This information will help you get ready for your Lutathera treatment at MSK. Lutathera is a type of peptide receptor radionuclide therapy (PRRT).
This information will help you get ready for your Lutathera treatment at MSK. Lutathera is a type of peptide receptor radionuclide therapy (PRRT).
About Lutathera
Lutathera is a targeted radioactive therapy. It is used to treat neuroendocrine tumors. It can help make the tumors grow more slowly or stop them from growing. It can also help manage symptoms caused by the tumors.
Lutathera has 2 main parts:
- The tumor-targeted part helps the medicine fight only the tumor cells, not your healthy cells. This helps keep the medicine from harming healthy parts of your body.
- The radioactive part uses radiation (waves of energy) to harm and kill the tumor cells.
You’ll get Lutathera as an intravenous (IV) infusion. This is when medicine is put into your bloodstream through a vein over time.
Getting ready for your Lutathera treatment
Before you get Lutathera, you’ll meet with a healthcare provider from the Molecular Imaging and Therapy Service (MITS). MITS is sometimes called the Nuclear Medicine service. You can meet with them in person or have a telemedicine visit.
You may need to have a blood test before your appointment. If you do, a MITS staff member will give you more information.
During your appointment, your MITS provider will review your medical history and ask you about your medicines. Tell them every medicine you’re taking. This includes patches, creams, prescription medicine, and over-the-counter (not prescription) medicine. You may need to stop taking some of them before your treatment.
The MITS provider will also talk with you about the goals of Lutathera treatment. They’ll use your medical history and the results of the blood test to see if Lutathera is right for you. If it is, they’ll go over the side effects with you and tell you what to expect. They will also give you information about your Lutathera treatment schedule.
Lutathera treatment schedule
The timeline below shows your Lutathera treatment schedule.
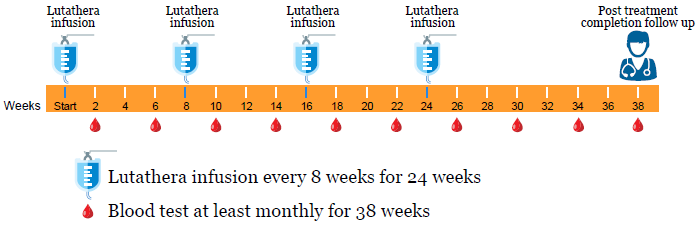
You’ll get Lutathera as 4 separate infusions. The infusions are 8 weeks apart. You’ll come to the main hospital at MSK for each infusion.
You’ll have regular blood tests between treatments and for 2 months after your last infusion. This is to make sure that your blood cell counts stay at their usual levels during your treatment. Your blood cell count is the amounts of the different types of cells in your blood. You can have these blood tests done at the MSK location closest to you.
Octreotide injections during Lutathera treatment
You may be getting octreotide injections (shots) as part of your cancer treatment. If you get octreotide too close before your Lutathera infusion, the treatment may not work as well. Your healthcare provider will give you more information.
Long-acting octreotide
If you take long-acting octreotide, don’t take it for 4 weeks before each Lutathera infusion. Your medical oncologist (cancer doctor) will give you an injection of long-acting octreotide after each infusion.
Short-acting octreotide
If you take short-acting octreotide (also called immediate-release octreotide), you can keep taking it during your Lutathera treatment. Do not use short-acting octreotide for 24 hours before each Lutathera infusion unless your healthcare provider gives you other instructions.
About your Lutathera infusion visits
The timeline below shows what to expect during each Lutathera infusion visit.
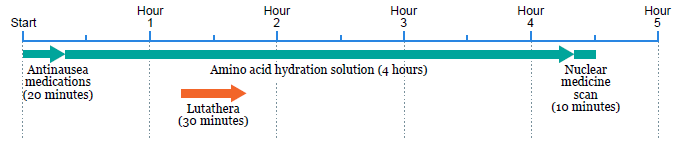
Your infusion visits will take most of the day. Please do not schedule other appointments on treatment days.
You’ll arrive in the morning and be done by mid to late afternoon. You may want to bring a book, laptop, or other things to keep yourself busy during your appointment. You can also bring food and a drink. Bring your appointment calendar with you to each treatment to schedule your next cycle and future lab appointments.
Where to go
Schwartz Cancer Research Building
1250 First Avenue (between East 67th and 68th Streets)
New York, NY 10065
Your Lutathera infusion visits will be in the MITS therapy suite. To get to the suite:
- Enter the hospital through the entrance at 1250 First Avenue.
- Turn left at the security desk in the lobby. If you have questions or need an elevator instead of the stairs, ask the security guard for help.
- Go up the stairs to check in at the reception desk at the top of the stairs. You can wait in the waiting area.
What to expect when you arrive
Many staff members will ask you to say and spell your name and birth date. This is for your safety. People with the same or similar names may be having treatment on the same day.
When it’s time for your appointment, a staff member will bring you to the MITS therapy suite. You’ll sit in a private room with a TV and WiFi.
Before your infusion, a nurse will measure your vital signs (pulse, temperature, breathing, and blood pressure). They will also place 2 IV lines in your veins.
Some people have a central venous catheter (CVC). This can be one of the following:
- An implanted port (Mediport®).
- A tunneled chest catheter.
- A peripherally inserted central catheter (PICC).
If you have a CVC, the nurse will place an IV line into it. They will place the other IV line into a vein in your arm or hand.
If you do not have a CVC, they will place an IV line into each of your arms or hands.
Medicine you’ll get
You’ll get a few different medicines during your infusion visits.
First, you’ll get anti-nausea medicine. This is medicine to keep you from vomiting (throwing up) or feeling nauseous (like you’re going to throw up).
Then, the nurse will connect an amino acid hydration solution to one of your IV lines. This is a medicine to protect your kidneys from the Lutathera. You’ll get this infused (put into your bloodstream) slowly, over 4 hours.
About 30 minutes after the amino acid infusion starts, your MITS provider will connect Lutathera to your other IV line. It will be infused over 45 minutes.
You will get a small dose of dexamethasone 1 hour after your Lutathera infusion ends.
Side effects
During and after the medicine infusions, you may have the following side effects:
- Hair thinning.
- Nausea.
- Vomiting.
- Pain or discomfort in your abdomen (belly).
A nurse will stay with you during your entire treatment to help with these symptoms if they happen.
Visitors can come with you to your Lutathera appointment. They must leave the room once the infusion is ready to begin. They can wait in the waiting room downstairs or leave the hospital. They can come back once your appointment is over.
Nuclear medicine scan
After the amino acid infusion, you’ll have a nuclear medicine scan. This is done to check where the Lutathera went in your body. You will lie down during the scan. The scan will take about 10 minutes.
Your Lutathera infusion visit and scan will take about 6 hours.
Radiation safety measures
After your Lutathera infusion, there will be radiation coming from your body. Before you leave your injection appointment, you’ll meet with a radiation safety staff member. They will talk with you about your radiation safety measures. They will also give you written instructions to follow at home.
To keep from exposing others to radiation, follow the radiation safety instructions below. You must follow these precautions for 2 to 11 days. This will depend on your specific Lutathera treatment.
- Avoid being in close physical contact with other people for a long period of time. You should stay at least 3 feet (about an arm’s length) away from other people most of the time. It’s OK to hug or be in close contact with another person for a short period of time.
- Do not use public transportation, such as a bus or train, right after your infusion appointment. If you do need to take public transportation soon after treatment, contact radiation safety for more details. It’s OK to use a car service.
- If you’re driving with another person in the car, sit as far away from them as you can. You should also do this if you’re using a car service.
- Practice good hygiene, such as washing your hands well with soap and water after using the bathroom. The radioactive material will leave your body through your body fluids in the weeks following your treatment. This includes blood and urine (pee).
In general, you must:
- Stay at least 3 feet away from others the first few days after treatment.
- Sleep alone for 6 days.
- Avoid holding or sleeping next to small children or pregnant people for 10 to 11 days.
Some security equipment, such as at the airport or outside a tunnel, can detect very small amounts of radiation. You will get a card that says you got radioactive medicine. It says you can give off small amounts of radioactivity for up to 2 months after your treatment. Show this card to law enforcement if they stop you at a checkpoint.
If you have any questions about radiation safety, call 212-639-7391 Monday through Friday from to
After your Lutathera infusion visits
There may still be traces of the radiation in your body a month after a Luthatera infusion. Follow the radiation safety instructions. It’s very important to follow these instructions in the bathroom to clean or flush bodily fluids, such as urine.
Drink lots of liquids after each infusion. This will help the radiation leave your body more quickly.
Tell a medical provider or staff member that you were treated with radioactive Lutetium -177 if:
- You need to give blood, urine, or stool (poop) samples during the first 10 days after a Lutathera infusion. The samples you give might be slightly radioactive.
- If you need medical care during the first month after a Lutathera injection. This includes needing an operation or hospital stay.
The medical provider or staff member should take universal precautions. They do not need to take any extra safety measures.
Octreotide injection
If you take long-acting octreotide injections, your medical oncologist will give you a long-acting octreotide injection after each infusion appointment.
Follow these safety measures during your Lutathera treatment, from your first infusion until 6 months after your last infusion.

- Always use birth control during sexual activity.
- Do not get pregnant.
- Do not get a person pregnant.
- Do not breastfeed.
Talk with your MITS healthcare provider if you have any questions.
When to call your care team
Watch the insertion sites for 48 hours (2 days) after your infusion. Your infusion sites are where the IV lines went into your body.
Call your care team if you notice any changes in the area, such as:
- Pain or a burning feeling.
- Redness or other skin color changes.
- Swelling.
- Broken skin.
- Blisters or liquid draining.
- Numbness, tingling, or other changes in sensation (feeling).
- Warm or hot skin.
Contact information
If you have any questions or concerns, please call the Molecular Imaging and Therapy Service.
- Monday through Friday from 9 a.m. to 5 p.m., call 212-639-3146. Ask for the Molecular Imaging and Therapy Service nurse.
- After 5 p.m., during the weekend, and on holidays, call 212-639-2000. Ask for the Molecular Imaging and Therapy Service fellow on call.
Learn about our Health Information Policy.