This information explains your neck dissection surgery at Memorial Sloan Kettering (MSK). It will also help you understand what to expect during your recovery.
This resource does not include information about how to prepare for your neck dissection surgery. For information about how to prepare for surgery, please see our full length guide, About Your Neck Dissection Surgery.
About Your Surgery

Head and neck cancer can spread to your lymph nodes. Lymph nodes are small oval or round glands along your lymphatic system. In your neck, your lymph nodes are organized into levels (see Figure 1).
If your doctor thinks that there’s a high risk that the cancer may have spread to the lymph nodes in your neck, or if it has already spread to those nodes, your treatment may include having a neck dissection. This is a surgery to remove the lymph nodes in the neck area.
There are several types of neck dissections. The type you will have depends on where the cancer is, whether it has spread to your lymph nodes, and whether it has spread to other structures in your neck. Sometimes, your surgeon can tell which lymph nodes are affected by examining you. If this isn’t possible, you may need to have a computed tomography (CT) scan or ultrasound of your neck so that your surgeon can see the area better.
In addition to the lymph nodes, other structures in your neck may need to be removed, including:
- The muscle on the side of the neck that helps you turn your head. When this muscle is removed, there will be an indent on that side of your neck. You will still be able to move your neck without difficulty.
- The nerve that allows you to raise your arm higher than your shoulder. Your surgeon will try to save this nerve. If it must be removed, you will have trouble raising your arm above a 90-degree angle on the side that the nerve was removed.
- A vein that collects blood from your brain, face, and neck. Removing this vein on one side of your neck won’t cause any problems. Other veins in your neck will collect and circulate the blood on that side of your neck and face.
- A salivary gland in the upper part of your neck. Removing this gland won’t cause any damage to your salivary function.
Once your lymph nodes have been removed, your surgeon will close your incision with staples or sutures (stitches). The type of incision line you have will depend on which lymph nodes and structures were removed. Your surgeon will discuss this with you.
Before Your Surgery
Your nurse will give you instructions for how to prepare for your surgery. For more information, see our resource About Your Neck Dissection Surgery.
What to Expect After Your Surgery
When you wake up after your surgery, you will be in the Post Anesthesia Recovery Unit (PACU).
You will receive oxygen through a thin tube that rests below your nose called a nasal cannula. A nurse will be monitoring your body temperature, pulse, blood pressure, and oxygen levels. You will also be wearing compression boots to help your circulation.
Depending on the amount of lymph nodes removed, you may have a drain called a ReliaVac®. The ReliaVac drain will be placed in your neck during your surgery. It helps prevent fluid from collecting under your skin (see Figure 2). The drain doesn’t hurt. It will be emptied regularly.
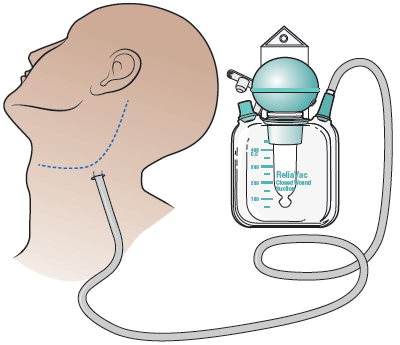
Depending on the type of surgery you had, you may stay in the PACU overnight. After your stay in the PACU, you will be taken to your hospital room.
Commonly Asked Questions
During Your Hospital Stay
Will I have pain?
You will have some pain after your surgery. Your doctor and nurse will ask you about your pain often and give you medication as needed. If your pain isn’t relieved, please tell your doctor or nurse.
You’ll have numbness on the side of your surgery from your earlobe to above your collar bone. This is normal and occurs because tiny skin nerves are cut and it takes months for this to heal. You may have permanent numbness on your earlobe.
You will first get pain medication through your IV. You will get pain medication by mouth once you are eating a regular diet. You will be given a prescription for pain medication before you leave the hospital.
How can I prevent constipation?
Prescription pain medication may cause constipation. Your doctor may prescribe medication to prevent constipation for you to take while you’re at home recovering from surgery. There are also other things you can do to prevent constipation, such as:
- Exercise, if you can. Walking is an excellent form of exercise.
- Drink plenty of liquids. Aim for 8 to 10 (8-ounce) glasses each day. Drink water, juices, soups, ice cream shakes, and other drinks that don’t have caffeine. Drinks with caffeine, such as coffee and soda, pull fluid out of the body.
- Go to the bathroom at the same time every day. Your body will get used to going at that time. Try to use the bathroom 5 to 15 minutes after meals. After breakfast is a good time, because the reflexes in your colon are strongest at this time.
- If you feel the urge to go, don’t put it off.
If these methods don’t help, talk with your doctor or nurse. They may recommend over-the-counter or prescription medication.
When can I eat?
For the first meal after your surgery, you will get clear liquids. If you can tolerate that (or if you’re not experiencing nausea), your diet will then progress to solid food.
When will my ReliaVac drain be removed?
Your ReliaVac drain will be removed when the amount of drainage is steadily decreasing and the output is less than 25 to 30 milliliters (about ½ ounce) in 24 hours. This is usually 3 to 5 days after surgery.
When will my staples or sutures be removed?
If you stay in the hospital for longer than 1 week, some or all of your staples or sutures may be removed before you leave.
If you stay in the hospital for less than 1 week, your staples or sutures will be removed during your post-operative visit (your first follow-up visit with your doctor after your surgery).
If you had radiation therapy to the neck before your surgery, your staples or sutures may stay in place for 2 to 3 weeks.
How long will I be in the hospital?
Your doctor or nurse will give you an estimate of how long you will be in the hospital. Most people are discharged on the day that their ReliaVac drain is removed. This is usually 3 to 5 days after surgery.
Some people may go home with the drain in place. If this is the case, your nurse will teach you how to care for it before you leave the hospital.
After You Leave the Hospital
Will I have pain when I am home?
The length of time each person has pain or discomfort varies. Follow the guidelines below to manage your pain.
- Call your doctor if the pain medication prescribed for you doesn’t relieve your pain.
- Don’t drive or drink alcohol while you’re taking prescription pain medication.
- Pain medication should help you as you resume your normal activities. Take enough medication to make sure you can gradually increase your activities. Pain medication is most effective 30 to 45 minutes after taking it.
- Keep track of when you take your pain medication. Taking it when your pain first begins is more effective than waiting for the pain to get worse.
As your incision heals, you will have less pain and need less pain medication. A mild pain reliever such as acetaminophen (Tylenol®) or ibuprofen (Advil®) will relieve aches and discomfort.
How do I care for my incision?
It’s very important that you keep your incision clean and remove any crust that develops on it. Crust can collect bacteria and lead to infection. Your doctor or nurse will teach you how to care for your incision before you’re discharged. Once you’re home, you must care for your incision daily as described below.
-
Gather the following supplies:
- Cotton swabs (such as Q-Tips®)
- Normal saline
- Bacitracin ointment
- Wash your hands thoroughly with soap and water or use an alcohol-based hand sanitizer such as Purell®.
- Take a cotton swab and dip it in the normal saline.
- Use the cotton swab to gently clean along the incision line around the staples or sutures. This will help loosen any crust that may have developed along the wound.
- Throw the swab away.
- Repeat the steps above with a fresh swab as many times as it takes to clean the incision line. Remember that you can only dip the swab once. You must use a clean swab each time you dip it into the saline.
- Apply a small amount of bacitracin ointment to the incision line with a clean cotton swab.
When can I shower?
You can shower 24 hours after your drain is removed from your neck. When showering, don’t let the water from your shower head hit your incision directly. Rather, allow the soap and water to run over your incision. Gently pat your incision dry with a clean towel.
What do I need to do to recover from my surgery?
After your sutures or staples are removed, your doctor or nurse may instruct you to do certain exercises every day. This will depend on how well you can turn your neck and move your arm(s) after surgery. The exercises will help you regain full range of motion and strength to the affected area(s). It’s important that you do them every day. Your doctor or nurse will show you how to do the exercises and will give you written instructions at your post-operative visit.
When can I resume my normal activities?
Your doctor and nurse will tell you when you can resume your normal activities during your post-operative visit. Until then, avoid all activity that could put strain on your incision, including:
- Driving
- Lifting items heavier than 10 pounds (4.5 kilograms)
- Vigorous exercise
- Sexual activity
When can I resume sexual activity?
Ask your doctor or nurse when you can resume sexual activity.
What type of follow-up care will I receive after I leave the hospital?
You will have your post-operative visit with your doctor about 1 week after you’re discharged from the hospital. Until then, be sure to follow all instructions given to you when you were discharged.
If you have any questions or concerns, you can contact your doctor’s office at any time after you have been discharged from the hospital.
When will I get my test results?
The lymph nodes will be examined for cancer after they’re removed. The test results are usually ready in 5 to 7 business days. Based on the results, you may need further treatment. Your doctor will discuss the results with you during your post-operative visit.
How can I cope with my feelings?
After surgery for a serious illness, you may have new and upsetting feelings. Many people say they felt weepy, sad, worried, nervous, irritable, or angry at one time or another. You may find that you can’t control some of these feelings. If this happens, it’s a good idea to seek emotional support.
The first step in coping is to talk about how you feel. Family and friends can help. Your nurse, doctor, and social worker can reassure, support, and guide you. It’s always a good idea to let these professionals know how you, your family, and your friends are feeling emotionally. Many resources are available to patients and their families. Whether you’re in the hospital or at home, we’re here to help you and your family and friends handle the emotional aspects of your illness.
Call Your Doctor or Nurse if You Have:
- A temperature of 100.4° F (38° C) or higher
- Increased discomfort, redness, or both around your incision line
- Skin around the incision line that’s hot to the touch
- Drainage or accumulation of fluid from the incision site
- Shortness of breath
- New or increased swelling around your incision
Learn about our Health Information Policy.