New data from researchers at Memorial Sloan Kettering Cancer Center (MSK) revealed the effects of Medicaid expansion on cancer death rates on a national scale. The landmark study found that states that adopted Medicaid expansion following the passage of the Affordable Care Act (ACA) in 2010 saw greater decreases in cancer mortality rates than states that did not. The findings were presented as part of the press program for this year’s virtual annual meeting of the American Society of Clinical Oncology (ASCO).

“In the United States, there are 1.8 million new cancer diagnoses every year. Cancer is a healthcare amenable condition, meaning that access to healthcare is expected to improve survival outcomes,” said Anna Lee, MD, MPH, lead author and radiation oncology fellow at MSK. “Knowing this information, we wanted to study if there was an additional cancer mortality benefit for residents of states that expanded to Medicaid under the ACA, compared to those that did not.”
According to data in 2016 from the National Center for Health Statistics, nearly 20 million Americans gained insurance between the years 2010 and 2016, as a result of the congressional approval of the ACA in 2010. Dr. Lee’s results found that age-adjusted cancer mortality saw a 29 percent decline in states with expanded Medicaid, falling from 65.1 to 46.3 per 100,000 individuals from 1999-2017. In states that did not expand Medicaid, rates dropped by 25 percent, from 69.5 to 52.3 per 100,000 individuals.
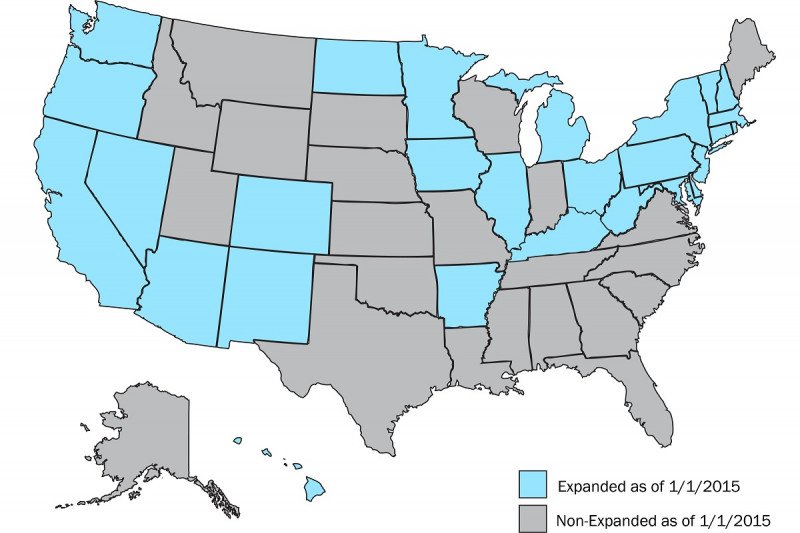
The study was conducted using data from the National Center for Health Statistics and included all U.S. residents. After assessing for baseline trends from 1999 to 2017, the researchers compared age-adjusted cancer-related mortality rates between 2011-2013 (prior to full state expansion) and 2015-2017 (the period following expansion) for states that adopted Medicaid expansion and those that did not. Deaths due to cancer in patients under the age of 65 were included in the analysis, as those patients 65 and older are eligible for Medicare. During the time period of this analysis, 27 states plus the District of Columbia had adopted Medicaid expansion, while 23 states had not.

“When specifically looking at the changes after the 2014 expansion, the additional mortality benefit for states that adopted Medicaid amounted to an estimated 785 fewer cancer deaths in 2017 alone,” said senior author Fumiko Chino, MD, a radiation oncologist at MSK. “We estimate that an additional 589 cancer deaths could have been prevented if non-expanded states had expanded Medicaid.”
Additionally, the researchers also looked at changes in sub-populations, including black and Hispanic patients. Although black patients had large morality gains during the study period, no additional mortality reduction was seen for black patients in states with Medicaid expansion. However, age-adjusted cancer mortality overall was consistently worse for black patients in states without expansion than in states with expansion (58.5 vs 63.4 per 100,000 individuals for the expansion and non-expansion states respectively in 2017).
In contrast, the greatest differential change in cancer mortality rates between expansion and non-expansion states was seen for Hispanic patients. However, there was significant year-to-year mortality variability in this population, which may cloud definitive conclusions in this population with known poor access to healthcare.
For the study analysis, the researchers used a statistical technique called difference-in-differences. They calculated the difference in mortality rates between the two periods for expansion and non-expansion states, and then calculated the difference between these values. The intent is to mitigate the effects of baseline population differences and other differences in access at the state level.
Comparing the mortality changes before and after ACA expansion, the difference in differences was -1.1 and -0.6 per 100,000 for expansion and non-expansion states respectively (p=0.006 expanded, p=0.13 non-expanded).
“We are proud to release the findings of the first nationwide study to show that Medicaid expansion is associated with a reduction in cancer deaths,” said Lee. “However, more research is needed to understand how national programs and policies, such as the ACA, will continue to improve access to care and decrease healthcare disparities.”