your affected side feels tighter than usual.
What should I do if I think I have lymphedema?
Call your healthcare provider if you notice any signs of lymphedema.
What’s the treatment for lymphedema?
Treatment for lymphedema can be simple or intensive. An occupational or physical therapist who specializes in lymphedema can help choose the best program for you.
Treatment has 4 main parts:
- Skin care. The suggestions listed earlier are examples of ways you can take care of your skin.
- Compression. Compression helps move lymph fluid out of the swollen area. Compression options include elastic (stretchy) garments, short-stretch compression bandages, and other inelastic (not stretchy) compression garments that are often used at night. Your lymphedema therapist will talk with you about the best option(s) for you.
- Exercise. An exercise program can help you manage your swelling. It’s important to slowly progress through your program so your muscles get used to it gradually.
- Manual lymphatic drainage (MLD). MLD is a gentle form of massage for your lymphatic system that may help move lymph fluid out of the swollen area. If you have questions about MLD or massage, talk with your lymphedema therapist.
Are there any medications I can take to reduce the swelling?
No. There are no approved medications to manage lymphedema.
Will the swelling go away?
The swelling might stay mild and stable, or it might slowly increase over time. Taking part in a treatment program to manage the swelling will help keep it under control.
When is it safe to start doing my usual activities and exercise?
You can go back to doing your usual activities slowly and gradually. Your lymphedema therapist might recommend that you wear a compression garment or bandage.
We encourage you to keep doing all the activities you enjoy. Talk with your healthcare provider or lymphedema therapist if you have questions about your daily activities or lymphedema.
Support Services
National Lymphedema Network
The National Lymphedema Network provides educational materials and community referrals.
www.lymphnet.org
415-908-3681
American Cancer Society (ACS)
The ACS provides information about the diagnosis and treatment of lymphedema.
www.cancer.org
800-227-2345
National Cancer Institute (NCI)
The NCI provides information about the diagnosis and treatment of lymphedema.
www.cancer.gov
800-4-CANCER (800-422-6237)
Step Up, Speak Out
Step Up, Speak Out provides resources and educational materials about lymphedema.
www.stepup-speakout.org
Learn about our Health Information Policy.
