This information describes the causes, symptoms, and treatment of atrial fibrillation (AY-tree-ul fih-bruh-LAY-shun). Atrial fibrillation is also called atrial fib or AFib.
- Atria (AY-tree-uh) are the upper chambers of your heart.
- Ventricles (VEN-trih-kulz) are the lower chambers of your heart.
- Artery (AR-tuh-ree) is a blood vessel (tube) that brings blood to and from your organs.
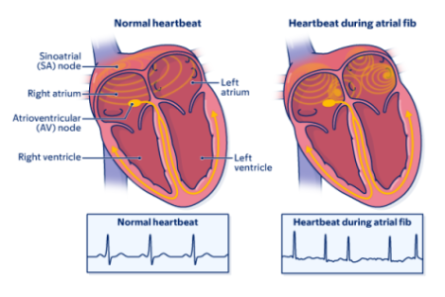
About atrial fib
Atrial fib is a common heart rhythm disorder that happens when your atria contracts (squeezes) very quickly and irregularly. This causes blood to pool in your atria instead of getting pumped into your ventricles. When blood pools in your atria, blood clots are more likely to form.
Causes of atrial fib
Your risk of atrial fib gets higher as you get older. Your risk also gets higher if you have other heart diseases.
The most common causes of atrial fib include:
- Having high blood pressure for a long time.
- A heart attack.
- Heart failure.
- Heart valve disease.
- Chronic (long-lasting) lung disease.
- Heart surgery. Less often, atrial fib can be caused by other types of surgery. Atrial fib during surgery is usually temporary.
Atrial fib can also be caused by:
- Drinking too much alcohol or binge drinking.
- Having too much caffeine.
- Hyperthyroidism (HY-per-THY-roy-dih-zum). This is when your thyroid is too active.”
- Medications that raise your heart rate, such as theophylline (an asthma medication found in some inhalers).
- Sleep apnea. This is a condition that causes you to stop breathing for short lengths of time while you sleep.
- An infection anywhere in your body.
- Chemotherapy. Talk with your healthcare provider about if your treatment needs to change, and which options are best for you.
If the cause of atrial fib is not known, it’s called lone atrial fibrillation.
Symptoms of atrial fib
Not everyone who has atrial fib knows they have it. Some people have no symptoms. Others have many symptoms that tell them something is wrong.
Mild symptoms include:
- Heart palpitations. This is when your heart beats faster or stronger than usual, or you have an irregular heartbeat.
- Chest discomfort.
- Heart racing.
- Shortness of breath.
- Feeling lightheaded or dizzy.
- Fatigue (feeling more tired or weak than usual).
As your heartbeat gets faster or more irregular, your symptoms may get worse. These can include:
- Chest discomfort.
- Trouble breathing or shortness of breath.
- Fainting or feeling like you’re going to faint.
- Confusion.
- Fatigue.
How to prevent and treat atrial fib
There are several ways to prevent and treat atrial fib:
Medications
Certain medications can slow down your fast heart rate, such as:
- Beta blockers, such as atenolol, metoprolol, and propranolol.
- Digoxin (Lanoxin®).
- Amiodarone (Cordarone®).
- Calcium channel blockers, such as verapamil and diltiazem.
- Sotalol (Betapace®).
Sometimes, these medications can make your heart beat too slowly. If that happens, you may need a pacemaker. A pacemaker is a small device that goes under your skin near your heart. This device keeps your heart from beating too slowly. Talk with your healthcare provider to see if a pacemaker is best for you.
Electrical cardioversion
Electrical cardioversion (ee-LEK-trih-kul KAR-de-o-VER-shun) is a procedure that can help bring your heart’s rhythm back to normal.
An electrophysiologist (ee-LEK-tr0h-FIH-zee-uh-LAH-jist) will do this procedure. An electrophysiologist is a cardiologist (heart doctor) with special training to treat heart rhythms that are not normal. They will use small electric shocks to make your heart beat normally.
This procedure is most often done if medication does not help ease your symptoms. Talk with your healthcare provider to see if this procedure is best for you.
Radiofrequency ablation
Radiofrequency ablation (RAY-dee-oh-FREE-kwen-see a-BLAY-shun) is a minimally invasive procedure. This means the procedure is done using a needle with less harm to your body.
An electrophysiologist will do this procedure. They will use a special needle to destroy tissues in your heart that are causing atrial fib.
This procedure may be done if medications and electrical cardioversion don’t work. Talk with your healthcare provider to see if this procedure is best for you.
About medications to lower your risk of stroke
Atrial fib can cause blood clots in your heart. If a blood clot leaves your heart and travels to your brain, it may get stuck in an artery. This can block blood flow to your brain and cause a stroke. Symptoms of stroke include trouble speaking, arm or leg weakness, headache, and drooping on one side of your face.
Your doctor will find the best treatment for you based on your risk factors for having a stroke. These risk factors include:
- Having a stroke in the past.
- Having congestive heart failure (CHF).
- Being 65 years old or older.
- Having high blood pressure that is not controlled.
- Having blood clots in the past.
- Having diabetes.
- Having vascular disease. This is a condition that affects your blood vessels or blood flow.
Examples of common blood thinners used for atrial fib are listed below. There are others, so be sure your care team knows all the medications you take.
Do not stop taking your blood thinner without talking with a member of your care team.
|
|
Resources
Visit the American Heart Association’s Atrial Fibrillation web page at www.heart.org/afib to learn more about atrial fib.
Learn about our Health Information Policy.