
Access to information about fertility preservation and family-building options before and after cancer treatment is a key factor in the psychological wellbeing of young patients. But, unfortunately many of them don’t get adequate advice at the time that they need it.
Each year, almost 150,000 people in the United States are diagnosed with cancer before the age of 45. (1) Many of these patients will not have started or completed their families at the time of diagnosis, and unfortunately, many cancer treatments can result in impaired fertility.
Professional guidelines from organizations such as the American Society of Clinical Oncology (ASCO) delineate the responsibility of health care providers to inform patients of potential risks to fertility from treatment, discuss fertility preservation (FP) options, and refer interested patients to appropriate reproductive specialists. (2) Yet despite this, oncology clinicians can face a number of barriers in having these discussions, including a lack of knowledge about FP, inadequate time in busy clinics, insufficient resources to educate patients, not knowing where to refer patients, and concerns about delaying treatment.
To help overcome these barriers, in 2009, Memorial Sloan Kettering (MSK) established the nurse-led Cancer and Fertility Program that provides resources to help clinicians have these discussions with their patients.
Cancer Treatments’ Impact on Fertility and Advances in Fertility Preservation
Surgical procedures may require removal of reproductive structures, and pelvic surgery and radiation may damage reproductive tissues and impair their function. Certain chemotherapy drugs and radiation exposure of the ovaries or testes can destroy eggs or the cells that develop into sperm. Cranial surgery or radiation involving the pituitary gland may disrupt hormonal regulation of sperm production and egg maturation. New targeted and immunotherapy agents are being introduced for an expanding number of cancers, with limited data available on how they may affect fertility. Because of the many factors involved, it is impossible to predict with certainty how any one patient’s fertility will be affected. So, for many young patients, reproductive concerns can be significant. However, advances in reproductive medicine enable many patients with cancer to preserve fertility before treatment. FP options currently available are described in Table 1.
The MSK Cancer and Fertility Program
The goal of our program is to ensure patients receive information about their fertility risks and FP options and are referred to appropriate reproductive specialists if interested. Not all patients will want or be able to pursue FP; however, for those who do, this must be completed before treatment begins. The program is multi-faceted, as illustrated in Figure 1. Ongoing education is provided to our clinicians at grand rounds, disease-specific service meetings, annual fellow and nursing orientations, and staff meetings. Clinician resources can be accessed at any location through the internet. These include updated references and policies, tips on discussing fertility, and algorithms with suggested work flows. In addition, we have identified reproductive specialists in the community to whom we can refer patients and a defined process for making these referrals. Resources for patients include educational booklets related to FP and family building, as well as videos on selected fertility topics, all available on MSK’s website.
The most significant component of the program is the availability of Fertility Nurse Specialists (FNS) to provide fertility-related consultations to our patients. Clinicians can refer any interested patient (regardless of age, diagnosis, treatment, or stage of disease) to these nurses for individualized education about risks and options, counseling to help with decision-making, and facilitation of referrals to reproductive specialists in the community. When making these referrals the FNS ensures all relevant clinical information is communicated and coordinates care as needed to ensure patient safety and to prevent or minimize treatment delays. The FNS also facilitates getting access to any financial assistance that may be available for patients. Consultations can be provided by phone, in the clinic, or in the inpatient setting. In addition to addressing FP before treatment, information can also be provided about family building after treatment, including information on using donor gametes, surrogacy with a gestational carrier, and adoption.
The final component of the program encompasses our research activities and ongoing efforts to assess and improve the program. For example we monitor the number of patient consultations provided by the FNS (see Figure 2). To date almost 3,000 patients have received a fertility consultation, a tribute to clinicians throughout MSK as it reflects their increasing commitment to incorporating fertility discussions into their practice.
Evaluating the Program - Patient Perspectives
We assessed satisfaction of patients with the fertility-related information they had received by comparing cohorts of patients who had been treated at our center before and after the program was initiated. (3) Satisfaction with the amount of information received on almost all fertility-related topics queried increased significantly after initiation of the program. Further, females who had a FNS consultation reported significantly higher rates of satisfaction than those who did not, highlighting the value to patients of speaking with a specialist focused on their fertility concerns. To our knowledge, this study is the first to report changes in patient satisfaction with information received over time within a single institution. Satisfaction with information about other family-building options also increased after the program was initiated.
We also found that a higher percentage of MSK patients pursued FP than has been reported by other institutions. Although women who did not undergo FP before treatment had more decision regret after treatment compared with women who preserved their fertility, they were less likely to experience regret if they received fertility counseling. This is consistent with the findings of other researchers who have found that fertility consultations may lead to improvements in quality of life, with less decisional regret after treatment is completed. (4)
After our program was initiated, a high percentage of patients pursued FP (44 percent of males and 18 percent of females). Other US patient groups have reported lower rates (24 percent of males and 5-10 percent of females).
The Cancer and Fertility Program provides value to our clinicians and patients, and MSK’s ongoing support of the program demonstrates the center’s commitment not just to making advances in the treatment of cancer, but also to addressing the quality of life issues patients face after treatment has ended
Table 1. Fertility Preservation Options
| Sperm Banking (freezing of sperm) |
|
|---|---|
| Testicular Shielding |
|
| Testicular Tissue Cryopreservationa |
|
| Oocyte and Embryo Cryopreservationb |
|
|---|---|
| Ovarian Tissue Cryopreservationb |
|
| Ovarian Transpositionc |
|
| Ovarian Suppression |
|
| Alternative Treatment for Select Patients with Early-Stage Gynecologic Cancersc |
|
- a – offered by Dr John Mulhall in our Department of Urology
- b – offered by reproductive endocrinologists in the community
- c – offered by Gynecologic Surgeons in our Department of Surgery
Figure 1 - MSK Cancer and Fertility Program
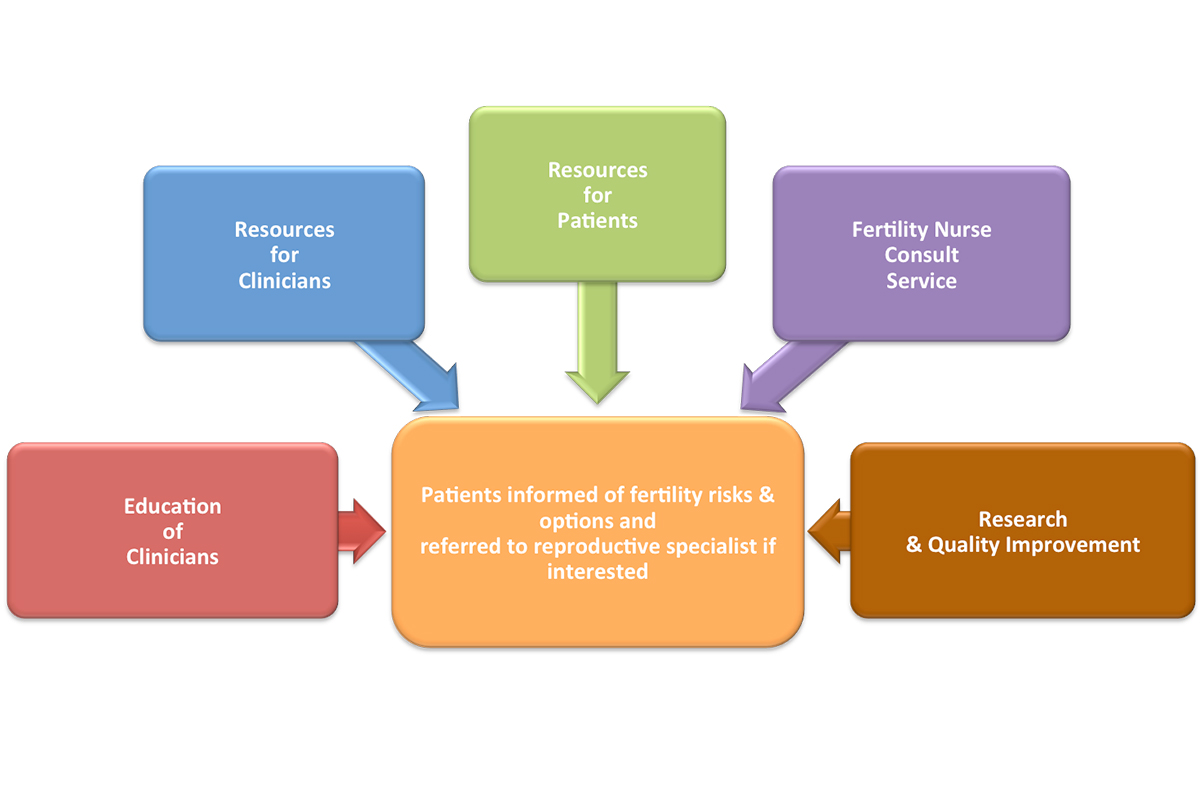
Figure 2 - Fertility Nurse Specialist Consultations
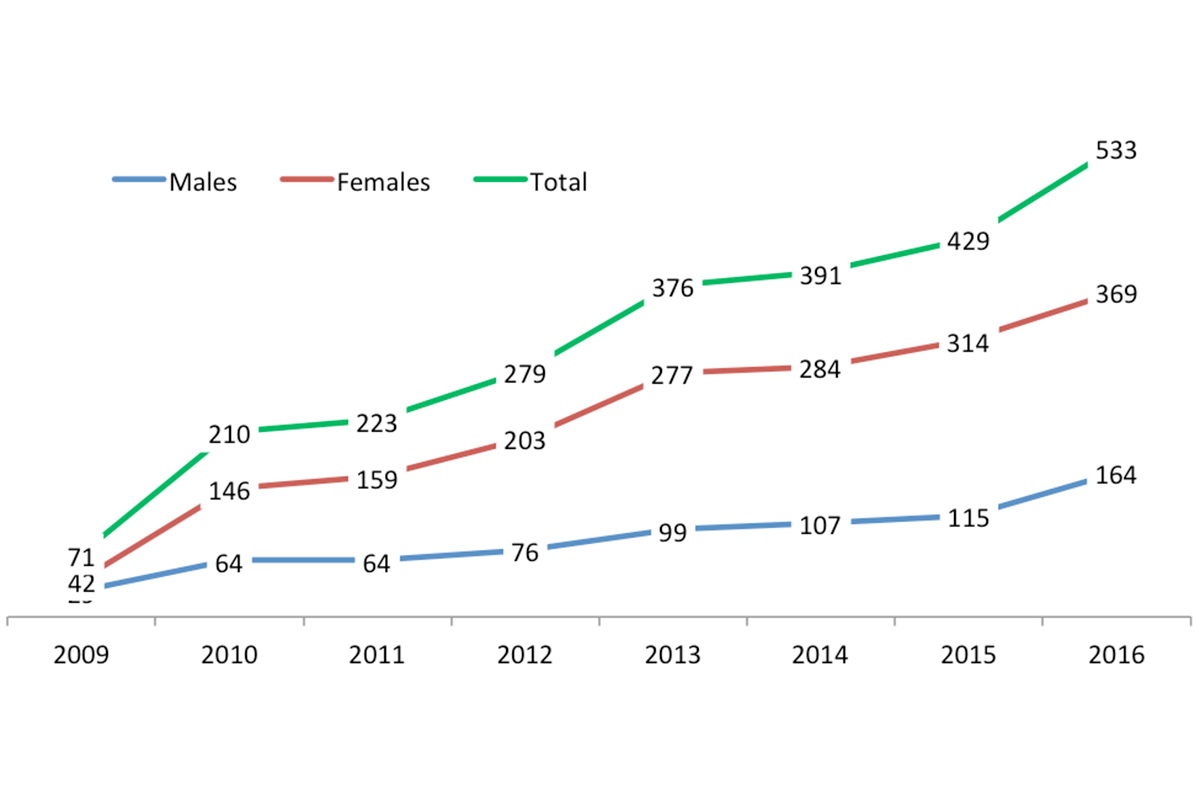
Note: our projected number of consultations for 2017 based on the first 6 months of the year is 626.