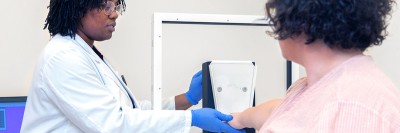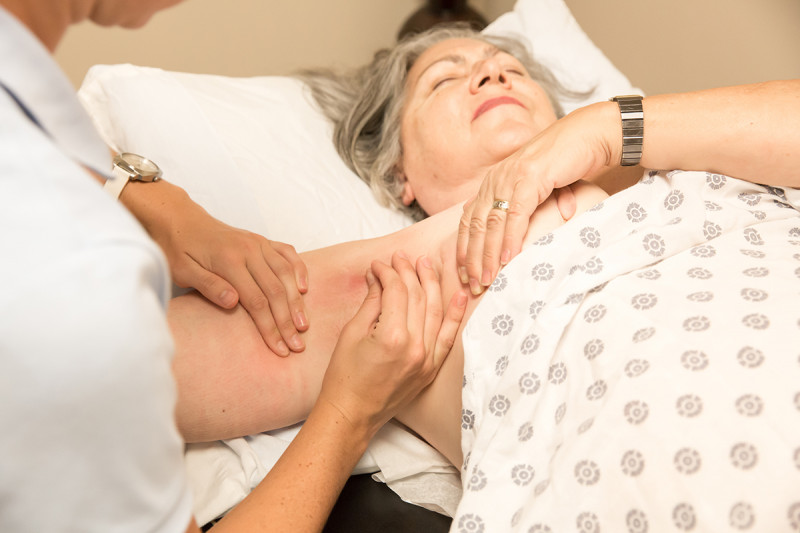
One of the most dreaded complications of cancer treatment is lymphedema — the uncomfortable and often disfiguring accumulation of fluid in the arms or legs. The condition is progressive and there are no known cures.
Lymphedema most commonly occurs following the removal of lymph nodes, a procedure that can injure the delicate vessels of the lymphatic system, which helps rid the body of toxins. About one in three people who undergo a lymph node dissection will develop the complication, which translates to roughly 50,000 new cases every year. Women with breast cancer are most at risk.
“A lot of patients describe it as worse than their actual cancer diagnosis,” says Babak Mehrara, Chief of the Plastic and Reconstructive Surgical Service at Memorial Sloan Kettering. “They wake up every day and they can’t do the things they want to do. They can’t wear their wedding ring.”
Previous research from Dr. Mehrara’s lab had suggested that lymphedema results from an uncontrolled inflammatory process promoted by certain immune cells. In a new paper, published on February 10 in the journal Nature Communications, he and his colleagues show that an FDA-approved drug that quells the actions of these inflammatory cells can reverse the debilitating condition, or prevent it from developing — at least in mice.
Whether the drug — which is applied directly to the skin — will have the same positive effects in humans is a question he and his team plan to explore in clinical trials.
Telling Tails
To study lymphedema and drugs that may fight it, Dr. Mehrara’s lab uses a mouse model that reproduces the hallmark features of the condition. Following a small injury to the lymphatic vessels in their tail, the mice reliably develop inflammation and swelling as well as a scarring process called fibrosis.
“The mouse model is very effective because it mimics the histological features of lymphedema very closely,” he says. “The inflammatory changes that we see are exactly the same as those we see in patients.”
When the team tested the drug, called tacrolimus, on the mice’s tails, they found that it could prevent lymphedema from developing when applied soon after the injury. It also greatly reduced the extent of lymphedema when applied later, after the condition had already developed.
Inflammation can impair the growth of new lymphatic vessels, but the topical treatment seemed to reverse that complication too. Treated mice showed growth of new, healthy lymphatic vessels, restoring function that had been lost due to the injury.
A Light Bulb Moment
Dr. Mehrara says the idea to test tacrolimus as a lymphedema treatment came from his experience as a plastic surgeon. Tacrolimus is commonly used to treat several skin disorders that are caused by inflammation, including psoriasis and eczema. It’s also used to prevent tissue rejection after an operation like a hand transplant. The drug works by suppressing the action of certain immune cells called CD4-positive T cells that provoke inflammation. These are the same cells that cause lymphedema.
“I thought, well, if the goal is to deplete these T cells, why not just use this drug that’s already commercially available and FDA approved? And so that’s what we did,” he says.
Safety Concerns
It’s important to note that while tacrolimus is FDA approved to treat certain inflammatory conditions, it is not a drug to be used indiscriminately. And it cannot yet be recommended or prescribed for lymphedema.
When prescribed for inflammatory skin conditions, it’s only meant to be applied over a very small area and for a limited period of time. The drug can cause kidney toxicity if too much is used.
“If you have lymphedema of your arm, you can’t smear tacrolimus on your whole arm because you’d get too high a dose,” Dr. Mehrara says.
Moreover, lymphedema can sometimes take years to develop and it’s not possible to predict who will develop it. Nevertheless, the study provides a proof of concept that a topical treatment for lymphedema is possible. “That’s the real point of this research paper,” he notes.
Dr. Mehrara says he plans to start applying in June for funds to conduct a clinical trial to test tacrolimus as a topical treatment for lymphedema in people. Because of the potential toxicity issues, the trial will only be for patients with very specialized cases of limited lymphedema.
In addition to tacrolimus, his lab is also testing several other chemicals — some that may be less toxic to the kidneys — in the hopes of finding a safe, effective treatment for this damaging condition that currently affects 6 million people in the United States.