The surgical procedure your treatment team recommends for you will depend in part on how advanced the testicular cancer is. This is called the cancer’s stage.
Surgery is the first step in most treatment plans and is the treatment for early-stage testicular cancer. MSK surgeons do more than 200 testicular procedures each year.
Surgery may be the only treatment you need for early-stage germ cell tumors that have not spread beyond the testicle. After surgery, you will have long-term surveillance (monitoring) for years.
Retroperitoneal Lymph Node Dissection
Retroperitoneal (REH-troh-PAYR-ih-toh-NEE-ul) lymph node dissection (RPLND) is a treatment for cancer.
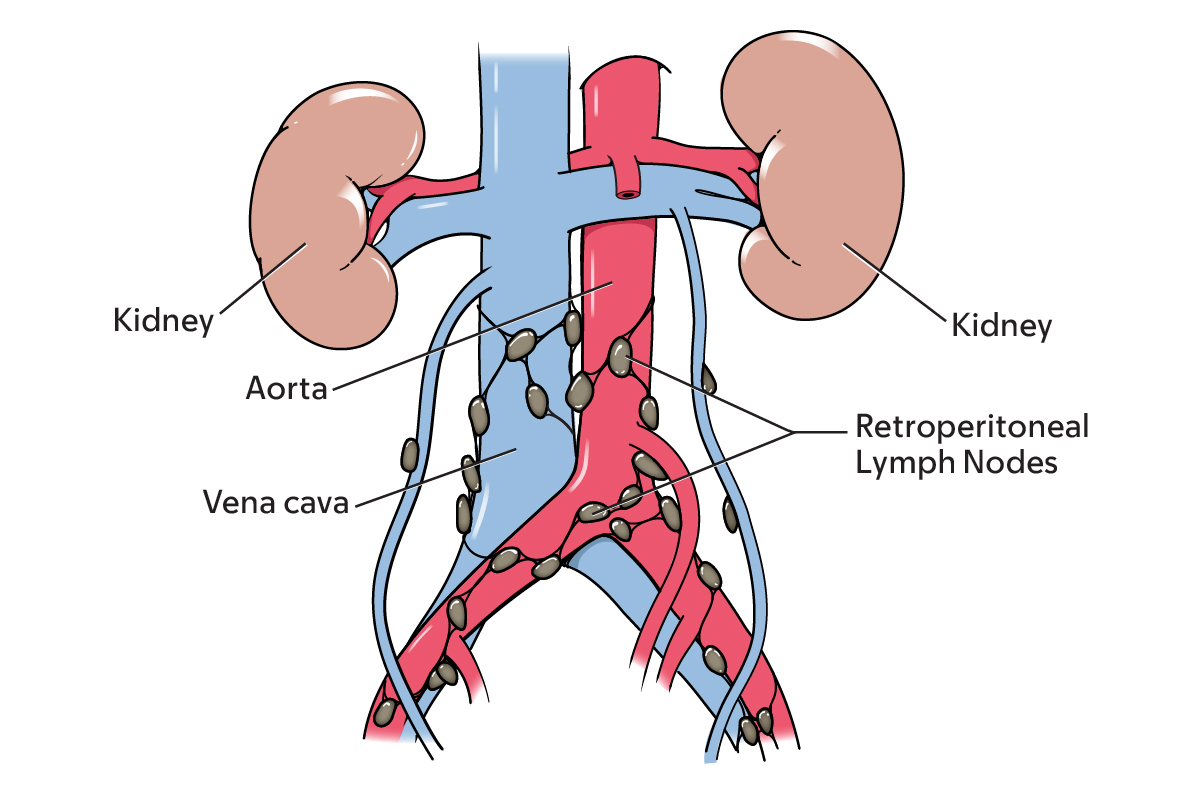
This surgery is done when a tumor is likely to spread, or already spread, to the lymph nodes in your abdomen. It removes the affected lymph nodes.
Your retroperitoneal lymph nodes are found in areas near your kidneys.
MSK has among the most experienced surgeons in the world for RPLND surgery for both nonseminoma and seminoma. RPLND can cure testicular cancer in about 8 or 9 out of every people who have this surgery.
RPLND removes the retroperitoneal lymph nodes. They’re often the first place testicular cancer spreads to. A RPLND surgery helps us learn if the cancer has spread to the lymph nodes.
Your surgeon will try to use methods that do not harm your nerves, if possible. This can prevent retrograde ejaculation, when semen flows back into your bladder instead of out through your penis. However, it can still take between 1 month and several years before your nerves recover.
We strongly recommend that you bank your sperm before your surgery. Your doctor and nurse will talk with you about sperm banking.
Your surgeon will make an incision (surgical cut) in your abdomen (belly) and will remove your lymph nodes through the incision. Your surgery will take 3.5 to 5 hours.
Some people may need RPLND after chemotherapy to remove lymph nodes that are still enlarged (big). This is called a post-chemotherapy RPLND.
We’re available 24 hours a day, 7 days a week