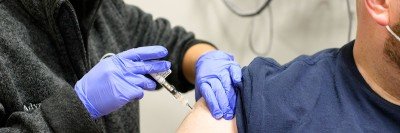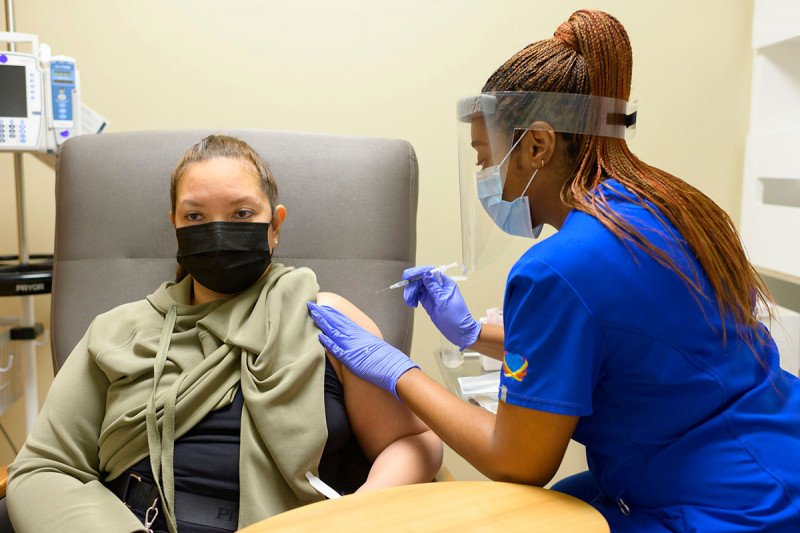
Memorial Sloan Kettering Cancer Center (MSK) and the Centers for Disease Control and Prevention (CDC) recommend people with cancer stay up-to-date on their COVID-19 vaccinations.
If you have cancer, you may have a weakened immune system (called immunocompromised). This can put you at higher risk for severe COVID-19. Protecting yourself from COVID-19, including getting vaccinated, is very important.
Mini Kamboj, MSK’s Chief Medical Epidemiologist, explains what you need to know about COVID-19 vaccines if you’ve had cancer.
This information is for people with weakened immune systems (called immunocompromised).
If you are not immunocompromised, please visit the CDC’s website for information about how many vaccine doses you should get and when:
What to know about the 2025–2026 COVID-19 vaccine
The 2025–2026 COVID-19 vaccine targets the variants that are going around now and expected to spread in the fall and winter seasons.
Everyone ages 6 months and older is eligible to get the 2025–2026 COVID-19 vaccine. If it’s been 3 months since your most recent COVID-19 vaccination or since you were infected with COVID-19, you should get the shot.
MSK recommends that all our patients get vaccinated as soon as they are eligible.
Should I get the 2025–2026 COVID-19 vaccine if I have cancer or have been treated for it?
Yes. The 2025–2026 COVID-19 vaccine is safe and recommended for people who have cancer or have been treated for it. COVID-19 has become less of a threat for some people. But it can still cause severe illness in people with medical conditions, such as cancer.
The latest CDC estimates show that about 1 in 6 people hospitalized with severe COVID-19 have weakened immune systems. This can happen if you are getting cancer treatment or have a history of cancer. The COVID-19 vaccine protects you from getting very sick if you get the infection.
How is the 2025–2026 COVID-19 vaccine different from the shots I already got?
The COVID-19 virus keeps changing. The vaccines are updated to match the latest versions of the virus. The 2025–2026 vaccine protects against newer strains that are now more common.
The updated vaccine replaces earlier COVID-19 vaccines. It’s designed to give you the best protection against getting very sick from the virus.
How effective is the COVID-19 vaccine for people with weakened immune systems?
The COVID-19 vaccine helps protect people with weakened immune systems from getting very sick or needing to go to the hospital. This includes people with cancer and weakened immune systems, and those ages 65 and older.
Immunity from vaccines fades after about 2 months. That’s why it’s important to stay up-to-date with the latest version of the vaccine. If you have a weakened immune system, you may need extra doses every 2 to 6 months.
Can I get the COVID-19 vaccine at the same time as my flu shot or my RSV shot?
You can get the flu, RSV, and COVID-19 vaccines at the same time.
I got COVID-19 recently. Do I still need to get the 2025–2026 COVID-19 vaccine? If so, when?
Yes. Even if you’ve had COVID-19, your immunity after infection fades over time. Getting vaccinated is a safer and more reliable way to stay protected. You should wait 3 months after your symptoms started, or after a positive result if you had no symptoms, before getting the 2025–2026 COVID-19 vaccine.
Is the COVID-19 vaccine safe?
Yes, the 2025–2026 COVID-19 vaccine is safe. It works in the same way as the original COVID-19 vaccines and all booster shots. They are made using the same process.
For all versions of COVID-19 vaccines, serious side effects have been very rare, and they are treatable. Read more about side effects and rare, serious health problems that have been reported after COVID-19 vaccination.
What are the possible side effects of the COVID-19 vaccine?
You could have soreness at the injection site, fatigue, headache, body aches, and fever. These symptoms don’t last long — about 1 to 3 days.
If you do have side effects, you can take an over-the-counter drug such as Advil or Tylenol to lower a fever, reduce chills, or relieve a headache or body aches.
Can the COVID-19 mRNA vaccines cause cancer?
No. COVID-19 mRNA vaccines do not cause cancer or make cancer come back. There is no scientific evidence to suggest that any vaccine, including mRNA vaccines, cause cancer or make it come back.
In fact, some vaccines help prevent cancer. For example, the Hepatitis B and Human Papilloma Virus (HPV) vaccines protect against infections that can lead to liver and cervical cancer.
It is also worth knowing that the same mRNA technology used in COVID-19 vaccines is now being studied as a way to stop cancer from coming back.
Should my caregivers get the COVID-19 vaccine?
Yes. When everyone in your household and close circle are vaccinated, it helps protect you and them. Vaccinated people are nearly half as likely to spread infections to others in their home compared with people who are not vaccinated.
Who is at risk for severe COVID-19
The CDC says that people who are “moderately to severely immunocompromised” are at increased risk of severe COVID-19 illness.
This includes:
- People with blood cancer.
- People who are actively being treated for solid tumors with chemotherapy — and some people being treated with immunotherapy.
- People without a functioning spleen (called asplenia).
- People who have had a stem cell transplant or received CAR T therapy within the past 2 years.
- People who are actively being treated for graft-versus-host-disease (GVHD) with immunosuppressive drugs (for example, sirolimus or Rapamune®).
- People with primary immunodeficiency disorders (for example, DiGeorge syndrome, Wiskott-Aldrich syndrome).
- People with active or untreated HIV infection.
- People actively using high-dose steroids (for example, 20mg of prednisone or more per day for at least 2 weeks).
- People actively being treated for an immune-related disease (for example, rheumatoid arthritis, Crohn’s disease, or psoriasis) with a tumor necrosis factor (TNF) inhibitor (for example, adalimumab or Humira®).
These eligibility criteria cover the most common situations. If you are receiving another treatment that has weakened your immune system, your doctor will be able to advise you about getting the COVID-19 vaccine.
Revaccination after certain treatments
Certain cancer treatments can completely or partially wipe out a patient’s immune system. Because of this, anything that your immune system learned before cancer treatment now may be completely gone. Your immune system needs to relearn how to fight COVID-19.
If you received any COVID-19 shots before, during, or shortly after cancer treatment, you may need to be revaccinated if your doctor thinks your immune system has recovered enough to respond to the vaccines.
Everyone who is currently eligible to be vaccinated is also eligible to be revaccinated if they received any of these treatments:
- Hematopoietic cell transplantation (also called a bone marrow transplantation or stem cell transplantation)
- CAR T therapy
- Treatment with B cell depleting drugs such as rituximab (Rituxan®)
Your healthcare team will determine whether you should be revaccinated and the best time to get the shots. Only healthcare providers can order revaccination for their patients after careful evaluation of eligibility. If you think you meet any of the criteria for revaccination, you should talk to your healthcare team.
How else to protect yourself from COVID-19
Even when you are completely up-to-date on your COVID-19 shots, you must still take certain precautions to protect yourself and your loved ones from COVID-19. You should:
- Wear a mask indoors and outdoors when you are around anyone you don’t live with.
- Wash your hands frequently for at least 20 seconds.
- Stay 6 feet apart from others you don’t live with.
- Avoid crowds and indoor spaces that are poorly ventilated.
- Encourage your close friends, family members, neighbors, and co-workers to be vaccinated.
- If you develop symptoms of COVID-19, contact your MSK care team and get tested.
How to get a COVID-19 vaccine
Starting October 1, 2025, we will have the 2025–2026 COVID-19 vaccine available for our patients. Ask a member of your care team for more information.
You don’t have to get vaccinated at MSK. You also don’t need a prescription to get a 2025–2026 COVID-19 vaccine in many states, including New York, New Jersey, and Connecticut. Go to vaccines.gov to find a place near you where you can get a vaccine. Most health insurance plans cover the COVID-19 vaccine, so you won’t have any out-of-pocket costs.
October 1, 2025