Our Mission
To provide training to develop independent, highly skilled, and confident Critical Care Medicine (CCM) attending physicians who can effectively lead teams, collaborate across subspecialties and mentor the next generation of critical care specialists. We aim to develop future leaders capable of supervising critical care units, research, and educational programs.
Our fellowship is unique because our intensivists have training in diverse specialties. Our intensivists come from backgrounds in internal medicine, pulmonary medicine, anesthesiology, infectious disease, nephrology, and palliative medicine.
Critical Care Medicine at MSK
For more than three decades, Memorial Sloan Kettering Cancer Center (MSK) has been ranked among the top two cancer institutions in the United States, renowned around the world not only for exceptional patient care but also for its latest diagnostics, surgical expertise, excellence in radiation and chemotherapy, nursing, and supportive care.
MSK has one of the world’s most recognized cancer research programs, offering hope to thousands of people with rare or late-stage cancer.
Our faculty, fellows, advanced practice providers (nurse practitioners and physician assistants), and residents provide daily care to patients in our modern 20-bed adult medical-surgical Intensive Care Unit (ICU) and throughout our 514-bed inpatient hospital.
Two teams of clinicians, a house staff team, and an advanced practitioner team supervised by board-certified intensivists, care for patients admitted to the ICU. A Consultation/Rapid Response Team provides consults and rapid response visits for acutely ill inpatients throughout MSK, and a Critical Care Center Stepdown Team cares for patients in the Medical Step-down Unit (SDU) and provides consultation in the Neurological Advanced Care Unit.
Our ICU maintains a high level of activity throughout the year. In 2024, a total of 1,305 patients were treated in the ICU, while 595 patients received care in the SDU. Additionally, the department received 1,841 requests for CCM consultations and managed 2,611 rapid response calls during the same period.
Critical Care Medicine Faculty and Staff
Our current CCM faculty consists of 21 intensivists with training in internal medicine, pulmonary, anesthesiology, infectious disease, nephrology, and palliative medicine. Our CCM faculty have appointments in the Departments of Medicine and Anesthesiology at New York-Presbyterian/Weill Cornell Medical Center (NYP-Cornell).
In addition to the CCM fellows, the ICU is staffed with anesthesiology residents from NYPH-Cornell. Medical students from Weill Cornell Medical College and other medical schools rotate through the ICU. Our advanced practice provider team includes 42 NPs and PAs, and our respiratory therapy team includes 60 therapists.
Additionally, the CCM Service has a dedicated research nurse, nutritionist, social worker, patient care representative, computer programmer, and informatics specialist.
Critical Care Medicine Fellowship Program
The CCM fellowship has 12 fellows each year, with a mix of one- and two-year fellows. Each fellow’s educational background usually includes primary specialties in internal and emergency medicine and secondary internal medicine subspecialties in pulmonary, nephrology, and infectious disease. The academic year is divided into 13 4-week blocks. This includes 1 block of vacation and 12 blocks of clinical rotations.
One-year CCM fellows spend a total of 12 blocks of clinical rotations at four separate hospitals: MSK (8 blocks), NYP-Cornell and Columbia University Medical Center for experience in cardiothoracic surgery and mechanical circulatory support (1 block), surgical critical care (1 block), and the New York Presbyterian Queens for a community-based medical ICU rotation (1 block) and neurocritical care (1 block).
Two-year CCM fellows spend clinical time as outlined above, and the second year is designed to give the senior fellows more opportunities for directing the ICUs and mentoring first-year fellows, as well as elective time to expand their clinical experience. Two blocks of dedicated research time are provided to complete research projects initiated during the first year and expand their clinical experiences. Available clinical electives are listed below.
Fellows participate in research, present at local and national conferences, publish peer-reviewed articles, and contribute to patient safety and quality-improvement projects.
Curriculum
Didactic Sessions
- Monthly conferences are categorized by organ systems and presented twice a week by attending physicians from MSK, regional institutions (NYP/ Weill Cornell Medical Center, NYP Columbia Medical Center, The Mount Sinai Hospital and others) and national institutions such as Cleveland Clinic, MD Anderson Cancer Center, and others.
- Ground rounds/Journal clubs presented by CCM and PCCM Fellows
- Weekly ventilators workshops
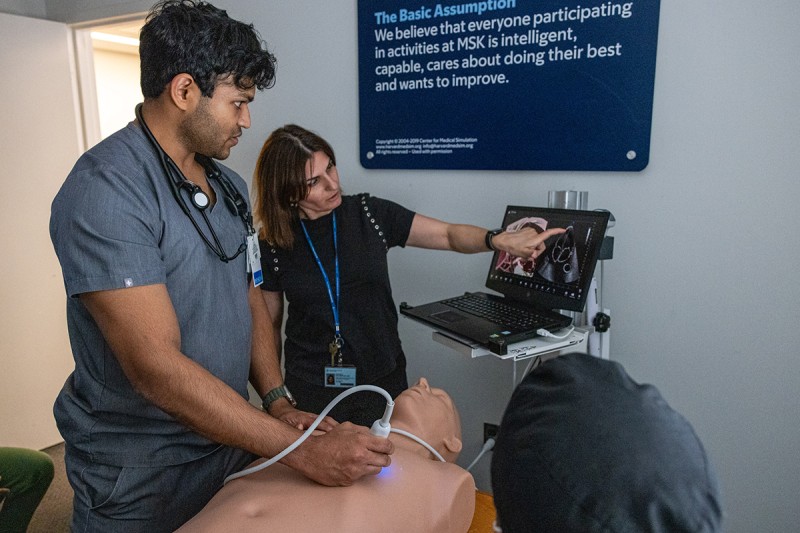
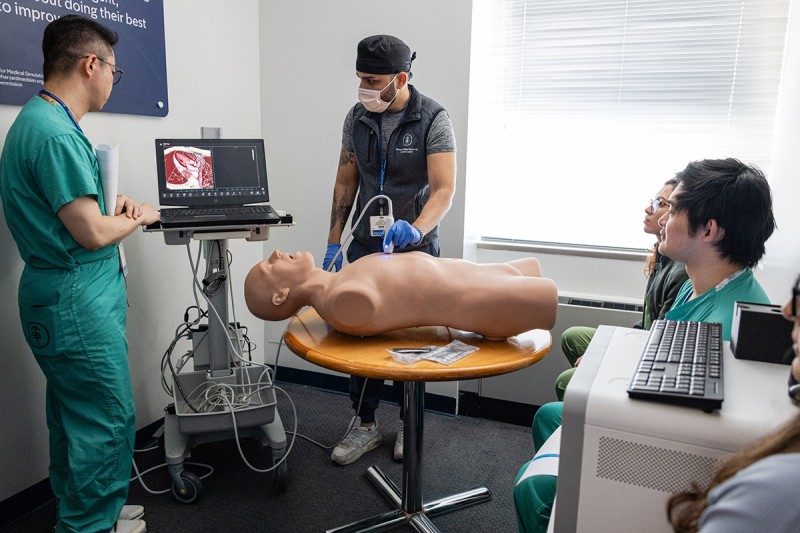
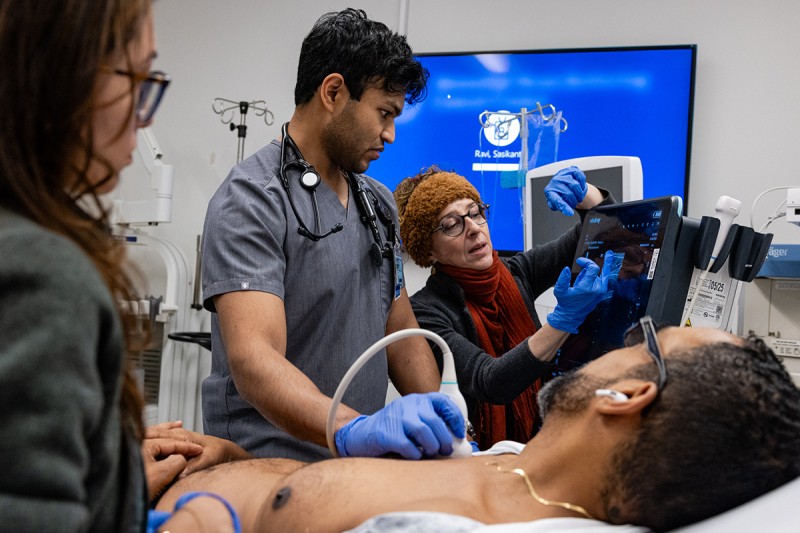
- Weekly ultrasound workshops (including advanced cardiac, abdominal, and thoracic ultrasounds)
- Weekly board review sessions
- Chief Seminars are held quarterly to provide an open forum discussion with the Chief of Service.
- The Career Development Curriculum aims to guide fellows through the stages of job hunting and support career growth.
Simulation and Workshops
- Procedural workshops
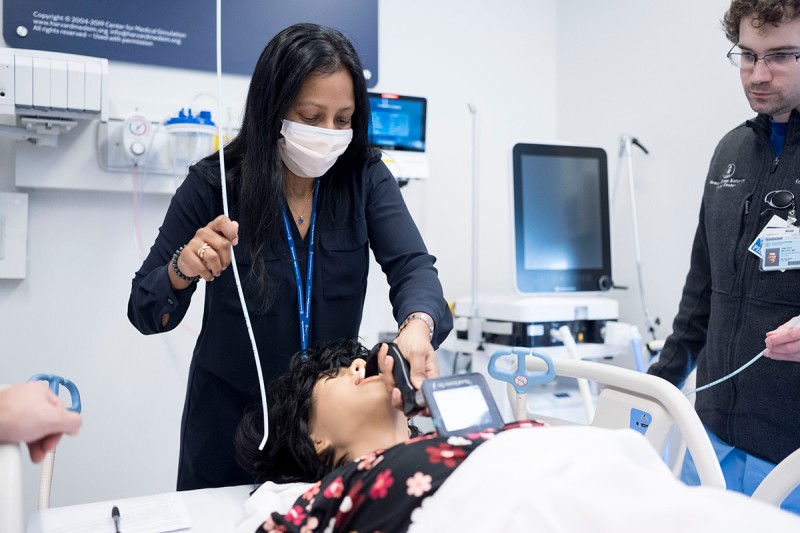
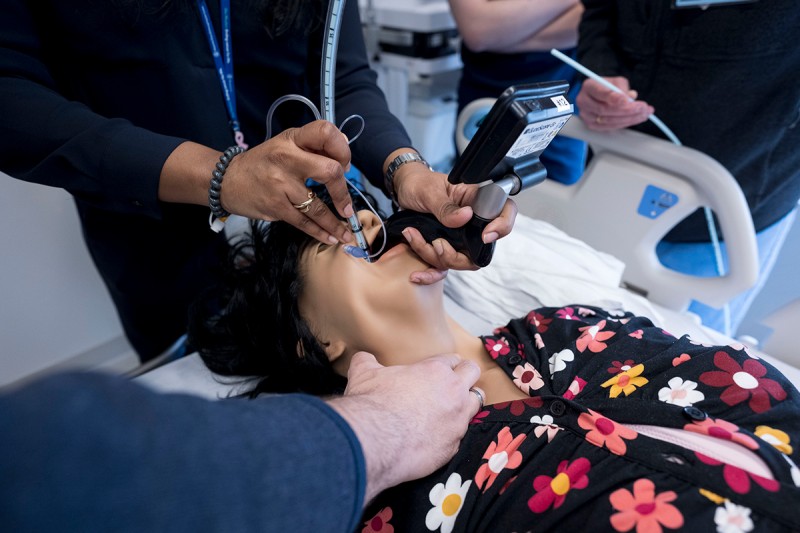
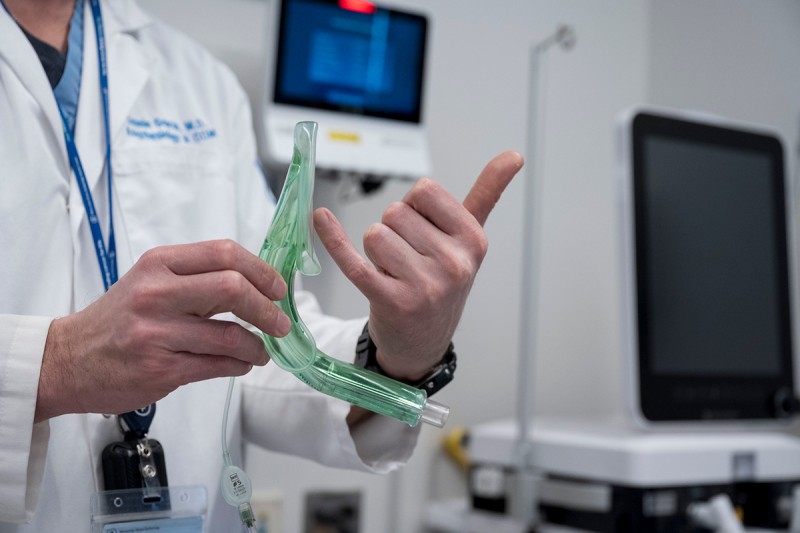
- Basic and advanced airway workshops
- Cardiopulmonary resuscitation workshop
- Bronchoscopy workshop
- Ultrasound workshop
- Critical Care case scenarios
-
Communication workshop designed to guide fellows about supportive and palliative care, and end of life discussions
Clinical Electives
- Operating room (one-month rotation aimed to gain expertise in airway management)
- Nutrition
- Infectious disease
- Nephrology
- Interventional pulmonology
- Pulmonology
- Echocardiogram
Research
The CCM Service conducts clinical trials in sepsis/septic shock, pneumonia, and acute respiratory distress syndrome as well as collaborative studies with national and international critical care networks.
The CCM Service also performs “homegrown” projects exploring novel biomarkers in the critically ill, outcome studies of chemotherapy, and ethics consultations in an oncologic ICU, rapid response teams, and ICU readmissions.
Our faculty includes experts in chimeric antigen receptor (CAR) T cell therapy complications, immune checkpoint inhibitor complications requiring critical care, sepsis, integrated critical care organizations, use and cost of CCM in the United States, and ICU design.
Campuses for Clinical Rotations
The Surgical Intensive Care Unit at New York-Presbyterian/Weill Cornell Medical Center is a 20-bed facility that focuses on caring for patients with severe injuries, those requiring intensive care following complex surgeries—including post-liver transplant patients, and individuals facing other life-threatening conditions. The trauma center at this medical center holds a Level I adult and Level II pediatric trauma designation from the American College of Surgeons, acknowledging its capacity to deliver top-tier care, particularly in critical and complicated cases.
The Cardiothoracic Intensive Care Unit (CTICU) is a 20-bed ICU that focuses on caring for postoperative cardiac and thoracic surgical patients. The New York-Presbyterian/Weill Cornell Medical Center Anesthesiology Critical Care Medicine team provides critical care services to ~1,000 cardiac surgery patients per year and to a portion of the >1,200 thoracic surgery cases performed annually. They serve a diverse and complex patient population that presents with coronary artery disease, aortic pathology, valvulopathies, congenital cardiac malformations, lung and esophageal pathology, and/or heart failure. They manage the entire range of mechanical circulatory support devices including intra-aortic balloon pumps and ventricular assist devices, as well as patients who undergo heart transplantation. The CTICU is the only ICU at WCMC that cares for patients on ECMO. Their faculty consists of dedicated intensivists who staff the ICU 24 hours a day.
The Cardiothoracic Intensive Care Unit (CITICU) is a 31-bed unit dedicated to the care of post-surgical patients following procedures such as coronary artery bypass grafting (CABG), valve repair or replacement, adult congenital defect correction, lung transplantation, thoracoabdominal surgeries, pulmonary thromboendarterectomy, and mechanical circulatory support including VADs (HeartMate 3, RVAD, Impella) and ECMO in all configurations. As a high-volume referral center, it regularly receives complex cases from across the tri-state area, reflecting its reputation for managing critically ill and high-acuity patients.
Neurocritical Intensive Care Unit is an 8-bed department caring for a very diverse population with large proportion of Chinese, Korean, and Russian speaking patients. NYP Queens NICU is the only ICU with a full body Computer Tomography scanner within the unit and with video EEG monitoring installed directly in every room. The unit cares for patients with strokes—both ischemic and hemorrhagic, as well as traumatic brain injuries, seizures, and complicated post-operative conditions.
The NYP Medical ICU is a 20-bed unit caring for a broad range of critically ill medical patients in the highly diverse neighborhood of Queens. Our fellows rotate here to gain experience at a community hospital caring for a broad range of medical pathologies more commonly seen in the non-oncologic setting.
Postgraduate Opportunities
Our two-year internal medicine or emergency medicine–CCM and one-year internal medicine subspecialty-trained fellows have secured positions as critical care attendings in community teaching and university-affiliated hospitals throughout the country.
Over 200 fellows have completed fellowship training since 2000. Several pulmonary–CCM graduates have proceeded to pursue additional fellowships in sleep medicine and interventional pulmonology at prestigious medical centers including the Cleveland Clinic, Johns Hopkins, Mayo Clinic, and Henry Ford Hospital.
Additionally, our graduates have become ICU directors, associate program directors of residency or fellowship programs, and departmental chairs as well as intensivists in large hospitals or private groups.
Application Process
Who Can Apply?
The CCM Service welcomes applicants trained in internal medicine and medical subspecialties (pulmonary, renal, and infectious disease) and emergency medicine.
Our training program is designed to equip trainees with a holistic approach to Critical Care Medicine where they feel comfortable and competent to care for critically ill patients with various diseases.
Our faculty is dedicated to teaching and providing advanced subspecialty training, and our trainees are highly qualified candidates who come from across the United States for this unique learning experience.
We appreciate your interest in our program and encourage you to apply to become part of our team.
Length of Program
1 or 2 years
Number of Positions
12
Program Eligibility
To apply, you must have a minimum of three years of ACGME residency training in internal medicine or emergency medicine in the United States.
How to Apply
Our program participates in the Electronic Residency Application Service (ERAS). ERAS will be used to transmit applications, letters of recommendation, transcripts, and other supporting credentials from applicants. We will be participating in program signaling. To apply for our fellowship, please complete an application through ERAS.
Interviews are conducted from August through early October.
The following items must be in your ERAS Common Application before your application will be reviewed:
- Three letters of recommendation and USMLE results
- Personal statement
- Research experience/publications/presentations
All CCM trainees are selected through the National Resident Matching Program (NRMP). To participate in this program, you must register online through the NRMP service. For additional information, please contact our program coordinator, Erickson Pinales.
Contact Us
Program Director

GME Coordinator
Erickson Pinales
Graduate Medical Education Coordinator
Department of Anesthesiology & Critical Care Medicine
Memorial Sloan Kettering Cancer Center
1275 York Avenue New York, NY 10065
Phone: 212-639-6674
Email: [email protected]