
A study by Memorial Sloan Kettering (MSK) recently published in JAMA Oncology (1) showed that radiation dose to the elective regions can be safely de-escalated for patients with human papillomavirus (HPV)-associated oropharyngeal cancer (OPC) who received concurrent chemotherapy.
In this study of 276 patients with HPV-OPC who received this radiation treatment with a de-escalated elective dose along with platinum-based chemotherapy:
- Locoregional control was 97%
- Progression-free survival was 88%
- Distant metastasis-free survival was 95.2%
- Overall survival rate at two years was 95%
The standard approach for treating HPV-OPC has been a dose of 70 Gy to the primary site of gross pathology and 50–60 Gy to the elective area that could potentially harbor microscopic subclinical disease. Due to the anatomic size of the elective area, high-dose radiation to a large region of the head and neck is associated with significant morbidity, including the need for feeding tube placement.
“This approach has decreased toxicity for all HPV-OPC patients who receive chemotherapy,” says radiation oncologist Nancy Lee, MD. “The difference in toxicity is dramatic.”
MSK radiation oncologists first established an effective de-escalation treatment for patients with HPV-OPC in 2015. In this study (2), Dr. Lee led a multidisciplinary team that combined a specialized PET scan imaging protocol augmented with genomic analysis suggesting 30 Gy therapy was effective to treat the majority of patients with HPV-OPC.
“Patients treated with conventional radiation approaches receive a huge dose in a large elective area of the head and neck during the first treatment portion of five or six weeks,” says radiation oncologist C. Jillian Tsai, MD, PhD . “That is very toxic, and we have been able to show that it’s not necessary to be effective. Our approach of 30 Gy (instead of 50–60 Gy), followed by 40 Gy works just as well, while greatly reducing side effects.”
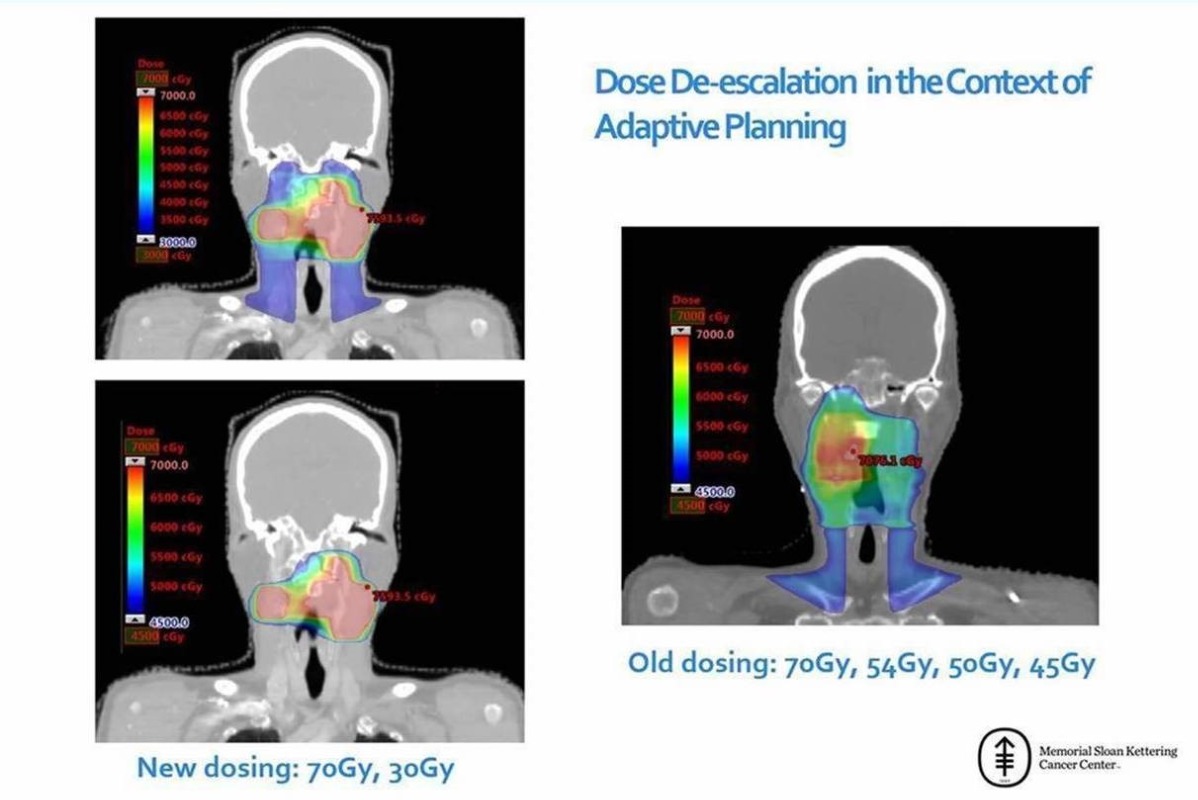
MSK has developed a novel treatment plan that can target the complex disease of HPV-OPC. It involves an initial 30 Gy over three weeks to subclinical regions, followed by a cone down of 40 Gy to both the site of gross pathology and the elective area, including suspected lymph nodes. The primary tumor still receives a total of 70 Gy but customized to the individual patients based on their treatment response, while doses to subclinical regions are substantially reduced.
This hybrid approach means a larger patient group can benefit from treatment while reducing the toxicity from standard therapy.
With additional studies already in progress, “We hope that in the future, many people with HPV-positive throat cancer will be able to receive an even less invasive, less intense, and more precise treatment,” says Dr. Lee.
Key Study Findings and Implications
- HPV-OPC is associated with significant morbidity using conventional radiotherapy
- MSK has developed a hybrid protocol to reduce radiotherapy toxicity to regions surrounding the primary tumor
- This treatment protocol has been shown to be both safe and efficacious in treating patients with HPV-OPC
Learn more about MSK’s Department of Radiation Oncology.
C. Jillian Tsai reports serving as a consultant for Varian Medical Inc.
- Tsai CJ, McBride SM, Riaz N, et al. Evaluation of Substantial Reduction in Elective Radiotherapy Dose and Field in Patients With Human Papillomavirus-Associated Oropharyngeal Carcinoma Treated With Definitive Chemoradiotherapy [published online ahead of print, 2022 Jan 20]. JAMA Oncol. 2022;e216416.
- Riaz N, Sherman E, Pei X, et al. Precision Radiotherapy: Reduction in Radiation for Oropharyngeal Cancer in the 30 ROC Trial. J Natl Cancer Inst. 2021;113(6):742-751.
- Tsai CJ, McBride SM, Riaz N, Lee NY. Reducing the Radiation Therapy Dose Prescription for Elective Treatment Areas in Human Papillomavirus-Associated Oropharyngeal Carcinoma Being Treated With Primary Chemoradiotherapy at Memorial Sloan Kettering Cancer Center. Pract Radiat Oncol. 2019;9(2):98-101.
- Phase II Trial: Adaptive Radiotherapy for Head and Neck Cancer
In addition to doctors C. Jillian Tsai and Nancy Lee, the following MSK authors on the JAMA Oncology paper are Sean M. McBride, Nadeem Riaz, Jung J. Kang, Daniel J. Spielsinger, Todd Waldenberg, Daphna Gelblum, Yao Yu, Linda C. Chen, Kaveh Zakeri, Richard J. Wong, Lara Dunn, David G. Pfister, Eric J. Sherman.