Jose’s Story about Laryngeal Cancer
In July 2005, Jose’s sore throat and persistent hoarseness prompted him to call the doctor. When a biopsy revealed early-stage laryngeal cancer, Jose chose to fly across the country from Arizona to New York for treatment. At Memorial Sloan Kettering, he received a six-week course of external-beam radiation therapy.

Jose
In the spring of 2005, Jose began to experience persistent hoarseness that didn’t seem to be related to any particular condition, such as a cold or flu. Although he was never a heavy smoker, Jose, then 51, had quit smoking cigarettes three years earlier but continued to smoke three to four cigars each week.
“I thought I would stop smoking the cigars for awhile, and the hoarseness would clear itself up,” Jose recalls. “It diminished but it never went away.” When the hoarseness continued into July, Jose, who lives in Arizona, got a referral to an otolaryngologist (a doctor who specializes in treating diseases of the ear, nose, and throat) in nearby Phoenix.
After performing a physical examination of Jose’s head and neck, the doctor used what’s called an endoscope, a flexible lighted tube with a lens on its tip, to examine his throat. Looking through the lens, the doctor was able to examine deep inside Jose’s throat to see what was causing the hoarseness.
As he removed the endoscope, the doctor told Jose that he could see some white spots on his left vocal cord that might indicate cancer. But he would need to remove some of the tissue for a biopsy to make a definitive diagnosis.
Waiting for the Results
The biopsy was performed by the doctor the following week. While waiting on the results, Jose, his wife, and daughter, went on a previously planned trip to Chicago.
Around this time, Jose began to keep a personal journal of his possible diagnosis as a way to stay calm, as well as to help him remember what the doctors told him. A few days after returning from the trip, he wrote: “I tried my best to enjoy every moment but I was edgy at times and scared at others. My throat hurt a bit but my hoarseness seemed improved. I waited patiently for the results and prayed that I’d be cancer-free.”
The moment they returned home from the trip, Jose called the doctor’s office to find out about his biopsy results. The receptionist told him that they did have Jose’s results, but that his doctor had gone on a week-long vacation. Because they couldn’t tell him the results over the phone, this meant he would have to wait another agonizing week to find out what the biopsy showed.
“I was on pins and needles trying to figure out what was going on. I lost it,” he says, remembering. After a very frustrating conversation, the receptionist finally agreed to get him an appointment with another doctor in the same practice the following day.
Diagnosis & Initial Misinformation
The next day, the doctor read without emotion from the chart and told Jose that he had stage I squamous cell carcinoma of the left vocal cord. (Squamous cell carcinoma begins in thin, flat cells called squamous cells that are found in many places in the body, including the passages of the respiratory tracts. The vocal cord sits at the top of the trachea — the tract that leads to the lungs and prevents food from entering the lungs. The vocal cords, which are two bands of muscle, are found within the larynx and are used to make speech.)
Although he did not explain why, the doctor — who seemed to Jose to be “a real rookie” — told him that he was not a good candidate for laser surgery, which is the minimally invasive surgical procedure commonly used to treat early-stage laryngeal cancer. He went on to say that radiation therapy might be an option, but that “it only works in about 80 percent of patients.” He also mentioned that if radiation did not work and surgery was not deemed possible, a tracheotomy — when a hole is cut through the neck and into the wind pipe — might be necessary to allow breathing.
“To top it all off,” Jose wrote, “he mentioned that if we chose radiation and it failed, the cancer could spread and there was a potential of my larynx having to be entirely removed, leaving me speaking through a [mechanical] voice box.”
The thought that he would need an artificial voice box was horrifying to Jose. Hearing this information from the doctor, he couldn’t believe how limited his treatment options seemed to be, not to mention how unfeeling the doctor was. Jose and his wife looked at one another, both knowing that they did not want this team of doctors to treat him. On their way out, he requested a copy of his file, including lab results.
Next Step: Trying to Find a New Doctor
When they got home, Jose called his 27-year-old daughter, who lived in New York City, and told her he had cancer. He remembers saying, “We can’t feel sorry for ourselves. We’ve got to attack it and find out where we can go to get this treated.”
Jose and his wife began researching early-stage laryngeal cancer on the Internet, looking into the various treatments options available, as well as physicians. In addition to looking locally, Jose was open to exploring doctors and hospitals in New York City who specialized in treating this type of cancer because he had grown up there and still had family and friends in the area.
Jose and his wife found two surgeons who looked like good options. One who practiced locally in Arizona was associated with the Mayo Clinic. The other was Snehal Patel, a head and neck surgeon at Memorial Sloan Kettering Cancer Center, who had trained with one of the surgeons who developed the technique of laser surgery to treat laryngeal cancer.
They scheduled back-to-back appointments with the surgeons — their first meeting would be with the doctor in Arizona. Jose would fly to New York to meet with Dr. Patel the following day.
After performing “a very cursory examination” consisting of a quick look down Jose’s throat without an endoscope, the Arizona doctor said that Jose was a candidate for laser surgery and he would like to operate as soon as possible. Jose and his wife asked about other options, such as radiation therapy, but the doctor discouraged radiation, saying that it would be costly and time-consuming.
When they mentioned that they were meeting the following day with a surgeon from Memorial Sloan Kettering, the doctor became defensive. As they were leaving, the doctor said, “’If you want to do this closer to home, here’s my card. And if not, that’s fine. I’ve got plenty of business.’ My wife and I couldn’t get out of there fast enough,” Jose remembered.
They hoped Dr. Patel would provide more answers.
An End to Misinformation
Jose brought his older daughter with him to his first appointment with Dr. Patel. Dr. Patel used a high-tech endoscope that took pictures and projected them onto a large monitor so that Jose could see exactly what the doctor was seeing. Dr. Patel pointed out the differences between the healthy and cancerous vocal cords to Jose, who was fixated on the sight of the tumor. As he later wrote in his journal, “I had never seen my lesion nor had anyone explained what the options for treatment were. Right from the start, I realized that I was in the best hands at Memorial Sloan Kettering.”
After the examination, Dr. Patel, who was “very gentle, very human,” sat with Jose and talked with him for quite some time. “I was hoping that Dr. Patel would tell me that laser surgery was possible,” he wrote in his journal, “but instead he stepped outside of his surgeon role. He asked me what kind of work I did and if I used my voice a lot.” A consultant by trade, Jose said that yes, he used his voice a great deal, so it was important for him to keep his voice.
Hearing this, Dr. Patel told him that he would recommend radiation therapy as opposed to throat surgery. To surgically remove the tumor, Dr. Patel explained, he would have to remove the cancerous region as well as some of the surrounding healthy tissue — meaning that there was a high probability that his voice would be affected. Radiation therapy, he said, was highly successful in treating early-stage laryngeal cancer and would give him the least amount of damage to his voice.
Jose told Dr. Patel about the contradictory information the other doctors had given him, including the worst-case scenario of the tracheotomy. Dr. Patel reassured him that a complete removal of the larynx would not happen “under any circumstances.” For the first time since his diagnosis, Jose began to trust the information he was hearing. Reflecting on the exchange, he later wrote, “Here was a surgeon who was not quick-on-the-draw to cut. Instead he was looking out for the best interest of the patient. That was uplifting.”
After Jose told Dr. Patel that he wanted to “run with it,” the doctor called Memorial Sloan Kettering radiation oncologist Nancy Lee, who agreed to see him later that afternoon. Jose wrote, “He told me that I would love Dr. Lee — that she was a little dynamo.”
“You Are Going to Be Fine”
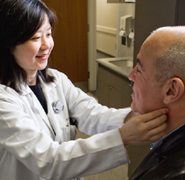
Personalized Care—Radiation oncologist Nancy Lee examines Jose
A few hours later, Jose was waiting in the appointment room when Dr. Lee walked in with seven of her fellows-in-training. He wrote in his journal, “The first thing she did was to come over and touch my arm. She said to me, ’Don’t worry. You have a very curable form of cancer, and if you decide to be treated here, we’re going to cure you. You are going to be fine.’ It was like a catharsis for me to hear her say that.”
Dr. Lee and her fellows performed another endoscopy. After the procedure, Dr. Lee told him that she agreed with Dr. Patel’s assessment, saying that radiation therapy was 95 percent successful with his type and stage of cancer.
Dr. Lee wanted to begin treatment immediately and estimated that Jose would need external beam radiation therapy five days a week for a total of 28 treatments. (External beam radiation therapy is a type of radiation therapy that uses a machine to aim high-energy rays at the cancer from outside of the body. Radiation is targeted at tumors with great precision, affecting only the cancerous regions and sparing the surrounding healthy tissues.)
“I loved her urgency and her confident resolve,” Jose recalls later in his journal. “Dr. Patel had been right — she was a dynamo.”
Dr. Lee recognized that receiving weeks of treatment in New York City would probably be inconvenient to a resident of Arizona. Although she was unfamiliar with the hospitals in Arizona, she offered to help him find a doctor closer to home who she felt could effectively oversee his treatment, which was a gesture that Jose appreciated. He was almost sure that he wanted to come to Memorial Sloan Kettering, but he also wanted to talk it over with his wife before making a decision.
Working Out the Details
After Jose briefed his wife on the appointment, they quickly agreed that he should pursue treatment at Memorial Sloan Kettering. “Given what I had experienced up until then, there was no comparison between the expertise of the doctors and the treatment I had received [there],” Jose says. “I knew it would be difficult for us to be apart for that amount of time, but we felt this was the best chance we had of getting me cured. And that was most important in the long run.”
At the same time, the logistics of his extended stay in New York came together. A friend of Jose’s offered him a spare bedroom in an apartment on the Upper West Side of Manhattan. This would mean that he would have an easy commute to the hospital for treatments, as well as a comfortable place to stay while away from his family. In addition, his daughter got him a free one-month pass to a gym close to the apartment so he could continue his workout regimen. He looked forward to being able to spend time with his older daughter, his parents, and other family and friends during his sojourn in New York.
Beginning Treatment in August
The following week, Jose returned to New York for a surgical procedure that would “map” his vocal cords and surrounding areas before any treatment began and changes in the tumor’s shape occurred. This precaution was taken in case the radiation was not successful and surgery became necessary sometime in the future. The only unpleasant side effect Jose experienced afterwards was a feeling of numbness at the tip of his tongue that lasted a few months and subsequently went away.
Before radiation treatment could begin, the radiation oncology team created a special face mask for Jose that he would wear during each treatment. The mask would keep his face and neck in the same place while radiation was administered to ensure that the radiation was targeting the cancer cells with the greatest precision. “The mask goes on like a cold liquid and then dries and becomes warm,” he says. “It’s like if somebody was putting on a mask in a spa. It fits skin-tight and it needs to dry entirely on your face.”
Describing his daily therapy, he wrote, “It is unnatural and somewhat unpleasant to have your head strapped down, but necessary to remain in the precise position at all times. [The radiation oncologist and technicians] are making sure they are concentrating the radiation in the area where the lesion is at its worst. So your head can’t move.”
Jose’s Daily Routine
For six weeks, Jose had radiation treatments at Memorial Hospital. He would arrive for his appointment, change into a robe, and sit in a waiting room until his name was called. “Treatment would take all of five minutes,” he says. “I had to hold my breath and not swallow. It takes a minute or so, maybe less, on the one side. Then they click off, change the ’gun’ and put it on the other side.” They radiated both sides, just in case any of the cancerous cells had spread to the other cord.
With each passing day, Jose’s throat became increasingly sore. Swallowing also became harder. Other than those side effects, he still felt pretty good. After his daily treatment, he spent his free time exercising at the gym, writing in his journal, going to the movies, and visiting family and friends.
Each treatment was carefully monitored by Dr. Lee, who would make slight changes to the location and dosage of radiation. Each week, an x-ray and endoscopy was taken of his vocal cord to measure the treatment’s progress. Modifications were made a few times during the course of treatment. As Jose wrote, “She is such a perfectionist — she was changing things by percentages of millimeters. Every week we have a 0.2 millimeter adjustment. I don’t even know what 0.2 millimeter is!”
Throughout the course of treatment, exercise was very important to Jose. He was able to continue his workouts every day until the final weeks of treatment. “When I got my diagnosis, exercising was always a way for me to feel that if the rest of my body was strong, there was no way this was going to beat me,” he says. “The exercise was a therapy for me — it was a psychological force for me to think of myself as not being sick.”
Looking back on the weeks of treatment, Jose says, “It was relatively pleasant. I missed my family but I wasn’t in unfamiliar places.” It was a boost to his spirits when his wife and three-year-old daughter came to visit him halfway through the course of treatment. He brought them to the hospital to meet Dr. Lee and watch one of his treatment sessions. He was proud of seeing how his daughter handled seeing him undergo treatment. As he wrote in his journal, “I was scared it might freak her out but she took it all in stride. We told her the mask was a Halloween mask. She was not fazed at all.”
Finally Hitting a Wall
Toward the fourth week of treatment, Jose’s throat was so inflamed that eating hard foods became difficult. “Eventually I was only eating yogurts and frappuccinos and apple sauce and those kinds of things,” he recalls. As his neck grew red and raw, he was told not to shave with a razor until the end of his therapy. He grew a beard.
Describing how it felt to “hit the wall,” Jose wrote, “My head was heavy and my eyes bleary and droopy.” Trying not to get frustrated, he would remember that Dr. Lee had warned him that this would happen. “Dr. Lee said that the healing would not be a linear progression but rather more like two steps forward and one step back.”
Despite these physical setbacks, his treatment continued to go well and his cancer was diminishing. After four weeks of treatment, Dr. Lee told him the cancer was almost gone and he was not in the 5 percent of patients for whom radiation does not work. As he wrote, “I was happy to hear that. My worst fear was that after all the sacrifice of time and distance from my family I would not respond to the treatment.”
Heading Home
After 28 sessions of radiation therapy, Jose’s last treatment was on October 10, 2005, and he flew back to Arizona to rejoin his wife and daughter. He scheduled a follow-up appointment with Dr. Lee two months later in early December.
Dr. Lee estimated that it would take about eight weeks for his throat and neck to recover completely. A few weeks after returning home, he wrote in his journal, “The recovery is happening just like Dr. Lee said it would, one day better and the next day worse. I lose my patience sometimes thinking it should all be smoother and in moments of weakness let fear creep into my mind thinking the cancer is not gone.”
Jose returned to New York that December for his follow-up appointment with Dr. Lee. She told him that his throat continued to look better and better. These appointments continued every two months, and Jose celebrated his two-year anniversary in October 2007. Eventually the appointments stretched to every three months and now, every four months.
Since then, Jose has begun alternating check-ups with a former clinical resident of Dr. Lee’s at Memorial Sloan Kettering named Jonathan Ashman. Dr. Ashman moved out to Arizona after his training was complete to join Arizona Oncology Services located in Phoenix. “Dr. Ashman told me in November, ’It looks so good that I can’t tell you ever had anything. It looks perfectly normal.’”
The Danger of Misinformation
Looking back on his experience, Jose feels incredibly lucky that he was able to make the connection with Memorial Sloan Kettering. “I had gotten so much misinformation,” he says. “For every Dr. Patel and Dr. Lee there are a hundred other doctors that are like the one I was dealing with in Arizona. They just don’t know any better because they aren’t willing to keep up with knowing what the latest cure or treatment is and what exactly the success rate of the newest treatment is.”
“Only at Sloan Kettering, and potentially a handful of other places in the United States, do you have this kind of team of doctors.”


