Uveal melanoma (also called ocular melanoma) is a cancer that forms in the eye. Although rare, this malignancy is often fatal when it spreads to other parts of the body, which happens in about half of all cases.
Memorial Sloan Kettering medical oncologist Alexander Shoushtari answers common questions about uveal melanoma and explains why treatment for this disease could soon improve dramatically for many people.
Why is this type of cancer called melanoma if it arises in the eye?
All melanomas share a common cell of origin, which is the melanocyte. These cells produce a pigment, called melanin, that makes hair, skin, and eyes appear darker. Most people are familiar with melanin in the skin, which protects it from damage by ultraviolet radiation. In the eyes, melanin also provides protection from the sun and determines eye color. All types of melanoma develop when melanocytes start to grow and divide uncontrollably. Uveal melanoma arises in the uveal tract, which is the middle layer of the wall of the eye.
How is uveal melanoma different from skin melanoma?
Most skin melanomas are triggered by exposure to sun and ultraviolet radiation, which causes DNA mutations. Compared with other cancer types, skin melanomas have very high rates of mutation. This provides more targets for immunotherapy drugs called checkpoint inhibitors, which have worked very well against skin melanomas. The mutations driving uveal melanomas are generally not caused by sun damage and are far fewer in number. Because uveal melanomas don’t have as many mutations to target with immunotherapy, those treatments are generally less effective than they are for skin melanomas.
How are uveal melanomas diagnosed?
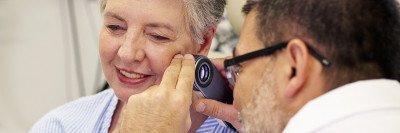
Usually someone will notice something wrong with their vision. It doesn’t typically cause pain. Depending exactly where the cancer is in the eye, people may describe a fluttering sensation or a feeling of drapes falling over their field of vision. It’s diagnosed through a dilated eye exam by an ophthalmologist. Usually the diagnosis can be made without a biopsy, which would be difficult to obtain anyway.
People with light-colored eyes seem to be at higher risk, as well as those who are Caucasian or of Western European ancestry. Even in this population, uveal melanoma is still very rare.
What has been the standard treatment for uveal melanomas?
Surgery and radiation can be used to remove or destroy a tumor directly. When surgery is done, it usually involves removing the eye. Radiation can often treat the tumor while preserving some vision. If the disease has spread, it becomes more difficult to treat. These cancers tend to go to the liver for reasons we don’t fully understand. Our interventional radiologists are very skilled at using minimally invasive methods to choke off the blood supply to tumors in the liver using a procedure called embolization. They often can treat these liver metastases to buy time for a patient to join a clinical trial.
Overall, for metastatic uveal melanoma, we’ve tried a variety of drugs with very modest success. The average survival time for metastatic uveal melanoma is between one and two years. Better treatments are urgently needed.
What are potential new treatments for uveal melanoma?
There’s a new drug called tebentafusp that showed very promising results in a large phase III clinical trial involving people with metastatic uveal melanoma. I am proud to be one of the most experienced investigators in the world using this drug, and we at MSK enrolled a lot of people in this trial. In the study, patients receiving tebentafusp had almost half the risk of death compared with those receiving a different drug — either a checkpoint inhibitor or chemotherapy. These results made big news when they were presented in April 2021 at the American Association for Cancer Research annual meeting.
Tebentafusp enables immune T cells to recognize and target the uveal melanoma cells by homing in on a protein on the cancer cells called gp100. The T cells normally ignore the protein, but tebentafusp acts as matchmaker — like forcing an introduction at an awkward dinner party — to make the immune cell recognize the cancer cell as a threat.
One limitation of tebentafusp is that it works only in people with a certain HLA type. HLAs, or human leukocyte antigens, are proteins found on most cells in your body. There are three general HLA groups, and HLA matching is used to connect patients and donors for blood or marrow transplants. About 40% to 50% of people with Western European ancestry have the HLA type needed for tebentafusp.
Even though this drug may help only half of patients, it’s very exciting. Tebentafusp is the first systemic therapy proven to help people live longer with uveal melanoma. It’s shattering the notion that “there’s not much that can be done” when this disease spreads. It’s also a symbol of how fast cancer research is progressing.
Are there other new uveal melanoma treatments being investigated at MSK?
MSK is one of the most active centers in the world for uveal melanoma trials. In addition to the tebentafusp study, we have trials open to people with specific mutations detected by MSK-IMPACT™. (MSK-IMPACT is a tumor-sequencing test available to MSK patients.) When we open trials testing molecularly targeted therapies, we fill them up quickly. For a rare cancer like uveal melanoma, a big, specialized center such as MSK can make a big difference in someone’s care because we can offer so much beyond standard therapies.