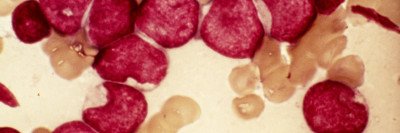
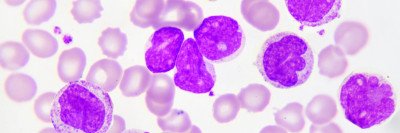
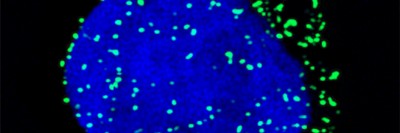
Acute myeloid leukemia (AML), one of the most common leukemias in adults, is diagnosed in about 20,000 people in the United States each year. The average age at diagnosis is 72. The disease affects more men than women.
Our experts can often provide a same-day appointment for patients with newly diagnosed acute myeloid leukemia (AML). Call 646-497-9154 to make an appointment.
Diagnosis of AML
Doctors do a variety of tests to diagnose AML. These tests allow them to analyze the specific features of the leukemia cells and look for any genetic abnormalities, such as rearranged chromosomes or gene mutations. Both of these occurrences are common in AML. Doctors may also look for specific proteins called antigens. These appear on the surface of leukemia cells.
Learn more about the diagnosis of AML.
Treatment for AML
Each person with AML has their own treatment needs. Standard recommendations include chemotherapy and blood or marrow stem cell transplantation. Many people with the form of AML called acute promyelocytic leukemia are first treated with arsenic trioxide (Trisenox®) in combination with all-trans-retinoic acid (ATRA), also called tretinoin (Vesanoid®). The development of both ATRA and arsenic trioxide was pioneered at MSK.
Learn more about treatment for AML.