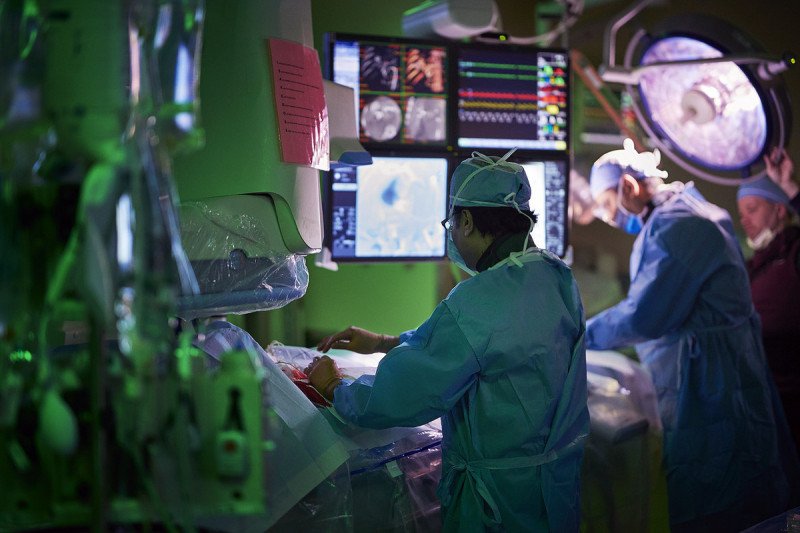
Interventional radiology for cancer involves the use of medical imaging to see inside the body coupled with minimally invasive techniques to diagnose and treat cancer, as well as provide relief from symptoms. Our doctors use tools such as catheters and needles to address a large variety of medical conditions that would have required surgery in the past.
At Memorial Sloan Kettering, we use interventional radiology (IR) techniques to deliver cancer-killing radioactive particles, chemotherapy, heat, cold, or even electric fields directly to tumors. Imaging techniques including CT, ultrasound, PET, and MRI help guide these procedures so your doctor can pinpoint the exact area of treatment, minimizing the effect on normal surrounding tissue.
Image-guided procedures have fewer risks for our patients and allow them to recover more quickly compared with surgery. In fact, the majority of patients who have an IR procedure are able to return home the same day. Also, IR procedures don’t require incisions and often can be done with conscious sedation, which means that you don’t have to undergo general anesthesia.
The most common diseases we treat with image-guided techniques include cancers of the lung, liver, kidney, and bone. But this is a growing field, and we are exploring its use in treating a variety of other cancer types.
Why Interventional Radiology Is Used
Image-guided techniques can be used as the primary treatment to destroy tumors, to prevent bleeding during surgery, or to relieve pain caused by cancer or its treatment. Sometimes we recommend IR procedures when someone is not well enough to have surgery.
In addition, our interventional radiologists may use these techniques to diagnose cancer (by performing image-guided biopsy), to drain infections and abnormal collections of fluid in the chest and abdomen, or to place devices such as chest ports so that patients who must receive regular infusions of chemotherapy drugs can have them delivered directly into the bloodstream.
Types of Interventional Radiology Procedures
Our interventional radiologists use a variety of techniques to treat cancer. These include ablation (burning or freezing a tumor), embolization (cutting off a tumor’s blood supply or targeting it with chemotherapy or radioactivity), and irreversible electroporation (punching holes in tumors with electric currents).
Other IR techniques can relieve pain. For example, vertebroplasty, kyphoplasty, and ablation are three methods we use to help patients with spine and other bony tumors.
This method involves placing a needle into the tumor and delivering heat or cold to destroy the cancer cells. It requires no incisions and is effective for some patients who are not candidates for surgery and who have isolated tumors. Ablation is also used in bones either to relieve pain or sometimes to keep metastases (cancer cells that have spread) under control after resistance to targeted therapies. In addition to destroying tumors, we have been investigating ablation as a method to activate immune cells to attack any remaining cancer cells.
In this technique, microscopic beads are injected into blood vessels that feed the cancer. Sometimes these beads are used to cut off the blood supply to the tumor to suffocate and kill it; other times it is used prior to surgery so tumors can be removed more safely, without significant blood loss. The beads can also be filled with either radioactivity or chemotherapy, depending on the cancer type, and used to shrink or kill the tumor.
What is histotripsy treatment?
Histotripsy (HISS-toh-trip-see) treatment is a noninvasive way to break down cancer tumors using sound waves. Noninvasive (NON-in-VAY-siv) means it’s a procedure that does less harm to your body. This procedure is not surgery. It does not use knives or needles, heat or radiation.
How does histotripsy work to treat cancer tumors?
Histotripsy kills cancerous tumors by focusing ultrasound energy on the tumor cells. The energy creates tiny bubbles that grow fast and pop, breaking the tumor into tiny pieces. Your body then naturally clears away the dead cancer cells. Histotripsy only targets the tumor and a small area of tissue around the tumor. These areas are called margins. Histotripsy does not harm nearby healthy tissue, so it’s safer than some other treatment options.
Which cancers is histotripsy treatment used for?
Histotripsy is mainly used to treat liver cancers, such as hepatocellular carcinoma, cholangiocarcinoma, and metastasis. Metastasis happens when cancer cells travel to the liver from other parts of the body. Histotripsy is often used to treat cancer that spreads to the liver from the colon, breast, or pancreas.
Histotripsy may be a good option for people that cannot have surgery. It is used for tumors that are hard to remove with surgery or ablation. Ablation is a treatment that kills cancerous tumors using heat, cold, or other energy. These tumors are in areas of the liver where surgery or other treatment may be risky. Histotripsy can also be an option for people who want a treatment with fewer side effects.
Researchers are studying whether histotripsy is an option to treat other types of cancer, such as kidney and pancreatic cancers.
Histotripsy side effects and recovery
Histotripsy has very few side effects. It’s a cancer treatment that’s gentler on your body.
Since histotripsy does not use heat or radiation, it’s less likely to harm healthy tissue around the tumor. Most people have little or no pain after treatment. They can get back to their usual activities fast. Recovery time is much shorter than recovery from surgery or ablation.
This is a new strategy we are currently studying that uses tiny needles to give cancer cells a jolt of electricity. The electricity produces holes in the cell membranes that destroy the cells, all without causing scarring or inflammation in nearby healthy tissues. IRE can be useful for treating tumors that are close to blood vessels and other sensitive structures — situations in which thermal ablation isn’t feasible.
Vertebral fractures are a common and painful side effect of spine tumors. During vertebroplasty, a special type of bone cement is injected directly into a collapsed vertebra to stabilize the spine before surgery or radiation therapy. The cement may also serve as a marker in patients who are treated with image-guided radiation therapy. Kyphoplasty provides spinal support and relieves pain, particularly in patients with spine tumors. A small balloon is inserted into the vertebra and inflated. This creates a space into which bone cement can be injected. Both of these procedures can also help improve patients’ mobility.
