This information will help you get ready for your transesophageal echocardiogram (TEE) at MSK.
A TEE is a procedure that uses ultrasound (sound waves) to create moving pictures of your heart. It lets your healthcare provider see how your:
- Heart valves are working
- Heart muscle is moving
- Blood is flowing
A TEE is a diagnostic exam. This means that it’s done to help your healthcare provider find a diagnosis (the cause of your illness) and decide on the best treatment plan.
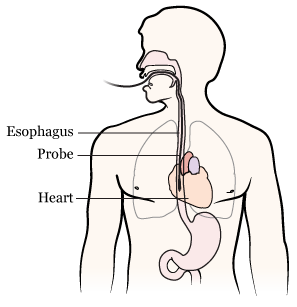
During your TEE, your healthcare provider will place a probe (flexible tube) into your esophagus (food pipe). This will help them get detailed pictures of your heart because your esophagus is directly behind your heart (see Figure 1).
7 days before your procedure
Ask about your medicine
Talk with your healthcare provider about the medications you’re taking. If you take insulin or other medications for diabetes, you may need to change the dose before your procedure. This is because you can’t eat after midnight on the evening before your procedure.
- If you take metformin (such as Glumetza® or Glucophage®), stop taking it 24 hours (1 day) before your procedure.
- If you are taking a blood thinner, ask the healthcare provider who prescribed it if you should continue this medication before your procedure.
Diabetes medicines
If you take insulin or other diabetes medicines, talk with your MSK healthcare provider and the healthcare provider who prescribes it. Ask them what to do before your surgery or procedure. You may need to stop taking it or take a different dose (amount) than usual. You may also need to follow different eating and drinking instructions before your surgery or procedure. Follow your healthcare provider’s instructions.
Your care team will check your blood sugar levels during your surgery or procedure.
GLP-1 medicines for weight loss
It’s important to tell your healthcare provider if you take a GLP-1 medicine. You will need to follow special eating and drinking instructions before your surgery or procedure. It is very important to follow these instructions. If you do not follow them, your surgery or procedure may be delayed or canceled.
- Follow a clear liquid diet the day before your surgery or procedure. Do not eat any solid food. Read Clear Liquid Diet to learn more.
- Stop drinking 8 hours before your arrival time. Do not eat or drink anything after this time, including clear liquids. You can have small sips of water with your medicines.
To learn more, read Eating and Drinking Before Your Surgery or Procedure When Taking GLP-1 Medicines.
Here are some examples of GLP-1 medicines. There are others, so be sure your care team knows all the medicines you take. Sometimes, these are prescribed to help manage diabetes or other conditions. Other times, they are prescribed for weight loss.
|
|
Get a letter from your healthcare provider, if needed
If you have an automatic implantable cardioverter-defibrillator (AICD), you’ll need to get a clearance letter from your cardiologist (heart doctor) before your procedure. A clearance letter is a letter that says you can safely have the procedure.
Arrange for someone to take you home
You must have a responsible care partner take you home after your procedure. A responsible care partner is someone who can help you get home safely. They should be able to contact your care team if they have any concerns. Make sure to plan this before the day of your procedure.
If you don’t have a responsible care partner to take you home, call one of the agencies below. They’ll send someone to go home with you. There’s a charge for this service, and you’ll need to provide transportation. It’s OK to use a taxi or car service, but you still need a responsible care partner with you.
| Agencies in New York | Agencies in New Jersey |
| VNS Health: 888-735-8913 | Caring People: 877-227-4649 |
| Caring People: 877-227-4649 |
3 days before your procedure
An endoscopy nurse will call you a few days before your procedure. They’ll review the instructions in this resource with you and ask you questions about your medical history. The nurse will also review your medications and tell you which medications to take the morning of your procedure.
The day before your procedure
Note the time of your procedure
A staff member will call you after noon (12 p.m.) the day before your procedure. If your procedure is scheduled for a Monday, they will call you the Friday before. If you don’t get a call by , call 212-639-7882.
The staff member will tell you what time to get to the hospital for your procedure. They’ll also tell you where to go for your procedure.
If you need to cancel your procedure for any reason, call the healthcare provider who scheduled it for you.
Instructions for eating
Stop eating at midnight (12 a.m.) the night before your surgery or procedure. This includes hard candy and gum.
Your healthcare provider may have given you different instructions for when to stop eating. If so, follow their instructions. Some people need to fast (not eat) for longer before their surgery or procedure.
The day of your procedure
Instructions for drinking
Between midnight (12 a.m.) and 2 hours before your arrival time, only drink the liquids on the list below. Do not eat or drink anything else. Stop drinking 2 hours before your arrival time.
- Water.
- Clear apple juice, clear grape juice, or clear cranberry juice.
- Gatorade or Powerade.
-
Black coffee or plain tea. It’s OK to add sugar. Do not add anything else.
- Do not add any amount of any type of milk or creamer. This includes plant-based milks and creamers.
- Do not add flavored syrup.
If you have diabetes, pay attention to the amount of sugar in your drinks. It will be easier to control your blood sugar levels if you include sugar-free, low-sugar, or no added sugar versions of these drinks.
It’s helpful to stay hydrated before surgeries and procedures, so drink if you are thirsty. Do not drink more than you need. You will get intravenous (IV) fluids during your surgery or procedure.
Stop drinking 2 hours before your arrival time. This includes water.
Your healthcare provider may have given you different instructions for when to stop drinking. If so, follow their instructions.
Things to remember
- Take only the medications your healthcare provider told you to take the morning of your procedure. Take them with a few sips of water.
- Don’t smoke the day of your procedure.
- Don’t put on any lotion, cream, powder, makeup, deodorant, perfume, or cologne.
- Don’t wear any metal objects. Remove all jewelry, including any body piercings.
- Leave all valuables, such as credit cards and jewelry, at home.
- If you wear contact lenses, wear your glasses instead.
What to bring
- A list of the medications you take at home, including patches and creams.
- Your rescue inhaler (such as albuterol for asthma), if you have one.
- A case for your glasses.
- Your Health Care Proxy form, if you have completed one.
Where to go
Your procedure will take place in the Endoscopy Suite at MSK. Its address is:
1275 York Avenue (between East 67th and East 68th Streets)
New York, NY 10065
Take the B elevator to the 2nd floor. Turn right and enter the Endoscopy/Surgical Day Hospital Suite through the glass doors.
Visit www.msk.org/parking for parking information and directions to all MSK locations.
What to expect
Once you arrive
Once you arrive, you’ll be asked to state and spell your name and date of birth many times. This is for your safety. People with the same or similar names may be having procedures on the same day.
After changing into a hospital gown, you’ll meet your nurse. They’ll place an intravenous (IV) catheter into one of your veins, usually in your hand or arm. The IV will be used to give you anesthesia (medication to make you sleep) during your procedure. You may also get fluids through the IV before your procedure.
You’ll talk with your healthcare provider before your procedure. They’ll explain the procedure and answer your questions.
Tell your healthcare provider if you have any of the following:
- You aren’t able to swallow liquids or food.
- You’ve had surgery to your esophagus.
- You’ve had radiation to your chest, spine, or upper back.
- You’re allergic to medications.
During your procedure
When it’s time for your procedure, you’ll go into the procedure room and be helped onto an exam table. You’ll be asked to remove your dentures or false teeth, if you have them. Your healthcare provider will set up equipment to monitor your heart, breathing, and blood pressure. You’ll get oxygen through a thin tube that rests below your nose. You’ll also get a mouth guard placed over your teeth to protect them. Your healthcare provider may also numb your throat with a spray.
Once you’re asleep, your healthcare provider will insert the probe into your mouth and pass it slowly down your esophagus. They’ll move it around slightly to take pictures of your heart and blood flow. This takes about 15 minutes.
After your procedure
In the recovery room
When you wake up after your procedure, you’ll be in the recovery room. Your nurse will continue to monitor your heart, breathing, and blood pressure. Once you’re fully awake, your nurse will remove your IV. Your nurse will explain your discharge instructions to you before you go home.
At home
- You may feel soreness in your throat. This will go away in 1 to 2 days. In the meantime, drink plenty of water and use cough drops to soothe your throat.
- Your healthcare provider may give you a prescription for antibiotics. Make sure to take them as directed.
- You may resume your normal activities 24 hours after your procedure.
- Do not drink alcoholic drinks for 24 hours after your procedure.
- Do not smoke for 24 hours after your procedure.
- You may have a little blood in the phlegm (mucus) or saliva that you cough up. If this happens for more than 24 hours or if there is a lot of blood, call your healthcare provider.
- Your results will be ready in 2 to 3 business days (Monday through Friday). Your results will be given to the healthcare provider who sent you for your TEE.
When to call your healthcare provider
Call your healthcare provider if you have any of the following:
- A fever of 101 °F (38.3 °C) or higher.
- Blood in your phlegm or saliva for more than 24 hours after your procedure.
- A lot of blood in your phlegm or saliva, such as when you cough.
Learn about our Health Information Policy.