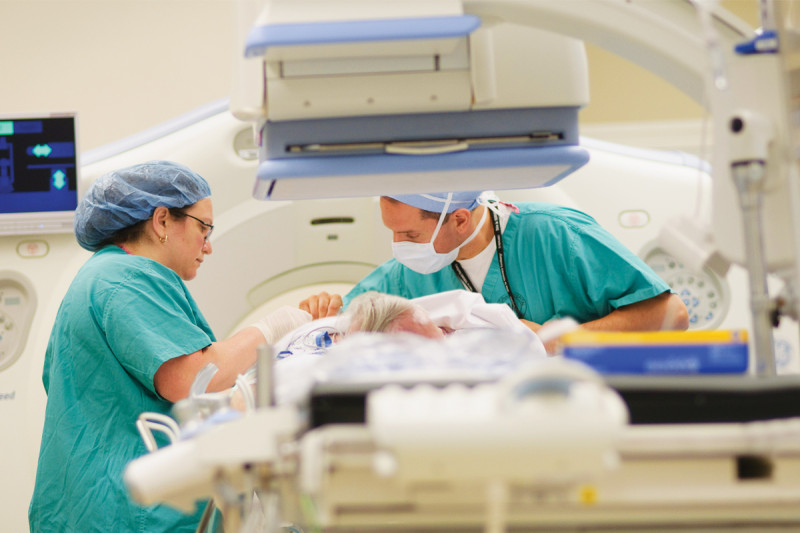
The Center for Image-Guided Interventions (CIGI) offers the most-advanced, minimally invasive diagnostic and treatment options for people with cancer. It is designed to create a unique multidisciplinary setting that fosters rapid innovations in cancer care.
CIGI facilitates collaborations among interventional radiologists, surgeons, and endoscopists. Using imaging technologies such as three-dimensional fluoroscopy, CT, ultrasound, PET, and MRI, our physicians perform diagnostic procedures and deliver a variety of treatments without the need for large incisions. These minimally invasive procedures can reduce the risk of complications, shorten hospital stays, and decrease cost.
CIGI has six procedure rooms with advanced imaging equipment. Each room also features a Wall of Knowledge that enables physicians in other procedure rooms to share real-time images and consult with one another via videoconferencing.
Interventional radiologists at CIGI work closely with physicians on Memorial Sloan Kettering’s multidisciplinary disease management teams to identify patients who would benefit from image-guided procedures.
Among the procedures we perform in CIGI are:
Image-guided biopsy is used to obtain tissue samples from an area that may not be palpable. A radiologist may use ultrasound, stereotactic imaging, or MRI ─ depending on what the abnormality looks like and which technique is most appropriate for visualizing it.
The image-guided approach is commonly used during fine-needle aspiration biopsy, often to biopsy breast tumors as well as masses in the prostate and hepatobiliary tract.
We use radiofrequency or cryoablation to treat some lung, liver, kidney, and bone tumors. CT imaging is used to guide the placement of a needle into the tumor, and cold or heat is then applied to destroy tumor cells. This technique requires no incisions and is effective for some patients who are not candidates for surgery and who have isolated tumors.
Vertebral fractures are a common and painful side effect of spine tumors. During vertebroplasty, a special bone cement is injected directly into a collapsed vertebra to stabilize the spine before surgery or radiation therapy. The cement may also serve as a marker in patients who are treated with image-guided radiation therapy.
This procedure is usually performed on an outpatient basis and can help improve patients’ mobility and quality of life.
Kyphoplasty is used to provide spinal support and relieve pain, particularly in patients with spine tumors. A small balloon called a tamp is inserted into the vertebra and inflated. This creates a space into which bone cement can be injected.
Embolization, a localized approach to destroying liver tumors, may be used to treat cancers that spread to the liver. During embolization, tiny particles are injected through a catheter that has been threaded into the hepatic artery, using the guidance of CT or ultrasound. The particles block blood flow to the tumor. This procedure may be used alone or in combination with surgery or chemotherapy.
The thermal and nonthermal focal therapies that we offer for select patients with small, localized prostate tumors can effectively destroy specific areas of cancer within the prostate while preserving normal prostate tissue and function. Side effects are often temporary and may be less severe than those associated with more-aggressive treatments.
Because focal therapy causes minimal injury to the prostate gland, it does not preclude further treatment with prostatectomy, radiation therapy, or additional focal treatment to another part of the gland, if necessary. Cancer that returns after radiation therapy may also be treated with additional focal therapy. Focal therapy is often performed on an outpatient basis or with a single overnight hospital stay.
We offer several focal therapy thermal techniques for prostate cancer treatment. These include:
High-Intensity Focused Ultrasound (HIFU) — HIFU uses the energy of intense sound waves, directed to the tumor with the guidance of MRI, to superheat and eliminate small tumors. HIFU is an attractive focal therapy approach because it is relatively noninvasive. The effectiveness of this treatment is monitored in real time, using MRI to measure the temperature within the prostate during therapy.
Interstitial Laser Therapy — A thin, flexible laser fiber is placed directly into the tumor, and MRI is used to guide the delivery of laser energy to the tumor with pinpoint precision. The laser superheats and destroys small prostate tumors.
Focal Cryoablation — A needle-thin probe delivers a solution that surrounds the tumor and kills it by freezing it at a very low temperature. Researchers at Memorial Sloan Kettering are evaluating the effectiveness of this new form of cryoablation.
We offer several focal therapy non-thermal techniques for prostate cancer. These include:
NanoKnife®/Irreversible Electroporation (IRE) — This technique uses a device called the NanoKnife to pass an electrical current through the tumor. The electricity creates very tiny pores in tumor cells, leading to cell death. Ultrasound or CT is used as a guide to focus the current precisely on the tumor, sparing blood vessels and other tissues.
Vascular Targeted Photodynamic Therapy (VTP) — A drug that destroys tumor cells and the blood vessels that support them is given intravenously and moves to the inside of the tumor. The drug is activated by exposing it to light of a very specific wavelength, which is delivered to the tumor site with specially designed fibers placed within the prostate.