This guide will help you get ready for your programmable or nonprogrammable ventriculoperitoneal (VP) shunt surgery at MSK. It will also help you know what to expect as you recover.
Use this guide as a source of information in the days leading up to your surgery. Bring it with you on the day of your surgery. You and your care team will use it as you learn more about your recovery.
In this resource, the words “you” and “your” mean you or your child.
About your surgery
A VP shunt is a device used to drain extra cerebrospinal fluid (CSF) from your brain. CSF is the fluid that surrounds your brain and spinal cord. It’s made in the ventricles (hollow spaces) inside your brain.
CSF protects your brain and spinal cord by acting like a cushion. It also brings nutrients throughout your brain and carries waste away.
If extra CSF builds up in your ventricles, it can cause hydrocephalus (HY-droh-SEH-fuh-lus). Hydrocephalus is when extra CSF makes your ventricles grow bigger and puts pressure on your brain and skull (see Figure 1). Hydrocephalus can happen if the flow of CSF is blocked. It also happens if not enough CSF is absorbed into your bloodstream.
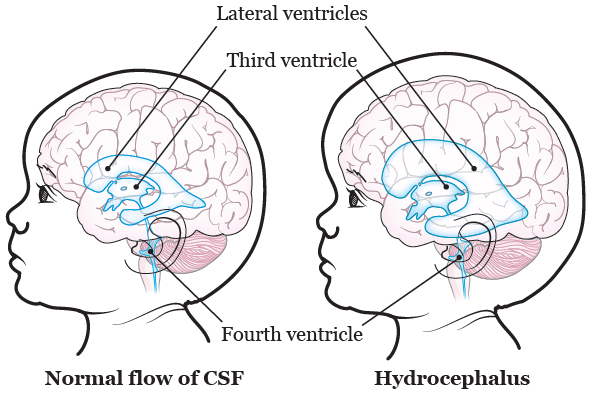
During this surgery, a VP shunt is placed into your head. The shunt drains the fluid out of your brain and moves it into your abdomen (belly). Then it’s absorbed by your body. This lowers the pressure and swelling in your brain.
Symptoms of hydrocephalus
Symptoms are different depending on your age and the stage of disease. The most common symptoms of hydrocephalus include:
- Increased head size and bulging soft spot in baby’s head.
- A headache that does not get better after resting or taking medicine.
- Vomiting (throwing up) with little or no nausea (feeling like you’re going to throw up).
- Fatigue (feeling unusually tired or weak).
- Irritability (becoming easily frustrated or annoyed).
- Personality changes (not acting like your normal self).
- Problems with thinking and memory, such as confusion.
- Trouble with balance or walking.
- Trouble waking up or staying awake.
- Trouble holding in your urine (pee).
- Seizures (uncontrollable shaking).
- High pitched cry in babies.
- Trouble eating.
-
Problems seeing, such as:
- Blurred vision
- Double vision
- Vision loss
- Eyes that turn downward (also called sunsetting)
The VP shunt will relieve your symptoms as it drains the fluid from around your brain. Some symptoms will disappear right away. Others will go away more slowly, sometimes over a few weeks.
About your VP shunt
A VP shunt has 3 parts (see Figure 2):
- A one-way valve and reservoir that controls the flow of fluid.
- A short catheter (thin, flexible tube) that drains the fluid away from your brain. It’s attached to the valve and can be placed in the front, back, or side of your head.
- A long catheter that moves the fluid into your abdomen. It’s attached to the valve and tunneled under your skin, behind your ear, down your neck, and into your abdomen.
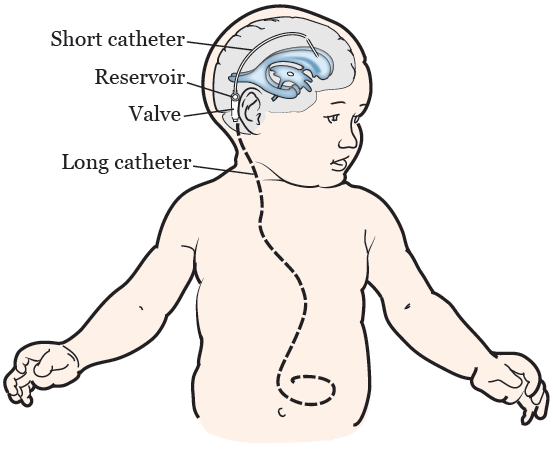
The amount of fluid that’s drained by your VP shunt depends on the settings on the shunt.
- With a nonprogrammable VP shunt, the settings are made by your doctor and cannot be changed.
- With a programmable VP shunt, the settings can be changed by your doctor.
Your neurosurgeon will talk with you about which type of VP shunt is best for you.
What to expect during your surgery
The surgery to place your VP shunt will be done in the operating room. Before your surgery, you will get anesthesia (medication to make you sleep during your surgery). Once you’re asleep, the nurse may need to shave a small amount of hair in the area where your incisions (surgical cuts) will be. Your entire head will not be shaved.
Your neurosurgeon will make small incisions in your head. Sometimes incisions are also made in your neck and abdomen. These incisions will be used to help guide the long catheter so it can be placed correctly.
Your incisions will be closed with sutures (stitches) or staples. You will not be able to see the catheter because it will be under your skin. But you may be able to feel the shunt tubing along your neck.
Once all the parts of the shunt are connected, it will start draining the extra fluid to reduce the pressure in your brain.
Your surgery will take about 1 hour.
Possible problems from surgery
Possible problems from VP shunts and the surgery to place them can include:
- Infection.
- The shunt not working as it should. This can be the shunt draining too much or too little fluid.
- Bleeding.
Your neurosurgeon will explain all the possible risks and problems before your surgery.
Getting ready for your surgery
This section will help you get ready for your surgery. Read it when your surgery is scheduled. Refer to it as your surgery gets closer. It has important information about what to do to get ready.
As you read this section, write down questions to ask your healthcare provider.
Getting ready for your surgery
You and your care team will work together to get ready for your surgery. Help us keep you safe by telling us if any of these things apply to you, even if you’re not sure.
You may need to follow special instructions before surgery based on the medicines and supplements you take. If you do not follow those instructions, your surgery may be delayed or canceled.
-
I take any prescription medicines. A prescription medicine is one you can only get with a prescription from a healthcare provider. Examples include:
- Medicines you swallow.
- Medicines you take as an injection (shot).
- Medicines you inhale (breathe in).
- Medicines you put on your skin as a patch or cream.
- I take any over-the-counter medicines, including patches and creams. An over-the-counter medicine is one you can buy without a prescription.
- I take any dietary supplements, such as herbs, vitamins, minerals, or natural or home remedies.
- I have a pacemaker, automatic implantable cardioverter-defibrillator (AICD), or other heart device.
- I have had a problem with anesthesia (A-nes-THEE-zhuh) in the past. Anesthesia is medicine to make you sleep during a surgery or procedure.
- I’m allergic to certain medicines or materials, including latex.
- I’m not willing to receive a blood transfusion.
- I use recreational drugs, such as marijuana.
Tell your doctor if you have a vagal nerve stimulator (VNS) or a programmable ventriculoperitoneal (VP) shunt.
About drinking alcohol
It’s important to talk with your healthcare providers about how much alcohol you drink. This will help us plan your care.
If you drink alcohol regularly, you may be at risk for problems during and after your surgery. These include bleeding, infections, heart problems, and a longer hospital stay.
If you drink alcohol regularly and stop suddenly, it can cause seizures, delirium, and death. If we know you’re at risk for these problems, we can prescribe medicine to help prevent them.
Here are things you can do before your surgery to keep from having problems.
- Be honest with your healthcare providers about how much alcohol you drink.
-
Try to stop drinking alcohol once your surgery is planned. Tell your healthcare provider right away if you:
- Get a headache.
- Feel nauseous (like you’re going to throw up).
- Feel more anxious (nervous or worried) than usual.
- Cannot sleep.
These are early signs of alcohol withdrawal and can be treated.
- Tell your healthcare provider if you cannot stop drinking.
- Ask your healthcare provider questions about drinking and surgery. All your medical information will be kept private, as always.
About smoking
If you smoke or use an electronic smoking device, you can have breathing problems when you have surgery. Vapes and e-cigarettes are examples of electronic smoking devices. Stopping for even a few days before surgery can help prevent breathing problems during and after surgery.
Your healthcare provider will refer you to our Tobacco Treatment Program if you smoke. You can also reach the program by calling 212-610-0507.
About sleep apnea
Sleep apnea is a common breathing problem. If you have sleep apnea, you stop breathing for short lengths of time while you’re asleep. The most common type is obstructive sleep apnea (OSA). With OSA, your airway becomes fully blocked during sleep.
OSA can cause serious problems during and after surgery. Tell us if you have or think you might have sleep apnea. If you use a breathing device, such as a CPAP machine, bring it on the day of your surgery.
Using MSK MyChart
MSK MyChart (mskmychart.mskcc.org) is MSK’s patient portal. You can use it to send and read messages from your care team, view your test results, see your appointment dates and times, and more. You can also invite your caregiver to make their own account so they can see information about your care.
If you do not have an MSK MyChart account, you can sign up at mskmychart.mskcc.org. You can also ask a member of your care team to send you an invitation.
If you need help with your account, call the MSK MyChart Help Desk at 646-227-2593. They are available Monday through Friday between and (Eastern time).
Help your body get ready for surgery
You can recover faster and easier if you help your body be in its best shape for your surgery. This section has examples of things you can do to get your body ready for surgery. Your care team will help you decide which activities are best for you.
Practice breathing and coughing
Practice taking deep breaths and coughing before your surgery. You can do this by:
- Walking around or playing.
- Blowing bubbles or blowing a tissue in the air.
- Using your incentive spirometer, if your care team gave you one.
Move around and be active
Try to do physical activity every day. Examples include walking, swimming, or biking. MSK also offers free virtual classes for all ages that can help you be active. Ask your healthcare provider for more information.
Practice meditation and mindfulness
Mindful breathing, meditation, yoga, movement practice, massage, and acupressure techniques can support you as you get ready for surgery.
Our Integrative Medicine and Wellness Service videos can help you find the right activities to add to your routines before surgery. Visit www.msk.org/integrative-medicine-multimedia to find the videos. You can also visit www.msk.org/meditation to see guided meditation videos made by our expert mind-body specialists.
Follow a healthy diet
An MSK Kids clinical dietitian nutritionist can talk with you about how to get ready for surgery. You can learn how to make sure your nutrition is the best it can be.
If you’re getting other cancer treatments before your surgery, they can cause taste changes, appetite loss, and trouble digesting food. This can make it hard to eat enough food, which can lead to weight loss. Your outpatient MSK Kids clinical dietitian nutritionist can work with you to make a plan that helps with eating challenges.
It’s also helpful to follow these general guidelines:
- Have small, frequent meals. For example, have a half-sized meal every 2 to 3 hours. Aim for 6 to 8 small meals a day instead of 3 large meals.
- Make and follow a meal schedule. Don’t wait to eat until you’re hungry. Put the schedule in a place for everyone to see.
- Keep your favorite go-to foods in your home where you can get to them easily.
- Buy single-serving food items that you can eat easily, such as drinkable yogurt smoothies or cheese sticks.
-
Cook in batches so you have leftovers.
- Keep 1 extra serving in your refrigerator for the next day, but not longer.
- Freeze the other extra servings. When you’re ready to use a serving, thaw it in the refrigerator or microwave, not on the kitchen counter. Then reheat it until it’s steaming hot.
- Include many different food groups and food types in your diet, unless your doctor or clinical dietitian nutritionist tells you not to.
- Sometimes drinking is easier than eating. Try getting more calories from liquids than solid foods. For example, have milkshakes or nutritional supplements such as PediaSure® or Carnation Breakfast Essentials®.
- Keep your dining experience enjoyable, with no stress. Try having family mealtimes or group snack times with family.
- Think of your nutrition as being just as important as your medicines.
Remember to choose foods that are high in calories and protein. Talk with your MSK Kids clinical dietitian nutritionist about foods that work best based on what you like or your meal patterns.
Fill out a Health Care Proxy form, if needed
If you’re age 18 or older and have not already filled out a Health Care Proxy form, we recommend you do now. If you already filled one out or have any other advance directives, bring them to your next appointment.
A health care proxy is a legal document. It says who will speak for you if you cannot communicate for yourself. This person is called your health care agent.
- To learn about health care proxies and other advance directives, read Advance Care Planning for People With Cancer and Their Loved Ones.
- To learn about being a health care agent, read How to Be a Health Care Agent.
Talk with a member of your care team if you have questions about filling out a Health Care Proxy form.
Within 30 days of your surgery
Presurgical testing (PST)
You’ll have a PST appointment before your surgery. You’ll get a reminder from your surgeon’s office with the appointment date, time, and location. Visit www.msk.org/parking for parking information and directions to all MSK locations.
You can eat and take your usual medicines the day of your PST appointment.
It’s helpful to bring these things to your appointment:
- A list of all the medicines you’re taking, including prescription and over-the-counter medicines, patches, and creams.
- Results of any medical tests done outside of MSK in the past year, if you have them. Examples include results from a cardiac stress test, echocardiogram, or carotid doppler study.
- The names and telephone numbers of your healthcare providers.
You’ll meet with an advance practice provider (APP) during your PST appointment. They work closely with MSK’s anesthesiology (A-nes-THEE-zee-AH-loh-jee) staff. These are doctors with special training in using anesthesia during a surgery or procedure.
Your APP will review your medical and surgical history with you. You may have tests to plan your care, such as:
- An electrocardiogram (EKG) to check your heart rhythm.
- A chest X-ray.
- Blood tests.
Your APP may recommend you see other healthcare providers. They’ll also talk with you about which medicine(s) to take the morning of your surgery.
Visit www.msk.org/parking for parking information and directions to all MSK locations.
Meet with other healthcare professionals, if needed
MSK has many different healthcare professionals who can help you before, during, and after your cancer treatment.
- Social workers can help you cope with the emotional, social, and physical effects of a cancer diagnosis. Our social workers provide counseling and practical assistance. They help families cope with their child’s disease, improve communication with family and friends, share information on community resources, and help adjust to medical treatment.
- Child life specialists are trained professionals who are experts in human growth and development. If you’re worried or stressed about your procedure, they can help you plan ways to be more comfortable and relaxed. MSK’s child life specialists have a variety of backgrounds and interests, including education, psychology, fine arts, and art therapy. Together, our skills and certifications offer a full range of child life services that educate and empower patients and their families during an illness.
- Counselors and therapists can meet with you and your family members and provide counseling for emotional problems related to coping with cancer. MSK’s counseling center also has support groups that meet regularly.
Your healthcare provider may offer you a referral to these services. You can also ask for a referral if you’re interested.
Talk with your social worker about housing, if needed
The Ronald McDonald House provides temporary housing for out-of-town pediatric cancer patients and their families.
MSK also has arrangements with several local hotels and housing facilities that may give you a special lower rate. Your social worker can talk with you about your options and help you make reservations. You can also call 212-639-8315 to talk with the Pediatric Patient Services Coordinator.
Tell us if you’re sick
If you get sick before your surgery, call the healthcare provider who scheduled your surgery. This includes a fever, cold, sore throat, or the flu.
7 days before your surgery
Follow your healthcare provider’s instructions for taking aspirin
Aspirin can cause bleeding. If you take aspirin or a medicine that has aspirin, you may need to change your dose or stop taking it 7 days before your surgery. Follow your healthcare provider’s instructions. Do not stop taking aspirin unless they tell you to.
To learn more, read How To Check if a Medicine or Supplement Has Aspirin, Other NSAIDs, Vitamin E, or Fish Oil.
Stop taking vitamin E, multivitamins, herbal remedies, and other dietary supplements
Vitamin E, multivitamins, herbal remedies, and other dietary supplements can cause bleeding. Stop taking them 7 days before your surgery. If your healthcare provider gives you other instructions, follow those instead.
To learn more, read Herbal Remedies and Cancer Treatment.
Have imaging scans, if needed
You’ll need to have imaging scans to help your healthcare providers plan your surgery. If you have them done somewhere other than MSK, your healthcare provider may ask you to bring the disc with copies of the imaging scans to one of your appointments.
2 days before your surgery
Stop taking nonsteroidal anti-inflammatory drugs (NSAIDs)
NSAIDs, such as ibuprofen (Advil® and Motrin®) and naproxen (Aleve®), can cause bleeding. Stop taking them 2 days before your surgery. If your healthcare provider gives you other instructions, follow those instead.
To learn more, read How To Check if a Medicine or Supplement Has Aspirin, Other NSAIDs, Vitamin E, or Fish Oil.
1 day before your surgery
Note the time of your surgery
A pediatric surgical coordinator will call you after the day before your surgery. If your surgery is scheduled for a Monday, they’ll call you the Friday before. If you do not get a call by , call 212-639-7056.
The surgical coordinator will tell you what time to get to the hospital for your surgery. They’ll also remind you where to go.
Visit www.msk.org/parking for parking information and directions to all MSK locations.
The night before your surgery
Shower
You can shower and wash your hair unless you’re given other instructions, you. Do not apply any hair products such as hair spray or hair gel.
Instructions for eating and drinking before your surgery
Do not eat or drink anything after a certain time on the night before your surgery. This exact time is based on your age and any other medical problems you have. Your healthcare provider will talk with you about what you can and cannot eat before surgery. If you do not follow the instructions your care team gives you, your surgery may be cancelled. |
The morning of your surgery
Do not eat or drink anything the morning of your surgery. This includes water, hard candy, and gum. If you do not follow the instructions your care team gives you, your surgery may be cancelled.
Take your medicines as instructed
A member of your care team will tell you which medicines to take the morning of your surgery. Take only those medicines with a sip of water. Depending on what you usually take, this may be all, some, or none of your usual morning medicines.
Starting 2 hours before your surgery, do not take any medicines.
Things to remember
- Wear something comfortable and loose-fitting.
- If you wear contact lenses, wear your glasses instead. Wearing contact lenses during surgery can damage your eyes.
- Do not wear any metal objects. Remove all jewelry, including body piercings. The tools used during your surgery can cause burns if they touch metal.
- Do not wear any lotion, cream, deodorant, makeup, powder, perfume, or cologne.
- Do not wear any hair products, such as hair spray or hair gel.
- Leave valuable items at home.
What to bring
- Pajamas with a loose-fitting or button-down shirt that will go over your head easily.
- 1 comfort item, such as a blanket or teddy bear.
- 1 or 2 portable electronic devices, such as a smartphone or tablet, and their chargers.
- All the medicines you’re taking, including prescription and over-the-counter medicines, supplements, patches, and creams.
- Your Health Care Proxy form and other advance directives, if you filled them out.
- A case for your personal items, if you have any. Eyeglasses, hearing aids, dentures, prosthetic devices, wigs, and religious articles are examples of personal items.
- This guide. You’ll use it to learn how to care for yourself after surgery.
Once you’re in the hospital
When you get to the hospital, take the B elevator to the 6th floor (the PSC) or the 9th floor (the PACC). Check in at the desk in the waiting room.
Many staff members will ask you to say and spell your name and birth date. This is for your safety. People with the same or a similar name may be having surgery on the same day.
We’ll give you a hospital gown, robe, and nonskid socks to wear when it’s time to change for surgery.
For caregivers, family, and friends
Read Information for Family and Friends for the Day of Surgery to help you know what to expect on the day of your loved one’s surgery.
Meet with a nurse
You’ll meet with a nurse before surgery. Tell them the dose of any medicines you took after midnight (12 a.m.) and the time you took them. Make sure to include prescription and over-the-counter medicines, patches, and creams.
Your nurse may place an intravenous (IV) line in one of your veins, usually in your arm or hand. If your nurse does not place the IV, your anesthesiologist (A-nes-THEE-zee-AH-loh-jist) will do it in the operating room.
Meet with an anesthesiologist
You’ll also meet with an anesthesiologist before surgery. They will:
- Review your medical history with you.
- Ask if you’ve had any problems with anesthesia in the past. This includes nausea (feeling like you’re going to throw up) or pain.
- Talk with you about your comfort and safety during your surgery.
- Talk with you about the kind of anesthesia you’ll get.
- Answer questions you have about anesthesia.
Get ready for surgery
When it’s time for your surgery, you’ll need to take off your eyeglasses, hearing aids, dentures, prosthetic devices, wig, and religious articles.
You’ll either walk into the operating room or a staff member will bring you there on a stretcher. Babies and young children may be carried into the operating room. A member of the operating room team will help you onto the operating bed.
Once you’re comfortable, your anesthesiologist will give you anesthesia and you’ll fall asleep. You’ll also get fluids through your implanted port, CVC, or IV line during and after your surgery.
During your surgery
After you’re fully asleep, your care team will place a breathing tube through your mouth into your airway. It will help you breathe. They’ll also place a urinary (Foley) catheter in your bladder. It will drain your urine (pee) during your surgery.
Your care team will shave a small amount of hair on your head in the area where you’ll be having surgery.
Your surgeon will close your incisions with staples or stitches once they finish your surgery. They’ll cover your incision with a bandage or head wrap.
Your care team will usually take out your breathing tube while you’re still in the operating room.
After your surgery
This section will help you know what to expect after your surgery. You’ll learn how to safely recover from your surgery both in the hospital and at home.
As you read this section, write down questions to ask your healthcare provider.
What to expect
You will be in one of the following units when you wake up after surgery.
- The Pediatric Intensive Care Unit (PICU)
- The Intensive Care Unit (ICU)
- The Post-Anesthesia Care Unit (PACU)
- The Neurology Advanced Care Unit (NACU)
Before your surgery, your care team will talk with you about what to expect when you wake up.
It’s normal to feel very tired after surgery. Your nurse will make sure you are comfortable and answer all of your questions.
A nurse will be keeping track of your temperature, pulse, blood pressure, and oxygen levels. You may get oxygen through a tube resting below your nose or a mask over your nose and mouth. You will also have dressings (bandages) over your incisions.
Parents can call the inpatient unit at any time. Ask your nurse for the phone number. Because of privacy concerns, staff will only give information to parents or spouses. Please tell friends and other relatives not to call the inpatient unit for information.
Pain medicine
Right after your surgery, you will get IV pain medicine through your implanted port, CVC, or IV line. Tell one of your healthcare providers if the medicine isn’t helping your pain.
Tubes and drains
You may have the following tubes and drains. Your healthcare provider will talk with you about what to expect.
- A urinary (Foley) catheter: This is a tube that drains urine from your bladder. Your care team will keep track of how much urine you’re making while you’re in the hospital.
- An IV: You will get fluids and medicines through your IV after surgery.
Physical therapy and occupational therapy
If you need help moving, crawling, walking, playing, or doing self-care tasks after your surgery, a physical therapist (PT), occupational therapist (OT), or both may visit you.
- Your PT can help you move and function better after surgery. They’ll help you get back the strength, balance, and coordination you need to do things like crawling, walking, climbing stairs, playing, or doing sports.
- Your OT can help you improve the skills you need to do important everyday activities. They’ll help you if you have trouble with self-care tasks (such as getting dressed and brushing your teeth), play activities, or skills you need for school or work.
Your PT and OT will talk with you about how often you will have physical therapy, occupational therapy, or both. To learn more, read Staying Active Before and After Surgery for Pediatric Patients.
Moving to your hospital room
You may stay in the PACU for a few hours or overnight. How long you stay depends on the type of surgery you had. A staff member will bring you to your hospital room after your stay in the PACU.
Once you’re fully awake, you will be moved to your hospital room. Your room will be in one of these places:
- The Pediatric Intensive Care Unit (PICU)
- The Adult Intensive Care Unit (ICU)
- The Neurology Advanced Care Unit (NACU)
The place that your room is depends on your age and condition.
In your hospital room
The length of time you’re in the hospital after your surgery depends on your recovery. Most people stay in the hospital for 1 to 3 days.
In your hospital room, you’ll meet one of the nurses who will care for you during your stay. A nurse will help you out of bed and into your chair soon after you get there.
Your care team will teach you how to care for yourself while you’re healing from your surgery.
You will be asked to move your arms, fingers, toes, and legs often. Your nurse will check your pupils with a flashlight and ask questions such as “What is your name?”
Depending on your treatment plan, you may start to work with a physical therapist. Over the next couple of days, you will increase your activity until you’re ready to go home.
Managing your pain
You may have some pain after your surgery. At first, you’ll get your pain medicine through your IV line. Once you’re able to eat, you’ll get oral pain medicine (medicine you swallow).
Your healthcare providers will ask you about your pain often and give you medicine as needed. If your pain is not relieved, tell one of your healthcare providers. It’s important to control your pain so you can use your incentive spirometer and move around. Controlling your pain can help you recover faster.
You’ll get a prescription for pain medicine before you leave the hospital. Talk with your healthcare provider about possible side effects. Ask them when to start switching to over-the-counter pain medicine.
You may have a headache after surgery. You will get medicine to help with these symptoms.
You may have a sore throat after surgery. This is because of the breathing tube you had during surgery. Your nurse will give you cool liquids to drink and lozenges to suck on to help with the discomfort.
Moving around and walking
Moving around and walking will help lower your risk for blood clots and pneumonia (lung infection). It will also help you start passing gas and having bowel movements (pooping) again. Your nurse, physical therapist, or occupational therapist will help you move around, if needed.
Read Frequently Asked Questions About Walking After Your Surgery to learn more about how walking can help you recover.
Read Call! Don't Fall! for Pediatric Patients to learn what you can do to stay safe and keep from falling while you’re in the hospital.
Eating and drinking
Your nurse will give you ice chips after your surgery. You will most likely be able to drink liquids a few hours after your surgery. After that, you will slowly go back to your normal diet.
If you have questions about your diet, ask to see a clinical dietitian nutritionist.
Leaving the hospital
Before you leave, look at your incision with one of your healthcare providers. Knowing what it looks like will help you notice any changes later.
Your healthcare provider will write your discharge order and prescriptions. You’ll also get written discharge instructions. One of your healthcare providers will review them with you before you leave.
At home
Read What You Can Do to Avoid Falling to learn what you can do to keep from falling at home and during your appointments at MSK.
Managing your pain
People have pain or discomfort for different lengths of time. You may still have some pain when you go home and will probably be taking pain medicine. Some people have soreness, tightness, or muscle aches around their incision for 6 months or longer. This does not mean something is wrong.
Follow these guidelines to help manage your pain at home.
- Take your medicine(s) as directed and as needed.
- Call your healthcare provider if the medicine prescribed for you does not help your pain.
- Do not drive or drink alcohol while you’re taking prescription pain medicine. Some prescription pain medicines can make you drowsy (very sleepy). Alcohol can make the drowsiness worse.
-
As your incision heals, you will have less pain and need less pain medicine. An over-the-counter pain reliever will help with aches and discomfort. Acetaminophen (Tylenol®) and ibuprofen (Advil® or Motrin®) are examples of over-the-counter pain relievers. Call your healthcare provider before taking ibuprofen (Advil® or Motrin®).
- Follow your healthcare provider’s instructions for stopping your prescription pain medicine.
- Do not take too much of any medicine. Follow the instructions on the label or from your healthcare provider.
- Read the labels on all the medicines you’re taking. This is very important if you’re taking acetaminophen. Acetaminophen is an ingredient in many over-the-counter and prescription medicines. Taking too much can harm your liver. Do not take more than one medicine that has acetaminophen without talking with a member of your care team.
- Pain medicine should help you get back to your usual activities. Take enough medicine to do your activities and exercises comfortably. It’s normal for your pain to increase a little as you start to be more active.
- Keep track of when you take your pain medicine. It works best 30 to 45 minutes after you take it. Taking it when you first have pain is better than waiting for the pain to get worse.
Some prescription pain medicines, such as opioids, may cause constipation. Constipation is when you poop less often than usual, have a harder time pooping, or both.
Caring for your incision
Your healthcare provider will take your sutures or staples in your incision out during your first appointment after surgery. This is about 7 to 10 days after surgery. They may need to stay in longer if you have had this surgery before.
It’s common for the skin below your incision to feel numb. This happens because some of your nerves were cut during your surgery. The numbness will go away over time.
Check your incision for any signs of redness, swelling, or drainage. Keep them clean and dry for 5 days after your surgery.
Call your healthcare provider’s office if:
- The skin around your incision is very red or getting more red.
- The skin around your incision is warmer than usual.
- The area around your incision is starting to swell or getting more swollen.
- You see drainage that looks like pus (thick and milky).
- Your incision smells bad.
Take off your bandage or head wrap, if you have one
If you have a bandage or head wrap over your incision, your surgeon will take it off 1 to 2 days after your surgery. After that, you can leave the incision uncovered. Once your incision is healed, it does not need to be covered.
Protect your incision from the sun
Protect your incision from the sun by wearing a hat or scarf. You should also wear sunscreen, but make sure your incision is fully healed before you put sunscreen on it.
Do not put anything on your incision
As your incision heals, it may burn, itch, or feel numb. Do not put on any creams, sunscreens, ointments, hair products, or use a hairdryer on your incision until it is completely healed. This may take about 6 weeks.
Showering
You may shower or bathe 24 hours (1 day) after surgery. But do not get your incision(s) wet for the first 5 days after surgery. Wear a shower cap to keep your incision from getting wet. It’s best to shower with someone in the bathroom to help you.
Starting 5 days after your surgery, take a shower and wash your hair every day to clean your incision. This helps loosen up any crusting on your incision. It will also help your healthcare provider remove your staples or sutures. If you have staples or stitches in your incision, it’s OK to get them wet.
When you wash your hair, use a gentle shampoo, such as baby shampoo. You can gently massage the area near your incision to wash off any dried blood or drainage. You can let the shower water run over your incision.
After you shower, pat the area dry with a clean towel.
Do not let your incision soak in water. If you’re taking a bath, do not put your head under water.
Eating and drinking
You can eat all the foods you did before your surgery, unless your healthcare provider gives you other instructions. Eating a balanced diet with lots of calories and protein will help you heal after surgery. Try to eat a good protein source (such as meat, cheese, tofu, fish, or eggs) at each meal. You should also try to eat fruits, vegetables, and whole grains.
It’s also important to drink plenty of liquids. Try to drink 8 to 10 (8-ounce) cups of liquids every day. Choose liquids without alcohol. Limit liquids with caffeine.
If you have questions about your diet, ask to see a clinical dietitian nutritionist.
Physical activity and exercise
Your incision may look like it’s healed on the outside when you leave the hospital. It will not be healed on the inside. For the first 6 weeks after your surgery:
- Do not lift anything heavier than 10 pounds (4.5 kilograms).
- Do not do any high-energy activities, such as jogging and tennis.
Do not play any contact sports, such as football, boxing, or wrestling, until your neurosurgeon says it’s OK. Wear a helmet to protect your head. Talk with your neurosurgeon for more information.
Exercise, such as walking and stair climbing, will help you gain strength and feel better. Try to walk each day. Have someone next to you to make sure you are safe. Start by walking a little more than you did the day before. Slowly increase the amount you walk.
It’s common to have less energy than usual after surgery. Recovery time is different for everyone. Do more activity each day as much as you can. Always balance activity periods with rest periods. Rest is an important part of your recovery.
Driving
Ask your healthcare provider when you can drive. Most people can start driving again 2 weeks after surgery. Do not drive while you’re taking pain medicine that may make you drowsy.
You can ride in a car as a passenger at any time after you leave the hospital.
Going back to work
Talk with your healthcare provider about your job. They’ll tell you when it may be safe for you to start working again based on what you do. If you move around a lot or lift heavy objects, you may need to stay out a little longer. If you sit at a desk, you may be able to go back sooner.
Going back to school
You can go back to school as soon as you feel ready. Tell your school nurse that you have a VP shunt.
Swimming
Do not swim in a pool or hot tub for at least 2 weeks after your surgery. If your incisions need more time to heal, you may need to wait longer. Your healthcare provider will tell you when it’s OK to swim at your first follow-up appointment after your surgery.
Traveling
Do not travel on an airplane until your doctor says it’s OK.
Safety guidelines to follow with a programmable VP shunt
Magnets may affect your VP shunt settings
The pressure setting of some programmable VP shunts may accidentally change if you come too close to a magnet. This depends on the model of your shunt.
Ask your neurosurgeon if you need to take special care when you’re near magnets. Follow the manufacturer’s guidelines about magnetic fields for your shunt.
Here are some general guidelines for VP shunts.
- Keep all electronic devices including laptops, tablets, and smartphones that may contain magnets at least 6 inches (15 centimeters) away from your shunt valve implant site.
- Keep wireless chargers 12 inches (30 centimeters) away from your shunt valve implant site.
- When using your cell phone, hold it to your ear on the side opposite to where your shunt valve is implanted.
- Do not use smartphone cases that have magnetic closures.
- Do not use headphones or ear buds that have magnetic parts. Check with the manufacturer to see if your headphones or earbuds are safe to use.
- Do not use magnetic therapy devices such as magnetic pads and pillows.
- Magnetic toys and refrigerator magnets need to be at least 6 inches (15 centimeters) away from your shunt valve.
- Hearing aids are safe to use with a shunt valve.
Metal detectors with a VP shunt
- Let security at airports and other locations with metal detectors know that you have programmable VP shunt.
- Your VP shunt will not affect airport security screening devices or metal detectors. Walk through the metal detector like usual.
Wear MedicAlert® jewelry
You should always wear a MedicAlert bracelet or necklace that says you have hydrocephalus and a programmable VP shunt. This will help emergency service workers care for you if you’re ever badly ill or hurt and need medical help.
You can buy a MedicAlert bracelet or necklace at most drug stores. You can also ask a member of your care team for an application. Visit the MedicAlert website at www.medicalert.org to learn more.
Magnetic resonance imaging (MRI) and other imaging scans
Before having an MRI:
- Tell the MRI technologist you have a programmable VP shunt before your MRI appointment. They will need to know your shunt’s model and setting. Show them your wallet card.
- Make an appointment with your neurosurgeon to have your shunt reprogrammed within 4 hours after your MRI scan.
- Do not have an MRI scan if you cannot get an appointment to have your shunt reprogrammed after your scan. Wait to have your scan until you can schedule an appointment to have your shunt reprogrammed.
Some programmable VP shunts are affected by MRI scans. Ask your neurosurgeon if your shunt is. If it is, follow the guidelines in this section before having and MRI.
Depending on the model of your programmable VP shunt, the magnet in the MRI scanner may change your shunt’s pressure setting. After your MRI, your shunt’s pressure setting will need to be checked, reprogrammed, or both. You may need to have X-rays to help see if the pressure setting has changed.
You do not need to take any special care if you’re having a computed tomography (CT) scan or X-ray. These scans will not affect your programmable VP shunt.
Tell your doctor if you need abdominal surgery
If you ever need to have abdominal surgery, tell your neurosurgeon. Tell the doctor doing the surgery that you have a programmable VP shunt.
Tell your neurosurgeon if you have peritonitis or diverticulitis. Peritonitis (PAYR-ih-tuh-NY-tis) is swelling in the lining of your abdomen. Diverticulitis (DY-ver-TIH-kyoo-LY-tis) is swelling in the lining of your colon. You may need emergency surgery or antibiotic treatment.
Do not play contact sports
Do not play any contact sports (such as football, boxing, and wrestling) with a nonprogrammable VP shunt. You can do noncontact sports (such as swimming and running).
Wear a helmet, if needed
Wear a helmet to lower your risk of head injury, if needed. Ask your neurosurgeon for specific guidelines on wearing a helmet.
Safety guidelines to follow while you have a nonprogrammable VP shunt
Wear MedicAlert® jewlery
You should always wear a MedicAlert bracelet or necklace that says you have hydrocephalus and a nonprogrammable VP shunt. This will help emergency service workers care for you if you’re ever badly ill or hurt and need medical help.
You can buy a MedicAlert bracelet or necklace at most drug stores. You can also ask a member of your care team for an application. Visit the MedicAlert website at www.medicalert.org to learn more.
Continue with imaging scans
You can have any imaging scan done after your surgery. This includes a magnetic resonance imaging (MRI), computed tomography (CT), or X-ray scan. You do not need to take any special care.
Tell your doctor if you need abdominal surgery
If you ever need to have abdominal surgery, tell your neurosurgeon. Tell the doctor doing the surgery that you have a nonprogrammable VP shunt.
Tell your neurosurgeon if you have peritonitis or diverticulitis. Peritonitis (PAYR-ih-tuh-NY-tis) is swelling in the lining of your abdomen. Diverticulitis (DY-ver-TIH-kyoo-LY-tis) is swelling in the lining of your colon. You may need emergency surgery or antibiotic treatment.
Do not play contact sports
Do not play any contact sports (such as football, boxing, and wrestling) with a nonprogrammable VP shunt. You can play noncontact sports (such as swimming and running).
Wear a helmet, if needed
Wear a helmet to lower your risk of head injury, if needed. Ask your neurosurgeon for specific guidelines on wearing a helmet.
Follow-up care
You will have regular visits with your neurologist, neurosurgeon, or both. They will monitor the function of your VP shunt over time.
Managing your feelings
You may have new and upsetting feelings after a surgery for a serious illness. Many people say they felt weepy, sad, worried, nervous, irritable, or angry at one time or another. You may find that you cannot control some of these feelings. If this happens, it’s a good idea to seek emotional support. Your healthcare provider can refer you to MSK’s Counseling Center. You can also reach them by calling 646-888-0200.
The first step in coping is to talk about how you feel. Family and friends can help. We can also reassure, support, and guide you. It’s always a good idea to let us know how you, your family, and your friends are feeling emotionally. Many resources are available to you and your family. We’re here to help you and your family and friends handle the emotional aspects of your illness. We can help no matter if you’re in the hospital or at home.
When to call your healthcare provider
These warning signs can appear quickly. If your child has any of these signs or symptoms, call their healthcare provider right away.
If you cannot wake your child, call 911 or go to the nearest emergency room right away.
Call your healthcare provider if you have any of the following.
- Increased head size and bulging soft spot in baby’s head.
- A headache that does not get better after resting or taking medicine.
- Vomiting (throwing up) with little or no nausea (feeling like you’re going to throw up).
- Fatigue (feeling unusually tired or weak).
- Irritability (becoming easily frustrated or annoyed).
- Personality changes (not acting like your normal self).
- Problems with thinking and memory (such as confusion).
- Trouble with balance or walking.
- Trouble waking up or staying awake.
- Trouble holding in your urine (pee).
- Seizures (uncontrollable shaking).
- High pitched cry in babies.
- Trouble eating.
- Problems seeing, such as blurred vision or vision loss.
- Eyes that turn downward (also called sunsetting)
-
You have warning signs of a VP shunt infection. These signs include:
- A fever of 100.4 °F (38 °C) or higher.
- Swelling, redness, or both along the shunt tubing from your head to your abdomen.
- Pain around the shunt or around the shunt tubing from the head to your abdomen.
Contact information
If you have questions or concerns, contact your healthcare provider. A member of your care team will answer Monday through Friday from to Outside those hours, you can leave a message or talk with another MSK provider. There is always a doctor or nurse on call.
If you’re not sure how to reach your healthcare provider, call 212-639-2000.
Support services
This section has a list of support services. They may help you as you get ready for your surgery and recover after your surgery.
As you read this section, write down questions to ask your healthcare provider.
MSK support services
Admitting Office
212-639-7606
Call if you have questions about your hospital admission, such as asking for a private room.
Anesthesia
212-639-6840
Call if you have questions about anesthesia.
Blood Donor Room
212-639-7643
Call for information if you’re interested in donating blood or platelets.
Bobst International Center
www.msk.org/international
888-675-7722
We welcome patients from around the world and offer many services to help. If you’re an international patient, call for help arranging your care.
Counseling Center
www.msk.org/counseling
646-888-0200
Many people find that counseling helps them. Our Counseling Center offers counseling for individuals, couples, families, and groups. We can also prescribe medicine to help if you feel anxious or depressed. Ask a member of your care team for a referral or call the number above to make an appointment.
Food Pantry Program
646-888-8055
We give food to people in need during their cancer treatment. Talk with a member of your care team or call the number above to learn more.
Integrative Medicine and Wellness Service
www.msk.org/integrativemedicine
Our Integrative Medicine and Wellness Service offers many services to complement (go along with) traditional medical care. For example, we offer music therapy, mind/body therapies, dance and movement therapy, yoga, and touch therapy. Call 646-449-1010 to make an appointment for these services.
You can also schedule a consultation with a healthcare provider in the Integrative Medicine and Wellness Service. They’ll work with you to make a plan for creating a healthy lifestyle and managing side effects. Call 646-608-8550 to make an appointment for a consultation.
MSK Library
library.mskcc.org
You can visit our library website or email [email protected] to talk with the library reference staff. They can help you find more information about a type of cancer. You can also visit the library’s Patient Education Resource Guide.
Nutrition Services
www.msk.org/nutrition
212-639-7312
Our Nutrition Service offers nutritional counseling with one of our clinical dietitian nutritionists. Your clinical dietitian nutritionist will talk with you about your eating habits. They can also give advice on what to eat during and after treatment. Ask a member of your care team for a referral or call the number above to make an appointment.
Patient and Community Education
www.msk.org/pe
Visit our patient and community education website to search for educational resources, videos, and online programs.
Patient Billing
646-227-3378
Call if you have questions about preauthorization with your insurance company. This is also called preapproval.
Patient Representative Office
212-639-7202
Call if you have questions about the Health Care Proxy form or concerns about your care.
Perioperative Nurse Liaison
212-639-5935
Call if you have questions about MSK releasing any information while you’re having surgery.
Private Duty Nurses and Companions
646-357-9272
You can request private nurses or companions to care for you in the hospital and at home. Call to learn more.
Rehabilitation Services
www.msk.org/rehabilitation
Cancers and cancer treatments can make your body feel weak, stiff, or tight. Some can cause lymphedema (swelling). Our physiatrists (rehabilitation medicine doctors), occupational therapists (OTs), and physical therapists (PTs) can help you get back to your usual activities.
- Rehabilitation medicine doctors diagnose and treat problems that affect how you move and do activities. They can design and help coordinate your rehabilitation therapy program, either at MSK or somewhere closer to home. Call Rehabilitation Medicine (Physiatry) at 646-888-1929 to learn more.
- An OT can help if you’re having trouble doing usual daily activities. For example, they can recommend tools to help make daily tasks easier. A PT can teach you exercises to help build strength and flexibility. Call Rehabilitation Therapy at 646-888-1900 to learn more.
Resources for Life After Cancer (RLAC) Program
646-888-8106
At MSK, care does not end after your treatment. The RLAC Program is for patients and their families who have finished treatment.
This program has many services. We offer seminars, workshops, support groups, and counseling on life after treatment. We can also help with insurance and employment issues.
Social Work
www.msk.org/socialwork
212-639-7020
Social workers help patients, families, and friends deal with common issues for people who have cancer. They provide individual counseling and support groups throughout your treatment. They can help you communicate with children and other family members.
Our social workers can also help refer you to community agencies and programs. If you’re having trouble paying your bills, they also have information about financial resources. Call the number above to learn more.
Spiritual Care
212-639-5982
Our chaplains (spiritual counselors) are available to listen, help support family members, and pray. They can contact community clergy or faith groups, or simply be a comforting companion and a spiritual presence. Anyone can ask for spiritual support. You do not have to have a religious affiliation (connection to a religion).
MSK’s interfaith chapel is located near Memorial Hospital’s main lobby. It’s open 24 hours a day. If you have an emergency, call 212-639-2000. Ask for the chaplain on call.
Virtual Programs
www.msk.org/vp
We offer online education and support for patients and caregivers. These are live sessions where you can talk or just listen. You can learn about your diagnosis, what to expect during treatment, and how to prepare for your cancer care.
Sessions are private, free, and led by experts. Visit our website to learn more about Virtual Programs or to register.
External support services
Access-A-Ride
web.mta.info/nyct/paratran/guide.htm
877-337-2017
In New York City, the MTA offers a shared ride, door-to-door service for people with disabilities who can’t take the public bus or subway.
Air Charity Network
www.aircharitynetwork.org
877-621-7177
Provides travel to treatment centers.
American Cancer Society (ACS)
www.cancer.org
800-ACS-2345 (800-227-2345)
Offers a variety of information and services, including Hope Lodge, a free place for patients and caregivers to stay during cancer treatment.
Cancer and Careers
www.cancerandcareers.org
646-929-8032
A resource for education, tools, and events for employees with cancer.
CancerCare
www.cancercare.org
800-813-4673
275 Seventh Avenue (Between West 25th & 26th Streets)
New York, NY 10001
Provides counseling, support groups, educational workshops, publications, and financial assistance.
Cancer Support Community
www.cancersupportcommunity.org
Provides support and education to people affected by cancer.
Caregiver Action Network
www.caregiveraction.org
800-896-3650
Provides education and support for people who care for loved ones with a chronic illness or disability.
Corporate Angel Network
www.corpangelnetwork.org
866-328-1313
Offers free travel to treatment across the country using empty seats on corporate jets.
Good Days
www.mygooddays.org
877-968-7233
Offers financial assistance to pay for copayments during treatment. Patients must have medical insurance, meet the income criteria, and be prescribed medicine that’s part of the Good Days formulary.
HealthWell Foundation
www.healthwellfoundation.org
800-675-8416
Provides financial assistance to cover copayments, health care premiums, and deductibles for certain medicines and therapies.
Joe’s House
www.joeshouse.org
877-563-7468
Provides a list of places to stay near treatment centers for people with cancer and their families.
LGBT Cancer Project
www.lgbtcancer.com
Provides support and advocacy for the LGBT community, including online support groups and a database of LGBT-friendly clinical trials.
LIVESTRONG Fertility
www.livestrong.org/fertility
855-744-7777
Provides reproductive information and support to cancer patients and survivors whose medical treatments have risks associated with infertility.
Look Good Feel Better Program
www.lookgoodfeelbetter.org
800-395-LOOK (800-395-5665)
This program offers workshops to learn things you can do to help you feel better about your appearance. For more information or to sign up for a workshop, call the number above or visit the program’s website.
National Cancer Institute
www.cancer.gov
800-4-CANCER (800-422-6237)
National LGBT Cancer Network
www.cancer-network.org
Provides education, training, and advocacy for LGBT cancer survivors and those at risk.
Needy Meds
www.needymeds.org
Lists Patient Assistance Programs for brand and generic name medicines.
NYRx
www.health.ny.gov/health_care/medicaid/program/pharmacy.htm
Provides prescription benefits to eligible employees and retirees of public sector employers in New York State.
Patient Access Network (PAN) Foundation
www.panfoundation.org
866-316-7263
Gives help with copayments for patients with insurance.
Patient Advocate Foundation
www.patientadvocate.org
800-532-5274
Provides access to care, financial assistance, insurance assistance, job retention assistance, and access to the national underinsured resource directory.
Professional Prescription Advice
www.pparx.org
888-477-2669
Helps qualifying patients without prescription drug coverage get free or low-cost medicines.
Red Door Community (formerly known as Gilda’s Club)
www.reddoorcommunity.org
212-647-9700
A place where people living with cancer find social and emotional support through networking, workshops, lectures, and social activities.
RxHope
www.rxhope.com
877-267-0517
Provides assistance to help people get medicines they have trouble affording.
Triage Cancer
www.triagecancer.org
Provides legal, medical, and financial information and resources for cancer patients and their caregivers.
Educational resources
This section lists the educational resources mentioned in this guide. They will help you get ready for your surgery and recover after your surgery.
As you read these resources, write down questions to ask your healthcare provider.
