This information explains what to expect during and after your child’s ophthalmic (op-thal-mik) artery chemosurgery (OAC).
MSK’s retinoblastoma team has recommended ophthalmic artery chemosurgery (OAC). This is a treatment to treat tumors in your child’s eye. Retinoblastoma is cancer of the eye.
The chemotherapy is injected (put) right into your child’s ophthalmic artery, a blood vessel in the eye. We will do this procedure in an outpatient setting, which means your child will not be admitted to the hospital.
We will do this procedure at New York-Presbyterian/Weill Cornell Medical Center, near MSK. It will be done by an interventional radiologist, a doctor with special training in image-guided procedures.
Your child must stop eating and drinking before their procedure. The Weill Cornell staff will give you information on when your child should stop eating and drinking.
About your child’s procedure
Your child will be given general anesthesia (medicine to make them sleep). Once they’re asleep, they may have an intravenous (IV) line inserted.
They also will insert a tiny catheter, a small, flexible tube thinner than angel hair pasta. It will go into 1 of your child’s femoral arteries, which are blood vessels in the upper leg. They will thread the catheter through the arteries up to the ophthalmic artery (see Figure 1).
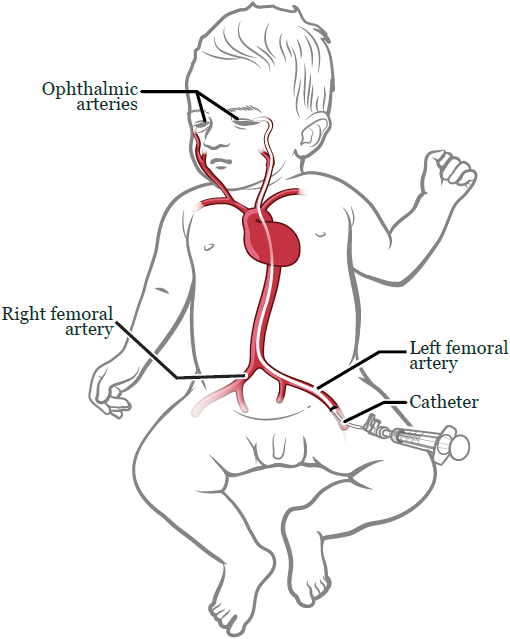
Tiny drops (about ⅕ of a teaspoon) of chemotherapy will be placed into the catheter and will go into the eye(s) that needs to be treated. Based on the size and features of your child’s retinoblastoma, they may get 1 to 3 of these chemotherapy medicines:
- Melphalan (Alkeran®, Evomela®)
- Topotecan (Hycamtin®)
- Carboplatin (Paraplatin)
After the chemotherapy is injected, the catheter will be taken out. They will place a large bandage on the insertion site on your child’s upper leg. The nurse will also put a knee brace on your child to keep their leg straight. This will help avoid bleeding.
This procedure takes about 60 to 90 minutes.
After your child’s procedure
- When your child wakes up, they will be in the Post Anesthesia Care Unit (PACU). This is the recovery room. They will spend at least 5 hours in the PACU.
- While your child is in the PACU, their nurse will check their upper leg and take their pulse on their foot.
- The nurse will let you know when your child can start drinking and eating again.
- The knee brace will be taken off once your child is ready to be discharged (leave the hospital).
- Make sure your child’s bandage stays on for 24 hours (1 day). Do not get the bandage wet.
Medicines
- The doctor or nurse practitioner may prescribe your child a steroid to take by mouth called Dexamethasone Intensol. It will help with the swelling and irritation in their treated eye. Your child should take this medicine with food to prevent stomach discomfort, as instructed by their doctor or nurse.
- Your child may be prescribed ondansetron (Zofran®, Zuplenz®) for nausea (feeling like you may throw up) or vomiting (throwing up). Have your child take this medicine as instructed by their doctor or nurse.
- Your child may also be prescribed tobramycin and dexamethasone (TobraDex®) eye ointment or drops. This medicine is a combination of an antibiotic and steroid. It helps with swelling and prevents infection in the treated eye. Give this medicine to your child as instructed by their doctor or nurse.
Side effects
Your child may have some side effects after their procedure. These include:
- Nausea
- Vomiting
- Redness, swelling, or bruising in their upper leg
- Swelling in their treated eye. This can make it hard for your child to open their eye.
- Mild discomfort in their treated eye
These side effects will get better 2 to 3 days after the procedure. Some swelling can last for up to 2 weeks.
Some side effects start 1 to 2 weeks after the procedure. These can include:
- Loss of eyelashes in their treated eye
-
A lower white blood cell count, also called neutropenia. This can raise your child’s risk for infection.
- For more information on neutropenia, read the resource Neutropenia (Low White Blood Cell Count).
- Redness above the eyebrow and forehead of their treated eye. This can last many weeks.
Follow-up
Your child must have their blood drawn 10 days after their procedure. You or your healthcare provider must fax these results to Weill Cornell at 212-746-6653 and to MSK at 646-227-7275.
Call your child’s healthcare provider if they have:
- Redness or swelling in the treated eye that lasts more than 2 weeks
- More redness, swelling, or pain in their upper leg
- Nausea or vomiting that lasts longer than 2 to 3 days
- Trouble keeping down their prescribed medicine because of vomiting
- A fever of 100.4° F (38° C) or higher
- Pain in the treated eye that lasts more than a few days
Contact information
If you have questions or concerns about your child’s prescriptions or their procedure, call Weill Cornell. You can reach them Monday through Friday from to at 212-746-4998. After , during the weekend, and on holidays, call the office. Ask to talk with the doctor on call.
For all other questions, call the MSK Retinoblastoma Clinic. You can reach them Monday through Friday from to at 212-639-7232. After , during the weekend, and on holidays, call 212-639-2000. Ask to talk with the ophthalmologist (eye doctor) or pediatric fellow on call.
Learn about our Health Information Policy.