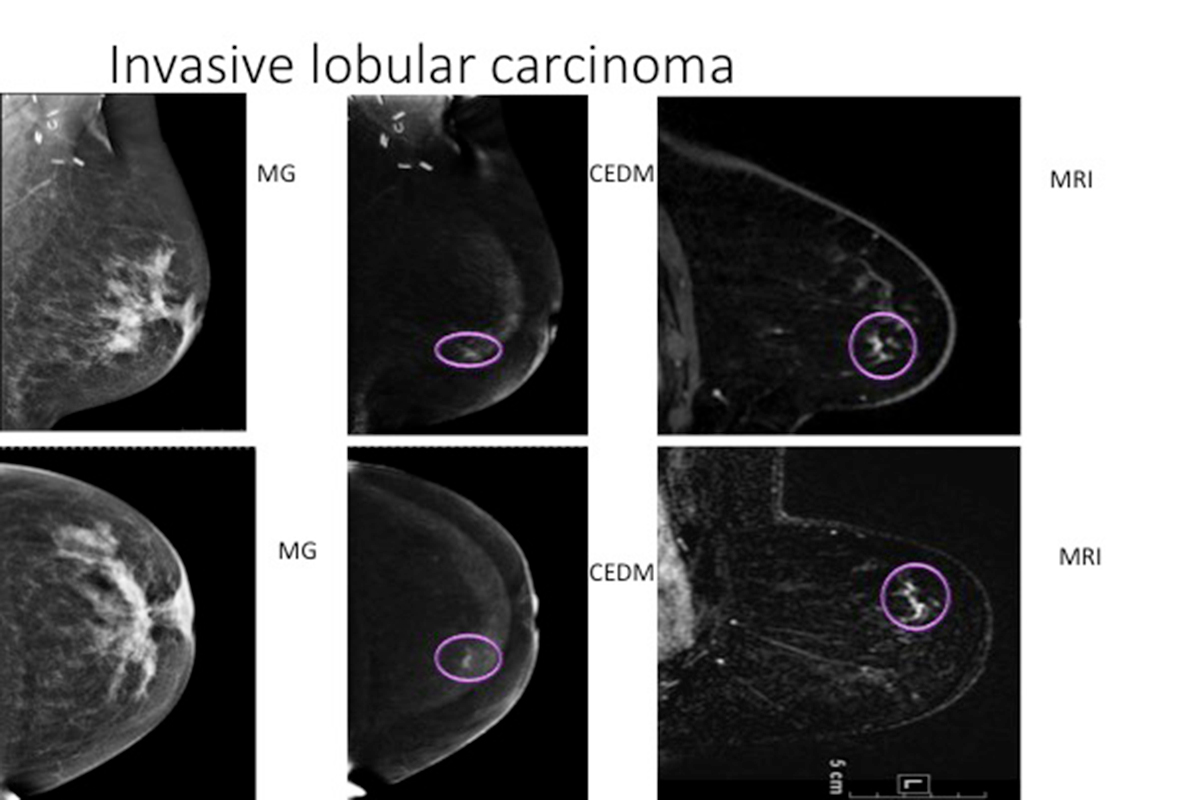

Recent research from Memorial Sloan Kettering shows that dual-energy contrast-enhanced digital mammography (CEDM) is as sensitive in detecting breast cancer as contrast-enhanced breast MRI when both were compared with standard mammograms.
CEDM is similar in concept to contrast-enhanced breast MRI with regards to the information that can be obtained by the exam, however, in many cases, CEDM may be better tolerated by women as it is a shorter, faster exam, performed in the same way as a standard mammogram.
The Technology
CEDM is an advanced breast-imaging technique designed to highlight areas that may not be detected with standard 2-D full-field digital mammograms (2D FFDM). As with a breast MRI, the administration of intravenous contrast in CEDM highlights areas of increased blood flow that may be associated with tumor growth.
CEDM has consistently been demonstrated to be more sensitive than standard mammography for the detection of breast cancer.
Women who are at an intermediate risk of developing breast cancer — those with a 15 to 20 percent chance in their lifetime based on risk assessment models — may benefit most from this type of examination.
Our Research
A retrospective review performed by radiologists in the Breast Imaging Service at MSK, published in Radiology in January 2017, demonstrated that the level of background parenchymal enhancement (BPE) detected on CEDM was in substantial agreement with that on MRI, supporting the premise that these two types of imaging studies evaluate the breast similarly. (1) In addition, on both MRI and CEDM studies, BPE demonstrated a significant relationship with menopausal status, radiation treatment, hormonal treatment, and breast density. (1)
BPE is the amount of normal breast tissue found to be enhanced after contrast is given during breast MRI examinations. (2) The degree of BPE is related to the vascular supply and permeability of breast parenchyma and is usually present in a bilateral, symmetrical distribution. (1) BPE is an important parameter to evaluate as it has been demonstrated to be an independent predictor of breast cancer risk even when compared with the well-studied mammographic breast density. (2)
Our research concludes that because of its low cost, potential broad availability, and ability to be used in women who cannot undergo MR imaging because of such things as metallic implants or claustrophobia, CEDM is a promising addition to current breast-imaging techniques. (1)
A previous study performed at MSK and published in the journal Radiology in 2013 also demonstrated CEDM to be comparable to contrast-enhanced breast MRI for depicting breast cancer, with both types of imaging studies showing improvement over conventional 2D FFDM. (3) Results of this study showed that both CEDM and contrast-enhanced breast MRI depicted 96 percent of the tumor while 2-D FFDM depicted 81 percent. (3)
We also recently investigated the performance of CEDM when used for breast cancer screening. Our preliminary results, yet to be published, showed that CEDM is a promising technology that may be used for breast cancer screening of women, particularly those at an intermediate risk of the disease. In our study, we reviewed 1,197 screening CEDM studies in women with intermediate risk factors performed from 2012 to 2016. During that time period, in correlation with patient risk factors, we found that CEDM had a cancer detection rate in 18 of 1,000 women, with the relative proportion of ductal carcinoma in situ to invasive cancer comparable to screening mammography. These results were presented at the annual meeting of the Radiological Society of North America in November 2017.
Assessing Risk
Medical advances in techniques for evaluating a woman’s risk of breast cancer have allowed doctors specializing in breast disease to stratify women into different categories of risk. (4) With this information, doctors can offer more personalized recommendations for ways women can be screened for the disease.
Screening for breast cancer with mammography has been proven to reduce mortality from the disease by up to 30 percent. (5)
The majority of women who develop breast cancer have no risk factors other than being a woman.(4)(5) These women are at an average risk or have less than a 15 percent chance of developing the disease in their lifetime, and annual screening mammography exams, with perhaps supplemental screening with whole breast ultrasound, are routine screening studies for these women.(4)(5) In contrast, women at an increased risk of breast cancer have a greater than 20 percent chance of developing the disease, with a number of identifiable factors that classify these women to be high risk. (4)(5) It is suggested that these women undergo breast MRI examinations to help detect breast cancer. (4)
Our work investigating CEDM suggests it to be a promising technology for breast cancer screening, particularly in women at an intermediate risk of developing the disease. Risk assessment may be an important component to deciding what type of breast cancer screening examinations might be best suited for individual women, many of whom may wish to take part in deciding with their doctors on which tests to have.
Women interested in learning more about their risk of breast cancer may consult with MSK’s RISE (risk assessment, imaging, surveillance, and education) program, where our experts take into account a combination of factors to determine if they are at an increased breast cancer risk and, if they are, to shape a long-term surveillance plan customized specifically for each individual. Contrast-enhanced mammography performed by the Breast Imaging Service at MSK may be a component of that customized surveillance and an option for mammograms in those women who do not have contraindications to receiving contrast.
- Sogani J, Morris E, Kaplan J, et al. Comparison of Background Parenchymal Enhancement at Contrast-Enhanced Spectral Mammography and Breast MR Imaging. Radiology. 2017;282:63–73.
- King V, Brooks J, Bernstein J, et al. Background Parenchymal Enhancement at Breast MR Imaging and Breast Cancer Risk. Radiology. 2011;260:1, 50-60.
- Jochelson M, Dershaw D, Sung J, et al. Bilateral Contrast-Enhanced Dual-Energy Digital Mammography: Feasibility and Comparison with Conventional Digital Mammography and MR Imaging in Women with Known Breast Carcinoma. Radiology. 2013;266:3, 743–751.
- Lee C, Dershaw D, Kopans D, et al. Breast Cancer Screening with Imaging: Recommendations from the Society of Breast Imaging and the ACR on the Use of Mammography, Breast MRI, Breast Ultrasound, and Other Technologies for the Detection of Clinically Occult Breast Cancer. Journal of the American College of Radiology. 2010;7:1, 18–27.
- Barke L, Freivogel M. Breast Cancer Risk Assessment Models and High-Risk Screening. The Radiologic Clinics of North America. 2017; 55:3 457-457.