This information will help you get ready for your sutured drainage catheter placement at MSK. It also explains how to care for the catheter at home.
About drainage catheters
A drainage catheter is a thin, flexible tube that drains fluid that has collected in your body. When this fluid is infected, it is called an abscess (AB-ses). An abscess may cause fever, pain, or blood test results that are not normal.
About your sutured drainage catheter placement
An interventional (IN-ter-VEN-shun-al) radiologist will place your drainage catheter. An interventional radiologist is a doctor with special training in using image-guided procedures to diagnose and treat disease. They will explain the procedure and give you time to ask any questions before you sign a consent form. Signing the consent form means that you agree to the procedure and understand the risks.
During your procedure, your doctor will put the catheter through your skin and into the area where fluid has collected. They will use fluoroscopy (real time X-rays), a computed tomography (CT) scan, or ultrasound to guide the catheter into place. Then they will secure it to your skin with a suture (stitch).
The procedure usually takes less than 1 hour.
After the procedure, your catheter will be attached to a small bag to collect the drainage. Fluid will drain from the catheter into the bag. Your doctor will tell you how much drainage to expect. They will take out the catheter when there is no more fluid collecting.
Often, drainage catheters are placed urgently if you are sick. In some cases, we will schedule you to come into the hospital for the procedure. If this is the case, follow the guidelines below.
What to do before your procedure
Ask about your medicines
You may need to stop taking some of your usual medicines before your procedure. Or, you may need to take a different dose (amount) than usual. Talk with your healthcare provider about how to take your medicines before your procedure. Do not change how you take your medicines without talking with a healthcare provider.
This section lists some examples of medicines, but there are many others. Make sure your care team knows all the prescription medicines, over-the-counter medicines, and dietary supplements you take. A prescription medicine is one you can only get with a prescription from a healthcare provider. An over-the-counter medicine is one you can buy without a prescription.
It’s very important to take your medicines and supplements the right way in the days before your procedure. If you don’t, we may need to reschedule your procedure.
Anticoagulants (blood thinners)
A blood thinner is a medicine that changes how your blood clots. Blood thinners are often prescribed to help prevent a heart attack, stroke, or other problems caused by blood clots.
If you take a blood thinner, ask your healthcare provider what to do before your procedure. They may tell you to stop taking it a certain number of days before your procedure. This will depend on the type of procedure you’re having and the reason you’re taking a blood thinner.
Here are some examples of blood thinners. There are others, so be sure your care team knows all the medicines you take. Do not stop taking your blood thinner without talking with a member of your care team.
|
|
Other medicines and supplements can change how your blood clots. Examples include vitamin E, fish oil, and nonsteroidal anti-inflammatory drugs (NSAIDs). Read How To Check if a Medicine or Supplement Has Aspirin, Other NSAIDs, Vitamin E, or Fish Oil. It will help you know which medicines and supplements you may need to avoid before your procedure.
Diabetes medicines
If you take insulin or other diabetes medicines, talk with your MSK healthcare provider and the healthcare provider who prescribes it. Ask them what to do before your surgery or procedure. You may need to stop taking it or take a different dose (amount) than usual. You may also need to follow different eating and drinking instructions before your surgery or procedure. Follow your healthcare provider’s instructions.
Your care team will check your blood sugar levels during your surgery or procedure.
GLP-1 medicines for weight loss
It’s important to tell your healthcare provider if you take a GLP-1 medicine. You will need to follow special eating and drinking instructions before your surgery or procedure. It is very important to follow these instructions. If you do not follow them, your surgery or procedure may be delayed or canceled.
- Follow a clear liquid diet the day before your surgery or procedure. Do not eat any solid food. Read Clear Liquid Diet to learn more.
- Stop drinking 8 hours before your arrival time. Do not eat or drink anything after this time, including clear liquids. You can have small sips of water with your medicines.
To learn more, read Eating and Drinking Before Your Surgery or Procedure When Taking GLP-1 Medicines.
Here are some examples of GLP-1 medicines. There are others, so be sure your care team knows all the medicines you take. Sometimes, these are prescribed to help manage diabetes or other conditions. Other times, they are prescribed for weight loss.
|
|
Diuretics (water pills)
A diuretic is a medicine that helps control fluid buildup in your body. Diuretics are often prescribed to help treat hypertension (high blood pressure) or edema (swelling). They can also be prescribed to help treat certain heart or kidney problems.
If you take a diuretic, ask the healthcare provider doing your procedure what to do before your procedure. You may need to stop taking it the day of your procedure.
We’ve listed some examples of common diuretics below. There are others, so be sure your care team knows all the medicines you take.
|
|
Take devices off your skin
You may wear certain devices on your skin. Before your procedure, surgery, or scan, some device makers recommend you take off your:
- Continuous glucose monitor (CGM)
- Insulin pump
Talk with your healthcare provider about scheduling your appointment closer to the date you need to change your device. Make sure to bring an extra device with you to put on after your procedure, surgery, or scan.
You may not be sure how to manage your glucose (blood sugar) while your device is off. If so, before your appointment, talk with the healthcare provider who manages your diabetes care.
Arrange for someone to take you home
You must have a responsible care partner take you home after your procedure. A responsible care partner is someone who can help you get home safely. They should be able to contact your care team if they have any concerns. Make sure to plan this before the day of your procedure.
If you don’t have a responsible care partner to take you home, call one of the agencies below. They’ll send someone to go home with you. There’s a charge for this service, and you’ll need to provide transportation. It’s OK to use a taxi or car service, but you still need a responsible care partner with you.
| Agencies in New York | Agencies in New Jersey |
| VNS Health: 888-735-8913 | Caring People: 877-227-4649 |
| Caring People: 877-227-4649 |
Tell us if you’re sick
If you get sick (including having a fever, cold, sore throat, or flu) before your procedure, call your IR doctor. You can reach them Monday through Friday from to
After , during the weekend, and on holidays, call 212-639-2000. Ask for the Interventional Radiology fellow on call.
Note the time of your appointment
A staff member will call you 1 to 2 business days before your procedure. If your procedure is scheduled for a Monday, they’ll call you on the Thursday before. They’ll tell you what time to get to the hospital for your procedure. They will also remind you where to go.
If you don’t get a call by noon (12 p.m.) on the business day before your procedure, call 646-677-7001. If you need to cancel your procedure for any reason, call the healthcare provider who scheduled it for you.
What to do the day before your procedure
Instructions for eating
Stop eating at midnight (12 a.m.) the night before your surgery or procedure. This includes hard candy and gum.
Your healthcare provider may have given you different instructions for when to stop eating. If so, follow their instructions. Some people need to fast (not eat) for longer before their surgery or procedure.
What to do the day of your procedure
Instructions for drinking
Between midnight (12 a.m.) and 2 hours before your arrival time, only drink the liquids on the list below. Do not eat or drink anything else. Stop drinking 2 hours before your arrival time.
- Water.
- Clear apple juice, clear grape juice, or clear cranberry juice.
- Gatorade or Powerade.
-
Black coffee or plain tea. It’s OK to add sugar. Do not add anything else.
- Do not add any amount of any type of milk or creamer. This includes plant-based milks and creamers.
- Do not add flavored syrup.
If you have diabetes, pay attention to the amount of sugar in your drinks. It will be easier to control your blood sugar levels if you include sugar-free, low-sugar, or no added sugar versions of these drinks.
It’s helpful to stay hydrated before surgeries and procedures, so drink if you are thirsty. Do not drink more than you need. You will get intravenous (IV) fluids during your surgery or procedure.
Stop drinking 2 hours before your arrival time. This includes water.
Your healthcare provider may have given you different instructions for when to stop drinking. If so, follow their instructions.
Things to remember
- Take your medicine with a few sips of water the morning of your procedure. Follow your doctor’s instructions.
- Do not use cream or petroleum jelly (Vaseline®). You can use deodorant and light moisturizers. Do not wear eye makeup.
- Remove any jewelry, including body piercings.
- Leave all valuables, such as credit cards and jewelry, at home.
- If you wear contact lenses, wear your glasses instead, if possible. If you don’t have glasses, please bring a case for your contacts.
What to bring with you
- Medicine for breathing problems, such as inhalers, medicine for chest pain, or both.
- A case for your glasses or contacts.
- Your Health Care Proxy form and other advance directives, if you have completed them.
- Your CPAP or BiPAP machine if you use one. If you cannot bring yours with you, we will give you one to use while you’re in the hospital.
What to expect when you arrive
Many staff members will ask you to say and spell your name and date of birth. This is for your safety. People with the same or similar names may be having procedures on the same day.
You will meet the doctor who will place the catheter. They will explain the procedure and ask you to sign a consent form.
Inside the procedure room
A member of your care team will bring you into the procedure room. If you don’t have an intravenous (IV) line, your nurse will put one in. They will give you medicine through your IV to make you feel drowsy. They will also give you an injection (shot) of local anesthesia. This is medicine to numb the area where they will place the catheter into your skin.
Then, your doctor will do the placement procedure. They will suture the catheter to your skin at the point where it leaves your body. You will be able to see the thread around your catheter.
What to do after your procedure
A staff member will bring you to the recovery room after your procedure. You will need to stay in bed until the medicine has worn off. You will then go back to your hospital room or go home with your caregiver.
About your catheter

You will have a black mark on the catheter above the suture (see Figure 1). Your nurse will show it to you. This mark should always be the same distance from your skin. If it changes, this means that the catheter has moved. Call Interventional Radiology right away so someone there can check it.
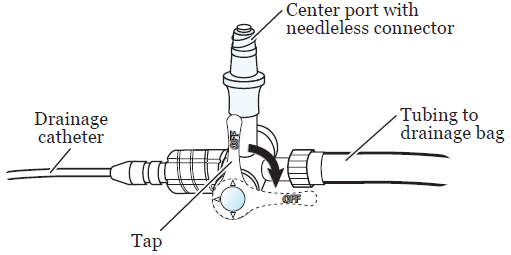
The end of the catheter outside of your body will be attached to a 3-way stopcock (see Figure 2). The stopcock has a tap that you can turn to control the flow of liquid. It also has 3 points of attachment.
The drainage bag connects to the attachment point opposite the catheter. The third attachment point has a protective cover on it called a needleless connector. You can inject fluids through the cover. You will have a dressing over the catheter.
You can attach the drainage bag to your clothes with a safety pin. You can also secure it to your leg with Velcro® straps. Use the twist cap at the bottom of the bag to drain it.
CathGrip® is a device that stops your catheter from coming out of your body if you accidentally pull on it.
Showering with a sutured drainage catheter
You may take showers, but you will need to keep your dressing dry. If the dressing gets wet, you will need to change it. Wet dressings are a common cause of skin problems. Take a hand-held shower to direct the water away from the dressing. You will also need to cover your dressing.
Before you shower, take off the belt and empty the drainage bag. Tape the drainage bag to your body near the catheter or use a strap to attach it to your waist. Tape plastic wrap or a gallon-sized bag over the dressing to keep it dry.
You can also use AquaGuard®, which is a one-time use waterproof cover to protect your dressing. Cover the catheter when you shower to keep it from getting wet.
Putting on the AquaGuard
- The edges of the AquaGuard have peelable tape. Fold over a corner of each side of the tape (see Figure 3).
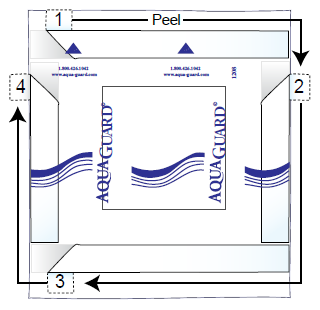
- Hold the AquaGuard with the arrows pointing towards your head. Peel off the top strip and put the top edge of the AquaGuard above the dressing. Smooth it down.
- Grab a folded corner and peel down one side, smoothing it as you go.
- Do the same to the bottom and remaining side.
- Do not let the tape on the AquaGuard touch the dressing. It can lift the dressing when you take off the AquaGuard after showering.
How to care for a sutured drainage catheter
Your nurse will teach you how to care for the catheter. Use this resource at home to remind you of what you learned. A visiting nurse can help you at home until you or your caregiver feel confident caring for the catheter. Ask your healthcare provider for more information about how to arrange for a visiting nurse.
Every day:
- Check the catheter.
- Flush the catheter with normal saline.
- Record the amount of drainage in the bag.
- Empty drainage from the bag.
Change your dressing, drainage bag, 3-way stopcock and needless connector once a week. You will also need to change the dressing if it gets loose, wet, or dirty. If you leave a wet dressing against your skin, it may make your skin irritated and sore.
You can check the catheter and flush it with the normal saline yourself or ask someone to help you. You may need someone to help you change the dressing and drainage equipment.
Check the catheter
Check the catheter every day. You can use a hand-held or full-length mirror to do this. If you see a problem, finish caring for the catheter, then call the nurse or fellow. The contact information is at the end of this resource.
- Find the black mark to make sure it is in the correct position.
- Check the dressing to make sure it is secure. Change the dressing if it is wet, dirty, has come loose, or started to pull away from the skin.
- Check the skin around the catheter when you change the dressing. There should be no redness, areas of broken skin, or rash. Fluid should not leak around the catheter.
- Look at the fluid in the bag. It should flow freely into the bag. There should be no change in the way it normally looks.
- Check the catheter and the drainage bag for kinks (twists or bends) in the tubing.
Flush the catheter
Flush the catheter with normal saline twice a day. Your doctor will tell you whether to use 3 milliliters (mL), 5 mL, or 10 mL of normal saline.
Here is a video that shows how to flush a biliary catheter. Follow the same directions to flush your sutured drainage catheter.
- Gather your supplies. You’ll need 1 (10 mL) prefilled normal saline syringe and 2 alcohol wipes.
- Wash your hands with warm water and soap for at least 20 seconds or use an alcohol-based hand sanitizer.
- Take the syringe out of the wrapper. Twist the cap off the syringe.
- With the cap off, remove the air from the syringe. To do this, hold the syringe open side up. Then push the plunger slowly until the normal saline is at the top.
If your doctor told you to flush with less than 10 mL, squirt the extra saline out. Then connect the syringe and lay it on the table. Do not let the tip of the syringe to touch anything.
- Sit or lie comfortably. Turn the stopcock toward the drainage bag (see Figure 2).
- Clean the needleless connector on the stopcock by rubbing it with an alcohol wipe for 15 to 30 seconds.
- Place the syringe onto the needleless connector. Hold the connector while you push and turn the syringe clockwise (to the right) to lock it into position.
- Push the plunger to push one-third of the normal saline into the catheter, then pause. Push in another one-third of the normal saline and pause again. Then push the rest of the normal saline into the catheter. Never pull back on the plunger. Always push forward.
Stop and call your doctor’s office if you have any of the following while flushing:
- Feel pain.
- Feel resistance.
- See leaking around the catheter.
Do not try to put in any more saline.
- When the syringe is empty, turn it counterclockwise (to the left) to take it off. Throw it away in your regular trash.
- Turn the stopcock back to the direction of the needleless connector (see figure 2). You will probably see fluid drain into the bag.
Empty the drainage from the bag
Measure and empty the drainage twice a day, or more often if needed.
-
Gather your supplies. You’ll need:
- The measuring container you got in the hospital.
- Non-sterile gloves.
- 2 alcohol wipes.
- Wash your hands with warm water and soap for at least 20 seconds or use an alcohol-based hand sanitizer.
- Put on the non-sterile gloves.
- Clean the cap at the bottom of the drainage bag with an alcohol wipe.
- Twist the cap open while holding it over the measuring container.
- Let the fluid drain into the container. Do not let the bottom of the bag touch the sides of the drainage container.
- When all fluid has drained out of the bag, twist the cap closed.
- Clean the cap with a new alcohol wipe.
- Measure the amount of fluid in the container, then flush the fluid down the toilet.
- Wash the measuring container with soap and water. Let it air dry.
- Throw out the gloves. Then, clean your hands with soap and water or an alcohol-based hand sanitizer.
- Record the amount of drainage on the drainage log at the end of this resource. Be sure to subtract the amount of your saline flush (3 mL, 5mL, or 10 mL) from the daily totals.
Change the dressing
Change the dressing, 3 way stopcock, needless connector and drainage system once a week. Change the dressing if it gets wet, dirty, loose, or pulls away from your skin. You can try to put the equipment together yourself or ask someone to help you. You’ll need someone to help you change the dressing and equipment.
- Gather your supplies:
- 2 Primapore® dressings.
- 3M™ No Sting Barrier Film.
- Adhesive remover wipe.
- Alcohol wipes.
- Gauze.
- Mild soap, such as Dove®. This should not have scents or harsh chemicals.
- A cup of water.
- Non-sterile gloves.
- CathGrip kit, if you’re changing the CathGrip.
- Waste basket.
- Wash your hands with warm water and soap for at least 20 seconds or use an alcohol-based hand sanitizer.
- Sit or lie comfortably. At this point, you will need someone to help you. The person doing the dressing change should follow the instructions below.
- Wash your hands and put on non-sterile gloves.
- Hold the catheter in place to prevent tension or pulling on the catheter. Gently take off the old dressing and throw it away. If the skin around the catheter is sensitive, rub the adhesive remover along the edge of the dressing. This can help ease any discomfort.
- Release the catheter from the straps on the CathGrip. Make sure the drainage bag is somewhere that it can’t fall. If you’re changing the CathGrip, use adhesive remover to release it from your skin.
- Throw out the old dressing, and the adhesive remover if you used it.
- Wet a gauze pad with soap and water. Use it to clean the skin around the catheter.
- Rinse the skin, then dry it with fresh gauze.
- Check the drainage catheter. The black ink mark should be just above the suture (see Figure 1).
-
Check the insertion site. Call your doctor’s office if you see any:
- Redness.
- Swelling.
- Leakage of fluid around the catheter.
- Foul-smelling drainage.
- Put the 3M No Sting Barrier Film on the skin. This protects your skin and helps the adhesive stick better.
- Place one Primapore dressing centered over the insertion site. Place a second Primapore dressing one-half inch below the insertion site. This will let the adhesive on the dressing to secure the catheter.
- Take off your gloves and throw them out. Then wash your hands.
- If you will not be changing your drainage bag at this time, go to step 11 below.
Change the stopcock and drainage equipment
Below is a video that shows how to change the equipment on a biliary catheter. Follow the same directions to change the equipment on your sutured drainage catheter.
-
Gather your equipment:
- Non-sterile gloves
- 1 needleless connector
- 1 sterile 3-way stopcock
- 1 drainage bag
- Safety pin or strap
- Gauze
- 1-inch Micropore® paper tape
- Waste basket
- Wash your hands with warm water and soap for at least 20 seconds or use an alcohol-based hand sanitizer.
- Open the packages with the needleless connector, 3-way stopcock, and drainage bag. Put the package from the drainage bag to one side.
- Take off the protective cover from the base of the needleless connector and throw it away. Attach the needleless connector to the center port of the stopcock (see Figure 1). Then put the stopcock down.
- Take the drainage bag out of the package. Connect the tubing from the drainage bag to the stopcock with a twisting motion. Close the drainage port on the bottom of the bag by turning it clockwise. Closing the port stops it from leaking.
- Place the assembled drainage bag back in its package. This will keep it clean until you are ready to connect it to the catheter.
- Wash your hands again, then put on the non-sterile gloves.
- If the bag is attached with a safety pin, take out the safety pin. Make sure you can reach the new drainage bag.
- Hold gauze under the connector and twist off the old stopcock and drainage system from the catheter. Then throw it away. Quickly attach the new stopcock and drainage system.
- Turn off the tap of the stopcock. It should face in the direction of the needleless connector.
- If you are not changing CathGrip right now, reattach the catheter to the CathGrip.If you are changing the CathGrip, place the catheter on the device straps. There are 2 straps, one with holes and one with jagged edges. The strap with the holes has 2 openings. Put the end of the strap with the jagged edges into the lower opening of the other strap. Pull it to secure it (see Figure 4).
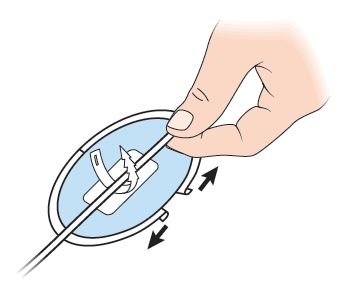
- Make sure that there is no pull or tension on the catheter. If you notice any tension or pull, change the position of the catheter in the CathGrip. This will stop the tube from kinking.
-
Secure the drainage bag. You can attach it to your waistband with the safety pin, or to your leg with the attached Velcro straps. The bag should be below the level of the catheter (see figure 5). This lets the catheter drain using gravity.
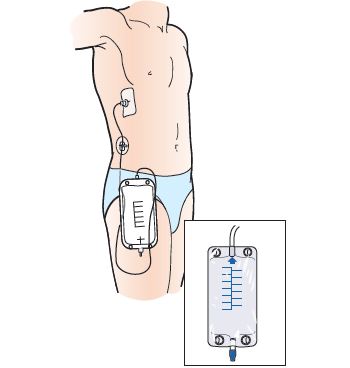
Figure 5. Drainage bag below the catheter
- Check to see that the fluid is draining into the new tubing.
- When you have finished, take off your gloves and wash your hands.
Change your CathGrip
The CathGrip will stop pulling, tension, or kinking of the drainage catheter and tubing. You will need your CathGrip kit for this part.
- Choose a position for the CathGrip. The CathGrip and drainage bag tubing should be below the catheter insertion site, both when you’re sitting and laying down. This will let it drain. The catheter should have a gentle bend and should not pull or have tension when it is attached.
- Rest the tubing on the side of your abdomen (belly) where you put the CathGrip.
- Check the site where you’ll place the CathGrip. Choose an area that’s not red or irritated. Use scissors or a hair trimmer to trim any long hairs at the site. Avoid using a razor.
- Open the CathGrip package.
- Clean the site with the alcohol wipe from the kit. This will get rid of oils and products from your skin, such as lotion or soap. Let the alcohol dry completely.
- Wipe the site with the BioPlus+ Skin Prep. This is included in the kit.
- Let area dry to the touch. This takes about 15 seconds.
- Take off the paper on the back of the CathGrip one side at a time (see Figure 4). Put in on your skin in the desired location. Do the same with the other side.
- Gently press the CathGrip to the skin for 5 seconds. This will seal it to the skin.
- Place the catheter on the device straps. There are 2 straps, one with holes and one with jagged edges. The strap with the holes has 2 openings. Put the strap with the jagged edges end into the lower opening of the other strap. Pull to secure (see Figure 6).
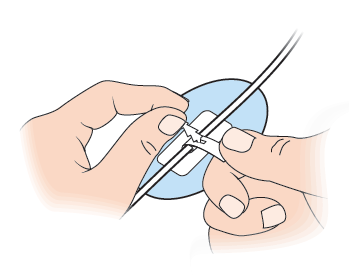
- Change the position of the catheter in the CathGrip if you notice any tension or pull.
Activities while you have your drainage catheter
- You can go to work and exercise with your catheter in place. Avoid movements that involve stretching from side to side or repeated bending. These could cause the catheter to move.
- Do not swim, take a bath, or put your catheter underwater. Talk with your Interventional Radiology doctor if you have a vacation planned. They can teach you what to do in this situation.
- The suture that holds the catheter in place can get uncomfortable. This usually happens if the suture gets pulled away from the skin. To prevent or lower the risk of this, make sure the catheter is not pulled when attaching the CathGrip. Always keep the tubing secured to your body with a CathGrip.
- Be sure not to tug on the catheter when you are getting dressed. Do not let clothing, such as pantyhose or a belt, kink the tubing. Clothing can usually cover the catheter.
- Try not to lie on your catheter when you sleep. This helps stop the catheter from kinking.
When to call your healthcare provider
Call your healthcare provider if you notice any of the following:
- The catheter is not draining, or the amount of drainage is much less than usual.
- The drainage looks bloody.
- There is leakage around the insertion site.
- You cannot flush the catheter, or it is difficult to flush.
- The catheter leaks when you flush it.
- The location of the black mark has changed.
- The catheter does not drain when the 3-way stopcock is in the upright position.
- The clamp is open or broken.
- You cannot straighten a kink in the tube that is causing a blockage.
- You have pain, tenderness, or swelling at the catheter site.
- Your skin around the catheter looks red, irritated, or different than usual.
- You have chills, or a fever of 100.4 °F (38 °C) or higher.
- You have any concerns about your catheter.
Ordering supplies
Your healthcare provider will give you enough supplies to last for 2 weeks. When you need more supplies, you can order them through your visiting nurse service. If you’re not able to order supplies through your visiting nurse service, call your IR doctor’s office.
- 3-way stopcock
- Adhesive Remover (1 box)
- Alcohol Wipes (1 box)
- Aquaguard (1 package)
- Argon Drainage bag (each)
- CathGrip (each)
- Drainage Discharge Kit
- Microfoam tape (1 box)
- Needless connector
- Non-sterile gloves (1 box)
- Plain gauze (1 package)
- Skin Prep (1 box)
- Telfa (each)
Prefilled syringes
You will need a prescription for prefilled normal saline syringes. You can get the prescription from the IR clinic.
If your local pharmacy does not have the syringes, you can get them from the outpatient pharmacy at Memorial Hospital. It’s open Monday through Friday, from to To reach the pharmacy, call 646-888-0730.
MSK also has retail pharmacies in other locations. Visit www.msk.org/locations/visiting-us/retail-pharmacy to find an MSK retail pharmacy near you.
Learn about our Health Information Policy.