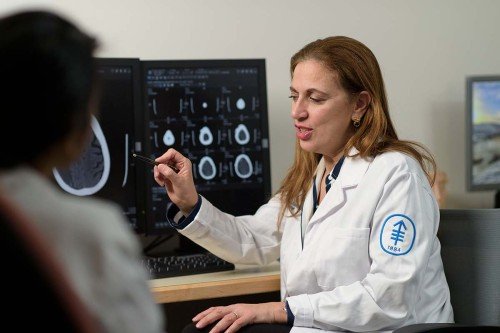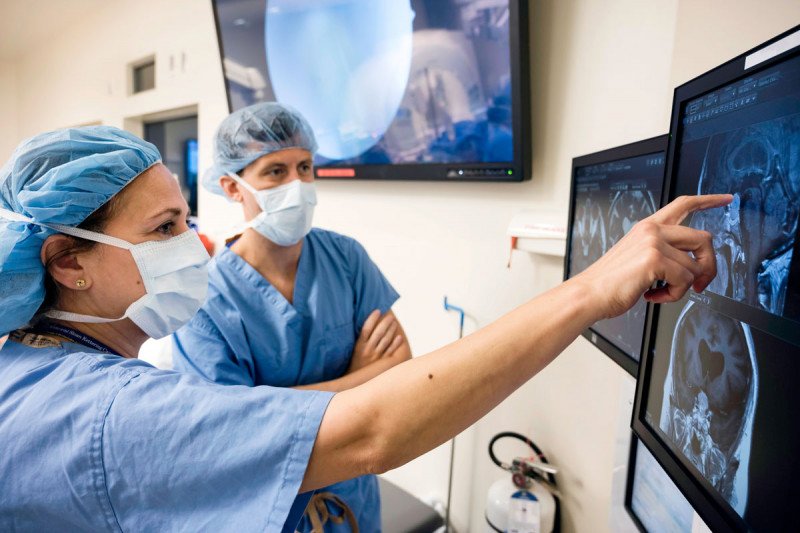
Chair of the Department of Neurosurgery Viviane Tabar (left) is part of a multidisciplinary team that works seamlessly to provide the best in surgical care for people with brain tumors.
Brain Cancer Diagnosis Procedures
To properly treat a primary brain tumor, it’s crucial that we have an accurate diagnosis. There are approximately 125 types of brain tumors and the treatment for each type is in many cases unique.
We’ll assess your condition and base a diagnosis on a number of factors, including:
- your symptoms and medical history
- results of your neurologic examination and other tests
- the size, location, and grade of the tumor as determined through diagnostic imaging
- the condition of your overall health
If your doctors suspect that you have a brain tumor, they may recommend diagnostic imaging. Our Brain Tumor Center specialists use CT, PET, and MRI scans to identify a brain tumor as well as determine its size, location, and grade (how quickly it’s growing). Knowing the size and location of the tumor helps your doctor plan the best treatment approach.
The first treatment for a brain tumor is often surgery. The goal of brain tumor surgery is to remove as much of the tumor as possible without causing harm to normal tissue. Surgery can also provide an opportunity to biopsy the tumor to learn more about what type it is and whether it’s cancerous.
Brain Tumor Biopsy
In a biopsy, we remove a tissue sample from the affected area and send it to a pathologist to analyze under a microscope. The pathologist determines what type of tumor it is and provides any other information that can help your doctors customize the most effective plan of care for you. The location of the tumor in your head determines which biopsy approach would be best for you. Some of the ways we perform biopsies include:
-
Craniotomy
Your surgeon removes a piece of your skull bone to access the tumor, and removes a sample of the tissue to send to the pathologist for analysis. -
Needle Biopsy
Your surgeon uses 3-D imaging to guide a very thin needle into the tumor and remove a tissue sample. This procedure is good for tumors located deep in the brain, and it helps protect healthy brain tissue. -
Neuroendoscopy
Your surgeon uses an endoscope (a thin tube with a light and lens on its tip) to operate and retrieves tissue through a small opening in the skull. This is a minimally invasive procedure. -
Lumbar Puncture (Spinal Tap)
Our experts take a sample of spinal fluid to look for abnormal cells, which may indicate the presence of a tumor. Learn more about this procedure.
Surgery for Primary Brain Tumors
Awake Surgery for Brain Tumors
At MSK, you will be cared for by one of the most experienced neurosurgery teams in the United States. Your neurosurgeon’s top priority is to keep you safe and make sure you have a good quality of life after your operation. Our surgeons perform more than 800 brain tumor operations each year.
Improvements in surgical techniques and imaging technologies have revolutionized brain surgery in recent years. Our neurosurgeons take a multidisciplinary approach to care and use the most-advanced surgical technologies, including:
Common Brain Surgery Imaging & Surgical Techniques
Functional MRI: Brain Mapping in Surgical Planning
To plan brain surgery, our surgeons use an imaging test called a functional MRI, or fMRI, performed in the days before the procedure. This is a specialized MRI that can create a functional “map” of your brain. During the MRI, you are asked to perform simple tasks such as moving your hands and feet, counting in your head, or thinking of words that begin with a particular letter.
These tests result in a scan that can show which areas of your brain are important to everyday functions such as vision, speech, touch, and movement. From this scan, your surgeon can determine whether the tumor involves these functional areas of the brain and figure out how much of the tumor can be safely removed during the surgery.
In some cases, the tumor is so close to a delicate area that the surgeon also performs mapping of the brain during the operation. Electrodes are used to stimulate the brain surface and identify with great precision the areas of the brain that are involved in specific tasks and that therefore need to be preserved.
MRI during Surgery
Memorial Sloan Kettering’s neurosurgeons perform brain surgery in an operating room equipped with an MRI scanner. At any point during surgery, your neurosurgeon can perform an MRI to determine whether the tumor has been removed completely. If the surgeon finds any remaining tumor tissue, surgery can be resumed immediately to remove it.
Using MRI during surgery enables neurosurgeons to operate with remarkable precision and remove as much of the brain tumor as possible. It also reduces the risks that might result from a second operation. Surgeries with intraoperative MRI are also likely to reduce tumor recurrence rates and minimize complications.
MRI Surgical Navigation with Frameless Stereotactic Surgery
Our surgeons also use a very precise technique called frameless stereotaxy – sometimes referred to as surgical navigation — to plan operations and guide the team during surgery.
Technicians begin by attaching six plastic self-adhesive dots around the scalp prior to surgery. At the start of surgery, they register the exact location of these dots via MRI and then relay the position of your head to the computer system.
The team directs a wand-like viewing device at the brain, which then projects an image onto a monitor in the operating room. The image is synchronized with the MRI scan, giving your neurosurgeon up-to-the-moment orientation during the procedure. The neurosurgeon can also use the viewing wand to help identify the outermost edges of the tissue to be removed, known as the tumor margins. This helps the surgeon to remove the entire tumor whenever possible.
Advantages of surgical navigation include enhanced accuracy and greater likelihood that the operation can be done with a smaller incision. The operation may also be shorter in length as a result. This technique is used in conjunction with MSK’s intraoperative MRI.
Awake Brain Surgery
Awake brain surgery, or awake craniotomy, is a surgical technique used for some patients with primary brain tumors. In this procedure, you receive local anesthesia and intravenous medications that result in sedation but not loss of consciousness.
During parts of the procedure, you are awakened and asked to speak or to demonstrate certain movements to help guide removal of the tumor, ensuring that areas of the brain critical to speech or movement remain intact.
Neuroendoscopy
Neurosurgeons perform certain surgical procedures through a minimally invasive procedure known as neuroendoscopy. In this technique, only a small opening must be made in the skull. The surgeon performs the operation using a thin tube with a powerful lens, high-resolution video camera, and tiny surgical instruments on its tip.
This minimally invasive procedure enables doctors to use a smaller incision than in conventional surgery, enhances their ability to perform microsurgical procedures, and usually results in less injury to healthy tissue.
Telemedicine Appointments
We know that rest is an important part of the healing process, and that travel to and from appointments can take a lot of time and energy. That’s why, for some neurosurgery visits, you may be able to see your MSK care team through our telemedicine program. If we determine that telemedicine would be appropriate for you, a member of your care team will reach out.
Telemedicine is the use of video technology to connect you with members of your MSK care team. We use secure technology to make sure all of your information stays private. You can communicate through face-to-face video conferencing via a desktop computer, laptop, or tablet device at several MSK locations. We can also use telemedicine while you or a loved one is in the hospital, either to connect you with your provider or to include someone who is not able to visit in person. During your appointment, your provider will be able to check how you’re doing, assess your follow-up needs, and discuss problems you may be having. You will be able to see and hear your MSK specialist, and they will be able to see and hear you — the only difference is that you won’t be in the same room.
A virtual visit saves you time and stress. It may also help prevent an unnecessary trip to an emergency room or urgent care center. In addition, telemedicine can help cut down on missed work days for both patients and caregivers due to travel for appointments.
New Patient Appointments
Available Monday to Friday, 8:00 a.m. to 6:00 p.m. (Eastern time)