This information explains heart failure, including causes and signs of heart failure, how heart failure is diagnosed, and how it’s treated.
About heart failure
Heart failure happens when your heart doesn’t pump blood as well as it should. Your heart delivers blood to your body’s cells, and if you have heart failure, your heart can’t supply your cells with enough blood. To make up for this, the heart may stretch to hold more blood to pump for the body, or it might become thick and stiff (see Figures 1 and 2).
Heart failure can cause fluid to build up in your body. This can cause you to have trouble breathing, swelling (edema) in your feet and legs, or both.
Watch this animation to learn more: https://watchlearnlive.heart.org/CVML_Player.php?moduleSelect=hrtflr.
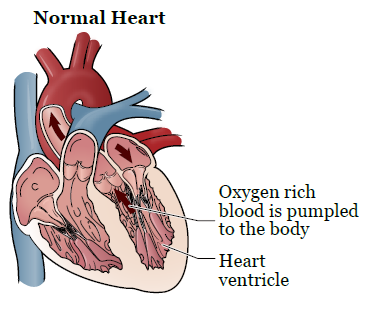
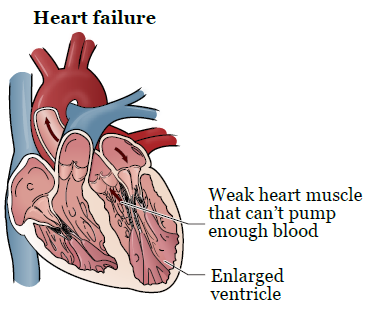
Types of heart failure
Left-sided heart failure
Systolic heart failure is when the left ventricle cannot contract (tighten) normally. This means that the heart cannot pump with enough force to push the blood through the body.
Diastolic heart failure is when the left ventricle cannot relax normally because the muscle gets stiff. This means the heart cannot fill with enough blood between each heartbeat.
Right-sided heart failure
Blood that has flowed through the body goes into the right side of the heart. The right ventricle pumps blood from the heart to the lungs to receive oxygen. Then, the blood goes into the left side of the heart. When the right side of the heart cannot pump normally, this causes fluid to build up in the body.
Causes of heart failure
Heart failure can be caused by many things, including:
- High blood pressure. With high blood pressure, your heart has to work harder to pump blood. This can make your heart enlarged (stretched out). When your heart is enlarged, it can’t pump as well.
- Coronary artery disease. This is damage in your heart’s blood vessels.
- Smoking. Smoking can cause blockages in your blood vessels which can make it harder for your heart to pump blood. This can make your heart weaker over time.
- Heart attacks. Heart attacks can cause parts of your heart to not without oxygen. This can make those parts weaker and can cause lasting damage to your heart.
- Valvular heart disease. This happens when one of the valves in your heart is damaged. This can make it harder for blood to flow through the valve, which can increase pressure in your heart.
- Congenital heart disease. This is a problem with your heart that you’re born with.
- Hyperthyroidism. This is when your thyroid gland makes more hormones than your body needs.
- Cardiomyopathy. This is a disease that makes your heart enlarged or thick, so it doesn’t pump blood well.
- An infection in your heart.
- An irregular heart rhythm that isn’t controlled, such as a condition called atrial fibrillation.
What is congestive heart failure (CHF)?
Congestive heart failure happens when blood or fluid builds up in the body. This can cause:
- Edema (swelling) in the legs.
- Bloated abdomen (belly).
- Congestion in the lungs which can cause trouble breathing.
If you have symptoms of heart failure, call your healthcare provider right away.
Symptoms of heart failure
The following things are common signs of heart failure:
- Trouble breathing when you’re active or resting. Some people might also need to sleep sitting up or with many pillows under their head to help them breathe.
- Swelling in your feet, ankles, legs, or abdomen (belly)
- Fatigue (feeling more tired or weak than usual)
- Feeling weak, dizzy, or lightheaded
- Fast heartbeat or uneven heartbeat
- Dry cough, which may have a white or pink mucus
- Sudden weight gain
- Chest pain
- Trouble focusing or not being as alert
- Not feeling hungry
- Nausea (feeling like you’re going to throw up)
How to diagnose heart failure
There are many different tests to diagnose heart failure. You may have 1 or more of the following tests below. Your healthcare provider will tell you what to expect.
- Chest x-ray. This will help your doctor see if there’s fluid in your lungs, if your heart is enlarged, or both.
- Blood tests. These tests will check for a hormone called brain natriuretic peptide (BNP) that’s released by the cells in your heart when you have heart failure.
- An echocardiogram (echo). This is an imaging test that uses ultrasound (sound waves) to take pictures of your heart. It shows how your heart is beating and pumping blood and can show if there’s anything wrong with your heart muscle, heart valves, or both.
How to treat heart failure
There are several types of medication used for treating heart failure. The medications work in different ways. The following are some examples, but there are others. Your cardiologist (heart doctor) will tell you which is best for you.
-
ACE inhibitors, angiotensin II receptor blockers (ARBs), and angiotensin receptor-neprilysin inhibitors (ANRIs) are medications that relax your blood vessels and lower your blood pressure. This makes it easier for your heart to pump. Some examples are lisinopril (Prinivil®) and losartan (Cozaar®).
- An ANRI is an ARB with a second medicine. This type of medication works in a similar way to ARB and ACEI, so you should only be on one type of these medications at the same time. The one ARNI currently available is sacubitril-valsartan (Entresto®).
- Beta blockers slow your heart rate and lower your blood pressure. This helps reduce the amount of work your heart has to do. Examples are carvedilol (Coreg®) and metoprolol (Lopressor®).
- Diuretics (water pills) help your body get rid of extra salt and fluid. They can help with swelling and can help you breathe better. One example is furosemide (Lasix®).
- Aldosterone receptor antagonists help get rid of extra fluid in your body. They also help you keep potassium in your body. One example is spironolactone (Aldactone®).
- Sodium-glucose cotransporter-2 (SGLT2) inhibitors were made to treat diabetes at first. They now have also been found to help with symptoms of heart failure. SGLT2 inhibitors help to decrease body weight and blood pressure and improve heart function. Examples are dapagliflozin (Farxiga®) and empagliflozin (Jardiance®).
- Nitrates widen your coronary arteries (arteries in your heart). This helps bring more blood to your heart muscle and can reduce chest pain. Examples include nitroglycerin and isosorbide dinitrate.
- Digoxin (Lanoxin®) helps your heart beat stronger.
How to manage heart failure
There are many ways you can take care of yourself if you have heart failure. Here are some tips for healthy habits and lifestyle changes you can make if you have heart failure. Following these tips will help you manage your heart failure symptoms.
-
Follow a healthy diet. Read the resource Eat Your Way to Better Health for healthy eating tips.
- Eat less salt. Most people with heart failure shouldn’t eat more than 2 grams of sodium every day but talk with your healthcare provider about the amount that’s right for you. Limit processed foods, such as canned soups, frozen meals, and deli meats. These foods can be high in sodium. Read the resource 2-Gram Sodium Diet to learn more about following a low-sodium diet.
- Drink fewer liquids. Most people with heart failure shouldn’t drink more than 4 (8-ounce) glasses of liquids every day. If you drink too much fluid, it could cause fluid build-up (retention). Talk with your healthcare provider about the amount that’s right for you.
- Lose weight, if you’re overweight.
- Talk with your healthcare provider about your cholesterol levels.
- Weigh yourself every day. If your weight increases by 2 pounds (about 1 kilogram) in 1 day or 4 pounds (1.08 kilograms) in 1 week, call your healthcare provider. This might mean you have fluid build-up.
- If you smoke, try to quit. MSK has specialists who can help you quit smoking. For more information about our Tobacco Treatment Program, call 212-610-0507. You can also ask your healthcare provider about the program.
- Don’t drink more than 1 alcoholic drink per day if you’re a female and 2 drinks per day if you’re a male.
- Exercise every day, if you can. Talk with your healthcare provider if you would like a referral to a physical therapist.
- Talk with your healthcare provider or cardiologist about how to manage other health problems (such as high blood pressure, high cholesterol, and diabetes), if you have them.
-
Join a cardiac rehabilitation program. This is a program that helps improve the health and well-being of people who have heart problems. The program includes:
- Exercises for heart health.
- Education on ways to lower your risk for other heart problems.
- Counseling to reduce stress.
When to call your healthcare provider
If you have symptoms of heart failure, call your healthcare provider right away.
Learn about our Health Information Policy.