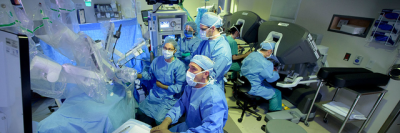
For some people, surgery is the best way of treating or curing cancer. MSK’s surgeons are very experienced in assessing whether surgery is the right treatment for the kind of cancer you have.
From the moment you hear the words “you need surgery,” MSK will guide you through this stressful time. You’re not alone. You’re in the care of a team with experts in the type of surgery you need.
Reasons for cancer surgery
Treatment: Cancer surgery can remove tumors and areas that have cancer. Surgery is a treatment that can lower the chances cancer comes back.
Diagnosis: Surgery helps diagnose what kind of cancer you have, and the stage of cancer.
Prevention: Some surgeries can prevent cancer from starting. This type of surgery removes the part of your body where cancer is likely to start.
Surgery to treat cancer
Surgery is the most common treatment for solid tumor cancers. It’s done to remove tumors and areas that have cancer.
Surgery can be done as the only treatment, or along with other treatments.
Other treatments may be done before, during, or after surgery. Treatments include radiation, chemotherapy, or other cancer treatments.
Sometimes surgery is all that’s needed to cure cancer. The goal of surgery is to remove all the cancer, or as much as we can. Your surgeon will talk with you about options that can treat the cancer and keep your quality of life.
MSK surgeons are experts in assessing the cancer, your health, and other factors. As a team, they will evaluate whether surgery is right for you. They will assess:
- The type of cancer you have.
- Where the cancer is located, and the best way to reach it and remove it.
- The extent of the cancer, and whether it has metastasized (spread) to other areas.
- How fast the cancer is growing.
- Your general health, and whether your body can recover well from surgery.

Surgery to diagnose and stage cancer
Surgery helps us diagnose what kind of cancer you have. It also helps us learn the cancer’s stage.
Staging is part of the cancer diagnosis process. It tells us if the cancer has spread, and how far.
You may have a biopsy, a procedure to take samples of tissue or cells to check for cancer. During a biopsy, your doctor removes a small number of cells or a piece of tissue. We then test the sample for signs of cancer, or to learn more about the tumor’s genetics.
Your care team will use this information along with diagnostic methods, such as imaging and blood tests. The information from the surgery and tests helps us choose the best treatment for you. It also may help us predict how well your treatment will work.
Surgery to prevent cancer
Some surgeries are done to lower the chances of getting cancer. For example, your doctor will remove polyps (growths) in the colon to prevent colorectal cancer.
Your care team may also recommend surgery if your family background raises your chance of getting cancer. You’re at higher risk for some cancers if you have certain genetic changes (mutations or variants). These changes may be hereditary, which means they’re passed on from parents to children.
Surgery is done to remove the part of the body where a hereditary cancer is likely to start. For example, some people have surgery to remove a breast because they’re at higher risk for hereditary breast cancer.
Reconstructive surgery after treatment
Plastic and reconstructive surgery changes how your body looks or works after treatment. For example, some people choose to have reconstructive surgery to rebuild a breast after a mastectomy. A mastectomy is surgery to remove a breast to treat or prevent breast cancer.
Plastic or reconstructive surgery also can replace normal tissue and nerves removed during treatment for head and neck cancer. It can repair places where we removed skin and tissue to treat skin cancer. Reconstructive surgery can create replacements for organs, such as the bladder, that we removed to treat cancer.
Surgery to help with cancer symptoms and pain
Palliative surgery can help with the symptoms of cancer, such as pain. It can improve the quality of life for people with advanced cancer. Palliative surgery also can help stop symptoms from getting worse. It may stop complications (problems), such as bleeding inside the body.

Types of cancer surgery
Minimally invasive cancer surgery
MSK surgeons are experts in surgery methods that do less harm to your body. For some people, we may recommend minimally invasive cancer surgery. This kind of surgery does less harm to your body because it’s done with small incisions (cuts).
MSK surgeons use these minimally invasive methods to diagnose, stage, and treat cancers. They include thoracic, gynecologic, gastrointestinal, prostate, and other cancers.
Benefits of minimally invasive cancer surgery may include:
- Less loss of blood.
- A shorter hospital stay
- A faster recovery
- Less scarring
- Less risk of infection
- Fewer complications (problems) during and after surgery
MSK surgeons do more than 30,000 operations each year. More than a third of those (about 10,000 each year) are done as outpatient procedures. That means you do not have to stay overnight and can go home the same day.
Surgeons at MSK Manhattan use minimally invasive surgery methods so you can recover faster. We use these methods at our main hospital and at our Josie Robertson Surgery Center in Manhattan.
There are 2 types of minimally invasive cancer surgery. They’re called laparoscopic surgery and robot-assisted surgery.
Laparoscopic cancer surgery
In laparoscopic surgery, your surgeon will make a small incision (cut). They will put a laparoscope through the incision. The laparoscope is a long, thin surgical tool with a video camera. It lets your surgeon see inside your body. Laparoscopic procedures can remove tumors or other tissue.
With a laparoscopic surgery, your surgeon directly controls the surgical tools with their hands. They can see the images from the laparoscope on a television monitor. Imaging lets your surgeon see the tumor very clearly. That helps their chances of getting out all the cancer.
Robotic-assisted laparoscopic surgery
With robotic-assisted surgery, your surgeon uses the da Vinci® Surgical System. They sit at a console and control a robot that moves the surgical tools. There are hand, finger, and foot controls.
The console has a special monitor where they can see very clear, 3D images from the laparoscope. Your surgeon can see and remove a tumor or other tissue. MSK’s operating rooms have the latest technology, including 11 robotic platforms.
At MSK, we use robotic-assisted laparoscopic surgery to diagnose, stage, and treat many types of cancer. This includes abdominal, gynecologic, lung, esophageal, prostate, hepatobiliary, and gastrointestinal cancers, among others. MSK’s general and cancer surgeons are very experienced in robotic surgery.
Meet MSK Surgeon Jeffrey Drebin
Why should I choose Memorial Sloan Kettering for cancer surgery?
Our surgeons are also cancer experts
MSK surgeons are specialists in both certain types of cancer, and in the surgery that treats that type of cancer. They’re experts who do many special, complex surgeries each year. Patients at hospitals that do a higher number of surgeries in general have better treatment results.
Our surgeons care deeply about finding better ways to treat and cure cancer. They’re trained in methods that make surgery more precise than ever before. Surgeons from around the world come to MSK to learn new surgery methods from our surgeons.
For example, MSK has developed methods that make pancreatic surgery safer for more people. MSK surgeons do more than 400 pancreatic cancer operations each year. This volume is among the highest in New York City and across North America as well.
MSK’s approach lets us do surgeries that many other hospitals label inoperable (which means surgery is not an option). They think it’s too hard to reach the tumor, or it’s too close to major blood vessels.
MSK’s surgeons are among the nation’s most experienced in complex genitourinary cancer surgeries. Genitourinary cancer affects the genitourinary (jeh-nih-toh-YOOR-ih-nayr-ee) system (body parts related to reproduction and to the urinary system). The Urology Service in the Department of Surgery performed more than 5,000 surgeries in 2022. It’s a worldwide leader in all types of surgery for this cancer.
In 2023, the American College of Surgeons announced MSK was the first-ever Level I Specialty Children’s Center in Oncology. This national honor means MSK meets the highest-quality standards for surgical care in young patients.General children’s hospitals can have experts in many areas. At MSK, our focus is cancer. Our surgeons are experts in in pediatric surgery or in cancer surgery.

MSK surgeons are part of a team
Surgeons at MSK are part of your cancer care team. They work closely with our cancer diagnosis team, medical oncologists (cancer doctors), and many other cancer experts. Their goal is to make sure your surgery goes smoothly. Together, they make sure you do well during and after cancer surgery.
We know when it’s not the right time for surgery
Surgery may not be the best treatment for you right now. Waiting to do surgery is a cancer treatment called active surveillance (monitoring).
Active surveillance is a successful treatment for prostate cancer. It’s also sometimes an option for thyroid and kidney cancers.
Cancer science research is giving our doctors the tools to better understand when a slow-growing cancer is not a threat. Our approach may let you delay treatment until you have symptoms or the cancer changes. Surgery has risks and side effects, and our surgeons will help you avoid it if they can.
Surgery with fewer side effects
MSK surgeons work hard help people fully recover after treatment. Their goal is to get your body working the way it did before cancer, if possible.
Cancer surgery can have side effects. They depend on the type of cancer, its location, and your general health. At MSK, we’re exploring technology and surgery methods that cause fewer side effects from surgery. We’ll help you understand the benefits and risks of your surgery.
Supportive care to help you recover after surgery
Your MSK care team will support you after surgery. We’ll give you instructions about what to expect after surgery, such as possible side effects. We have an online library of patient education resources with important information to help you recover sooner. Your care team will share this information with you.
For example, they may help you learn how to change your bandages and care for your surgical wound. They may show you how to drain fluid from the surgery site. They’ll explain what to watch for after surgery, such as bleeding and signs of infection.
Pain management is an important part of cancer care. MSK was the first cancer center in the United States to have a service just for treating pain in people with cancer. Our pain experts will help relieve or manage pain after surgery. They can help while you’re still in the hospital, and after you’re home.
MSK’s rehabilitation services help you get moving and strong again after surgery. Your cancer care team includes physiatrists, physical therapists, respiratory therapists, occupational therapists, and other rehabilitation specialists. They can get you back to your usual activities as soon as possible. They can help with your breathing, speech problems, muscle strength, lymphedema, and many other issues after surgery.