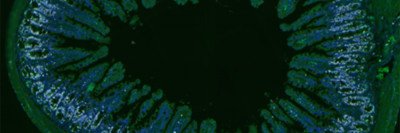
Mouse Intestinal Tissue
Graft-versus-host disease (GVHD) is a major complication of bone marrow transplantation, which is used to treat advanced blood cancers and other blood-related diseases. GVHD occurs when donor immune cells called T cells attack healthy tissues in the recipient.
One form of GVHD involves damage to the gut, or gastrointestinal tract. This can cause nausea, pain, diarrhea, and other symptoms. Researchers have shown that this damage is caused by T cells from the donor that travel to the gut, leading to impairment of the epithelial layer, which lines the surface of the organ.
What has not been clear is exactly where the T cells are attacking the intestinal tissue, or which specific cells are affected. Now, Memorial Sloan Kettering researchers in the laboratory of Alan Hanash have answered that question. They have demonstrated that T cells preferentially target a site in the intestines called the stem cell compartment. The findings suggest that drugs recently approved to treat inflammatory bowel disease may be effective in treating GVHD by protecting intestinal stem cells from the donor’s immune cells.
Pinpointing the Damage Site
The epithelial layer consists of tight folds that create fingerlike projections called villi. At the base of the villi are tiny pockets called crypts. The intestinal stem cell compartment located at the base of the crypts contains two types of cells: stem cells and niche cells. Stem cells can develop into many different cell types. These stem cells replenish the mature epithelial cells in the villi when they die. The niche cells help nurture and support the stem cells.
In previous research, Dr. Hanash’s lab found that stem cells in the crypts become depleted in mice with GVHD. The donor T cells are somehow responsible for this stem cell reduction. But is it a direct attack?
“We needed to find out the nature of the damage to the stem cells,” Dr. Hanash says. “Are the T cells actually targeting the stem cells themselves, or do they attack the niche that supports the stem cells? Or are they really targeting the entire gut, and as a part of damaging everything, you lose some stem cells?”
Now, they have the answer: T cells go straight to the crypts and attack the stem cell compartment. This finding, published in Immunity, could help researchers find ways to block this damage following a transplant.
Visual Virtuosity
What is both impressive and critical to the success of this project is how this discovery was made — through a virtuosic feat of imaging by Ya-Yuan Fu, a researcher in the Hanash laboratory. Dr. Fu developed a way to visualize the T cells, the intestinal tissue, and its epithelial lining using an approach called 3-D microscopy.
“Tracking the location of T cells in the gut has been difficult,” Dr. Hanash says. “Normally we get a two-dimensional image that is just a slice of what is going on in the tissue. Dr. Fu used her skills to generate these incredible high-resolution 3-D images that keep it all together and show everything.”
One surprise revealed by the imaging was how the T cells migrate to the crypt. T cells primarily use vasculature (blood vessels) to circulate and move into tissues. The vasculature is much denser in the villi, where the mature epithelial cells are. It would seem more straightforward for the T cells to migrate primarily to the villi. But that does not happen.
The reason for this appears to be a molecule called MAdCAM-1. It is present on the surface of intestinal blood vessels and was already known to play a role in attracting T cells to the intestines. Dr. Fu’s imaging experiments revealed that blood vessels expressing MAdCAM-1 are more abundant near the crypts than in the villi. This draws most of the T cells toward the crypt region.
“The data suggests that the amount of MAdCAM-1 in a certain region of tissue correlates directly with T cell invasion and with stem cell injury,” Dr. Fu says.
Protection for Stem Cells
As a final step, the researchers proved in mice that blocking the interaction between MAdCAM-1 and T cells reduces T cell invasion of the crypt and protects stem cells after bone marrow transplantation.
“Therapies that block this interaction might protect transplant patients from intestinal complications of GVHD,” Dr. Hanash says. The US Food and Drug Administration has already approved drugs like this for inflammatory bowel disease, and they are currently being tested against GVHD in clinical trials.
“Our findings reveal exactly why these drugs could be effective,” he says. “Not just by preventing T cells from getting to the gut in general but by preventing them from going to the crypts and the stem cell compartment.”
This research was supported by National Institutes of Health award numbers K08-HL115355, R01-HL125571, R01 HL146338, and P30-CA008748. Support was also received from the Susan and Peter Solomon Divisional Genomics Program, the Parker Institute for Cancer Immunotherapy, the Ludwig Center for Cancer Immunotherapy, and the Anna Fuller Fund. Dr. Hanash received additional support from the Amy Strelzer Manasevit Research Program and a Scholar Award from the American Society of Hematology. Dr. Fu received additional support from a New Investigator Award from the American Society for Blood and Marrow Transplantation (now renamed as the American Society for Transplantation and Cellular Therapy) and Sanofi Genzyme. Dr. Hanash has consulted for Ziopharm and Nexus Global Group.