Computational biologist Joao Xavier has spent most of his career researching how bacterial cells interact with one another and produce complex group behaviors. He had never studied cancer before joining Memorial Sloan Kettering, in 2009.
“I came here partly because I was intrigued by cancer biology,” he says. “I kept seeing all these parallels between microbial communities and tumors that I wanted to explore.”
Cancer cells and bacteria are different in many ways, but common principles hold for how populations of all types of cells behave and evolve. The emergence of drug resistance is one example. Dr. Xavier explains that in the same way antibiotic treatment of an infection can create strong evolutionary pressure that favors the survival of drug-resistant bacteria, so can treatment with some cancer drugs select for clones of cells within a tumor that grow in spite of the drug, eventually rendering the tumor unresponsive.
“Whether we are interested in drug resistance or other aspects of cancer biology, we can learn a lot about tumors at the conceptual level by studying bacterial evolution,” he says.
From Bacterial Biofilms to Tumors
Bacteria commonly grow in densely packed communities known as biofilms, aggregates of cells embedded in a gluey matrix. Dr. Xavier’s team has developed computer models to analyze how cells within biofilms interact chemically and biophysically, and combines this computational research with laboratory experiments.
Recently they applied a similar system to study how cancer cells within a tumor interact with noncancerous cells known as macrophages.
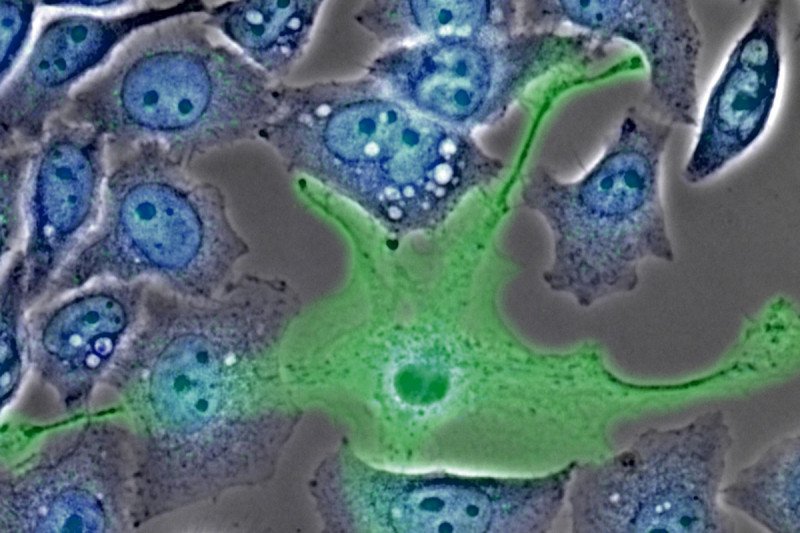
A macrophage is a type of cell that inhabits organs and tissues and forms an essential part of the body’s line of defense against pathogens. In people with cancer, however, macrophages often start growing inside and around a tumor, and their normal function can be subverted to help the tumor grow and metastasize.
The work was a multidisciplinary collaboration led by Dr. Xavier, postdoctoral fellow Carlos Carmona Fontaine, and Sloan Kettering Institute cancer biologist Johanna Joyce. Together, the researchers set out to explore the spatial patterns of macrophages in tumors.
A New Perspective on Cancer Cell Metabolism
“When a tumor is small, it’s uniformly infiltrated by macrophages,” Dr. Xavier explains. “But as it grows, macrophages tend to stay on the outside” of the tumor, possibly shielding the cancer cells within from detrimental cells and factors in the nearby environment. “This pattern had been observed in many tumor types, but to our knowledge no one had looked at why it forms,” he says.
He and his colleagues used the same computer models they use for research on bacterial biofilms to make predictions about the complex interplay of cancer cells and macrophages and tested these predictions in experiments with cells growing in culture. Ultimately their research showed that the redistribution of macrophages to the tumor periphery is driven by metabolic changes in tumor cells that lead to high levels of lactic acid, making the tumor’s interior toxic to macrophages. Over time, macrophages stay at the tumor’s periphery, where they have better access to nutrients.
Dr. Xavier thinks the research, which was published in the journal PNAS last year, may inspire more scientists to consider how changes in cancer cell metabolism affect noncancerous cells in the tumor microenvironment. In addition, the findings could open possibilities for the development of new drugs that act on tumor-associated macrophages rather than on cancer cells.
“Our research is only a small piece in this puzzle,” Dr. Xavier says. “But it’s a unique piece that we were able to contribute perhaps in part because we’re not cancer biologists and came to the problem with an outside perspective.”
This research was supported by the National Institutes of Health under award numbers CA148967 and DP2OD008440.
