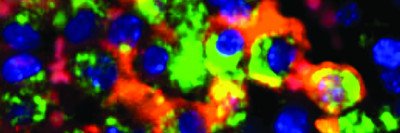
Multiphoton Microscopy
What it does: Using multiphoton microscopy, researchers can conduct high-resolution live imaging deep within a tissue. The method enables scientists to peer inside tumors to get a detailed view of cells in action.
The problem it solves: Getting a clear picture of how cells interact is essential to understanding how cancer develops and progresses. But studying this activity in a living person is challenging because most of the interesting and biomedically relevant interactions take place below the surface.
Why it’s important: Live imaging within tumor tissue can reveal important new insights into how the body reacts when cells turn cancerous. One critical aspect is the response of the immune system. What are the first signals sent to sound the alarm and draw immune cells to infiltrate the tumor? How do these immune cells interact with the tumor? What do they do to destroy it, or are they hijacked by the tumor for its own needs?
What MSK experts say: The multiphoton microscope, arriving in late 2017, will be housed in the lab of Sloan Kettering Institute immunologist Morgan Huse but will be accessible to any MSK researcher interested in studying dynamic behavior in tissues. Dr. Huse will primarily be using the microscope to study the interaction between immune cells and tumor cells. In experiments, the lens of the microscope could be placed against a tumor to capture live images of cell activity inside. “An analogy would be the difference between watching a zebra on a savannah as opposed to seeing it at the zoo,” Dr. Huse explains. “There are certain questions you can’t address outside the complex tissue environment that immune cells navigate in a live animal.”

Multiplexed Ion Beam Imaging (MIBI)
What it does: MIBI, which is scheduled to arrive at MSK in January, is one of the newest imaging technologies to hit the field of single-cell biology. It allows researchers to simultaneously measure 50 to 100 different molecules produced by a cell with subcellular resolution. The approach leaves tissue sections intact, preserving relationships between individual cells, including those of a tumor.
The problem it solves: To understand many issues in cancer biology, it helps to know which cells are making which molecules, in what amounts, and where they are in relation to one another and to the tumor. Scientists typically obtain that information through immunohistochemistry, in which antibodies tagged with a fluorescent or colored label bind to those molecules and are visualized under a microscope. Using this method, scientists can identify only a handful of different molecules at once. MIBI uses something called mass spectrometry, in which specific metals give off ions of different weights when sprayed with a beam of electrons. Rather than trying to distinguish between colors, scientists can measure these ions precisely and use them to generate a profile of the molecules that are present. Two- and three-dimensional images can then be generated for every cell in the sample.
Why it’s important: MIBI allows scientists to measure the delicate molecular architecture of a tissue, at a cellular and subcellular level. They can determine exactly what immune cell types reside in a tumor, for example, and what characteristic molecules they are making. That will lead to the design of smarter clinical trials, and ultimately to better treatments.
What MSK experts say: Pathologist Travis Hollmann and Dana Pe’er, Chair of Computational and Systems Biology, will be overseeing the tool’s operation at MSK. “MIBI represents an enormous step forward for single-cell biology,” Dr. Hollmann says.
Machine Learning for Digital Pathology
What it does: MSK data scientist Thomas Fuchs is using machine learning, a type of artificial intelligence (AI), to train computers to recognize cancer on digitized pathology slides. As part of the effort to harness AI technology, the Department of Pathology is digitizing more than 40,000 pathology slides per month. A new innovation center, the Warren Alpert Center for Digital and Computational Pathology at MSK, was also established to improve diagnostic efficiency and accuracy while exploring new techniques to study the morphology (the form and structure) of tumor samples. One goal is to teach computers to recognize certain features in tumors. Through massive data analysis, computers will eventually be able to identify cancer within a sample, as well as determine subtle variations, such as subtypes and degrees of aggressiveness. Dr. Fuchs, who studied machine learning at private companies and academic institutions before being recruited by NASA’s Jet Propulsion Laboratory, explains that the principles of space exploration translate well to pathology. “Some of the same algorithms we used for the Mars Rover to recognize different kinds of terrain, like sand and rocks, we can use to differentiate cancer versus benign tissue on slides.” As a first step, Dr. Fuchs’s lab is training a computer with data from 15,000 prostate cancer biopsy slides taken at MSK in 2016.

The problem it solves: Cancer pathologists can spend hours each day studying slides that may yield little useful information. A single prostate biopsy, for example, can produce 50 slides that must be reviewed. What’s more, determining whether tissue is malignant and assigning it a grade is still subjective. MSK is aiming to speed slide analysis and archiving as well as make pathologic analysis more objective.
Why it’s important: According to Dr. Fuchs and David Klimstra, Chair of the Department of Pathology, the technology can free pathologists to focus less on slide review and more on important questions regarding how cancer behaves. Drs. Fuchs and Klimstra expect that in the short term, the computers should increase efficiency by detecting the most relevant slides for pathologists to focus on, reducing the number they have to review. In the longer term, the hope is that the computers can provide new insights by establishing morphologic correlations not possible using current technology.
What MSK experts say: “We are hoping to improve efficiency but also to superimpose higher-level machine learning to better understand disease,” says Dr. Klimstra. “We’re trying to change how pathology is practiced, not just at MSK but in all communities.”

Vascular-Targeted Photodynamic (VTP) Therapy
What it does: The technology uses a light-sensitive drug and thin optical fibers that give off a particular wavelength of light to destroy tumors with virtually no side effects. The drug is injected into the blood- stream. When it encounters the light from the fibers, which are inserted into the prostate, the drug generates unstable molecules called free radicals. These destroy tumor cells and the small blood vessels that feed them.
The problem it solves: It could enable many men with prostate cancer to avoid surgery or radiation and the risk of complications those procedures entail. In some cases, VTP therapy could be offered to men who otherwise might choose to undergo active surveillance, an approach in which those with low-risk cancers forego immediate treatment for close observation. Some patients under active surveillance see their cancer progress to the point where it needs treatment by surgery or radiation. Having the option to destroy the tumor earlier with minimal ill effects would prevent the need for more-aggressive treatment down the road.
Why it’s important: Most men receiving VTP therapy have little to no sensation that they have even been treated. In fact, the first patient whom urologic surgeon Jonathan Coleman treated said he felt nothing at all. Dr. Coleman was convinced he had done the procedure wrong. “And yet, when we looked at the MRI a few days later, the tumor was gone,” he says. VTP therapy has potential for treating other cancer types as well. MSK is collaborating with the Weizmann Institute of Science in Israel to begin clinical trials testing the technology in bladder cancer, esophageal cancer, breast cancer, and pancreatic cancers.
What MSK experts say: “Many prostate tumors are not life-threatening, but men are understandably reluctant to let them linger,” Dr. Coleman says. “By selecting the right patients, we may be able to treat a large number of tumors effectively with a greatly reduced risk of complications, such as impaired urinary control and sexual function, that lower quality of life.”