Since the mid-1980s, mammography has been the primary screening modality for breast cancer. While it has reduced mortality rates, there are some notable drawbacks. Mammography fails to detect as many as 30 percent of cancers because overlying normal breast tissue obscures them from view. Further, 10 percent of women are asked to return after their initial mammogram for additional imaging to evaluate possible abnormalities, most of which turn out to be normal.
Currently, the most sensitive imaging modality available for detecting breast cancer is full breast magnetic resonance imaging (MRI), a vascular-based test. Compared with mammography, which detects approximately five cancers per 1,000 women screened, MRI can find ten to 15 additional cancers in women with a negative mammogram. The use of MRI has been restricted to a very small subset of women at very high risk for breast cancer since it costs several thousand dollars.
Two powerful new screening tools in our fight against breast cancer are in development that take advantage of the fact that breast cancers often have increased vascularity: contrast-enhanced digital mammography (CEDM) and abbreviated breast MRI (AB-MRI).
Contrast-Enhanced Digital Mammography Detects More Cancers
With CEDM, the patient receives iodine contrast through an IV line and then is positioned and compressed in the usual manner. Early studies show that CEDM detects more breast cancers than standard mammography. The detection rate with CEDM is comparable to breast MRI; however, CEDM is far less expensive, about the same as a standard digital mammogram, so many more women can benefit from a vascular-based screening test. CEDM also appears to produce fewer false-positive readings than standard mammography. See Figure 1.
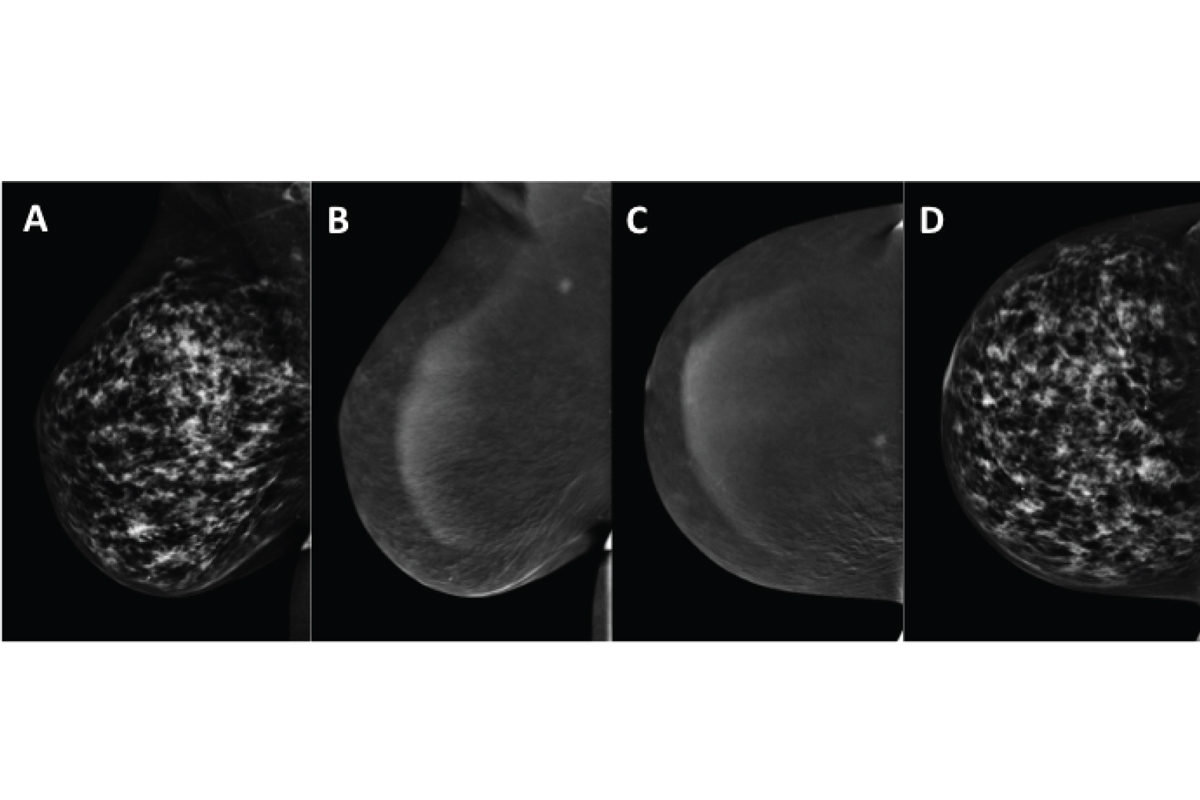
Memorial Sloan Kettering Cancer Center (MSK) is the first institution to explore the potential of CEDM to screen women for breast cancer; we have performed approximately 1,000 CEDMs since 2012. Patients tolerate the iodine-based contrast agent well; we have seen very few adverse reactions. We currently have an open trial comparing the clinical utility of CEDM and whole breast screening ultrasound. This trial is open to women 30 years of age and older who are scheduled for a screening mammogram and breast ultrasound and who have not had a breast MRI within the past 12 months. Women with a history of breast conservation are eligible if their lumpectomy took place at least 18 months prior.
Optional clinical CEDMs may also be scheduled for intermediate-risk women who do not qualify for a breast MRI. However, we strongly encourage women to enroll in the CEDM screening trial until its role as an alternative technique is firmly established. In a second trial, we are evaluating the use of CEDM in women with a palpable breast mass. MSK physicians may schedule clinical CEDMs through the Cancer Information Service (CIS). Other physicians may call 646-888-5499 to schedule. To enroll a patient in one of the CEDM research trials, please call 646-888-4857.
Abbreviated Breast MRI: A Faster, Less Costly Option
AB-MRI is another exciting, vascular-based imaging method that may change the way we screen women for breast cancer. Although a regular MRI is the most sensitive test for breast cancer, it takes approximately 30 to 45 minutes to complete, contributing to its high cost. In an AB-MRI, imaging includes only the most useful series and takes less than ten minutes to complete. Early studies have found that the accuracy is similar to a full standard MRI protocol. By reducing the number of images obtained, the cost of an abbreviated breast AB-MRI can be reduced from several thousand dollars to a few hundred, so more women can be screened. AB-MRI uses a gadolinium-based contrast agent, rather than the iodine-based agent used in CEDM.
We will soon open a new clinical trial comparing AB-MRI to digital breast tomosynthesis, a 3-D imaging approach already embraced by MSK and adopted by more than half of imaging centers nationwide. The technique generates thin slices through the breast so that cancers are less likely to be obscured by overlying tissue. Studies indicate that digital breast tomosynthesis is 30 percent more accurate in finding early breast changes than digital mammography and significantly reduces the number of false-positives.
Breast cancer continues to be the second leading cause of cancer death in women in the United States. New modalities such as CEDM and AB-MRI are major advances in breast cancer screening techniques. Future studies will continue to provide insight on how new diagnostic techniques compare to current practice and help determine how often we should perform vascular screening.