This information will help you get ready for your endoscopic submucosal dissection (en-doh-SKAH-piksub-myoo-KOH-sul dy-SEK-shun) procedure at MSK. Read this resource at least once before your procedure. Use it as a reference in the days leading up to your procedure.
What is an endoscopic submucosal dissection?

An ESD is a procedure to remove tumors in your digestive tract. Your digestive tract is made up of your esophagus (food pipe), stomach, small intestine, large intestine (colon), and rectum (see Figure 1).
A gastroenterologist (GAS-troh-EN-teh-RAH-loh-jist) will usually do your ESD during an endoscopy (en-DOS-koh-pee) procedure. A gastroenterologist is a doctor with special training in the gastrointestinal (GI) system. This includes the esophagus, stomach, and intestines.
Sometimes, the doctor cannot do an ESD during an endoscopy. Talk with your healthcare provider about what to expect and how to get ready for your ESD. Follow the instructions in this resource carefully.
During your procedure, your doctor will place a flexible tube, called an endoscope into your mouth. They will guide the endoscope down your esophagus, into your stomach, and into your small intestine (see Figure 1).
The scope is connected to a video monitor. This allows them to see the inside your intestines and look for anything that is not normal on the video monitor. They will use the scope to remove any tumors and stitch the area, if needed. When they’re finished, they will remove the scope.
Figure 2 shows the tumor removal process:
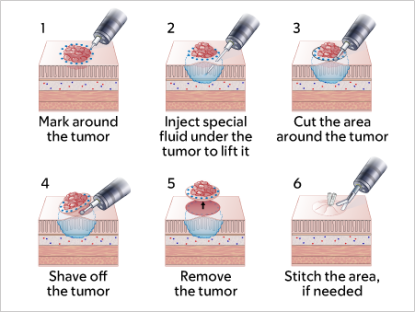
Your procedure usually takes 1 to 3 hours, but sometimes it may be longer.
What to do 2 weeks before your procedure
Ask about your medicines
You may need to stop taking some of your usual medicines before your procedure. Or, you may need to take a different dose (amount) than usual. Talk with your healthcare provider about how to take your medicines before your procedure. Do not change how you take your medicines without talking with a healthcare provider.
This section lists some examples of medicines, but there are many others. Make sure your care team knows all the prescription medicines, over-the-counter medicines, and dietary supplements you take. A prescription medicine is one you can only get with a prescription from a healthcare provider. An over-the-counter medicine is one you can buy without a prescription.
It’s very important to take your medicines and supplements the right way in the days before your procedure. If you don’t, we may need to reschedule your procedure.
Anticoagulants (blood thinners)
A blood thinner is a medicine that changes the way your blood clots. Blood thinners are often prescribed to help prevent a heart attack, stroke, or other problems caused by blood clots.
If you take a blood thinner, talk with the healthcare provider who scheduled your procedure and the healthcare provider who prescribes it. Ask them what to do before your procedure. They may tell you to stop taking the medicine a certain number of days before your procedure. This will depend on the type of procedure you’re having and the reason you’re taking a blood thinner.
Here are some examples of blood thinners. There are others, so be sure your care team knows all the medicines you take. Do not stop taking your blood thinner without talking with a member of your care team.
|
|
Other medicines and supplements can change how your blood clots. Examples include vitamin E, fish oil, and nonsteroidal anti-inflammatory drugs (NSAIDs). Ibuprofen (Advil®, Motrin®) and naproxen (Aleve®) are examples of NSAIDs, but there are many others.
Read How To Check if a Medicine or Supplement Has Aspirin, Other NSAIDs, Vitamin E, or Fish Oil. It will help you know which medicines and supplements you may need to avoid before your procedure.
Diabetes medicines
If you take insulin or other diabetes medicines, talk with your MSK healthcare provider and the healthcare provider who prescribes it. Ask them what to do before your surgery or procedure. You may need to stop taking it or take a different dose (amount) than usual. You may also need to follow different eating and drinking instructions before your surgery or procedure. Follow your healthcare provider’s instructions.
Your care team will check your blood sugar levels during your surgery or procedure.
GLP-1 medicines for weight loss
It’s important to tell your healthcare provider if you take a GLP-1 medicine. You will need to follow special eating and drinking instructions before your surgery or procedure. It is very important to follow these instructions. If you do not follow them, your surgery or procedure may be delayed or canceled.
- Follow a clear liquid diet the day before your surgery or procedure. Do not eat any solid food. Read Clear Liquid Diet to learn more.
- Stop drinking 8 hours before your arrival time. Do not eat or drink anything after this time, including clear liquids. You can have small sips of water with your medicines.
To learn more, read Eating and Drinking Before Your Surgery or Procedure When Taking GLP-1 Medicines.
Here are some examples of GLP-1 medicines. There are others, so be sure your care team knows all the medicines you take. Sometimes, these are prescribed to help manage diabetes or other conditions. Other times, they are prescribed for weight loss.
|
|
Get a letter from your healthcare provider, if needed
A clearance letter is a letter from your doctor that says it’s safe for you to have a procedure. You may need to get one or more clearance letters before your procedure. Your MSK healthcare provider will tell you if you do. They must have your clearance letter at least 1 day before your procedure.
Clearance letter for an automatic implantable cardioverter-defibrillator (AICD) or permanent pacemaker (PPM)
Tell your MSK healthcare provider if you have an AICD or PPM. You will need a clearance letter from your cardiologist (heart doctor).
Clearance Letter for Other Symptoms
You’ll need a clearance letter from a doctor if you’ve had any of these during the last 6 weeks:
- Chest pain.
- Trouble breathing that’s new or has gotten worse.
- Fainting.
What to do 1 week before your procedure
Stop taking certain medications
If you take aspirin, ask the healthcare provider that prescribes it to you if you can stop taking it 1 week before your procedure. Aspirin and medications that contain aspirin can cause bleeding. Read How To Check if a Medicine or Supplement Has Aspirin, Other NSAIDs, Vitamin E, or Fish Oil to learn more.
If your healthcare provider doesn’t want you to stop taking aspirin, tell the healthcare provider doing your ESD procedure at least 10 days before the procedure.
Arrange for someone to take you home
If your doctor cannot do an ESD during your procedure, you must have a responsible care partner take you home afterwards. A responsible care partner is someone who can help you get home safely. They should be able to contact your care team if they have any concerns. Make sure to plan this before the day of your procedure.
If you don’t have a responsible care partner to take you home, call one of the agencies below. They’ll send someone to go home with you. There’s a charge for this service, and you’ll need to provide transportation. It’s OK to use a taxi or car service, but you still need a responsible care partner with you.
| Agencies in New York | Agencies in New Jersey |
| VNS Health: 888-735-8913 | Caring People: 877-227-4649 |
| Caring People:877-227-4649 |
What to do 3 days before your procedure
An endoscopy nurse will call you between and 3 days before your procedure. They will review the instructions in this guide with you and ask you questions about your medical history. The nurse will also review your medications and tell you which medications to take the morning of your procedure.
What to do 2 days before your procedure
If you take an iron supplement, you’ll need to stop taking it 2 days before your procedure. Iron supplements can cause dark stains in your digestive (GI) path, which can make it harder for your healthcare provider to see it clearly.
What to do the day before your procedure
Note the time of your procedure
A staff member will call you after noon (12 p.m.) the day before your procedure. If your procedure is scheduled for a Monday, they will call you on the Friday before. If you do not get a call by , call 212-639-5014, or the Admissions Office at 212-639-7882.
The staff member will tell you what time to get to the hospital for your procedure. They will also remind you where to go.
If you need to cancel your procedure, call the GI scheduling office at 212-639-5020.
Instructions for eating
Stop eating at midnight (12 a.m.) the night before your surgery or procedure. This includes hard candy and gum.
Your healthcare provider may have given you different instructions for when to stop eating. If so, follow their instructions. Some people need to fast (not eat) for longer before their surgery or procedure.
What to do the day of your procedure
Instructions for drinking
Between midnight (12 a.m.) and 2 hours before your arrival time, only drink the liquids on the list below. Do not eat or drink anything else. Stop drinking 2 hours before your arrival time.
- Water.
- Clear apple juice, clear grape juice, or clear cranberry juice.
- Gatorade or Powerade.
-
Black coffee or plain tea. It’s OK to add sugar. Do not add anything else.
- Do not add any amount of any type of milk or creamer. This includes plant-based milks and creamers.
- Do not add flavored syrup.
If you have diabetes, pay attention to the amount of sugar in your drinks. It will be easier to control your blood sugar levels if you include sugar-free, low-sugar, or no added sugar versions of these drinks.
It’s helpful to stay hydrated before surgeries and procedures, so drink if you are thirsty. Do not drink more than you need. You will get intravenous (IV) fluids during your surgery or procedure.
Stop drinking 2 hours before your arrival time. This includes water.
Your healthcare provider may have given you different instructions for when to stop drinking. If so, follow their instructions.
Things to remember
- Take only the medications you were told to take the morning of your procedure. Take them with a few sips of water.
- Don’t put any lotions, creams, or powder on your chest or arms.
- Remove any jewelry, including body piercings.
- Leave all valuables, such as credit cards and jewelry, at home. There won’t be lockers available to store your valuables in.
- If you wear contacts, wear your eyeglasses instead.
What to bring
- Your rescue inhaler (such as albuterol (Ventolin®) for asthma), if you have one.
- A case for your eyeglasses.
- Your Health Care Proxy form, if you have completed one.
- If you have an implanted pacemaker or cardioverter-defibrillator (AICD), bring your wallet card with you.
Where to go
Your procedure will take place at one of these locations:
David H. Koch Center
530 East 74th Street
New York, NY 10021
Take the elevator to the 8th floor.
Endoscopy Suite at Memorial Hospital (MSK’s main hospital)
1275 York Avenue (between East 67th and East 68th Streets)
New York, NY 10065
Take the B elevator to the 2nd floor. Turn right and enter the Surgery and Procedural Center through the glass doors.
Visit www.msk.org/parking for information about parking at these locations.
What to expect when you arrive
When it’s time for your procedure, a member of your care team will bring you into the procedure room. Your care team will attach equipment to monitor your heart, breathing, and blood pressure. You’ll get oxygen through a thin tube that rests below your nose. They’ll also place a mouth guard over your teeth to protect them.
Your nurse or anesthesiologist will place an intravenous (IV) line into a vein, usually in your arm or hand. You’ll get anesthesia through your IV, which will make you fall asleep. Once you’re asleep, your doctor will start the procedure. Your procedure usually takes 1 to 3 hours, but sometimes it may be longer.
What to do after your ESD procedure
Inside the Post-Anesthesia Care Unit (PACU)
When you wake up, you’ll be in the PACU. Your nurse will continue to monitor your heart, breathing, and blood pressure.
If your doctor did an ESD, you’ll need to stay in the hospital overnight so your nurse can monitor you. You’ll move to an inpatient bed when one is available. If you do not have any issues overnight, you’ll be able to leave the hospital the next day.
If your doctor did not do an ESD, you can go home the same day. You must have a responsible care partner take you home afterwards.
At home
For the first 7 days after your procedure:
- Do not drink alcohol.
- Do not do any strenuous exercise (such as jogging and tennis).
- Do not lift anything heavier than 10 pounds (4.5 kilograms).
- Try to stay local, and don’t travel long distances, such as outside of the country.
Most people can go back to work 7 days after having this procedure, but everyone is different, so it may be shorter or longer for you. If you need to do a lot of heavy lifting at your job, talk with your healthcare provider before going back to work.
Follow-up care
You’ll have a follow-up visit with your healthcare provider 2 weeks after your procedure. During this visit, they will talk with you about your results and go over a treatment plan.
When to call your healthcare provider
Call your healthcare provider if you have:
- A fever of 101 °F (38.3 °C) or higher.
- Intense pain, hardness, or swelling in your abdomen (belly).
- Blood in your vomit (throw up).
- Intense throat pain that won’t go away.
- Weakness, faintness, or both.
- Dark stools (poop) or blood in your stool.
- Any other questions or concerns.
If you have chest pain or trouble breathing, call 911 or go to your nearest emergency room.
Contact information
If you have any questions or concerns, call Dr. Nishimura’s office at 212-639-6029, or Dr. Beauvais’ office at 212-639-5909. You can reach a staff member Monday through Friday from to After , during the weekend, and on holidays, call 212-639-2000 and ask for the GI doctor on call.
Learn about our Health Information Policy.
