At Memorial Sloan Kettering, our multidisciplinary team will devise a treatment strategy for you based on the stage of the cervical cancer, the size of the tumor, the surrounding tissues that may be affected, and whether the cancer has spread to other parts of the body. We also take into consideration your age and whether you wish to have children.
The earlier that cervical cancer is diagnosed and treated, the more likely it can be effectively cured. We typically treat cervical cancer with surgery, in some cases combined with radiation therapy, chemotherapy, or both.
For early-stage cancers in which abnormal cells are found in the cervix, our doctors may recommend a loop electrosurgical excision procedure (LEEP), in which an electrical current through a thin wire loop is used to remove the sample tissue. LEEP takes only about ten minutes under local anesthetic.
Alternatively or in addition to a LEEP procedure, our doctors may recommend a cone biopsy (conization) to more precisely remove a cone-shaped piece of tissue from the cervix with a scalpel. A cone biopsy is performed in an operating room and may include general anesthesia.
More than 90 percent of early-stage cancers are treated successfully with these surgical procedures and do not require any further treatment.
Minimally Invasive Surgery
For early-stage cervical cancers that are confined to the cervix, our doctors may recommend a hysterectomy, a type of surgery that involves removing the uterus entirely. The surgeon may also need to remove some tissue next to the uterus and cervix, as well as lymph nodes from the pelvis, to examine them for cancer cells.
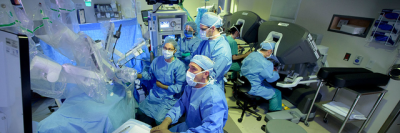
At Memorial Sloan Kettering, the majority of these operations, known as radical hysterectomies, are performed minimally invasively — either with laparoscopy or robotics. Our surgeons have been leaders in adopting these techniques, which typically offer several advantages over traditional, open abdominal surgery for early-stage as well as more-advanced cervical cancer, such as shorter hospital stays, less risk for infection, and lower cost.
With laparoscopy, a thin, lighted tube with a video camera at its tip (a laparoscope) is inserted through a tiny incision in the abdominal wall. The surgeon can operate through this minor surgical “port” using specially designed surgical instruments.
We were also the first cancer hospital to acquire the state-of-the-art robotic da Vinci® Surgical System platform to assist in minimally invasive cancer surgeries. The use of this system during surgery can often result in less pain and faster recovery for patients.
Sentinel Lymph Node Mapping and Biopsy
To remove as few pelvic lymph nodes as possible when assessing the extent to which cervical cancer has spread, Memorial Sloan Kettering doctors pioneered an approach called sentinel lymph node mapping (or intraoperative lymphatic mapping). Today, we are one of the few cancer hospitals in the United States using this approach.
Sentinel Lymph Node Mapping for Gynecologic Cancers
During many cervical cancer surgeries, we use a dye that can be traced with imaging techniques to identify the first lymph node (the sentinel node) to which cancer cells would travel after leaving the cervix. If this node is free of cancer cells, our surgeons do not remove additional lymph nodes. If the sentinel node does contain cancer cells, the surgeon removes additional lymph nodes for further examination.
The goal of using this technique is to treat the cancer while removing as few lymph nodes as possible, which can result in a shorter surgery and fewer side effects such as swelling of the legs, known as lymphedema.
Fertility-Sparing Radical Trachelectomy
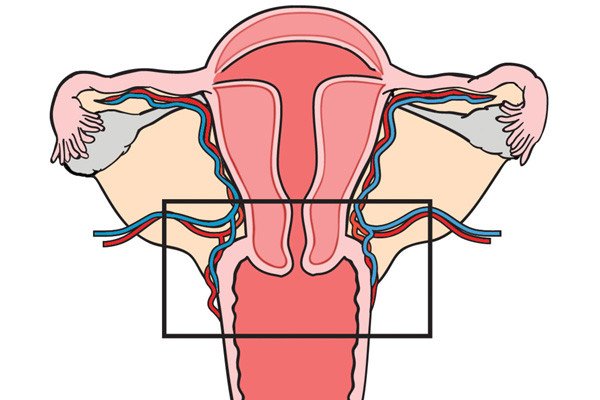
If you are a woman of childbearing age with early-stage cancer and you think you may wish to become pregnant at some point, our doctors can in many cases offer you a novel surgical approach called fertility-sparing radical trachelectomy.
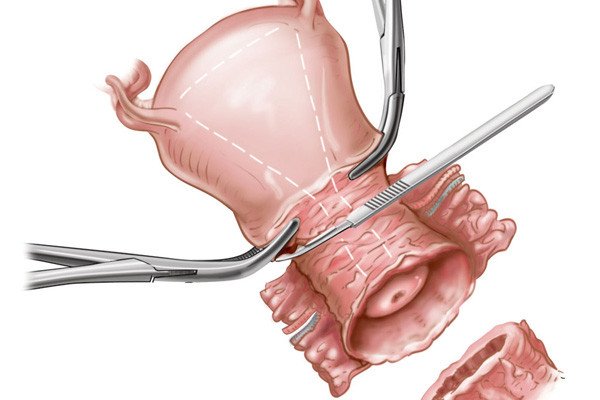
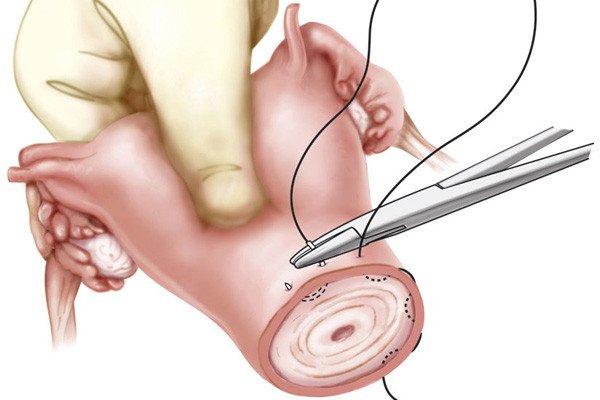
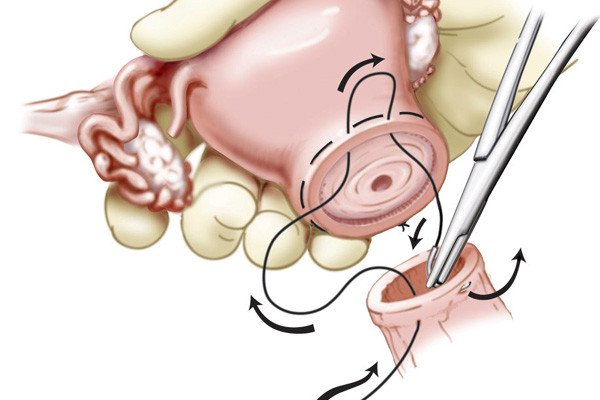
During a radical trachelectomy, the surgeon starts with either a minimally invasive surgery (laparoscopy) or an open, traditional surgery to identify and remove the sentinel lymph node. A pathologist will then test the sentinel lymph node for cancer. If it is cancer-free, only partial removal of the cervix is needed, thereby avoiding the need to remove the entire uterus. This preserves the ability of a woman to conceive a child in the future, with delivery by cesarean section.
Due to refinements made by our surgeons, radical trachelectomy can be an effective way to remove early-stage cervical cancer without compromising your outcome. As of 2011, Memorial Sloan Kettering surgeons have performed more than 100 radical trachelectomies, making it the largest program of its kind in the United States. The majority of women attempting conception after this procedure are successful, and most babies are delivered full term.
We’re available 24 hours a day, 7 days a week