This information will help you get ready for radiation therapy to your chest, including what to expect before, during, and after your treatment. You will also learn about side effects and how to care for yourself during your treatment.
This information is general. Your radiation therapy team will design a treatment and care plan just for you. Because of that, some parts of your treatment may be different than what’s described here. Your radiation therapy team will talk with you about what to expect.
About radiation therapy
Radiation therapy uses high-energy rays to treat cancer. It works by damaging the cancer cells and making it hard for them to reproduce. Your body is then naturally able to get rid of these damaged cancer cells. Radiation therapy also affects normal cells. However, your normal cells are able to repair themselves in a way that cancer cells cannot.
During treatment, a machine will aim beams of radiation directly to the tumor. The beam passes through your body and destroys cancer cells in its path. You will not see or feel the radiation.
Radiation therapy takes time to work. It takes days or weeks of treatment before cancer cells start to die. They will keep dying for weeks or months after treatment ends.
You can have radiation therapy before, during, or after surgery or chemotherapy.
Your role on your radiation therapy team
Your radiation therapy care team will work together to care for you. You’re a part of that team, and your role includes:
- Getting to your appointments on time.
- Asking questions and talking about your concerns.
- Telling us when you have side effects.
- Telling us if you’re in pain.
-
Caring for yourself at home by:
- Quitting smoking if you smoke. MSK has specialists who can help. To learn more about our Tobacco Treatment Program, call 212-610-0507. You can also ask your nurse about the program.
- Caring for your skin based on our instructions.
- Drinking liquids based on our instructions.
- Eating or avoiding the foods and drinks we suggest.
- Staying around the same weight.
Simulation
Before you begin your treatment, you will have a treatment planning procedure called a simulation. This is done to make sure that:
- Your treatment site is mapped.
- You get the right dose of radiation.
- The amount of radiation that gets to your nearby tissues is as small as possible.
During your simulation, you will have x-rays and your skin will be marked with little tattoo dots. These marks identify the area that will be treated.
Your simulation will take 2 to 4 hours.
Getting ready for your simulation
During your simulation, you will be lying in one position for a long time. If you think you will be uncomfortable lying still, you can take acetaminophen (Tylenol®) or your usual pain medication before your simulation. If you think you may get anxious during your procedure, speak with your doctor about whether medication may be helpful.
Some people will need to have a positron emission tomography-computed tomography (PET-CT) scan done during the simulation. If you are having one, your nurse will give you detailed instructions to prepare you for the scan. Some people are allergic to intravenous (IV; given through a vein) contrast (dye). If you are, your nurse will tell you what to do.
If you are having a PET-CT, do not eat or drink anything except water for 6 hours before your appointment time. This includes gum, hard candy, cough drops, and mints. If you have had anything except water, your PET-CT scan may need to be rescheduled.
Wear comfortable clothes that are easy to take off because you may need to change into a hospital gown. Do not wear jewelry, powders, or lotions.
Take devices off your skin
You may wear certain devices on your skin. Before your simulation or treatment, some device makers recommend you take off your:
- Continuous glucose monitor (CGM)
- Insulin pump
If you use one of these, ask your radiation oncologist if you need to take it off. If you do, make sure to bring an extra device to put on after your simulation or treatment.
You may not be sure how to manage your glucose (blood sugar) while your device is off. If so, before your appointment, talk with the healthcare provider who manages your diabetes care.
Day of your simulation
What to expect when you arrive
A member of your radiation therapy team will check you in when you arrive. They’ll give you an identification (ID) wristband with your name and date of birth. During your appointment, many staff members will check your ID wristband and ask you to say and spell your name and date of birth. This is for your safety. People with the same or a similar name may be getting care on the same day.
Your radiation therapists will review what to expect during the simulation. If you haven’t already signed a consent form, they will go over the form with you. They will answer any questions you have and ask for your signature.
If your treatment will be to your esophagus, you may be asked to swallow barium liquid. It makes it easier to see your esophagus on the x-rays that will be taken later.
During your simulation
For your simulation, you may need to get undressed from the waist up and change into a gown. You should keep your shoes on. If you wear a head covering, such as a wig, turban, or cap, you may have to remove it. Your radiation therapists will help you lie down on a table and make every effort to ensure your comfort and privacy.
Although the table will have a sheet on it, it is hard and has no cushion. If you have not taken pain medication and think you may need it, tell your radiation therapists before your simulation begins. Also, the room is usually cool. If you feel uncomfortable at any time, let your radiation therapists know.
Throughout your simulation, you will feel the table move into different positions. The lights in the room will be turned on and off and you will see red laser lights on each wall. Your therapists use these laser lights as a guide when they position you on the table. Do not look directly into the red beam because it may damage your eyes.
Although your radiation therapists will walk in and out of the room during your simulation, there will always be someone who can see and hear you. You will hear your radiation therapists speaking to each other as they work, and they will explain to you what they are doing. Do not move once your simulation begins, because it may change your position. However, if you are uncomfortable or need help, tell your radiation therapists.
To help pass the time, your radiation therapists can play music for you. You may bring a CD of your own from home, if you wish.
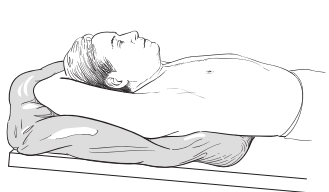
Positioning
You will probably be lying on your back throughout your simulation. While you are lying on the table, a mold will be made of your upper body. Your radiation therapists will pour a warm fluid into a large plastic bag that will be sealed and placed on the table. You will lie on top of the bag, on your back, with your arms raised above your head (see Figure 1). The fluid will feel warm at first, but it will cool as it hardens. While it is cooling, your therapists will tape the bag to your skin so that it takes the shape of your upper body and arms. This procedure takes about 15 minutes.
During your simulation, and every day of your treatment, you will lie in this mold. It helps ensure that you are in the correct position each time you receive your treatment.
X-ray images
While you are lying in your position, you will get x-rays of the area to be treated. These may be done on an x-ray machine called a simulator or on a computed tomography (CT) scan machine. If you are having a CT scan, you may be given contrast through an IV line before your scan. These scans are used only to map your treatment. They are not used for diagnosis or to find tumors. If you need other imaging, your nurse will explain this to you.
It will take about 45 minutes to get your x-rays. During the scan, you will hear the machine turn on and off. Even if the noise seems loud, your radiation therapists will be able to hear you if you speak with them.
Skin markings (tattoos)
Your radiation therapists will draw on your skin in the area being treated with a felt marker. You may need permanent skin markings called tattoos. Your radiation therapists will use a sterile needle and a drop of ink to make the tattoo. The sensation of getting one feels like a pinprick. The tattoo marks are no bigger than the head of a pin. The felt marking can be washed off after your simulation. The tattoos are permanent and will not wash off. If you are concerned about receiving tattoos as part of your radiation treatment, talk with your radiation oncologist.
After the tattoos are made, your radiation therapists will take several photographs of you in your simulation position. The photographs and tattoo marks will be used to position you correctly on the table each day of your treatment.
After your simulation
At the end of your simulation, we will give you an appointment for your set-up procedure. This is the final appointment before your treatment begins. You will also be assigned to a machine for your daily treatment.
Scheduling your treatment
Your treatment may be given in several different schedules. Your radiation therapy team will tell you what to expect.
You must come in every day that you are scheduled for your treatment. Treatment may not be as effective if you skip or miss appointments. If you need additional time due to unforeseen circumstances, your radiation oncologist will tell you. If for some reason you can’t come in for treatment, you must call your radiation oncologist’s office to let your team know. If you need to change your schedule for any reason, speak with your radiation therapist.
Treatment planning
During the time between your simulation and start of treatment, your radiation oncologist will work with a team to plan your treatment. They will use your simulation x-rays and CT scan to plan the angles and shapes of your radiation beams. The details are carefully planned and checked. This takes between 5 days and 2 weeks.
Vitamins and dietary supplements
Many people ask about taking vitamins during treatment. You may take a daily multivitamin, if you wish. Do not take more than the recommended daily allowance of any vitamin. Do not take any other vitamins or any supplements without talking to your doctor. This includes both nutritional and herbal supplements.
Set-up procedure
Before your first treatment, you will be scheduled for a set-up procedure. This procedure usually takes about 1 hour. If pain medication was helpful during simulation, you may want to take it before this procedure.
When you come for your set-up procedure, you will be shown to the dressing room and asked to change into a gown. Your therapists will bring you to the room where you will receive your treatment each day. They will position you on the treatment table. You will lie exactly as you were lying day of your simulation.
Special x-rays called beam films will be taken to make sure that your position and the area being treated are correct. The beam films will be repeated throughout your treatment. They are not used to see how your tumor responds to the treatment.
During your treatment
After you check in at the reception desk, have a seat in the waiting room. When your radiation therapists are ready for you, they will tell you to change into a gown. You should keep your shoes on during the treatment.
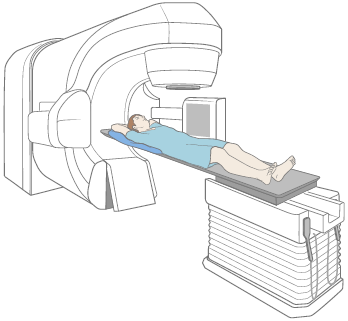
Your radiation therapists will bring you into the treatment room and help you lie in your mold on the table (see Figure 2). You will be positioned exactly how you were lying during your set-up procedure.
Once you are positioned correctly, your radiation therapists will leave the room, close the door, and begin your treatment. You will not see or feel the radiation, but you may hear the machine as it moves around you and is turned on and off. You will be in the treatment room for 10 to 30 minutes, depending on your treatment plan. Most of this time will be spent putting you in the correct position. The actual treatment only takes a few minutes.
Your radiation oncologist may recommend that you do certain things during your treatment. For example, you may be asked to hold your breath during treatment so that your lungs are not moving, or we may watch the movement of your lungs as you breathe during treatment. If one of these techniques is right for you, your radiation oncologist will discuss it with you. You may also get x-rays before your treatment to make sure that the area being treated has not changed with your positioning.
Although you will be alone during the treatment, your radiation therapists will see you on a monitor and hear you through an intercom at all times. They will make sure that you are comfortable during the treatment. Breathe normally during the treatment, but do not move. However, if you are uncomfortable or need help, speak to your radiation therapists. They can turn off the machine and come in to see you at any time, if necessary.
Neither you, nor your clothes will become radioactive during or after treatment. It is safe for you to be around other people.
Weekly visits during treatment
Your radiation oncologist and radiation nurse will see you each week to talk with you about any concerns, ask about any side effects you may be having, and answer your questions. This visit will be before or after your treatments each ________________. You should plan on being at your appointment about 1 extra hour on those days.
If you need to speak with your radiation oncologist or radiation nurse any time between your weekly visits, call your radiation oncologist’s office or ask the support staff or your radiation therapists to contact them when you come in for treatment.
Side effects
Some people develop side effects from radiation therapy. Which side effects and how severe they are depend on many factors, such as the area being treated, the dose of radiation, the number of treatments, and your overall health. The side effects may be worse if you are also getting chemotherapy. Below are the most common side effects of radiation therapy to the chest. You may have all, some, or none of these.
Cough or shortness of breath
Some people develop a cough or shortness of breath during treatment. Call your doctor or nurse if you develop these symptoms, or if they become worse during your treatment. Below are suggestions to help you feel more comfortable if you have a cough or shortness of breath.
- Do not smoke. Smoking will irritate the lining of your airway and cause more coughing. If you would like help to stop smoking, your nurse can refer you to our Tobacco Treatment Program.
- Use 1 or 2 pillows to elevate your upper body while you sleep.
- Use a humidifier while you sleep. Be sure to change the water and clean the humidifier as directed by the manufacturer.
- Fatigue may increase your shortness of breath. Follow the suggestions described in the “Fatigue” section. They can help to minimize your fatigue.
- Use cough medication as directed.
Pain or difficulty swallowing and heartburn
If your esophagus is in the area being treated, it may become inflamed. This can make it hard or painful to swallow. Some people also get heartburn from radiation to this area. These side effects usually begin the second or third week of treatment. They can last until about 2 weeks after your treatment is done. Below are suggestions to minimize discomfort and ensure that you get enough calories and protein during your treatment.
-
Avoid substances that may irritate your esophagus, such as:
- Very hot foods and liquids
- Dry, hard, and coarse foods (e.g., chips, pretzels, crackers)
- Spices (e.g., pepper, chili, Tabasco®, curry)
- Acidic or citrus foods and juices (e.g., orange, grapefruit, pineapple, tomato)
- Substances containing caffeine (e.g., coffee, tea, cola, chocolate)
- Alcohol
- Tobacco
- Take small bites of food and chew well before you swallow.
- Soft, moist, or puréed foods may be easier to swallow. Sauces and gravies may also be helpful.
- Cold foods and liquids may be helpful. Some people find that fruit nectars are particularly soothing.
- If you are having difficulty swallowing pills, ask your doctor or nurse if the medication comes in a liquid form. If not, many pills can be crushed and taken with applesauce. However, check with your doctor, nurse, or pharmacist before crushing any pill. Not all pills can be crushed.
- If you are having heartburn, do not eat at bedtime. Sit upright for at least 30 minutes after each meal. This will prevent your stomach juices from backing up into your esophagus.
- You can drink liquid nutritional supplements if you are not eating enough food. There are many products available and they come in a variety of flavors. Speak with your doctor or nurse about how to select the product that will be best for you.
- Let your doctor or nurse know if you start having any of the symptoms described above. There are medications that can be prescribed to make you more comfortable.
- You can call or set up an appointment with our dietitian, if you need help with your diet.
Skin and hair reactions
During radiation therapy, your skin and hair in the area being treated will change. This includes the area on your chest and on your back where the radiation beam leaves your body. This is normal and expected. After 2 to 3 weeks, your skin may become pink or tanned. It may even become bright red or very dark later on.
Your skin may feel dry and itchy, and may look flaky during treatment. Sometimes, the skin in sensitive areas may blister, open, and peel. If this happens, tell your doctor or nurse.
You may also notice a rash, especially in any area where you have had previous sun exposure. Although this may be a side effect of treatment, a rash could also be a sign of infection. If you develop a rash at any time during your treatment, tell your doctor or nurse.
Your nurse may apply special dressings or creams and teach you how to care for your skin. Your doctor may stop your treatment until your skin heals. This skin reaction sometimes becomes more severe during the week after treatment is done. If this happens, call your doctor or nurse. Your skin will gradually heal after your treatment is completed, but this often takes 3 to 4 weeks.
You may lose some or all of the hair on your chest. Your hair will usually grow back 2 to 4 months after your treatment is completed.
Below are guidelines to help you care for your skin during treatment. Follow these guidelines until your skin gets better. These guidelines refer only to the skin in the area being treated with radiation.
Keep your skin clean
- Bathe or shower daily using warm water and a mild unscented soap, such as Neutrogena®, Dove®, baby soap, Basis®, or Cetaphil®. Rinse your skin well and pat it dry with a soft towel.
- When washing, be gentle with your skin in the area being treated. Do not use a washcloth, a scrubbing cloth, or brush.
- The tattoo marks you received before your treatment are permanent and don’t wash off. You may get other markings during treatment such as an outline of your treatment area with a purple felt-tipped marker. You can remove these markings with mineral oil when your radiation therapists say it’s okay.
- Do not use alcohol or alcohol pads on the skin in the area being treated.
Moisturize your skin often
- Start using a moisturizer when you begin treatment. This can help to minimize any skin reaction. You can use over-the-counter moisturizers. When choosing a moisturizer pick one that does not have any fragrances or lanolin. There are a number of products that are good to use, and your nurse may suggest one of these to you. Use only one at a time unless your nurse tells you to use more.
- If you are using a moisturizer, apply it 2 times a day.
Avoid irritating your skin in the area being treated
- Wear loose-fitting cotton clothing and undergarments in the area being treated. Avoid tight clothing that will rub up against your skin.
- Use only the moisturizers, creams, or lotions that you have discussed with your radiation oncologist or nurse.
- Don’t use makeup, perfumes, powders, or aftershave in the area being treated.
- Don’t put tape on your treated skin
- If your skin is itchy, don’t scratch it. Apply moisturizer. Ask your nurse for recommendations on how to relieve the itching.
- Don’t shave in the area that is being treated. If you must shave, use only an electric razor. Stop if your skin becomes irritated.
- Don’t let your treated skin come into contact with extreme hot or cold temperatures. This includes hot tubs, water bottles, heating pads, and ice packs.
- If you have no skin reactions during your treatment, you can swim in a chlorinated pool. However, be sure to rinse off the chlorine right after getting out of the pool.
- Avoid tanning or burning your skin during treatment and for the rest of your life. If you are going to be in the sun, use a PABA-free sunblock with an SPF of 30 or higher. Also, wear loose-fitting clothing that covers you as much as possible.
Fatigue
Fatigue is a feeling of being tired or weak, not wanting to do things, not being able to concentrate, or feeling slowed down. You may develop fatigue after 2 to 3 weeks of treatment, and it can range from mild to severe. Fatigue may last 6 weeks to 12 months after your treatment ends.
There are a lot of reasons why you may develop fatigue during treatment, including:
- The effects of radiation on your body.
- Traveling to and from treatment.
- Not having enough restful sleep at night.
- Not eating enough protein and calories.
- Having pain or other symptoms.
- Feeling anxious or depressed.
- The side effects of certain medications.
You may find that your fatigue is worse at certain times of the day. Below are suggestions to help you manage your fatigue.
Ways to manage fatigue
- If you are working and are feeling well, continue to do so. However, working less may help increase your energy.
- Plan your daily activities. Pick those things that are necessary and most important to you and do them when you have the most energy. For example, you may go to work but not do housework, or watch your children’s sports event but not go out to dinner.
- Plan time to rest or take short naps (10 to 15 minutes) during the day, especially when you feel more tired. If you do nap, try to sleep for less than 1 hour at a time.
- Try to sleep at least 8 hours every night. This may be more sleep than you needed before you started radiation therapy. You may also find it helpful to go to sleep earlier at night and get up later in the morning. One way to sleep better at night is to be active during the day. For example, if you are able to exercise, you could go for a walk, do yoga, or ride a bike. Another way to sleep better at night is to relax before going to bed. You might read a book, work on a jigsaw puzzle, listen to music, or do calming hobbies.
- Ask family and friends to help you with things like shopping, cooking, and cleaning. Check with your insurance company to see if they cover home care services.
- Some people have more energy when they exercise. Ask your doctor if you can do light exercise, such as walking, stretching, or yoga.
- Eat foods and drink liquids that are high in protein and calories. Your nurse will give you the resource Eating Well During Your Cancer Treatment.
- Other symptoms, such as pain, nausea, diarrhea, difficulty sleeping, or feeling depressed or anxious, can increase your fatigue. Ask your radiation oncologist or nurse for help with any other symptoms you may have.
Loss of appetite
Some people find that their appetite decreases during treatment. It is important that you eat well and try not to lose weight during your treatment. If you have a mold to position you for treatment, it may not fit correctly if your weight changes. Also, your body needs enough protein and calories to help you recover from your treatment. Your nurse will give you the resource Eating Well During Your Cancer Treatment. It contains many suggestions to help you increase your intake of calories and protein. Try the different foods that are recommended.
Below are suggestions to help you maintain your weight:
-
Choose foods that increase how much protein and calories you eat. Protein-rich foods you can eat include:
- Lean meats
- Eggs
- Skinless poultry
- Low-fat yogurt
- Fish
- Lactose-free dairy items
- Low-fat tofu
- Try to eat small meals often throughout the day. If you never seem to feel hungry, make a schedule to make sure you eat regularly (for example, every 2 hours).
- Eat your meals slowly in a relaxing setting. Eat with family or friends whenever possible.
- Vary the color and texture of your foods to make them more appealing.
- Bring snacks and drinks with you when you come in for treatment. You can have these while you are waiting or while you are coming to and from the department each day.
- Drink liquid nutritional supplements if you are not eating enough food. There are many products available, and they come in many flavors. Ask your dietitian which product is best for you.
- You may take a daily multivitamin if you wish. Do not take more than the recommended daily amount of any vitamin. Do not take any supplements unless your doctor approves them. This includes both nutritional and herbal supplements.
Nausea
Some people experience nausea, with or without vomiting, at some time during treatment. This may occur as early as the first treatment. If you have nausea or vomiting, tell your radiation oncologist or nurse. Medication can be prescribed to relieve this. A change in your diet may also be helpful. Below are suggestions to help reduce your nausea and ensure you eat enough foods and liquids:
- Eat a light meal before your treatment.
- When feeling nauseous, start by nibbling on dry, starchy foods (toast, crackers, pretzels), and progress to small, frequent meals throughout the day.
- Some people find drinking ginger tea helpful for managing nausea. You can drink ginger tea if you have no sores in your mouth.
- Drink only a small amount of liquid with your meals to prevent feeling full or bloated.
- Sip liquids in between meals throughout the day. Using a straw may help. Try freezing your favorite beverages in ice cube trays and sucking on these during the day.
-
Select foods that will not cause nausea. Foods that are usually well tolerated include:
- Foods at room temperature or cooler
- Liquids that are cooled or chilled
- Dry, starchy foods, such as toast, soda crackers, Melba toast, dry cereal, pretzels, and angel food cake
- Yogurt, sherbet, and clear liquids (e.g., apple juice, Jell-O®, ginger ale)
- Cold chicken or turkey, baked or broiled, with the skin removed
- Soft fruits and vegetables
-
Avoid foods and liquids that may increase nausea. These include:
- Hot foods with strong odors
- Spicy, fatty, greasy, and fried foods
- Very sweet foods
- Acidic or citrus foods and juices (e.g., orange, grapefruit, pineapple, tomato)
- Alcohol
Changes to your blood cell counts
Bone marrow is the substance inside bone that makes blood cells. You have 3 kinds of blood cells. White blood cells fight off infection. Platelets help your blood to clot when you injure yourself. Red blood cells carry the oxygen you need for energy.
You may have lowered blood cell counts when large areas of bone marrow are in the area being treated. If you are also getting chemotherapy, it can also impact your blood cell count.
We will monitor you throughout your treatment with a blood test called a complete blood count (CBC). If your counts drop, we may stop your treatment until they return to higher levels. We will discuss precautions with you.
If you develop the following symptoms, notify your doctor or nurse immediately:
- A temperature of 100.4° F (38° C) or higher
- Shaking chills
- Flu-like symptoms
- Bleeding
You may need to be evaluated to see if you have an infection.
Sexual and reproductive health
You may have concerns about how cancer and your treatment can affect your sex life. You are not radioactive. You can’t pass radiation to anyone else. It’s safe to be in close contact with others.
You can be sexually active during your radiation therapy, unless your radiation oncologist gives you other instructions. If you or your partner are able to have children, you must use birth control (contraception) to prevent pregnancy during your radiation therapy.
Talking with your radiation oncologist or nurse about your sexual health can be hard, but it’s an important conversation to have. They may not bring it up unless you share your questions and concerns. You may feel uncomfortable, but most people in cancer treatment have similar questions. We work hard to make sure everyone in our care feels welcome.
Sexual health programs
MSK offers sexual health programs. These programs can help you manage the ways your cancer or cancer treatment affects your sexual health or fertility. Our specialists can help you address sexual health or fertility issues before, during, or after your radiation therapy.
- To learn about our Female Sexual Medicine & Women’s Health Program or to make an appointment, call 646-888-5076.
- To learn about our Male Sexual & Reproductive Medicine Program or to make an appointment, call 646-888-6024.
- To learn about our Cancer and Fertility Program, talk with your healthcare provider.
Other sexual health resources
Read Sex and Your Cancer Treatment to learn more about sexual health during cancer treatment.
The American Cancer Society also has resources about sexual health issues during cancer treatment. They’re called Sex and the Adult Male with Cancer and Sex and the Adult Female with Cancer. You can search for them at www.cancer.org or call 800-227-2345 for a copy.
Emotional health
|
|
|
You might also worry about telling your employer you have cancer or about paying your medical bills. You may worry about how your family relationships may change, or that the cancer will come back. You may worry about how cancer treatment will affect your body, or if you will still be sexually attractive.
It’s normal and OK to worry about all these things. All these kinds of feelings are normal when you or someone you love has a serious illness. We’re here to support you.
Ways to cope with your feelings
Talk with others. When people try to protect each other by hiding their feelings, they can feel very alone. Talking can help the people around you know what you’re thinking. It might help to talk about your feelings with someone you trust. For example, you can talk with your spouse or partner, close friend, or family member. You can also talk with a chaplain (spiritual advisor), nurse, social worker, or psychologist.
Join a support group. Meeting other people with cancer will give you a chance to talk about your feelings and learn from others. You can learn how other people cope with their cancer and treatment and be reminded you’re not alone.
We know that all cancer diagnoses and people with cancer are not the same. We offer support groups for people who share similar diagnoses or identities. For example, you can join a support group for people with breast cancer or for LGBTQ+ people with cancer. Visit www.msk.org/vp to learn about MSK’s support groups. You can also talk with your radiation oncologist, nurse, or social worker.
Try relaxation and meditation. These kinds of activities can help you feel relaxed and calm. You might try thinking of yourself in a favorite place. While you do, breathe slowly. Pay attention to each breath or listen to soothing music or sounds. For some people, praying is another way of meditation. Visit www.msk.org/meditations to find guided meditations lead by our Integrative Medicine and Wellness providers.
Exercise. Many people find that light movement, such as walking, biking, yoga, or water aerobics, helps them feel better. Talk with your healthcare provider about types of exercise you can do.
We all have our own way of dealing with tough situations. Often, we do what worked for us in the past. But sometimes that’s not enough. We encourage you to talk with your doctor, nurse, or social worker about your concerns.
After your treatment
Please be sure to keep your follow-up appointments with your radiation oncologist. He or she will evaluate your response to treatment. You may have blood tests, x-rays, and scans during these visits. Before coming, write down your questions and concerns. Bring this and a list of all your medications with you. You can also call your radiation oncologist or nurse at any time after your treatment is completed, or in between follow-up visits, if you have any questions or concerns.
Support services
MSK support services
Counseling Center
www.msk.org/counseling
646-888-0200
Many people find that counseling helps them. Our counseling center offers counseling for individuals, couples, families, and groups. We can also prescribe medicines to help if you feel anxious or depressed. Ask your healthcare provider for a referral or call the number above to make an appointment.
Integrative Medicine and Wellness Service
www.msk.org/integrativemedicine
Our Integrative Medicine and Wellness Service offers many services to complement (go along with) traditional medical care, including music therapy, mind/body therapies, dance and movement therapy, yoga, and touch therapy. Call 646-449-1010 to schedule an appointment for these services.
You can also schedule a consultation with a healthcare provider in the Integrative Medicine and Wellness Service. They will work with you to come up with a plan for creating a healthy lifestyle and managing side effects. Call 646-608-8550 to make an appointment.
Nutrition Services
www.msk.org/nutrition
212-639-7312
Our Nutrition Service offers nutritional counseling with one of our clinical dietitian nutritionists. Your clinical dietitian nutritionist will talk with you about your eating habits. They can also give advice on what to eat during and after treatment. Ask a member of your care team for a referral or call the number above to make an appointment.
Rehabilitation Services
www.msk.org/rehabilitation
Cancers and cancer treatments can make your body feel weak, stiff, or tight. Some can cause lymphedema (swelling). Our physiatrists (rehabilitation medicine doctors), occupational therapists (OTs), and physical therapists (PTs) can help you get back to your usual activities.
- Rehabilitation medicine doctors diagnose and treat problems that affect how you move and do activities. They can design and help coordinate your rehabilitation therapy program, either at MSK or somewhere closer to home. call Rehabilitation Medicine (Physiatry) at 646-888-1929 to learn more.
- An OT can help if you’re having trouble doing usual daily activities. For example, they can recommend tools to help make daily tasks easier. A PT can teach you exercises to help build strength and flexibility. Call Rehabilitation Therapy at 646-888-1900 to learn more.
Resources for Life After Cancer (RLAC) Program
646-888-8106
At MSK, care does not end after your treatment. The RLAC Program is for patients and their families who have finished treatment.
This program has many services. We offer seminars, workshops, support groups, and counseling on life after treatment. We can also help with insurance and employment issues.
Sexual Health Programs
Cancer and cancer treatments can affect your sexual health, fertility, or both. MSK’s sexual health programs can help you before, during, or after your treatment.
- Our Female Sexual Medicine & Women’s Health Program can help with sexual health problems such as premature menopause or fertility issues. Ask a member of your MSK care team for a referral or call 646-888-5076 to learn more.
- Our Male Sexual & Reproductive Medicine Program can help with sexual health problems such as erectile dysfunction (ED). Ask a member of your care team for a referral or call 646-888-6024 to learn more.
Tobacco Treatment Program
www.msk.org/tobacco
212-610-0507
MSK has specialists who can help you quit smoking. Visit our website or call the number above to learn more. You can also ask your nurse about the program.
Virtual Programs
www.msk.org/vp
Our Virtual Programs offer online education and support for patients and caregivers. These are live sessions where you can talk or just listen. You can learn about your diagnosis, what to expect during treatment, and how to prepare for your cancer care.
Sessions are private, free, and led by experts. Visit our website for more information about Virtual Programs or to register.
Radiation therapy support services
American Society for Therapeutic Radiology and Oncology
www.rtanswers.org
800-962-7876
This website has detailed information about treating cancer with radiation. It also has contact information for radiation oncologists in your area.
External support services
There are many other support services to help you before, during, and after your cancer treatment. Some offer support groups and information, while others can help with transportation, lodging (a place to stay), and treatment costs.
For a list of these support services, read External Support Services. You can also talk with an MSK social worker by calling 212-639-7020.
Lung Cancer Alliance
www.lungcanceralliance.org/get-help-and-support/
800-298-2436
Offers personalized support, information, and referral services at no cost by a team of trained, dedicated staff members to help patients, their loved ones, and those at risk with dealing with lung cancer. Advocates for increased lung cancer research funding and equitable access, coverage, and reimbursement for screening, treatment, diagnostics, and testing. Conducts nationwide education campaigns about the disease, risk, and early detection.
Questions to ask your radiation oncologist
Before your appointment, it’s helpful to write down questions you want to ask. Examples are listed below. Write down the answers during your appointment so you can review them later.
What kind of radiation therapy will I get?
How many radiation treatments will I get?
What side effects should I expect during my radiation therapy?
Will these side effects go away after I finish my radiation therapy?
What kind of late side effects should I expect after my radiation therapy?
Learn about our Health Information Policy.