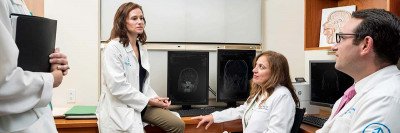
About Your Transsphenoidal Surgery
The main treatment for most pituitary tumor patients is a minimally invasive operation called transsphenoidal surgery.
Memorial Sloan Kettering surgeons are particularly experienced in using this technique, also called transnasal endoscopy, to remove pituitary gland tumors through the nose.
The approach allows MSK surgeons Viviane Tabar and Marc Cohen to bypass brain tissue, operating instead through an incision inside the nasal passage. An endoscope — a thin, lighted tube with a camera at its tip — is inserted through the nasal passage and the sinuses are opened up for a magnified view of the skull base.
Because the view is so clear, your surgeon is better able to remove all of a tumor while preserving normal, healthy tissue. The risk for neurologic complications with this technique is very low, and the surgery leaves no visible scar.
This high-definition approach is effective for small tumors hidden within the pituitary gland as well as for large tumors that extend to critical areas such as the optic nerves, cavernous sinus, and carotid artery.
Nasoseptal Flap
The nasoseptal flap refers to tissue in the nasal septum, the structure between the two airways of the nostrils. Surgeons are able to use this tissue to construct a seal between the brain and the nose after removal of large pituitary gland tumors or other skull base tumors.
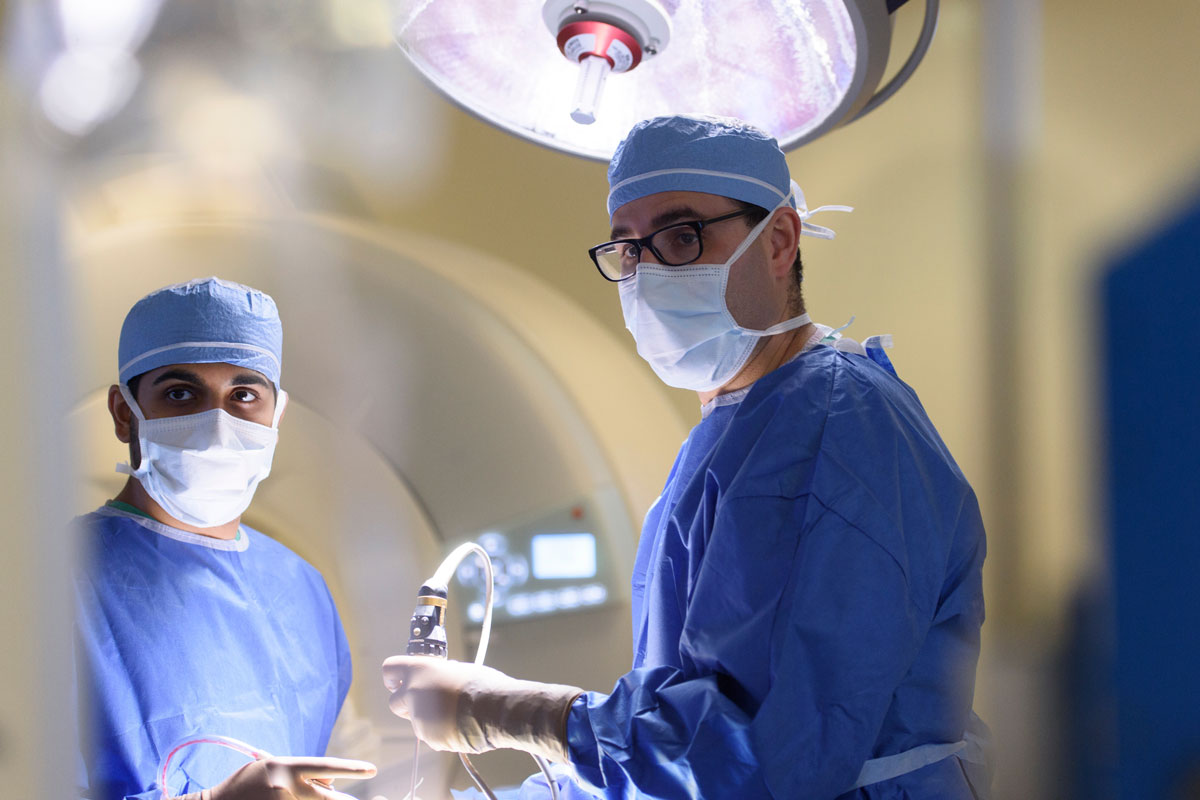
The introduction of this minimally invasive approach in recent years has transformed surgery to remove pituitary tumors and other skull base tumors by providing a safe, reliable way to separate the brain from the nasal cavity and prevent leakage of cerebrospinal fluid. Our surgeons are experienced in using endoscopic approaches to complete the procedure.
The risk for neurological complications is very low, and the technique leaves no visible scar. Recovery can begin right away, because there is little or no need for external incisions to heal. Usually patients are discharged from the hospital after just two or three days.
Intraoperative MRI for Pituitary Tumor Surgery
At Memorial Sloan Kettering, our patients benefit from the use of intraoperative MRI to assist in the removal of pituitary gland tumors.
An MRI is a test that uses strong magnetic fields to produce pictures of the inside of your body. Intraoperative MRI refers to the use of an MRI scanner during surgery.
The pictures produced by an MRI show the difference between normal and diseased tissue. MRI scans do not involve the use of radiation.
Memorial Sloan Kettering is one of just a handful at hospitals around the country to use intraoperative MRI. This advanced technology allows our surgeons to confirm that a tumor has been entirely removed while patients are still under anesthesia.
This enhanced accuracy not only helps to preserve healthy tissue and prevent postoperative complications but also reduces the likelihood that a second surgery will be needed.
Telemedicine Appointments
We know that rest is an important part of the healing process, and that travel to and from appointments can take a lot of time and energy. That’s why, for some neurosurgery visits, you may be able to see your MSK care team through our telemedicine program. If we determine that telemedicine would be appropriate for you, a member of your care team will reach out.
Telemedicine is the use of video technology to connect you with members of your MSK care team. We use secure technology to make sure all of your information stays private. You can communicate through face-to-face video conferencing via a desktop computer, laptop, or tablet device at several MSK locations. We can also use telemedicine while you or a loved one is in the hospital, either to connect you with your provider or to include someone who is not able to visit in person. During your appointment, your provider will be able to check how you’re doing, assess your follow-up needs, and discuss problems you may be having. You will be able to see and hear your MSK specialist, and they will be able to see and hear you — the only difference is that you won’t be in the same room.
A virtual visit saves you time and stress. It may also help prevent an unnecessary trip to an emergency room or urgent care center. In addition, telemedicine can help cut down on missed work days for both patients and caregivers due to travel for appointments.
Monday through Friday, to (Eastern time)