This information will help you get ready for your external beam radiation therapy to your breast or chest wall at MSK. It will help you know what to expect and how to care for yourself before, during, and after radiation therapy.
About radiation therapy
Radiation therapy uses high-energy radiation to treat cancer. It works by damaging cancer cells and making it hard for them to multiply. Your body can then get rid of the damaged cancer cells. Radiation therapy also affects normal cells, but they can fix themselves in a way that cancer cells can’t.
Radiation therapy takes time to work. It takes days or weeks of treatment before cancer cells start to die. They keep dying for weeks or months after radiation therapy ends.
At MSK, most people have radiation therapy to their breast or chest wall after surgery. If your treatment plan includes chemotherapy (chemo), you will probably start your radiation therapy 4 weeks after finishing your chemo treatment. We will talk with you about what to expect.
About external beam radiation therapy
External beam radiation therapy is a type of radiation therapy. With external beam radiation therapy, a treatment machine aims beams of radiation at the target area. The beams pass through your body and damage cancer cells in their path. You will not see or feel the radiation.
You may be having radiation therapy to 1 or more of these areas:
- Your breast.
- Your chest wall.
- The lymph nodes near your collarbone.
- The lymph nodes under your arm.
- The lymph nodes near your sternum (breastbone).
Your radiation oncologist and nurse will talk with you about your treatment plan.
Your role on your radiation therapy team
Your radiation therapy care team will work together to care for you. You’re a part of that team, and your role includes:
- Getting to your appointments on time.
- Asking questions and talking about your concerns.
- Telling us when you have side effects.
- Telling us if you’re in pain.
-
Caring for yourself at home by:
- Quitting smoking if you smoke. MSK has specialists who can help. To learn more about our Tobacco Treatment Program, call 212-610-0507. You can also ask your nurse about the program.
- Caring for your skin based on our instructions.
- Drinking liquids based on our instructions.
- Eating or avoiding the foods and drinks we suggest.
- Staying around the same weight.
Before your radiation therapy to your breast or chest wall
Simulation
You will have a treatment planning procedure called a simulation before you start your radiation treatments. You will not get any radiation during your simulation.
During your simulation, your radiation therapists will take imaging scans. They may mark your skin with little tattoo dots. These things help us:
- Map your treatment area.
- Make sure you get the right dose (amount) of radiation.
- Limit the dose of radiation that gets to your nearby tissues.
Your simulation will take 60 to 90 minutes.
Pain medicine
You’ll lie in one position for about 30 to 60 minutes during your simulation. The exact length of time depends on your radiation treatment plan. Tell us if you think you’ll be uncomfortable lying still. You can also take an over-the-counter pain medicine or your usual pain medicine 1 hour before your appointment.
What to wear
Wear comfortable clothes that are easy to take off. You will need to undress from the waist up and change into a hospital gown.
Do not wear jewelry, powder, lotion, or cream unless a member of your care team says it’s OK.
Take devices off your skin
You may wear certain devices on your skin. Before your simulation or treatment, some device makers recommend you take off your:
- Continuous glucose monitor (CGM)
- Insulin pump
If you use one of these, ask your radiation oncologist if you need to take it off. If you do, make sure to bring an extra device to put on after your simulation or treatment.
You may not be sure how to manage your glucose (blood sugar) while your device is off. If so, before your appointment, talk with the healthcare provider who manages your diabetes care.
What to expect when you arrive
A member of your radiation therapy team will check you in when you arrive. They’ll give you an identification (ID) wristband with your name and date of birth. During your appointment, many staff members will check your ID wristband and ask you to say and spell your name and date of birth. This is for your safety. People with the same or a similar name may be getting care on the same day.
Your radiation therapists will review what to expect during the simulation. If you haven’t already signed a consent form, they will go over the form with you. They will answer any questions you have and ask for your signature.
During your simulation
You will need to undress from the waist up and change into a hospital gown for your simulation. A staff member will bring you to the changing room. Keep your shoes on. If you need help changing, tell a member of your radiation therapy team. A care provider will help you in the changing room.
If you wear a head covering, you may need to take it off. Wigs, turbans, and caps are examples of head coverings.
Once you’re ready, your therapists will bring you to the simulation room. They will help you lie on the simulation table. The table will have a sheet on it, but it’s hard and has no cushion. Tell your radiation therapists if you have not taken pain medication and think you might need it. Tell them before your simulation begins starts, if you can.
Throughout your simulation, you will feel the table move into different positions. Your radiation therapists will turn the lights in the room on and off. You will see red or green laser lights on each wall. Your radiation therapists use these as a guide when they position you on the table. Do not look straight into the lasers. They can harm your eyes.
Your radiation therapists will walk in and out of the room during your simulation. Someone will always be able to see and hear you. You will hear your radiation therapists talking to each other as they work. They will also tell you what they are doing.
The simulation room often feels cool. If you feel uncomfortable, tell your radiation therapists. They will do everything they can to make sure you’re comfortable and have privacy.
Positioning
You may lie on your back or on your belly. In either position, you will raise one or both arms above your head. Do not move once your simulation starts. It’s important to stay in the same position. If you’re uncomfortable or need help, tell your radiation therapists.
Deep inspiration breath hold (DIBH)
Your radiation therapists may ask you to hold your breath for 15 to 20 seconds at a time during your simulation and treatment. Whether they do depends on your treatment plan and the shape of your body. Your care team will let you know if you will need to do this.
To learn more, watch About Deep Inspiration Breath Hold (DIBH) and the Visual Coaching Device.
Imaging scans
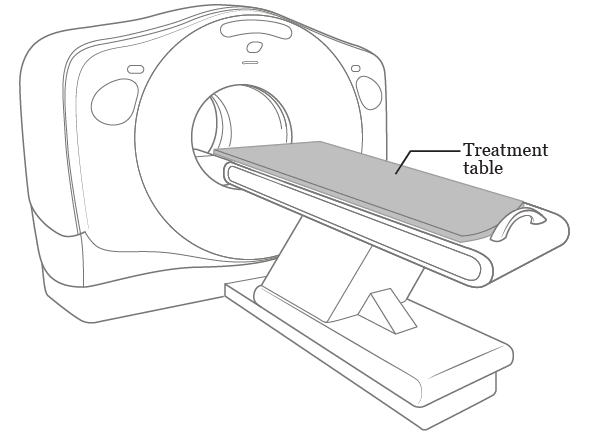
You’ll have imaging scans of your treatment area. These may be done on an x-ray machine called a simulator or on a computed tomography (CT) scan machine (see Figure 1). We will use these scans to map your treatment. We will not use them for diagnosis or to find tumors. If you need other imaging scans, your radiation nurse will tell you what to expect.
The imaging scans will take about 45 minutes. During the scans, you’ll hear the machine turn on and off. Even if the noise seems loud, your radiation therapists will be able to hear you if you talk to them.
Skin markings (tattoos)
Your radiation therapists may use a felt-tipped marker to draw on your skin in the treatment area. You may also need skin markings called tattoos. Not everyone needs tattoos. Your care team will talk with you about what to expect.
If you need tattoos, your radiation therapists will use a sterile (clean) needle and a drop of ink to make them. Each tattoo will feel like a pinprick. They will not be bigger than the head of a pin.
After they make the tattoos, your radiation therapists will take photos of you in your position. They will use the photos and tattoos to make sure you’re in the right position for your radiation treatments.
You can wash off the felt markings after your simulation. If you need tattoos, they are permanent. They will not wash off. If you’re concerned about having tattoos as part of your radiation therapy, talk with your radiation oncologist.
Scheduling your radiation treatments
At the end of your simulation appointment, you’ll schedule your set-up procedure and radiation appointments. You’ll also be assigned to a radiation treatment machine for your radiation treatments.
Your radiation oncologist will talk with you about your treatment schedule.
- If you’re getting radiation therapy after a lumpectomy, your doctor will talk with you about whether you need whole breast or partial breast radiation. Most people have radiation treatments every day for 1 to 4 weeks.
- If you’re getting radiation therapy to your chest wall or the lymph nodes near your collarbone, under your arm, or near your sternum, you’ll have radiation treatments every day for 5 to 6 weeks.
You must come to every one of your radiation treatment appointments. Your radiation therapy may not work as well if you skip or miss treatments. If you cannot come to one of your treatments for any reason, call your radiation oncologist’s office to tell your radiation team. If you need to change your schedule for any reason, speak with your radiation therapists.
Treatment planning
Between your simulation and your first radiation treatment, your radiation oncologist will work with a team to plan your radiation treatments. They’ll use the imaging scans done during your simulation to plan the angles and shapes of your radiation beams. They will carefully plan and check the details. This takes 1 to 2 weeks.
During your radiation therapy to your breast or chest wall
Vitamins and dietary supplements during radiation therapy
Vitamins, minerals, and herbal or botanical (plant-based) supplements are examples of dietary supplements.
It’s OK to take a multivitamin during your radiation therapy. Do not take any other dietary supplements without talking with a member of your care team.
Avoid antioxidant supplements, such as:
|
|
You do not need to remove these antioxidants from your diet. If you want to talk with a clinical dietitian nutritionist about your diet or supplements, tell your radiation nurse.
Skin care
On the day of your first radiation treatment, you’ll start putting triamcinolone 0.1% cream on your skin in the treatment area. This is a prescription cream that will help protect your skin. You’ll use it every day, once in the morning and once in the evening. This includes the days you don’t have treatment. Your radiation nurse will give you more information about it before your first treatment.
Your radiation oncologist may recommend using Mepitel® Film to protect your skin in the treatment area. If they do, a nurse will put the Mepitel Film on your skin in the treatment area before your first treatment. Keep it on until the edges start to peel up. Once they do, see your radiation nurse for touch up or replacement as needed.
Radiation treatment appointments
You’ll stay in one position for about 10 to 20 minutes during each of your radiation treatments, depending on your treatment plan. If you think you’ll be uncomfortable lying still, you can take acetaminophen (Tylenol) or your usual pain medicine 1 hour before your appointments.
Set-up procedure
You’ll have a set-up procedure at your first radiation treatment appointment. The set-up procedure and first treatment usually takes about 1 hour.
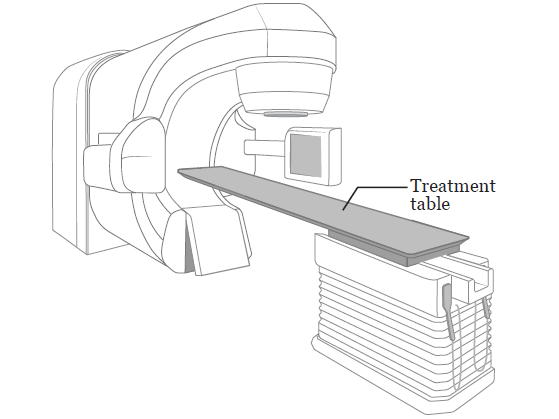
Your radiation therapists will bring you to the room where you’ll get your radiation treatments each day. They’ll help you lie on the treatment table (see Figure 2) in the same position you were in during your simulation.
Your radiation therapists will take special x-rays called beam films to make sure your position and the treatment area are correct. The beam films will be repeated throughout your treatment. They aren’t used to see how you respond to the treatment.
During your radiation treatments
You’ll be in the exact same position as you were during your simulation and set-up procedure. Your radiation therapists will do everything they can to make sure you’re comfortable. Then, they’ll leave the room, close the door, and start your treatment.
Stay still during your radiation treatments. You will not see or feel the radiation, but you may hear the machine as it moves around you and turns on and off. Your radiation therapists will be able to see you on a monitor and talk with you through an intercom during your whole treatment. Tell them if you’re uncomfortable or need help.
You’ll be in the treatment room for 10 to 20 minutes, depending on your treatment plan. You’ll spend most of this time getting in the right position. The actual treatment only takes a few minutes.
Your radiation treatments will not make you immunocompromised (weaken your immune system). They do not affect your blood counts like chemo can.
Your radiation treatments will not make you or your clothes radioactive. It’s safe for you to be around other people.
About boosts
You may get an extra dose of radiation called a boost after you finish the first part of your radiation therapy. During the boost, radiation will be directed to just the area where the lump or cancer cells were found. It will not be directed to your whole breast. Your care team will tell you if you will be getting a boost.
During your boost appointment
Before your boost, your radiation therapist will mark your skin with a felt-tipped marker to outline the boost field. Wear a shirt that you don’t mind getting stained. The dye from the marker may stain your clothes. Also, these skin markings are not permanent. Do not wash them off until you finish treatment.
You’ll get about the same amount of radiation that you got for your other treatments, but it will be aimed at a smaller area. You may use a different treatment machine for your boost or lie in a different position.
Status check visits
Your radiation oncologist and nurse will see you each week to talk with you about your concerns, ask about any side effects you’re having, and answer your questions. Plan to be at your treatment appointment for about an extra 15 to 30 minutes on those days.
During these visits, your radiation oncologist and nurse will check your skin in the treatment area. They may prescribe ointments or creams and special dressings to care for your skin.
If you need to speak with your radiation oncologist or nurse between your status check visits, call your radiation oncologist’s office. You can also ask your radiation therapists or another staff member to contact them.
Weekly emails
We’ll email you a questionnaire about your symptoms every week. This questionnaire helps your radiation therapy team know how you’re doing and if you’re having any side effects. You’ll complete the questionnaire once a week for 6 weeks after you finish radiation therapy.
It’s helpful to read Communicating With Your Care Team: When to Call or Use MSK MyChart and How to Take Pictures of Your Skin for Your Healthcare Provider.
Side effects of radiation therapy to your breast or chest wall
You may have side effects from radiation therapy. The type and how strong they are depends on many things. These include the dose of radiation, the number of treatments, and your overall health. The side effects may be worse if you’re also getting chemo.
You may start to notice side effects about 2 to 3 weeks after you start radiation therapy. They may get worse for up to 2 weeks after your radiation therapy, but they’ll slowly get better over 4 to 6 weeks after your last treatment. Some side effects may take longer to go away.
Follow the guidelines in this section to help manage your side effects during and after your radiation therapy.
Skin and hair reactions
Your skin and hair in the treatment area will change during your radiation therapy. This is normal.
- Your skin may turn pink, red, tanned, or look like it has sunburn. The skin in the folds under your arm and breast, over your collar bone, and in other parts of the treatment area that have been in the sun may blister and peel.
- Your skin may become very sensitive and itchy.
- You may get a rash, especially in any area where your skin has been in the sun. Tell a member of your radiation therapy team if you get a rash at any time during your radiation therapy. Rashes are sometimes a sign of an infection.
- You may lose some or all of your hair under your arm on the treated side. It usually grows back in 2 to 4 months after you finish radiation therapy.
If your skin becomes open, wet, and oozing, contact your radiation team. They may prescribe a cream called Silvadene® (silver sulfadiazine). Your radiation oncologist may also stop your radiation therapy until your skin heals. Most people don’t need to stop their treatments.
Skin reactions from radiation therapy are usually strongest 1 or 2 weeks after you finish radiation therapy and then start to heal. It often takes 3 to 4 weeks for skin reactions to heal. If you have any questions or concerns, don’t hesitate to contact your radiation oncologist or nurse.
Skin care guidelines
Follow these guidelines to care for your skin during treatment. Keep following them until your skin gets better. These guidelines refer only to the skin in the treatment area.
Your radiation nurse will give you more information about caring for your skin. This may include applying ointments, creams, special dressings, or all 3. Follow their instructions.
- Bathe or shower daily using warm water and a mild unscented soap such as Neutrogena®, Dove®, baby soap, Basis®, or Cetaphil®. Rinse your skin well and pat it dry with a soft towel.
- You can use deodorant on intact (not broken) skin in the treatment area. Stop using it if your skin becomes irritated.
- When washing, be gentle with your skin in the treatment area. Do not exfoliate your skin.
- The tattoo marks you got before your treatment are permanent and don’t wash off. You may get other markings during treatment, such as an outline of your treatment area with a purple felt-tipped marker. You can take off these markings with mineral oil when your radiation therapists say it’s OK.
- Put a thin layer of 0.1% triamcinolone cream on the treatment area 2 times every day. You do not need to take off the cream before your radiation treatments as long as you apply a thin layer. Keep using the 0.1% triamcinolone cream 2 times every day for 2 weeks after you finish radiation therapy.
- Do not use alcohol or alcohol pads on your skin in the treatment area.
Avoid irritating your skin in the treatment area
- Wear loose-fitting cotton clothing and undergarments in the treatment area. Avoid tight clothing that will rub up against your skin, including underwire bras.
- Do not use makeup, perfume, powder, or aftershave in the treatment area.
- Do not put tape on your skin in the treated area. This includes adhesive (sticky) bandages.
- If your skin is itchy, do not scratch it. Keep using the 0.1% triamcinolone cream 2 times every day. This is the best treatment for itching.
- Avoid shaving in the treatment area. If you must shave, use only an electric razor. Stop if your skin becomes irritated.
- Do not let your treated skin come into contact with extreme hot or cold temperatures. This includes hot tubs, water bottles, heating pads, and ice packs.
- If you don’t have any skin reactions during your treatment, you can swim in a chlorinated pool. Rinse off the chlorine right after getting out of the pool.
- Avoid tanning or burning your skin during treatment and for the rest of your life. If you’re going to be in the sun, use a sunblock with an SPF of 30 or higher. Wear loose-fitting clothing that covers as much of your skin as possible.
Breast discomfort or swelling
You may have some tenderness in your breast on your affected side, especially at your nipple. You may also develop extra fluid in your breast that may cause sharp, stabbing sensations. Your breast or chest may feel heavy or swollen. Your shoulder on your affected side may also feel stiff.
These sensations can start within the first few days of your radiation therapy. They can go on for many months after you finish radiation therapy. Below are suggestions to help you reduce this discomfort.
- If you wear bras, you may want to choose soft, loose bras without an underwire. Sports bras or cotton bras are good choices. You may even find it more comfortable to not wear a bra at all.
- Take pain medicines such as nonsteroidal anti-inflammatory drugs (NSAIDS) as needed. Some examples of NSAIDs are ibuprofen (Advil®) and naproxen (Aleve®). If you can’t take an NSAID, you can take acetaminophen (Tylenol) instead.
Fatigue
Fatigue is feeling tired or weak, not wanting to do things, not being able to concentrate, feeling slowed down, or lacking energy.
You may develop fatigue after 2 to 3 weeks of radiation treatments. The fatigue can range from mild to severe, and it may be worse at certain times of day. Your fatigue will gradually go away after you finish radiation therapy, but it can last for several months.
Managing fatigue
- If you’re working and are feeling well, it’s OK to keep working. If you feel fatigued, working less may help you have more energy.
- Plan your daily activities. Pick the things you need or really want to do and do them when you have the most energy. For example, you may go to work but not do housework or watch your children’s sports event but not go out to dinner.
-
Plan time to rest or take short (10 to 15-minute) naps during the day, especially when you feel more tired.
- Try to sleep at least 8 hours every night. This may be more sleep than you needed before you started radiation therapy. You may also find it helpful to:
- Go to sleep earlier at night and get up later in the morning.
-
Be active during the day. For example, if you’re able to exercise, you could go for a walk, do yoga, or ride a bike.
- Relax before going to bed. For example, read a book, work on a jigsaw puzzle, listen to music, or do a calming hobby.
- Ask family and friends to help you with chores and errands. Check with your insurance company to see if they cover home care services.
- Some people have more energy when they exercise. Ask your radiation oncologist if you can do light exercise, such as walking, stretching, or yoga. Read Managing Cancer-Related Fatigue with Exercise to learn more.
- Eat foods and drink liquids that are high in protein and calories. Read Eating Well During Your Cancer Treatment or Nutrition and Breast Cancer: Making Healthy Diet Decisions to learn more.
Symptoms such as pain, nausea (feeling like you’re going to throw up), diarrhea (loose or watery bowel movements), trouble sleeping, or feeling depressed or anxious can increase your fatigue. Ask your radiation oncologist or nurse for help with any other symptoms you may have.
Sexual and reproductive health
You can be sexually active during your radiation therapy unless your radiation oncologist gives you other instructions. You will not be radioactive or pass radiation to anyone else. If you or the person you’re sexually active with can get pregnant, it’s important to use birth control (contraception) during your radiation therapy.
You may have concerns about how cancer and your treatment can affect your sex life. You are not radioactive. You can’t pass radiation to anyone else. It’s safe to be in close contact with others.
You can be sexually active during your radiation therapy, unless your radiation oncologist gives you other instructions. If you or your partner are able to have children, you must use birth control (contraception) to prevent pregnancy during your radiation therapy.
Talking with your radiation oncologist or nurse about your sexual health can be hard, but it’s an important conversation to have. They may not bring it up unless you share your questions and concerns. You may feel uncomfortable, but most people in cancer treatment have similar questions. We work hard to make sure everyone in our care feels welcome.
Sexual health programs
MSK offers sexual health programs. These programs can help you manage the ways your cancer or cancer treatment affects your sexual health or fertility. Our specialists can help you address sexual health or fertility issues before, during, or after your radiation therapy.
- To learn about our Female Sexual Medicine & Women’s Health Program or to make an appointment, call 646-888-5076.
- To learn about our Male Sexual & Reproductive Medicine Program or to make an appointment, call 646-888-6024.
- To learn about our Cancer and Fertility Program, talk with your healthcare provider.
Other sexual health resources
Read Sex and Your Cancer Treatment to learn more about sexual health during cancer treatment.
The American Cancer Society also has resources about sexual health issues during cancer treatment. They’re called Sex and the Adult Male with Cancer and Sex and the Adult Female with Cancer. You can search for them at www.cancer.org or call 800-227-2345 for a copy.
Emotional health
|
|
|
You might also worry about telling your employer you have cancer or about paying your medical bills. You may worry about how your family relationships may change, or that the cancer will come back. You may worry about how cancer treatment will affect your body, or if you will still be sexually attractive.
It’s normal and OK to worry about all these things. All these kinds of feelings are normal when you or someone you love has a serious illness. We’re here to support you.
Ways to cope with your feelings
Talk with others. When people try to protect each other by hiding their feelings, they can feel very alone. Talking can help the people around you know what you’re thinking. It might help to talk about your feelings with someone you trust. For example, you can talk with your spouse or partner, close friend, or family member. You can also talk with a chaplain (spiritual advisor), nurse, social worker, or psychologist.
Join a support group. Meeting other people with cancer will give you a chance to talk about your feelings and learn from others. You can learn how other people cope with their cancer and treatment and be reminded you’re not alone.
We know that all cancer diagnoses and people with cancer are not the same. We offer support groups for people who share similar diagnoses or identities. For example, you can join a support group for people with breast cancer or for LGBTQ+ people with cancer. Visit www.msk.org/vp to learn about MSK’s support groups. You can also talk with your radiation oncologist, nurse, or social worker.
Try relaxation and meditation. These kinds of activities can help you feel relaxed and calm. You might try thinking of yourself in a favorite place. While you do, breathe slowly. Pay attention to each breath or listen to soothing music or sounds. For some people, praying is another way of meditation. Visit www.msk.org/meditations to find guided meditations lead by our Integrative Medicine and Wellness providers.
Exercise. Many people find that light movement, such as walking, biking, yoga, or water aerobics, helps them feel better. Talk with your healthcare provider about types of exercise you can do.
We all have our own way of dealing with tough situations. Often, we do what worked for us in the past. But sometimes that’s not enough. We encourage you to talk with your doctor, nurse, or social worker about your concerns.
After your radiation therapy to your breast or chest wall
Follow-up appointments
It’s important to come to all your follow-up appointments with your radiation oncologist. During these appointments, they will check how you’re recovering after your radiation therapy.
Write down your questions and concerns before your follow-up appointments. Bring this and a list of all your medicines with you. You can also call your radiation oncologist or nurse any time after you finish radiation therapy or between follow-up appointments.
At some point, your radiation oncologist may transfer your care to a survivorship nurse practitioner (SNP). The SNP is a member of the MSK Breast Cancer team. They work closely with your radiation oncologist. As your needs decrease, your SNP and radiation oncologist may transfer your follow-up care to your local doctor. The timing for this will depend on your particular cancer and treatment plan.
When to call your radiation oncologist or nurse
Call your radiation oncologist or nurse if:
- You have a fever of 100.4 °F (38 °C) or higher.
- You have chills.
- Your skin is painful, peeling, blistering, moist, or weepy.
- You have discomfort in the treatment area.
- Your breast, underarm (armpit), or arm is getting more swollen.
- You have any new or unusual symptoms.
Support services
MSK support services
Counseling Center
www.msk.org/counseling
646-888-0200
Many people find that counseling helps them. Our counseling center offers counseling for individuals, couples, families, and groups. We can also prescribe medicines to help if you feel anxious or depressed. Ask your healthcare provider for a referral or call the number above to make an appointment.
Integrative Medicine and Wellness Service
www.msk.org/integrativemedicine
Our Integrative Medicine and Wellness Service offers many services to complement (go along with) traditional medical care, including music therapy, mind/body therapies, dance and movement therapy, yoga, and touch therapy. Call 646-449-1010 to schedule an appointment for these services.
You can also schedule a consultation with a healthcare provider in the Integrative Medicine and Wellness Service. They will work with you to come up with a plan for creating a healthy lifestyle and managing side effects. Call 646-608-8550 to make an appointment.
Nutrition Services
www.msk.org/nutrition
212-639-7312
Our Nutrition Service offers nutritional counseling with one of our clinical dietitian nutritionists. Your clinical dietitian nutritionist will talk with you about your eating habits. They can also give advice on what to eat during and after treatment. Ask a member of your care team for a referral or call the number above to make an appointment.
Rehabilitation Services
www.msk.org/rehabilitation
Cancers and cancer treatments can make your body feel weak, stiff, or tight. Some can cause lymphedema (swelling). Our physiatrists (rehabilitation medicine doctors), occupational therapists (OTs), and physical therapists (PTs) can help you get back to your usual activities.
- Rehabilitation medicine doctors diagnose and treat problems that affect how you move and do activities. They can design and help coordinate your rehabilitation therapy program, either at MSK or somewhere closer to home. call Rehabilitation Medicine (Physiatry) at 646-888-1929 to learn more.
- An OT can help if you’re having trouble doing usual daily activities. For example, they can recommend tools to help make daily tasks easier. A PT can teach you exercises to help build strength and flexibility. Call Rehabilitation Therapy at 646-888-1900 to learn more.
Resources for Life After Cancer (RLAC) Program
646-888-8106
At MSK, care does not end after your treatment. The RLAC Program is for patients and their families who have finished treatment.
This program has many services. We offer seminars, workshops, support groups, and counseling on life after treatment. We can also help with insurance and employment issues.
Sexual Health Programs
Cancer and cancer treatments can affect your sexual health, fertility, or both. MSK’s sexual health programs can help you before, during, or after your treatment.
- Our Female Sexual Medicine & Women’s Health Program can help with sexual health problems such as premature menopause or fertility issues. Ask a member of your MSK care team for a referral or call 646-888-5076 to learn more.
- Our Male Sexual & Reproductive Medicine Program can help with sexual health problems such as erectile dysfunction (ED). Ask a member of your care team for a referral or call 646-888-6024 to learn more.
Tobacco Treatment Program
www.msk.org/tobacco
212-610-0507
MSK has specialists who can help you quit smoking. Visit our website or call the number above to learn more. You can also ask your nurse about the program.
Virtual Programs
www.msk.org/vp
Our Virtual Programs offer online education and support for patients and caregivers. These are live sessions where you can talk or just listen. You can learn about your diagnosis, what to expect during treatment, and how to prepare for your cancer care.
Sessions are private, free, and led by experts. Visit our website for more information about Virtual Programs or to register.
Radiation therapy support services
American Society for Therapeutic Radiology and Oncology
www.rtanswers.org
800-962-7876
This website has detailed information about treating cancer with radiation. It also has contact information for radiation oncologists in your area.
External support services
There are many other support services to help you before, during, and after your cancer treatment. Some offer support groups and information, while others can help with transportation, lodging (a place to stay), and treatment costs.
For a list of these support services, read External Support Services. You can also talk with an MSK social worker by calling 212-639-7020.
Questions to ask your radiation oncologist
Before your appointment, it’s helpful to write down questions you want to ask. Examples are listed below. Write down the answers during your appointment so you can review them later.
What kind of radiation therapy will I get?
How many radiation treatments will I get?
What side effects should I expect during my radiation therapy?
Will these side effects go away after I finish my radiation therapy?
What kind of late side effects should I expect after my radiation therapy?
Learn about our Health Information Policy.