
Many people with thyroid cancer have surgery to remove the cancer. The type of surgery depends on the type of thyroid cancer you have and its stage.

There are many options for thyroid cancer treatment. You may feel overwhelmed as you explore them.
This guide will help you better understand your options and get ready to talk with your doctors. You’ll have the information you need to make the best decisions for your care together.
Your care team includes doctors, nurses, and other experts in thyroid cancer. MSK’s thyroid cancer experts will make a treatment plan just for you.
Your personal thyroid cancer treatment plan will target the type and stage of thyroid cancer you have. It will be based on the latest research and therapies. You may have a few therapies used together for the best treatment results.
Your MSK care team will talk with you about the best therapies for you. You may have one treatment, or a few treatments together.
Treatment for thyroid cancer at MSK can include:

Many people with thyroid cancer have surgery to remove the cancer. The type of surgery depends on the type of thyroid cancer you have and its stage.

Radiation therapy uses high-energy X-rays or other types of radiation to kill cancer cells. It includes radioactive iodine treatment.
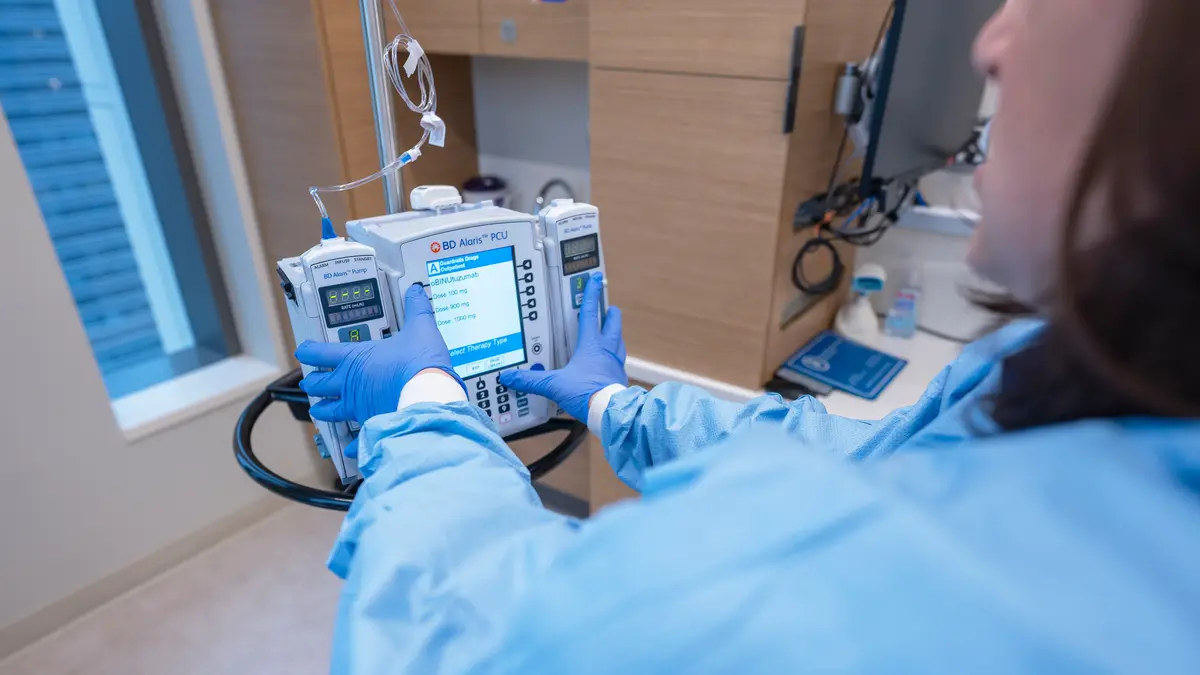
Chemotherapy, targeted therapy, and immunotherapy are called systemic therapies. Treatments are given by mouth, intravenous (IV) infusion, or injection (shot). They spread throughout the body to treat cancer.
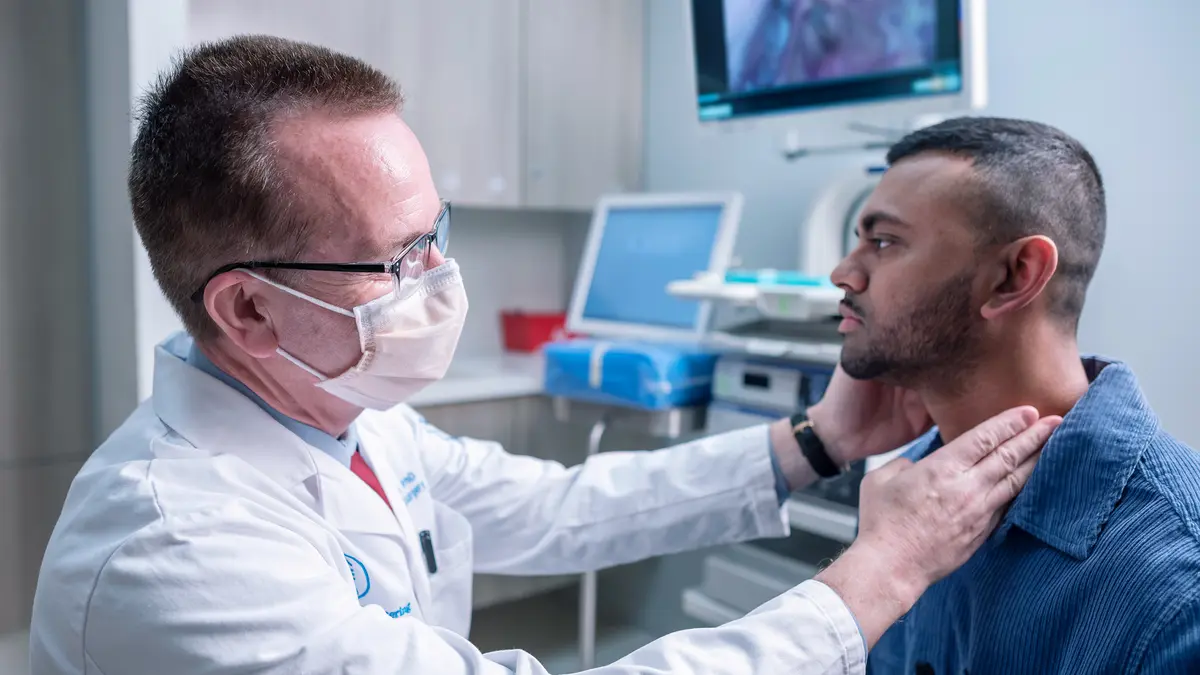
MSK’s Thyroid Nodule Assessment Program offers a fast, precise diagnosis if you have a lump (growth) in your thyroid.
We care for every person with kindness, warmth, and respect.
Your care team includes doctors, nurses, and other experts who focus on thyroid cancer. They work together using the latest science and research to create your care plan.
At MSK, we take care of the person, not just the cancer. We offer support and resources to help you during and after thyroid cancer treatment.
Your care plan may include nutrition advice, physical therapy, exercise, and mental health support. Our rehabilitation experts help you manage the side effects of thyroid cancer and its treatments.
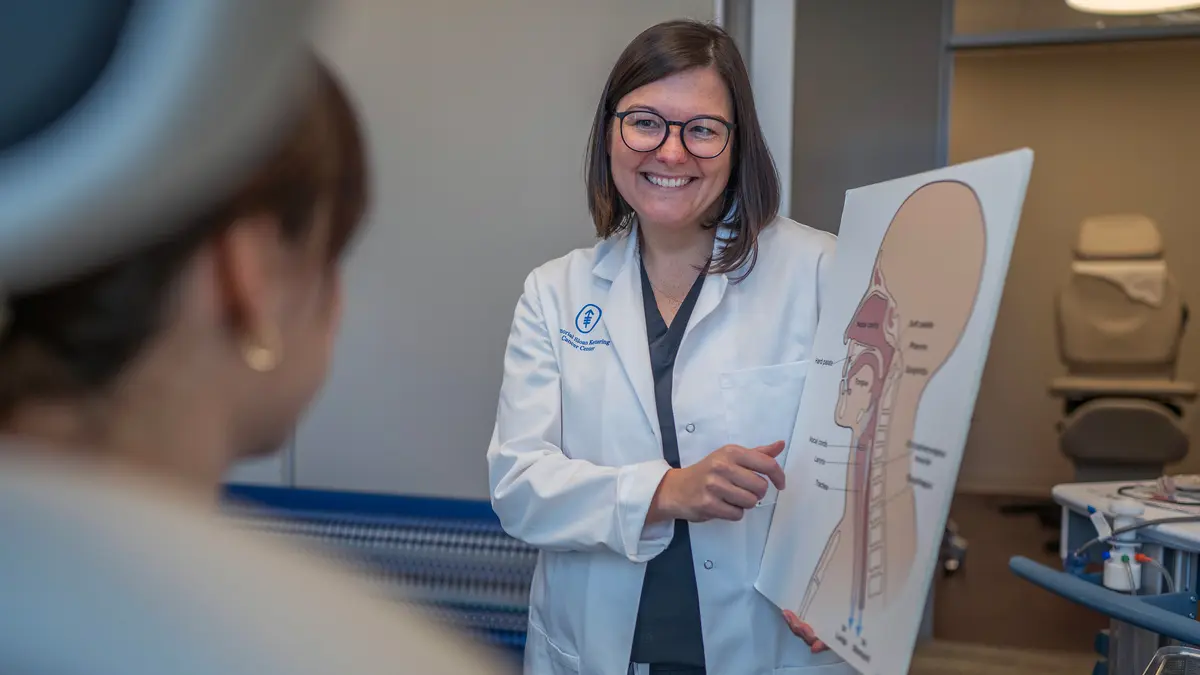
Speech pathologist Louise Cunningham helps with speech, voice, and swallowing problems after thyroid gland surgery.
You’ll get the best possible thyroid cancer care at MSK. Your care team has experts in treating the type of thyroid cancer you have.
At MSK, we offer:
Many people with cancer prefer to get treatment closer to home. MSK provides excellent cancer care on Long Island and in locations in Westchester County, New Jersey, and New York City. You can meet with your surgeon and have chemotherapy, radiation therapy, and genetic testing.
Talk with an MSK Care Advisor. We're here 24 hours a day, 7 days a week.
Thyroid cancer treatments work very well, but the cancer can come back. About 1 out of every 10 people treated for thyroid cancer are at risk for getting it again.
Thyroid cancer can come back a few months, years, or even decades later.
The risk depends on the type of thyroid cancer, too. For example, medullary thyroid cancer is more likely to come back than low-risk papillary thyroid cancer.
We describe thyroid cancer as low risk or high risk. Tests can tell us whether there is a high or low chance cancer will spread outside the thyroid gland. We base your treatment options on that risk level.
Your care team may talk with you about joining a thyroid cancer clinical trial.
Anyone can join a clinical trial from the very start of treatment, if there’s one that’s right for you.
MSK strongly encourages people from all races, genders, ages, and backgrounds to join clinical trials. It’s very important for research studies to include people from many backgrounds. It’s how our researchers can learn if a new treatment works for everyone, not just one group of people.
MSK is home to one of the largest clinical trial programs in the country. This means that we offer more cancer clinical trials than many other cancer centers in the U.S.
Learn more about MSK’s current thyroid cancer clinical trials.
Clinical trials are research studies to test new treatments, procedures, or devices to see how well they work. Every cancer treatment given to a person was first tested in a clinical trial.
Clinical trials can help us learn about new thyroid cancer drugs, such as:
MSK runs one of the country’s largest cancer clinical trials programs. An MSK clinical trial may give you access to new treatments that are not yet available at most hospitals. Watch our short video that can help you decide if a clinical trial is right for you.
If you join a clinical trial, you may be able to try new drugs to treat your type of thyroid cancer. Our patients may get a new treatment at MSK years before it’s offered at most other places.
Researchers follow strict rules to make sure all clinical trials are safe. The MSK research team will answer your questions and help you get ready for the trial. We follow your progress and keep you safe every step of the way.
sometimes years before they’re available to everyone.
from your expert care team.
for treatments you get during a clinical trial.
At MSK, your care is always a team effort. Our care teams combine the skill and experience of many kinds of thyroid cancer experts. They work together to give you the best cancer treatment.

Head and neck surgeon Dr. Snehal Patel’s care team, with RN Brianna McDonald (left), physician assistant Annie Chang, Dr. Patel, office coordinator Jennifer Savery, and RN Sadie Mercer.
MSK has Magnet® designation for our nurses’ excellent patient care, strong leadership, and a culture that values constant improvement. Only about 1 out of every 10 hospitals in the country have Magnet status. It’s one of the highest honors a hospital can earn for nursing excellence.
Your care team has special training in how to diagnose and treat thyroid cancer. Their goal is to support you during and after treatment for thyroid cancer.
We take care of the person, not just the cancer. Our social workers are here to help you and your family with the emotional, social, and physical effects of cancer.
Your care team has doctors, nurses, and other healthcare providers who are experts in thyroid cancer. They include:
Medical oncologist Dr. Devika Rao shares tips on what to expect during your first visit at MSK, and how to get ready.
We want to ensure your first visit is as productive and supportive as possible. Here are some tips on how you can best prepare.
Your team meets with a panel of experts who review and talk about your diagnosis. They discuss new ideas and the latest research. This expert panel then works together to choose your treatment plan.
A head and neck surgeon is a doctor with special training in surgery on the head and neck. This includes cancers of the tonsils, tongue, mouth, lips, larynx, nose, sinuses, salivary glands, and thyroid gland.
A radiation oncologist is a cancer doctor with special training in using radiation therapy (RT) to treat cancer.
A head and neck medical oncologist is a cancer doctor who specializes in head and neck cancers. This includes cancers of the tonsils, tongue, mouth, lips, larynx, nose, sinuses, salivary glands, and thyroid gland.
An endocrinologist (EN-doh-krih-NAH-loh-jist) is a doctor with special training in endocrine problems. These disorders affect glands and organs that make hormones. They include diabetes, infertility, and thyroid, adrenal, and pituitary gland problems.
A dental oncologist is a general dentist with special training in managing oral problems from cancer, treating cancer, or both.
A maxillofacial (max-ill-o-FAY-shul) prosthodontist (pros-thoh-DON-tist) has special training in treating problems of the face, jaw, and nearby soft tissue. They’re trained in making a prothesis (pros-THEE-sis), an artificial (man-made) piece that replaces a body part. It’s also called a prosthetic.
An oral and maxillofacial (max-ill-o-FAY-shul) surgeon is a doctor with special training in treating many problems and injuries that affect the head, neck, mouth, jaw, and face.
A neurosurgeon is a doctor with special training in surgery on the central nervous system (brain, spinal cord or spine, and nerves).
A plastic and reconstructive surgeon is a doctor with special training in cosmetic and reconstructive surgery. These procedures restore function and appearance.
A radiologist is a doctor with special training in using imaging to diagnose and treat disease. Imaging includes X-rays, sonography, ultrasound (US), computed tomography (CT), and magnetic resonance imaging (MRI).
A pathologist is a doctor who uses a microscope to make a diagnosis from cell and tissue samples. They analyze the samples to learn more about a health condition, such as cancer.
A social worker is a healthcare provider with special training in helping people cope with problems in their lives. They support you emotionally by providing counseling and practical help.
Talk with an MSK Care Advisor. We're here 24 hours a day, 7 days a week.

Clinical social worker Nicole Wood supports MSK patients and their families during and after cancer treatment.
Cancer treatment affects your body and emotions. The experience is not the same for everyone. We will support you during your treatment.
But you’re also a person with a life beyond cancer. We want to help you get back to it. That’s why we have many programs and services to support you and your loved ones.
You can connect with other people going through cancer treatment in our virtual support groups, led by a social worker.
Or you may need help with side effects of treatment. We have experts with special training in treating pain.
Your caregivers are a very important part of your care team. They need support, too. We have a Caregivers Clinic to help your loved ones cope with cancer.
Our Integrative Medicine and Wellness Service offers complementary, natural, and holistic treatments. They include acupuncture, meditation, massage therapy, yoga, and exercise.
You may want support to cope with side effects of treatment. These may include pain, fatigue (feeling very tired), nerve problems, nausea, insomnia, and stress.
Without using prescription drugs, integrative therapies can help improve and control side effects of cancer treatment.
MSK integrative medicine services are available in New York City, New Jersey, Westchester, and on Long Island.
Pain management is an important part of cancer care. MSK was the first cancer center in the country to have a service just for treating pain in people with cancer.
Our pain experts will help relieve or manage pain after surgery. They can help while you’re still in the hospital, and after you’re home.
We have experts who manage the symptoms and side effects of cancer treatment, such as nausea during chemotherapy.
We offer counseling and support to help you manage anxiety, depression, anger, or loneliness. There are individual and group counseling sessions, both in person and through telemedicine visits. Counseling is open to you and your family, separately or together.
We also run support groups and programs if you want to talk with other people going through a similar experience. Our social workers can offer information about how to talk about your diagnosis with family members, work colleagues, and friends.
Cancer treatment can affect your digestion (how your body breaks down the food you eat). It can change your taste, how you eat, and how hungry you are.
Our clinical dietitian nutritionists can help with:
MSK is a place where people of all genders and sexual orientations feel welcome and treated with respect. Our LGBTQI+ Cancer Care Program gives you the support you need during cancer care. It’s for LGBTQI+ people getting screened or treated at MSK, or in our survivorship program.
We believe cancer care needs to be as convenient as possible. We have thyroid cancer treatment locations in New York City, Westchester, on Long Island, and in New Jersey.
At our locations, you can meet with your care team and get your thyroid cancer treatment. You may be able to have chemotherapy or radiation therapy, or join a clinical trial. Our endocrinologists are located in Manhattan and Montvale, N.J.
MSK brings its expert care closer to you so you can get back home to what matters most.
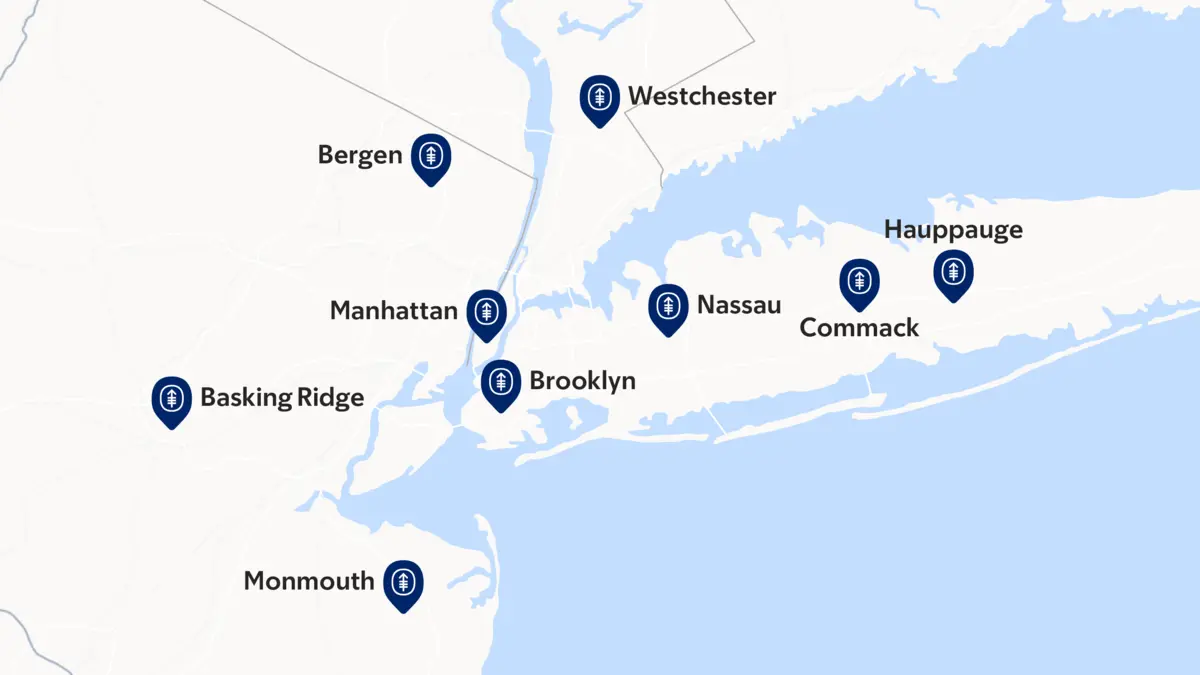
We’ll guide you about where you can go for check-ups, procedures, or treatments, based on your diagnosis and treatments.