This information explains how to use lidocaine (LY-doh-kane) in your nebulizer machine to help relieve your cough. Lidocaine is a local anesthetic (medication that numbs an area of your body).
Nebulized 2% preservative-free lidocaine HCl solution may help manage your cough when other medications don’t help. Follow your healthcare provider’s instructions closely when using nebulized lidocaine.
Your healthcare provider will tell you to use nebulized albuterol (al-BYOO-ter-ahl) before using nebulized lidocaine. Don’t use any other medications before or with nebulized lidocaine unless your healthcare provider tells you to.
Getting Your Supplies
Your healthcare provider will give you a prescription for 2% preservative-free lidocaine HCl solution, sterile syringes, and blunt needles. Pick up these supplies from the pharmacy at Memorial Sloan Kettering (MSK).
Store the lidocaine solution at room temperature away from sunlight. Room temperature is 68 °F to 77 °F (20 °C to 25 °C).
Instructions
-
Gather your supplies (see Figure 1). Put them on a clean, flat surface, such as your kitchen table. You’ll need:
- A 5 milliliter (mL) vial of 2% preservative-free lidocaine HCl solution.
- An alcohol wipe.
- A sterile syringe.
- A blunt needle.
- An empty plastic container with a screw-top lid, such as a laundry detergent bottle. Label it “Home Sharps – Not for Recycling.” You’ll put the used needle and syringe in this container. For more information, read the resource How To Store and Get Rid of Your Home Medical Sharps.
- Your nebulizer.
- Eye goggles that seal to your face, such as swimming or safety goggles.
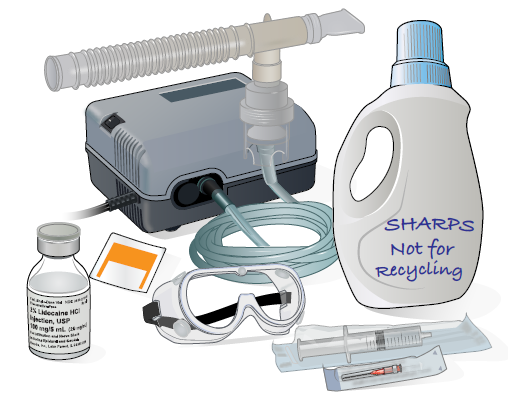
Figure 1. Your supplies -
Make sure the lidocaine solution is safe to use.
- Compare the name and strength on the medication’s label to the name and strength on your prescription. If they’re different, don’t use the medication.
- Check the expiration date on the medication’s label. If the expiration date has passed, don’t use the medication.
-
Look at the medication inside the vial. It should be a clear, colorless liquid with no solid particles (pieces). Don’t use the medication if:
- The liquid is cloudy.
- The liquid has any color.
- There’s anything solid in the liquid.
- The vial is leaking.
- Set up your nebulizer. Follow the instructions in the video Using Your Jet Nebulizer.
-
Clean your hands.
- If you’re washing your hands with soap and water, wet your hands with warm water and apply soap. Rub your hands together for at least 20 seconds, then rinse. Dry your hands with a paper towel. Use that same towel to turn off the faucet.
- If you’re using an alcohol-based hand sanitizer, be sure to cover all parts of your hands with it. Rub your hands together until they’re dry.
-
Take the cap off the vial (see Figure 2). You’ll see a rubber stopper underneath.
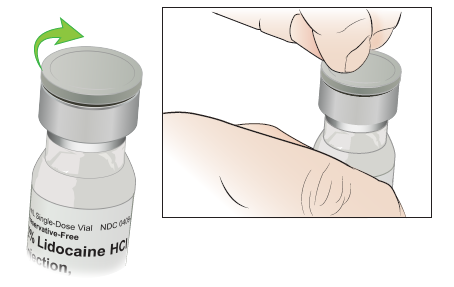
Figure 2. Take the cap off the vial -
Clean the top of the vial with an alcohol wipe for 15 to 30 seconds (see Figure 3). Let it dry.
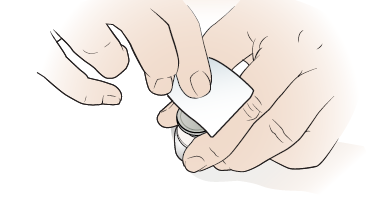
Figure 3. Clean the top of the vial - Take the needle and syringe out of their packaging. Screw the needle onto the syringe. Take the cover off the needle and throw it away.
- Put the needle into the middle of the rubber stopper. Make sure the needle tip is in the liquid.
-
Gently pull the plunger up to draw the medication into the syringe (see Figure 4). Draw up all the medication in the vial.

Figure 4. Draw the lidocaine solution into the syringe - Once all the medication is in the syringe, pull the needle straight up out of the vial.
-
Check the syringe for air bubbles. If you see any:
- Hold the syringe with the needle pointing up.
- Gently tap the side of the syringe with your fingers until the air bubbles rise to the top near the needle (see Figure 5).
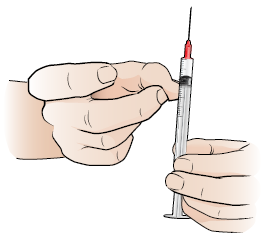
Figure 5. Tap the side of the syringe - Slowly push the plunger up to push the air bubbles out of the syringe. Be careful not to push out any medication.
-
Squirt the medication from the syringe into the small nebulizer cup (see Figure 6). Don’t put any other medication in the cup with the lidocaine solution. Put the needle, syringe, and vial into your plastic sharps container.
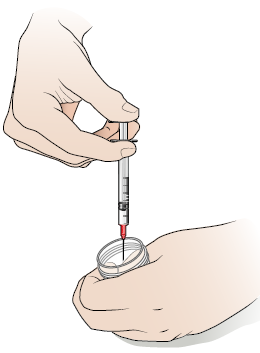
Figure 6. Squirt the medication into the nebulizer cup -
Attach the cap to your nebulizer. Use your nebulizer following the instructions in the video Using Your Jet Nebulizer.
- It’s best to wear eye goggles when you use nebulized lidocaine. The goggles will keep the mist from getting in your eyes.
Keep the plastic container with your used needles in a safe place. Follow the instructions in the resource How To Store and Get Rid of Your Home Medical Sharps.
After Using Nebulized Lidocaine
Nebulized lidocaine can make your lips, tongue, mouth, and throat numb. To lower your risk of choking or biting your tongue:
- Don’t eat or drink for at least 1 hour after using nebulized lidocaine. This includes gum and hard candies. You can start eating and drinking again once the numbness has worn off and you can swallow as usual.
- Sit upright for at least 1 hour after using nebulized lidocaine. You can lie down once the numbness has worn off and you can swallow as usual.
It’s normal to have a bitter taste in your mouth after using nebulized lidocaine.
Things to Do While You’re Using Nebulized Lidocaine
Tell your healthcare providers you use nebulized 2% lidocaine HCl solution. This includes your doctors, nurses, pharmacists, and dentists.
Medications like lidocaine can cause a blood problem called methemoglobinemia (meth-EME-moh-gloh-bih-NEE-mee-uh). Your risk of getting methemoglobinemia may be higher if you have glucose-6-phosphate dehydrogenase (G6PD) deficiency, heart problems, or lung problems.
Tell your healthcare provider if you’ve ever had methemoglobinemia.
When to Call Your Healthcare Provider
Call your healthcare provider if:
- You have more trouble breathing than usual
- You have chest pain or pressure
- Your heartbeat is irregular, faster, or slower than usual
- You have trouble swallowing or speaking
-
You have any signs of an allergic reaction, such as:
- A rash, hives (itchy, raised bumps on your skin), or itching
- Red, swollen, blistered, or peeling skin
- Wheezing
- Tightness in your chest or throat
- An unusually hoarse (low, raspy) voice
- Swelling in your mouth, face, lips, tongue, or throat
-
You have any signs of a lidocaine overdose, such as:
- Numbness or tingling around or in your mouth that doesn’t get better
- Mental status changes, such as confusion, anxiety, irritability, or agitation
- Tinnitus (ringing in your ears)
- Muscle twitching and seizures
- Breathing more slowly than usual
- Nausea (feeling like you’re going to throw up) or vomiting (throwing up)
- Blue lips and fingers
- Higher or lower blood pressure than usual
- Feeling very sleepy
-
You have signs of methemoglobinemia, such as:
- Blue or gray lips, nails, or skin
- Seizures
- Feeling very dizzy or passing out
- A very bad headache
- Fatigue (feeling very tired or having less energy than usual)
Learn about our Health Information Policy.