Note: This story was originally published in 2022 and has been updated.
Saad Usmani, MD, a hematologic oncologist specializing in multiple myeloma, is Chief of the Myeloma Service at Memorial Sloan Kettering Cancer Center (MSK). Dr. Usmani has more than 15 years of experience specializing in the care of patients with multiple myeloma and other disorders affecting plasma cells.
Here Dr. Usmani discusses the current outlook for the disease and his vision for developing new treatment approaches at MSK that will improve multiple myeloma prognosis (outcome), as well as the most recent advances in the field. This includes the latest FDA approval of the monoclonal antibody drug daratumumab as part of a combination treatment for people newly diagnosed with the disease.
What is multiple myeloma, and how is it diagnosed?
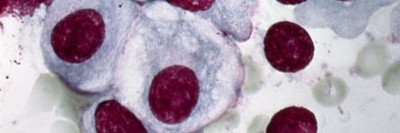
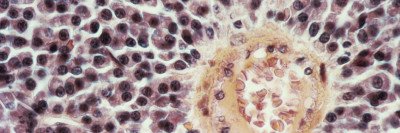
Multiple myeloma arises from a type of white blood cell called a plasma cell. It develops when a normal plasma cell changes into a myeloma cell, which can multiply uncontrollably. Multiple myeloma symptoms include bone pain or fractures, backache, frequent infections, weight loss, fatigue, and other conditions.
We diagnose multiple myeloma by doing blood, urine, bone marrow, and imaging tests. The disease can be classified as being “smoldering myeloma,” which is typically closely monitored, and “active myeloma,” which requires treatment.
Although multiple myeloma is a rare cancer, incidence of the disease is rising as the population ages. In 2026, there will be around 36,000 cases in the United States.
Is multiple myeloma curable?
Multiple myeloma is currently not curable, but we can manage the disease effectively for years. For active myeloma, treatment may include chemotherapy, proteasome inhibitors, immune-modifying drugs or other medications, or stem cell transplantation. Treatments can bring the disease into remission, but it often returns.
What is a typical multiple myeloma prognosis?
As with all cancers, the prognosis for multiple myeloma depends on many factors. These include how well the patient is able to do certain activities of daily living, as well as other health problems they might have. Also important is how much myeloma is present, how far it has spread, and the specific type and subtype.
We have made a great deal of progress in the past two decades, thanks to the development of more effective drugs. The overall five-year survival rate for people with active multiple myeloma in the United States has increased steadily over time, to more than 62% today. It’s important to remember that even the most recent statistics apply to many people who did not have access to the newer treatments. So we expect the survival rate to improve more in the next decade.
What are the newest multiple myeloma drug treatments?
There are several types of new multiple myeloma drugs that have been developed over the past two decades.
Monoclonal antibody drug treatments
- Since 2010, we have seen the emergence of multiple myeloma drugs called monoclonal antibodies. These are man-made proteins that act like antibodies made by the human immune system. The drugs bind to other proteins, called antigens, that are abundant on the surface of myeloma cells.
- The most significant monoclonal antibody has been daratumumab (Darzalex®). The Food and Drug Administration approved daratumumab in 2015, and it changed the practice of myeloma treatment. I had the privilege of leading several trials in the clinical development of daratumumab.
- Daratumumab has been added to standard-of-care drug combinations to make the treatment more effective. Since 2019, the FDA has made multiple approvals for daratumumab combined with other drugs for the treatment of people with newly diagnosed multiple myeloma. Most recently, in 2026, the FDA approved the combination of daratumumab added to a standard “triplet” therapy of three other drugs (bortezomib, lenalidomide, and dexamethasone) in people who are newly diagnosed and not receiving a stem cell transplant as their initial treatment. These more-effective therapies are allowing an increasing number of patients to defer a transplant – a complex procedure that requires a long hospital stay.
CAR T cell therapies
- More recently we’ve had the development of CAR T cell therapies, which genetically engineer a patient’s own immune cells. The CAR T cells being investigated have mainly targeted BCMA.
- In 2021, the FDA approved idecabtagene vicleucel (Abecma®), and, in 2022, it approved ciltacabtagene autoleucel (also known as cilta-cel or Carvytki™). Both CAR T therapies target BCMA, and both approvals were for treating adults with relapsed or refractory (hard-to-treat) multiple myeloma.
- Newer trials, including at MSK, are testing CAR T therapy that targets a different protein, called GPRC5D. It’s always important to have more than one antigen to target, especially if the drugs aimed at the first antigen stop working. Our team is also working on combination CAR T treatments that target BCMA and GPRC5D together.
Bispecific antibody drug treatments
- Bispecific antibodies are a relatively new class of drugs in multiple myeloma. One part of the antibody recognizes an antigen on the patient’s own T cells (such as CD3), and the other part of the antibody recognizes an antigen on the myeloma cell (such as BCMA, GPRC5D, or FcHR5).
- In October 2022, the FDA approved the BCMA-directed bispecific antibody teclistamab (Tecvayli™), for people with multiple myeloma in whom previous therapies have not worked. As reported in the The New England Journal of Medicine, teclistamab shrank cancer in 63% of patients in a clinical trial whose cancer had stopped responding or had progressed after at least three previous therapies. In nearly 40% of these patients, the cancer disappeared completely. These are remarkable results.
- In August 2023, the FDA granted accelerated approval to a second BCMA-directed bispecific antibody called elranatamab (Elrexfio™) for people with multiple myeloma in whom previous therapies had not worked. Results from a phase 2 clinical trial published in Nature Medicine showed that elranatamab shrank cancer in 61% of patients whose cancer had stopped responding or had progressed after at least four previous therapies, with the response still evident 15 months later in 71.5% of patients. MSK played a leadership role in the clinical testing of this drug from the very beginning, led by MSK myeloma specialist and cellular therapist Alexander Lesokhin.
- In August 2023, the FDA also granted accelerated approval to a GPRC5D-directed bispecific antibody called talquetamab-tgvs (Talvey™) in people with resistant forms of multiple myeloma. Because GPRC5D is a different target from BCMA, it provides an important new treatment option for people in whom BCMA-directed drugs did not work.
Why are bispecific antibodies such promising treatments for multiple myeloma?
The FDA has approved three bispecific antibodies in the last year, based on very encouraging results in clinical trials. Although some of the CAR T therapies have had similar success, there is a significant difference: For CAR T therapies, we must remove the patient’s own T cells, engineer them to recognize the antigen, and then infuse them back into the body, which can take six or seven weeks.
Bispecific antibodies are a form of off-the-shelf therapy that we can give to patients right away. Even if they are not completely effective, there are situations where we could give these drugs as a “bridge” therapy while they are awaiting CAR T therapy.
Newer trials at MSK and elsewhere are testing bispecific antibodies earlier in the disease process, usually combined with other therapies.
What is your vision for improving treatment for multiple myeloma over the next decade at MSK?
A big focus for us will be what we can do for high-risk patients — those with aggressive disease that relapses very fast. That’s about one-fourth of multiple myeloma patients, and we currently don’t have good treatments for them. For standard-risk patients, we are getting good results, especially with the newer drugs, but we keep on treating them for a long time. We are trying to find out: If someone has a sustained deep response, can we stop treatment?
We also are looking at whether we can intervene with smoldering myeloma and change some of the risk factors by modifying nutrition and altering the microbiome. There is a subset of smoldering myeloma patients who are at high risk for progressing to active myeloma. Do we have to wait until they show symptoms like broken bones or kidney failure, or can we do something to delay that happening? We will be asking those questions in the studies we plan to do here.
MSK also leads one of three national myeloma consortiums (the Alliance Myeloma Committee), so we will be very involved in collaborative trials testing different approaches. This is an exciting time to be a myeloma researcher.
- Multiple myeloma is not currently curable but can be effectively managed for years.
- New drugs developed over the past two decades have significantly improved prognosis.
- Three bispecific antibodies, a form of off-the-shelf immunotherapy, have been recently approved by the FDA.
Dr. Usmani is supported by a career development award from the
Leukemia and Lymphoma Society.