This information explains the causes, diagnosis, and treatment of Barrett’s esophagus.
About Barrett’s Esophagus
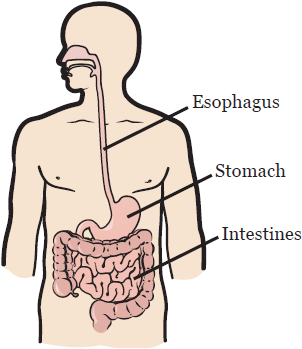
The esophagus is the tube that carries food and liquids from your mouth to your stomach (see Figure 1). If you have Barrett’s esophagus, the normal cells that line your esophagus are replaced by a type of cell not usually found in the esophagus. These new cells look more like the cells that line your intestines. This process is called intestinal metaplasia (meh-tuh-play-zhuh).
Having Barrett’s esophagus can increase your risk of getting esophageal cancer. Because of this risk, it’s important that you have regular medical check-ups and follow your treatment plan.
Causes and Risk Factors
The exact cause of Barrett’s esophagus isn’t known. Most people with Barrett’s esophagus have a history of having GERD. GERD is a disorder where the contents of your stomach flow back into your esophagus. It’s also called reflux. GERD can cause heartburn (a burning feeling in your throat or chest).
Over time, the acid and bile from your stomach damage the lining of your esophagus. Some people with a history of GERD can get Barrett’s esophagus if this damage is severe. For more information about GERD, read the resource Gastroesophageal Reflux Disease (GERD).
Most people who develop Barrett’s esophagus are:
- Older (over the age of 40)
- Male
- Caucasian
- Obese or overweight
Diagnosing Barrett’s Esophagus
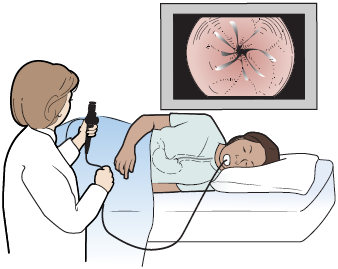
You’ll need to have an endoscopy procedure to diagnose Barrett’s esophagus. During the endoscopy, your healthcare provider will use a flexible tube called an endoscope to see the inside of your esophagus on a video monitor (see Figure 2).
Before the procedure, you’ll get anesthesia (medication to make you sleepy), so you won’t feel any discomfort. During your endoscopy, your healthcare provider will look for color changes in your esophagus. They will look for an orange color in the lower part of the esophagus. Your healthcare provider may do a biopsy by taking a sample of tissue from the lining of your esophagus in the area of orange color. This sample will be sent to MSK’s pathology department to look for intestinal metaplasia and precancerous tissue (tissue that may become cancer). If your sample has precancerous tissue, this is called dysplasia.
Treatment for Barrett’s Esophagus
Your treatment for Barrett’s esophagus will depend on whether or not you have dysplasia.
Treatment for no dysplasia
Medications
If you don’t have dysplasia, Barrett’s esophagus can be treated with the same medications used to treat GERD. These medications help reduce the acid in your stomach and relieve other symptoms you might have. They also may help prevent irritation to the esophagus. If medication doesn’t help your symptoms, you may need anti-reflux surgery. If you need this surgery, your healthcare provider will go over it with you.
Medication won’t cure Barrett’s esophagus, but it may help slow it down, so it doesn’t get worse. Even if you don’t have dysplasia, your healthcare provider will still need to monitor your condition, so you may need an endoscopy every few years.
Treatment for dysplasia
The treatment for Barrett’s esophagus will be different if you have dysplasia. Levels of dysplasia range from low-grade to high-grade. The level of dysplasia shows the cancer risk and helps your healthcare provider decide the type of treatment that you need.
- Low-grade dysplasia: If you have low-grade dysplasia, your cells show few precancerous changes. The risk of these cells turning into cancer is low. However, the more areas with low-grade dysplasia you have, the higher the risk of it turning into cancer.
- If you have high-grade dysplasia, your cells show many precancerous changes. The risk of these cells turning into cancer is very high.
The 2 main types of treatment for dysplasia are endoscopic treatments and surgery.
Endoscopic treatment
Endoscopic treatments kill or remove your abnormal tissue (pre-cancerous cells) without having to remove your esophagus. The types of endoscopic treatments include:
- Endoscopic mucosal resection (EMR): During an endoscopy, a salt solution may be injected under the abnormal tissue to raise it up. Then, the abnormal tissue is shaved off and sent to the pathologist for testing.
- Radiofrequency ablation (RFA): During this procedure, a special device is put down your esophagus. This device will give off short bursts of intense radio waves (heat) to kill the abnormal tissue.
- Cryoablation: During this procedure, very cold liquid and gas are put into your esophagus through an endoscope to freeze and kill the abnormal tissue.
- Photodynamic therapy (PDT): During this procedure, a medication that makes the abnormal cells sensitive to light is given through an injection (shot) into your vein. Then, red laser light is used to kill the abnormal tissue.
Surgery
Your healthcare provider may recommend that you have surgery to remove your esophagus or the damaged parts of it. This is called an esophagectomy. Your healthcare provider will tell you more about this procedure if you need to have it done.
Lifestyle Changes for Barrett’s Esophagus
If you have Barrett’s esophagus, your healthcare provider will recommend treatment and follow-up exams. You should also try to follow some lifestyle changes such as:
- Sitting up after meals. This can help you avoid having stomach acid back up into your esophagus.
- Avoiding food 2 to 3 hours before bedtime.
-
Avoiding foods that cause acid, such as:
- Foods and drinks with caffeine, such as coffee, teas, sodas, and chocolate
- Dairy products, such as milk
- Peppermint
- Tomatoes or tomato sauce
- Alcohol
- Sleeping with the head of your bed raised up, so your head is above your stomach. You can do this by putting blocks or wedges under your bed frame.
- Avoiding large, fatty meals, such as meals with fried foods or processed meats.
Talk to your healthcare provider if you have any questions.
Learn about our Health Information Policy.
