This information explains heart attacks, including signs of a heart attack. It also explains how heart attacks are diagnosed and treated.
About heart attacks
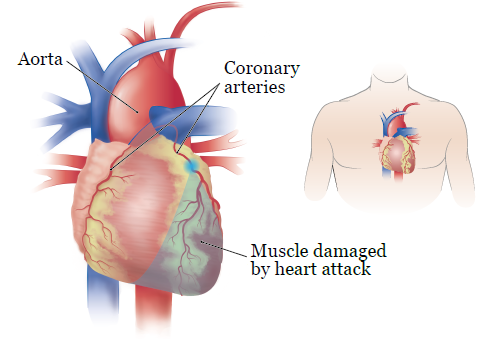
A heart attack, also known as myocardial infarction (MI), happens when one of your coronary arteries becomes blocked. The coronary arteries are the blood vessels that carry blood to your heart muscle. This can cause part of your heart muscle to weaken because blood can’t flow to it (see Figure 1). When part of your heart muscle is weakened, the heart muscle won’t work as well.
Common signs of a heart attack
The following are signs of heart attack. You may have 1 or more of these signs.
- Pain, pressure, or discomfort in your chest.
- Pain, tingling, or discomfort in your arms, back, neck, jaw, or stomach.
- Having trouble breathing while resting and when doing mild physical activity. This includes walking a few blocks or climbing a flight of stairs.
- Wheezing (a whistling or squeaking sound when you breathe).
- Sweating.
- Fast or uneven heartbeat.
- Feeling dizzy or lightheaded.
- Indigestion, a feeling of burning or discomfort in your upper abdomen (belly).
- Nausea (feeling like you’re going to throw up) with or without vomiting (throwing up). This is a common symptom of heart attacks in women.
If you think you’re having a heart attack, call 911 right away. Do not drive yourself to the hospital. Emergency medical technicians (EMTs) can start treating you on the way to your closest emergency room.
Ways to diagnose a heart attack
There are many different tests to diagnose a heart attack. When you arrive at the emergency room, you may have one or more of the following tests.
Electrocardiogram (EKG)
An electrocardiogram (ee-LEK-troh-KAR-dee-oh-gram) measures the electrical activity of your heart. This means it measures things such as how fast your heart is beating, and many other things. During this test, your healthcare provider will place sensors (electrodes) on your chest, arms, legs, or all 3. The sensors will show how your heart is working.
Blood test
This blood test will look for a protein called troponin that’s released when your heart muscle is damaged.
Echocardiogram (echo)
An echocardiogram (EH-koh-KAR-dee-oh-gram) is an imaging test that uses ultrasound (sound waves) to take pictures of your heart. It shows how your heart is beating and pumping blood. It can also show if there’s anything wrong with your heart muscle or heart valves.
Stress test
A stress test helps show if your heart is getting enough blood when it’s under stress or working harder. Your doctor may ask you to exercise or give you medicine through an intravenous (IV) line in your vein. This will raise your heart rate and blood pressure.
Cardiac catheterization (cardiac cath) and coronary angiogram
This is a procedure that shows if there are blockages in any of your coronary arteries. You will get medicine to help you relax before the procedure.
During the procedure, your healthcare provider will insert a thin catheter into a blood vessel in your arm or leg. A catheter is a thin, flexible tube. Then, they will move the catheter up to your heart. This is called cardiac catheterization or cardiac cath.
Your healthcare provider will put a special dye through the catheter into your heart. They will use an x-ray machine to watch the dye move out of your heart and through your coronary arteries. This is called a coronary angiogram.
Treating and preventing heart attacks
A heart attack can be treated with medicine, cardiac catheterization, or surgery. Many of the following treatments may also prevent future heart attacks.
Medicine
There are many types of medicine used for treating and preventing heart attacks. These medicines work in different ways. The following are some examples, but there are others. Your cardiologist (heart doctor) will talk with you about which is best for you.
Over-the-counter medicine
Aspirin
Aspirin helps to prevent your platelets from clumping (forming blood clots). Aspirin lowers the risk of death after a heart attack.
Prescription medicine
ACE inhibitors
ACE inhibitors relax your blood vessels. This helps your heart work better after a heart attack and lowers your blood pressure. Examples include enalapril (Vasotec®) and lisinopril (Prinivil®).
Anticoagulants (blood thinners)
Anticoagulants thin your blood and prevent blood clots from forming. Examples include heparin and enoxaparin (Lovenox®)
Anti-platelet medicine
Anti-platelet medicine is similar to aspirin. It prevents blood clots from forming inside your arteries. They can prevent re-blockage if you have stents placed. Examples include clopidogrel (Plavix®), prasugrel (Effient®), and ticagrelor (Brilinta®). Read the Cardiac catheterization section below to learn more about stents.
Beta blockers
Beta blockers slow your heart rate and lower your blood pressure. This helps reduce the amount of work your heart has to do. Examples are carvedilol (Coreg®) and metoprolol (Lopressor®).
Nitrates
Nitrates widen your coronary arteries. This helps bring more blood to your heart muscle and reduces chest pain. Examples include nitroglycerin and isosorbide mononitrate (Imdur®).
Statins
If you have high cholesterol (too much cholesterol in your blood), it can clog your arteries. This can make you more likely to have a heart attack.
Statins lower your cholesterol and reduce the fatty deposits (plaques) inside your arteries. This lowers your risk of future heart attacks. Statins also help to secure any existing fatty deposits on the walls of your arteries. This keeps them from breaking off and causing a blockage. Examples include atorvastatin (Lipitor®) and rosuvastatin (Crestor®).
Procedures and surgeries
If you’ve had a heart attack in the past, you may not be able to have certain procedures. If this happens, your healthcare provider may prescribe medicine to treat and prevent future heart attacks. Talk with your healthcare provider to learn more.
Sometimes, you may need more advanced care after a heart attack, including an angioplasty, stent placement, or surgery. If you have a heart attack at MSK and need advanced care, you may need to go to another hospital. Your healthcare provider will talk with you about what treatment is best for you.
The following are procedures you may get after a heart attack.
Cardiac catheterization and coronary angiogram
During a cardiac catheterization, a small catheter is placed inside your artery. Your healthcare provider will place the catheter in one of your arteries. This may be the radial artery (in your wrist) or a femoral artery (at the top of your thigh).
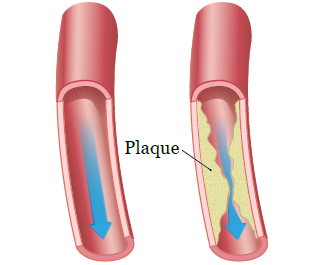
Your healthcare provider will put contrast dye through the catheter into your coronary arteries. Contrast is a dye used to help see your arteries more clearly. This will help them see any blockages there may be (see Figure 2). If they see blockages, your healthcare provider can do an angioplasty.
Coronary angioplasty and stent placement
During coronary angioplasty (also called angioplasty) your healthcare provider will place a catheter into the blocked artery. The catheter has a balloon at the end.
When the catheter reaches the blockage and is in place, your healthcare provider will inflate the balloon. The balloon pushes outward against the wall of your artery (see Figure 3). This widens the artery and improves blood flow to your heart.
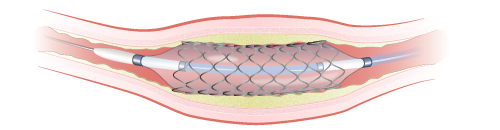
Your healthcare provider may also put a stent into your artery during this time. A stent is a hollow metal tube that keeps your artery open (see Figure 4).
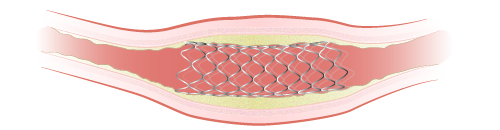
Coronary artery bypass surgery
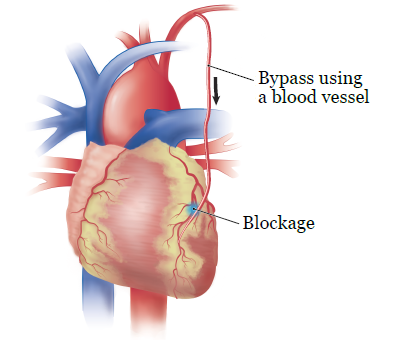
Coronary artery bypass surgery is surgery to help your blood bypass (go around) a blockage. During surgery, your healthcare provider will attach a blood vessel from another part of your body to your coronary artery. This is usually a blood vessel in your arm or leg. They will attach it above and below the blockage to let your blood go around the blockage (see Figure 5).
Lifestyle changes after a heart attack
The following are ways you can care for yourself after you’ve had a heart attack. Some are lifestyle changes that can help you avoid having another heart attack.
- If you smoke, try to quit. MSK has specialists who can help you quit smoking. To learn more about our Tobacco Treatment Program, call 212-610-0507 or ask your nurse for information about the program.
- If you’re overweight, try to lose weight. Talk with your healthcare provider about safe ways to do this.
- Follow a healthy diet that includes lots of fruits and vegetables. To learn more, read Eat Your Way to Better Health or talk with a clinical dietitian nutritionist.
- Talk with your primary care provider or cardiologist if you have other health problems. This includes high blood pressure, high cholesterol, and diabetes.
-
Join a cardiac rehabilitation program. These are programs that help improve the health and well-being of people who have heart problems. The programs include:
- Safe exercises for heart health.
- Education on ways to lower your risk of other heart problems.
- Counseling to lower stress. Stress can raise your risk for heart disease.
To learn more, and for more resources, visit the American Heart Association website at www.heart.org/en/health-topics/heart-attack/heart-attack-tools-and-resources/patient-information-sheets-heart-attack.
Learn about our Health Information Policy.
