Even people who’ve had no experience with cancer have some idea of the side effects it can cause. Hair and weight changes, nausea, and other issues are common and can impact a person’s quality of life. But there are less-known complications that can have equally important effects. Many of them can last for years after treatments are over.
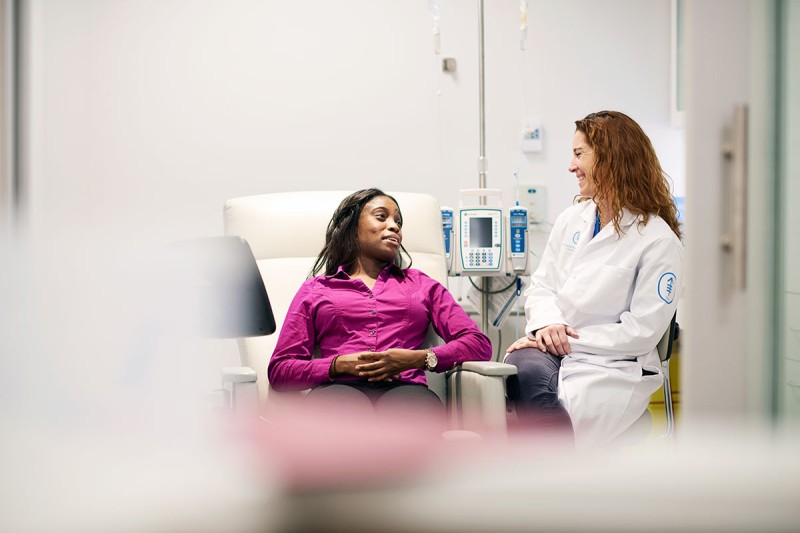
At Memorial Sloan Kettering, “we do everything we can to cure you, but treatments can affect your body in serious ways,” says Kevin Browne, Deputy Chief Nursing Officer. Each person’s response to therapy is also different. Some people hardly experience side effects or aren’t bothered by those they do have. Others face a tougher road.
The upside is that there are ways to avoid many of these unwanted effects, or at least to make them less severe if they do happen. We spoke with Mr. Browne and Erica Fischer-Cartlidge, a clinical nurse specialist at MSK, about some surprising side effects of cancer treatments and how people can reduce their impact.
Falls Caused by Peripheral Neuropathy
People who are having treatment for cancer are at serious risk for falls. Chemotherapy can cause neuropathy, a loss of feeling or pain in the feet that can make you unsteady. Other therapies can affect your sense of balance and ability to catch yourself if you start to slip. Just being on new medications as part of your treatment can also have an effect.
Many patients assume that they’re not at risk for falling, especially if they’re younger or if they feel strong and healthy, like they normally would. But the risk still very much applies.
Injuries from a fall can be catastrophic — even fatal. Falls are the second leading cause of accidental or unintentional injury deaths worldwide, according to the World Health Organization. And they happen despite every effort by hospitals and healthcare centers to stop them.
If you’re being treated in the hospital, the unfamiliar surroundings can be disorienting, especially when you get out of bed to use the bathroom, move to a chair, or take a walk. But people receiving treatment outside the hospital are equally at risk.
The first step to reduce your risk is to be aware of it in the first place. Next, ask for help. This is especially true if you’re in the hospital and need to get out of bed, as most falls happen on the way to or in the bathroom.
“That’s what your nurses are there for,” says Mr. Browne. “Always, always, always call for help before you need to get up. You’re never bothering anyone, and it’s much more important that you be safe.”
Other ways to lower your risk are to wear shoes with backs and supportive soles (no flip-flops) and to bring a companion with you to any outpatient treatment sessions to help you get where you need to go afterward. Rise to your feet slowly, and give yourself time to adjust to standing after you’ve been sitting for a while. If you feel weak or dizzy, sit down and let your caregiver or healthcare team know immediately.
Cancer-Related Fatigue
Most people anticipate that cancer treatment will make them tired. Indeed, fatigue is the most common side effect that people experience. But you might not realize just how deep that exhaustion can go, or how much it can affect your state of mind.
“Fatigue can be really upsetting for people,” says Ms. Fischer-Cartlidge. “They may not be able to physically do things, like activities with their children or even just daily routines that they are used to, and that can have a big psychological impact. It’s as important to address those emotional issues as it is to address the physical side effects of treatment.”
People with cancer also might not realize that fatigue can be the root of other problems they might think are due to something else, like not sleeping well and shortness of breath.
If you’re overwhelmed by fatigue, make sure to report it to your doctor or your healthcare team. Be as specific as you can. For instance, say, “I was so tired, I couldn’t work for three days” instead of “I am feeling tired.” Your doctor or nurse might be able to prescribe something to help with other conditions like nausea or pain that are adding to your fatigue. They can also talk with you about how exercise or diet changes might offer some improvement. Ms. Fischer-Cartlidge points to research that has shown people who walk for 20 minutes at least three times a week during cancer treatment could have less fatigue.
Talking with an expert can also help address the emotional effects of dealing with being exhausted all the time. “We have such robust resources at MSK, including social workers, psychologists, and support groups,” she adds. “These can all be really helpful with coping.”
Hormone and Sexual Changes Due to Cancer Treatment
People having treatment for breast cancer often take hormonal therapies, like tamoxifen or aromatase inhibitors, as part of their care plan. These can cause unpleasant side effects, like hot flashes, decreased interest in sex, and the onset of menopause. But these therapies, as well as androgen-suppressing drugs, which are commonly used to treat prostate cancer, can also affect the balance of hormones in men.
“Men can get hot flashes and lose their desire to have sex, just like women can,” says Ms. Fischer-Cartlidge. “It’s a side effect that’s often not stressed when men are being treated for cancer, so it can come as a surprise.” It’s also a topic that many men are uneasy discussing, so they may downplay their discomfort.
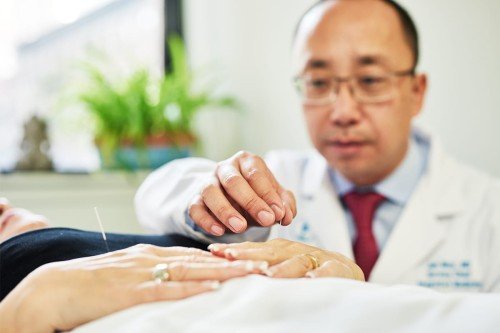
Hot flashes can be managed holistically. Complementary medicine treatments, such as acupuncture, and calming techniques, such as deep breathing and cool showers, can provide some relief. MSK also has extensive sexual health programs for women and men who are dealing with hormonal changes as well as the full range of side effects that cancer treatment can cause, including infertility and erectile dysfunction.
The vast majority of women will stop having periods during chemo treatment, if they haven’t yet gone through menopause, due to hormone fluctuations. Whether a woman’s period starts up again is unpredictable. “It might return; it might not,” says Ms. Fischer-Cartlidge.
Short-Term Memory Problems (Chemo Brain)
Often referred to as “chemo brain,” the cognitive effects of cancer treatment are quite real — and troublesome. Mental changes go beyond simple forgetfulness and can last for years after treatment is over.
Ms. Fischer-Cartlidge estimates that 80% of her patients complain about their cognitive health at some point in their treatment. “People have issues with finding the right words, their attention span, focusing, and concentration. These can seriously impact their daily life,” she says.
The cause of this pervasive mental fog isn’t clear, she adds, saying, “There are lots of theories but no firm understanding of why this happens.”
But you don’t have to exist in a cloud of confusion. Occupational therapy is similar to physical therapy but uses mental exercises instead of physical ones to improve the brain’s functioning. It can make a big difference in relieving chemo brain symptoms. Occupational therapists teach techniques that can help people with memory, time management, and organization. The therapy can be tailored to each individual’s needs.
Ms. Fischer-Cartlidge recommends doing word searches and using a smartphone, notebook, or voice recorder to keep lists or memos.







