This information will help you get ready for your uterine fibroid embolization (EM-boh-lih-ZAY-shun). It will also help you understand what to expect after your procedure.
About uterine fibroids
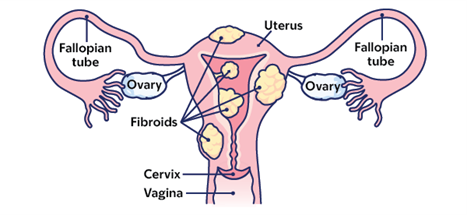
Fibroids are benign (not cancer) tumors. They are muscular and fibrous tissue that grow from the smooth muscle cells of the uterus. Fibroids can be microscopic (very small) in size or grow as large as a cantaloupe. It is rare for them to become cancerous. Some people with fibroids have no symptoms. Others can experience symptoms such as:
- Bleeding a lot from the vagina.
- Pain or pressure on the bladder and bowel.
- Enlarged (very big) abdomen (belly).
- Loss of fertility (your ability to have biological children).
Most often, fibroids that do not cause symptoms do not require treatment.
Facts about fibroids
- Fibroids are most common in people ages 30 to 50.
- One in every 4 people will get fibroids during their reproductive (childbearing) years.
- Black people are 2 to 3 times as likely to have fibroids than white, Asian, or Hispanic people.
What is a uterine fibroid embolization (UFE)?
Uterine fibroid embolization (UFE) is a procedure to block the arteries (blood vessels) of the uterine fibroids. Blocking the arteries to the fibroids stops the flow of blood to them. This makes them shrink.
UFE may be a way to treat fibroids instead of:
- A hysterectomy (HIS-the-REK-toh-mee), which is a surgery to remove the uterus.
- A myomectomy (MY-ohm-EK-toh-mee), which is a surgery to remove each fibroid.
You should not have this procedure if you’re pregnant. Doctors are still studying how UFE may affect the ability to get pregnant. Some people have had healthy pregnancies after this procedure. If having children in the future is important to you, talk with your healthcare provider before deciding on treatment.
Are there any risks to having a uterine fibroid embolization (UFE)?
All medical procedures could have risks. Your doctor will talk with you about the risks of a UFE and answer any questions you have.
Here are some of the signs we watch for after a UFE:
-
Pain and mild fever
- Some people may have pain, cramping, or a low fever (less than 100.4 °F) for a few days after UFE. This is called post embolization syndrome. It’s common. We treat this with pain medicine and medicines that reduce swelling and inflammation.
-
Periods may stop earlier than expected
- Some people have amenorrhea, which means they stop having their monthly period. This is not common in people younger than 35. It often does not cause menopause symptoms, such as hot flashes.
-
Infection of the uterus lining
- In rare cases, the lining of the uterus can get infected. This is called endometritis, which most often responds well to antibiotics.
About your uterine fibroid embolization (UFE)
An interventional (IN-ter-VEN-shun-al) radiologist (also called an IR doctor) will do your UFE. An IR doctor has special training in using image-guided procedures to diagnose and treat disease. Imaging includes X-rays, sonography, ultrasound (US) magnetic resonance imaging (MRI), and computed tomography (CT).
You’ll meet with the IR doctor who will do your UFE. They’ll explain the procedure to you and answer your questions. You’ll be asked to sign a consent form, which says you agree to the procedure and understand the risks.
Your IR doctor will thread a catheter into the small arteries of the fibroids. They’ll use X-rays to guide the catheter to the right place. Then, they’ll inject (put) very small particles through the catheter into your arteries. The particles will block the blood flow to the fibroids and make them shrink.
Your procedure will be done with a local anesthetic (medicine that numbs an area of your body). You’ll also get intravenous (IV) pain and sedation (seh-DAY-shun) medicine that will keep you comfortable during the procedure.
You’ll go home the same day as your procedure.
What to do before your uterine fibroid embolization (UFE)
Ask about your medicines
You may need to stop taking some of your usual medicines before your procedure. Or, you may need to take a different dose (amount) than usual. Talk with your healthcare provider about how to take your medicines before your procedure. Do not change how you take your medicines without talking with a healthcare provider.
This section lists some examples of medicines, but there are many others. Make sure your care team knows all the prescription medicines, over-the-counter medicines, and dietary supplements you take. A prescription medicine is one you can only get with a prescription from a healthcare provider. An over-the-counter medicine is one you can buy without a prescription.
It’s very important to take your medicines and supplements the right way in the days before your procedure. If you don’t, we may need to reschedule your procedure.
Anticoagulants (blood thinners)
A blood thinner is a medicine that changes how your blood clots. Blood thinners are often prescribed to help prevent a heart attack, stroke, or other problems caused by blood clots.
If you take a blood thinner, ask your healthcare provider what to do before your procedure. They may tell you to stop taking it a certain number of days before your procedure. This will depend on the type of procedure you’re having and the reason you’re taking a blood thinner.
Here are some examples of blood thinners. There are others, so be sure your care team knows all the medicines you take. Do not stop taking your blood thinner without talking with a member of your care team.
|
|
Other medicines and supplements can change how your blood clots. Examples include vitamin E, fish oil, and nonsteroidal anti-inflammatory drugs (NSAIDs). Read How To Check if a Medicine or Supplement Has Aspirin, Other NSAIDs, Vitamin E, or Fish Oil. It will help you know which medicines and supplements you may need to avoid before your procedure.
Diabetes medicines
If you take insulin or other diabetes medicines, talk with your MSK healthcare provider and the healthcare provider who prescribes it. Ask them what to do before your surgery or procedure. You may need to stop taking it or take a different dose (amount) than usual. You may also need to follow different eating and drinking instructions before your surgery or procedure. Follow your healthcare provider’s instructions.
Your care team will check your blood sugar levels during your surgery or procedure.
GLP-1 medicines for weight loss
It’s important to tell your healthcare provider if you take a GLP-1 medicine. You will need to follow special eating and drinking instructions before your surgery or procedure. It is very important to follow these instructions. If you do not follow them, your surgery or procedure may be delayed or canceled.
- Follow a clear liquid diet the day before your surgery or procedure. Do not eat any solid food. Read Clear Liquid Diet to learn more.
- Stop drinking 8 hours before your arrival time. Do not eat or drink anything after this time, including clear liquids. You can have small sips of water with your medicines.
To learn more, read Eating and Drinking Before Your Surgery or Procedure When Taking GLP-1 Medicines.
Here are some examples of GLP-1 medicines. There are others, so be sure your care team knows all the medicines you take. Sometimes, these are prescribed to help manage diabetes or other conditions. Other times, they are prescribed for weight loss.
|
|
Diuretics (water pills)
A diuretic is a medicine that helps control fluid buildup in your body. Diuretics are often prescribed to help treat hypertension (high blood pressure) or edema (swelling). They can also be prescribed to help treat certain heart or kidney problems.
If you take a diuretic, ask the healthcare provider doing your procedure what to do before your procedure. You may need to stop taking it the day of your procedure.
We’ve listed some examples of common diuretics below. There are others, so be sure your care team knows all the medicines you take.
|
|
Take devices off your skin
You may wear certain devices on your skin. Before your procedure, surgery, or scan, some device makers recommend you take off your:
- Continuous glucose monitor (CGM)
- Insulin pump
Talk with your healthcare provider about scheduling your appointment closer to the date you need to change your device. Make sure to bring an extra device with you to put on after your procedure, surgery, or scan.
You may not be sure how to manage your glucose (blood sugar) while your device is off. If so, before your appointment, talk with the healthcare provider who manages your diabetes care.
Stop taking nonsteroidal anti-inflammatory drugs (NSAIDs)
NSAIDs, such as ibuprofen (Advil® and Motrin®) and naproxen (Aleve®), can cause bleeding. Stop taking them 2 days before your procedure. If your healthcare provider gives you other instructions, follow those instead.
To learn more, read How To Check if a Medicine or Supplement Has Aspirin, Other NSAIDs, Vitamin E, or Fish Oil.
Reactions to contrast dye
Contrast is a special dye that makes it easier for your IR doctor to see differences in your internal organs. Internal organs are the organs inside of your body. This procedure is usually done with contrast.
Some people can have an allergic reaction to contrast. Most reactions are mild, such as hives.
Some people can have very rare but more serious reactions, such as anaphylaxis (A-nuh-fih-LAK-sis). This is a bad allergic reaction that can cause hypotension (a sudden drop in blood pressure) or trouble breathing.
Anaphylaxis is treated with an epinephrine (eh-pih-NEH-frin) autoinjector, commonly known as an EpiPen®. This is an injection (shot) of epinephrine (adrenaline) into a muscle.
Tell your healthcare provider if you have had an allergic reaction to contrast dye in the past. You may need to take medicine before your procedure to help with the allergy.
Arrange for someone to take you home
You must have a responsible care partner take you home after your procedure. A responsible care partner is someone who can help you get home safely. They should be able to contact your care team if they have any concerns. Make sure to plan this before the day of your procedure.
If you don’t have a responsible care partner to take you home, call one of the agencies below. They’ll send someone to go home with you. There’s a charge for this service, and you’ll need to provide transportation. It’s OK to use a taxi or car service, but you still need a responsible care partner with you.
| Agencies in New York | Agencies in New Jersey |
| VNS Health: 888-735-8913 | Caring People: 877-227-4649 |
| Caring People: 877-227-4649 |
Tell us if you’re sick
If you get sick (including having a fever, cold, sore throat, or flu) before your procedure, call your IR doctor. You can reach them Monday through Friday from to
After , during the weekend, and on holidays, call 212-639-2000. Ask for the Interventional Radiology fellow on call.
Note the time of your appointment
A staff member will call you 2 business days before your procedure. If your procedure is scheduled for a Monday, they’ll call you on the Thursday before. They’ll tell you what time to get to the hospital for your procedure. They will also remind you where to go.
If you don’t get a call by noon (12 p.m.) on the business day before your procedure, call 646-677-7001. If you need to cancel your procedure for any reason, call the healthcare provider who scheduled it for you.
What to do the day before your uterine fibroid embolization (UFE)
Instructions for eating
Stop eating at midnight (12 a.m.) the night before your surgery or procedure. This includes hard candy and gum.
Your healthcare provider may have given you different instructions for when to stop eating. If so, follow their instructions. Some people need to fast (not eat) for longer before their surgery or procedure.
Medicine to prevent reaction to contrast dye
Your doctor may have told you to take medicine to prevent an allergic reaction to contrast. If they did, take the first dose 13 hours before your arrival time. Take the second dose 2 hours before your arrival time.
What to do the day of your uterine fibroid embolization (UFE)
Instructions for drinking
Between midnight (12 a.m.) and 2 hours before your arrival time, only drink the liquids on the list below. Do not eat or drink anything else. Stop drinking 2 hours before your arrival time.
- Water.
- Clear apple juice, clear grape juice, or clear cranberry juice.
- Gatorade or Powerade.
-
Black coffee or plain tea. It’s OK to add sugar. Do not add anything else.
- Do not add any amount of any type of milk or creamer. This includes plant-based milks and creamers.
- Do not add flavored syrup.
If you have diabetes, pay attention to the amount of sugar in your drinks. It will be easier to control your blood sugar levels if you include sugar-free, low-sugar, or no added sugar versions of these drinks.
It’s helpful to stay hydrated before surgeries and procedures, so drink if you are thirsty. Do not drink more than you need. You will get intravenous (IV) fluids during your surgery or procedure.
Stop drinking 2 hours before your arrival time. This includes water.
Your healthcare provider may have given you different instructions for when to stop drinking. If so, follow their instructions.
Things to remember
- Follow your healthcare provider’s instructions for taking your medicines the morning of your procedure. It’s OK to take them with a few sips of water.
- If you’re taking pain medicine, take it before your procedure with a few sips of water. You can take acetaminophen (Tylenol®). Do not take any NSAIDs, such as ibuprofen (Advil and Motrin) and naproxen (Aleve).
- Do not put on body cream, lotion, or petroleum jelly (Vaseline®). You can use deodorant and facial moisturizers. Do not wear eye makeup.
- Do not wear any metal objects. Take off all jewelry, including body piercings. The tools used during your procedure can cause burns if they touch metal.
- Leave valuable items at home.
- If you wear contact lenses, wear your eyeglasses instead, if you can. If you do not have eyeglasses, bring a case for your contacts.
- Wear something comfortable and loose-fitting.
What to bring
- A list of all the medicines you take at home, including prescription and over-the-counter medicines, patches, and creams.
- Medicines for breathing problems (such as your inhaler), medicines for chest pain, or both.
- Your cell phone and charger.
- A case for your personal items, if you have any. Eyeglasses or contacts, hearing aids, dentures, prosthetic devices, wigs, and religious articles are examples of personal items.
- Your Health Care Proxy form and other advance directives, if you filled them out.
- Your breathing device for sleep apnea (such as your CPAP machine), if you use one. If you cannot bring it, we will give you one to use while you’re in the hospital.
What to expect when you arrive
Many doctors, nurses, and other staff members will ask you to say and spell your name and date of birth. This is for your safety. People with the same or similar names may be having procedures on the same day.
Once you’re brought to the presurgical area, you’ll get a hospital gown and nonskid socks to wear. You’ll take off your eyeglasses, hearing aids, dentures, prosthetic devices, wig, and religious articles.
Meet with a nurse
You’ll meet with a nurse before your procedure. Tell them the dose of any medicines you took after midnight (12 a.m.) and the time you took them. Make sure to include prescription and over-the-counter medicines, patches, and creams.
Your nurse will place an intravenous (IV) line into a vein in your arm or hand, unless you already have:
- A central venous catheter (CVC) or any other type of central line.
- A peripherally inserted central catheter (PICC).
- An implanted port (also called a mediport or Port-A-Cath).
You’ll be under sedation for your procedure. When you’re under sedation, you’ll get a sedative. This is medicine that makes you sleepy and relaxed during your procedure. A member of your care team will review your medical history with you to get you ready for sedation.
They will:
- Ask you if you’ve had any problems with sedation in the past. This includes nausea (feeling like you’re going to throw up) or pain.
- Talk with you about your comfort and safety during your procedure.
- Talk with you about the kind of sedation you’ll get.
- Answer any questions you may have about sedation.
What to expect during your procedure
When it’s time for your procedure, you’ll be brought into the procedure room and helped onto the table. You’ll lie flat on your back.
A member of your care team may put compression boots on your lower legs. These gently inflate and deflate to help blood flow in your legs. You’ll be attached to equipment to monitor (keep track of) your heart rate, breathing, and blood pressure. You’ll also get oxygen through a thin tube that rests below your nose.
During your procedure
A member of your care team will clean the skin in the area where your IR doctor will be working. This area is called the insertion site. The insertion site will likely be in your groin (the area between your belly and thigh). Sometimes, the insertion site may be in your wrist. A member of your care team will also shave the insertion site, if needed.
You’ll get an injection (shot) of a local anesthetic to numb the insertion site. Then, your IR doctor will put a needle into an artery in the numbed area. They’ll thread a catheter through the needle into the artery.
Your IR doctor will guide the catheter until it reaches the smaller arteries that supply blood to the fibroids. They’ll use live X-ray pictures and contrast injections to guide the catheter to the right place. The contrast dye will help them in the pictures of the blood vessels that go to the fibroids. This is called an arteriogram (ar-TEER-ee-oh-gram).
Once the catheter is in the right place, your IR doctor will start the embolization. They’ll inject an embolic (blocking) agent into the catheter. These are tiny particles, each the size of a grain of sand.
The particles will move through the catheter into the smaller arteries that supply blood to the fibroids. The particles will plug up these arteries, blocking blood, and making the fibroids shrink. Blood will keep flowing in the other parts of your uterus.
Your IR doctor will take out the catheter after the procedure. They’ll use a small closure device to stop any bleeding from the insertion site. Then, a member of your care team will clean the insertion site. They’ll cover it with a small dressing (bandage), such as a Band-Aid®.
This procedure takes about 1 hour.
What to expect after your procedure
After your procedure, you’ll be brought to the Post-Anesthesia Care Unit (PACU). While you’re in the PACU, your nurse will monitor the insertion site for any bleeding. Tell your nurse if your dressing feels wet or warm.
Your nurse will also monitor how you’re feeling after your procedure. If you have pain, they’ll give you pain medicine through your IV. Most people have severe (very bad) cramping 6 to 12 hours after the procedure.
You’ll be in the PACU for 1 to 4 hours before you’re discharged home with your responsible care partner. You must urinate (pee) before you leave.
Your IR doctor will send prescriptions to your pharmacy. The prescriptions will be for:
- Pain medicine
- Antinausea medicine (medicine to keep you from feeling like you’re going to throw up).
- Anti-inflammatory medicine (medicine that reduces pain, fever, and swelling)
Take the pain medicine as prescribed when you’re at home. The pain often gets better the first few days after the procedure. Within 4 or 5 days, most people only need to take pain medicine 1 to 2 times a day.
Most people feel back to normal 1 to 2 weeks after their procedure.
You’ll have a follow-up appointment with your IR doctor about 2 weeks after your procedure.
What to do at home after your uterine fibroid embolization (UFE)
- You can take off your dressing (bandage) the day after your procedure.
- Do not shower or bathe for the first 24 hours (1 day) after your procedure. You can shower or bathe like you normally do after that.
- Do not lift anything heavier than 10 pounds (4.5 kilograms) for 3 days after your procedure.
- Do not exercise for 2 weeks after your procedure.
-
Do not work for 1 week after your procedure if you lift heavy objects or do heavy physical activity at your job.
- For some jobs, you can go back to work the day after your procedure. This is OK if you sit at a desk or don’t do a lot of physical activity at work.
- Follow your IR doctor’s instructions when taking your medicines.
- You may notice some blood in your urine (pee) for a few days after your procedure. This is normal and will go away with time.
When to call your healthcare provider
Call your healthcare provider if you have:
- A fever of 100.4° F (38° C) or higher.
- Pain, nausea (feeling like you’re going to throw up), or vomiting (throwing up) that will not stop.
- Pain, nausea, or vomiting that’s worse than it was before your procedure.
- Redness, swelling, or bleeding around the insertion site.
- Any symptoms that are worrying you.
Learn about our Health Information Policy.