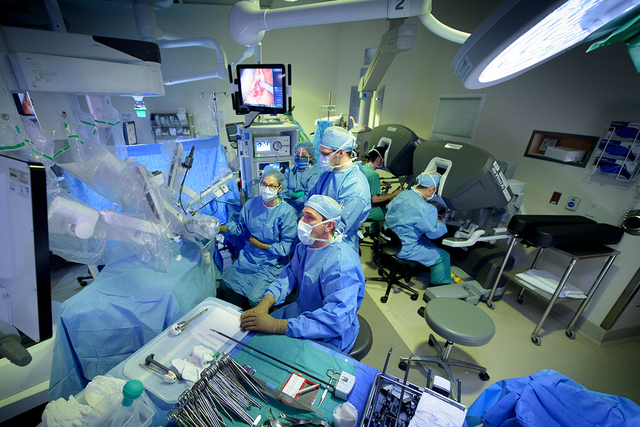
On February 28, the US Food and Drug Administration released a statement cautioning about the use of robotic surgery in mastectomy and other cancer surgeries.
In the notice, Terri Cornelison, assistant director for women’s health in the FDA’s Center for Devices and Radiological Health, said that “the use of robotically assisted surgical devices for any cancer-related surgery has not been granted marketing authorization by the agency, and therefore the survival benefits to patients when compared to traditional surgery have not been established.”

Robot-assisted surgery is an extension of laparoscopic surgery, a minimally invasive approach that allows surgeons to perform operations using cameras and instruments inserted through small incisions. The robot adds improved vision and control to laparoscopic procedures. Its enhancements include the ability to see things in high definition and three dimensions as well as robotic arms that can be precisely controlled.
In an interview, Jeffrey Drebin, Chair of Memorial Sloan Kettering’s Department of Surgery, spoke about what this FDA advisory means for patients.
Why do you think this statement was released?
In November 2018, a study published in the New England Journal of Medicine and led by researchers from University of Texas MD Anderson Cancer Center reported that in women treated for early-stage cervical cancer, traditional open surgeries were associated with a lower risk of the cancer coming back compared with minimally invasive surgical procedures. This was true whether the surgeon used a robot or other laparoscopic techniques, so these findings were really not about the robot per se.
Additionally, more and more hospitals are beginning to use surgical robots. This is due in part to the trainings offered by the companies that make them. The FDA may have felt they needed to inform people on what is known about these procedures.
What are the potential benefits of robotic surgery?
For patients, the main benefit of the robot, or of any laparoscopic procedure, is smaller incisions. What comes along with these smaller incisions is the potential for less pain after the operation, less blood loss, a shorter hospital stay, and a quicker recovery.
But cancer surgery is very different from other operations that may be done minimally invasively, like a gallbladder removal or a hip replacement. With a cancer surgery, the size of the incision is not the most important thing for patients. The most important thing is giving patients the best chance of being cured of their cancer.
If that can be done with smaller incisions and less discomfort, then that’s a plus. But if the trade-off is a higher risk that the cancer will come back, that’s not a trade-off I would choose, or that most patients would choose.
What is MSK’s approach to using robotic surgery?
One of the questions the NEJM study didn’t look at was the experience level of the surgeons. It’s very clear that what makes the biggest difference in the outcome of any cancer surgery is the surgeon’s level of experience and training. If one of our surgeons offers a patient the option of robotic surgery, it’s because we have a really good idea that this is going to be better for that individual patient.
For many types of cancer, randomized, controlled trials that have shown that the outcomes for minimally invasive surgery are the same as open surgery in terms of cancer-related death. The trials also found that outcomes such as pain, bleeding, and length of hospital stay are often better. We’ve studied this in prostate cancer, colon cancer, lung cancer, head and neck cancers, and stomach cancer. For uterine cancer, outcomes for robotic hysterectomies are equivalent to open surgeries. We frequently offer robotic surgery to patients with many types of cancer when we believe it’s appropriate.
The FDA statement specifically mentions mastectomies performed with robotic techniques. MSK doesn’t currently offer this procedure, although some members of our team have talked about using it. Whether it ultimately turns out to benefit patients is something that would need to be studied in carefully designed trials over a period of time.
Why should someone choose MSK for cancer surgery?
Experience makes the biggest difference. The robot and other laparoscopic devices are really no different from a scalpel or a pair of forceps. They are all just tools.
The best surgeons use the right tool for the right case for each patient. They don’t simply use the same tool over and over. Surgeons at MSK are able to personalize the best approach for every patient because of the level of training and experience that we have with all of these techniques.








